Disguising Cancer as Salmonella
Interview with
Chris - Making cancer cells resemble the Salmonella bacterium might sound like an odd thing to, but oddly enough, it could hold the key to creating anti-cancer vaccines which trigger the immune system to actually attack cancers. And to explain how, we're joined by Professor Julie Magarian Blander from the Mt. Sinai School of Medicine in New York. Hello, Julie.
Julie - Hello.
Chris - So first of all, why doesn't the immune system attack cancer in the first place?
Julie - The immune system recognises its own tissues by a process called pattern recognition. So when it's searching for microbes, it's really searching for patterns that are associated with microorganisms and these patterns are absent from normal healthy tissues. Therefore, because tumour cells and cancerous cells are derived from normal cells, they don't have those microbial patterns that the immune system likes to see and target.
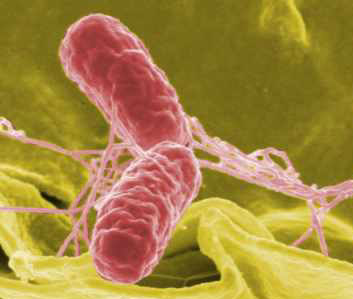 Chris - So that's why they escape normal surveillance. So what were you doing with Salmonella?
Chris - So that's why they escape normal surveillance. So what were you doing with Salmonella?
Julie - With Salmonella there is this protein called flagellin which Salmonella and other bacteria actually use for locomotion and therefore, we took this protein - the sequence of this protein - it's easy to express in cells because it's a protein in nature. We expressed it in tumour cells in order to make them look more microbial to the immune system. By doing so, we could target the receptors that recognise these patterns or structures that are associated specifically with microbes. In this way, you are tricking the immune system to think that tumour cells actually have a component that's derived from microbes and then they're targeted this way.
Chris - So the cells are made to look more like a bacterium. This gets the interest of the immune system via these special receptors it has to pick up pathogens. The immune system then attacks the tumour cells. That's all very well for the tumour cells that you have added the Salmonella-like gene to it, but what about the tumours elsewhere around the body?
Julie - So, in animal models, in mice, the strategy is to take the tumour cell itself, introduce this flagellin protein in order to target the receptors of the immune system and then irradiate the tumour cell and use that as a whole cell cancer vaccine. We have done two different sets of experiments where animals that do not have tumours have been vaccinated and then we tested their protection against subsequent challenge from a wild-type tumour that does not express the flagellin. We've also done experiments where animals that bear tumour already were vaccinated and then we monitored the immune response. In both cases, we were able to see that the immune system efficiently mounts a robust immune response - both the CD8 cytotoxic T-cell response and a helper response system important for making those CD8 T cells aggressive and capable of attacking the tumour cells.
Chris - So the immune system, once it's been primed using the Salmonella resembling vaccine cells, which are actually killed and don't go anywhere else once you put them in, the system then begins to attack the rest of the tumour. Presumably, there's some kind of crossover then. The immune system learns to recognise the cancer cells, having had its interest peaked by the presence of the Salmonella flagellin gene.
Julie - Yes, exactly. What we were able to show is that we can boost the memory response. The whole basis for vaccination for infectious diseases is, for example, you vaccinate with a particular component of a microbe and then the individual that's been vaccinated is protected, sometimes throughout their lifetime, against the infection itself. Here, it's the same idea. Because the microorganism has been seen the flagellin from the microbial components from Salmonella within tumour cells, the immune system can then make a response to that tumour and then subsequently that memory response is what protects against further development or growth of the tumour.
Chris - And there's no danger that the immune system might be led to start attacking healthy tissue because it gets interested in the cells and reacts to the wrong thing on them and then starts attacking healthy tissue.
Julie - Yes. This has been a caveat for whole cell cancer vaccines and many investigators do not prefer that, but there are also powerful mechanisms of tolerance that are inherent to the immune system. We have not addressed this in our study, but those mechanisms are so powerful that we think that we might be favouring the presentation of specific cancer derived molecules and those are the ones that are preferentially going to be targeted. So, cancer cells can share normal proteins with healthy cells, but they also have their own set of proteins that they express and there's a lot of efforts in identifying what those proteins are. Our hope is that by introducing flagellin, we can bypass the process of systematically identifying the individual proteins that cancer cells might have unique to them and not expressed on normal cells. In this way, we could, without knowing what those specific proteins are, we could prime the immune system to a whole slew of things that are going to be new to the immune system. And therefore, those normal proteins may not be targeted but it is something that we need to test in animals.
Chris - And just to finish off, talking of animals, the mice that you tested in your study, how did they do? What sort of improvement or clinical outcome did you get with those animals that were treated with this vaccine?
Julie - We had several models where we had transplantable lymphoma cells and also melanoma cells that are metastatic. With the melanoma cells, it was really dramatic. These melanoma cells are injected intravenously into mice and they metastasise to the lung. Those mice that were vaccinated with the flagellin containing melanoma whole cell vaccine did not have any metastasis. Their lungs were completely free of metastasis compared to the control animals that were not vaccinated. And similarly, the subcutaneous growth of those tumours, lymphoma cells that we have transplanted subcutaneously into the immunised mice, all the mice rejected the tumour and were capable of mounting a robust memory response to that tumour compared to the wild type unimmunised controls.
Chris - Super! We'll leave it there but thank you for bringing this up to speed. That's Julie Magarian Blander from the Mt. Sinai School of Medicine in New York.









Comments
Add a comment