Stem Cells for Heart Disease
Interview with
Chris - We've heard from Niall already what a heart attack is and that it leads inevitably to the irreversible destruction of the tissue that makes up the heart, but now we're asking if there's anything we can do to put that right. Stem cells enter the frame here, so how are you trying to investigate this?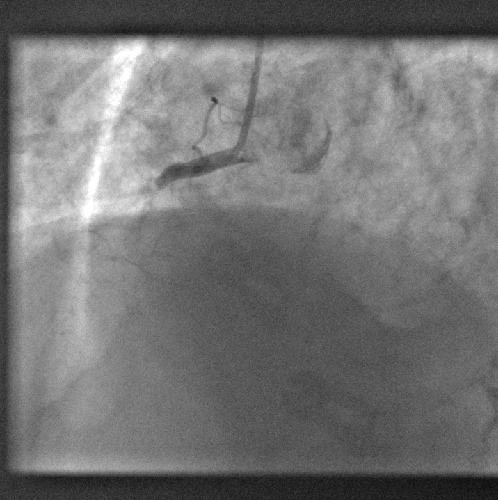
Anthony - We're starting with a very simple approach, hopefully a relatively obvious one. We think that adult bone marrow has cells in it that have the potential to repair damaged organs, due to some interesting work undertaken during the last five to ten years.
Chris - Why should it be the bone marrow?
Anthony - All of our textbooks talk about the fact that you're born with as many heart cells as you will ever have, in fact, you die with fewer heart cells. The heart can't regenerate itself, as opposed to the liver, which will grow back again even if you lose a substantial amount of it. Some recent, exciting evidence suggests that the heart might have cells that can regenerate. The question has arisen of where these cells could come from. Clearly with modern diseases the system that can repair and regenerate the heart is not able to deal with the consequences of a heart attack.
Chris - Presumably, when you've had a heart attack resulting in quite serious devastation to a region of the heart, any cells in that region that could have stem cell like properties and could repair that area will, themselves, have been destroyed.
Anthony - Indeed, but there are thoughts that there are little niches or collections of stem cells tucked away around the heart that are able to grow in the surrounding areas; but by no means enough of them. Some evidence that has come to light suggesting that the bone marrow might be producing the body's police mechanism, which goes around looking for the damage that occurs on a daily basis. Every time you knock your arm you're going to lose a few cells here and there, and the system from the bone marrow might well be replacing those few cells that get lost. Unfortunately though, not the large amount of cells that get damaged or lost in a heart attack.
Chris - So how would you aim to manage a heart attack with these stem cells?
Anthony - Our first study, which has recruited about 70 patients now, is dealing with patients who have had heart failures. They've had a big heart attack or several heart attacks at some point in their lives, their heart is damaged and no longer works as a pump. This causes them to get breathless, tire easily, collect fluid on their lungs and lead a poor quality of life. What we have done so far is to take a sample of their bone marrow, process it to get out what we think are the clever cells and inject those cells back into the heart in an attempt to see if they will actually improve.
Chris - When you say 'injected them into the heart' would you put them directly into the damaged muscle, or just into the blood vessel?
Anthony - Both. The research out there at the moment suggests that if you put it directly into the blood vessels around the heart or directly into the heart muscle itself it does have an effect. Our study is actually testing which mechanism, or route, is better.
Chris - Do you actually know how these cells are working? Has anyone managed to do any studies to follow them to see where they go, what they turn into and what changes they induce to happen in the bits of the heart that you think they're effecting?
Anthony - Well that's a very interesting question, the great debate now amongst the scientists who are doing this work is the mechanism. There are at least five different mechanisms by which these cells might be beneficial that have been shown in the animal models. The problem is that although they've shown up to a 40% improvement in heart function in the animal models, it's suggested that it could be any one of those five mechanisms, or a combination of a number of them causing this improvement. In Man it's very hard to demonstrate mechanism as you don't have the same access to what happens to the cells and therefore we don't know for sure how many cells actually stay in the heart and do some good.
Chris - Does it actually have a clinically beneficial effect, in the sense that you have people who couldn't climb stairs or make the bed before, but after this procedure they find they're a lot better off?
Anthony - The answer to that has to be yes, but the problem with this field is that it's dominated by lots of small studies that are not the gold standard of randomised control trials. Our objective is to produce randomised control trials so our patients can make their own minds up. It's a blinded study, so we don't know if our patients receive cells or a placebo, but so far approximately half of our patients seem to have got better and half not. This suggests that something is going on, but it's not until the end of the study that we can unblind it and see exactly what has happened.
Chris - Do you have any feeling for how long the beneficial effect might last for? Some therapies seem to produce a massive improvement to start off with, but when you follow people up for longer the effect seems to go away again. Is there a worry that could happen here?
Anthony - Our study is looking at patients at one year and at six months, so the effects are holding out to at least one year. Beyond that, its such a new area we have no way of predicting what will happen. If we can find a route or a mechanism of administering these cells and taking these cells out of people that is straightforward then we may be able to re-administer cells in an effort to get more improvement or to restore improvement should it start to decline.
Chris - I suppose that another major benefit is that as the cells are coming from the person themselves there are no additional risks from diseases or rejection, as it's not foreign tissue.
Anthony - There are certainly risks associated with this, but as you rightly say it avoids all issues about transplanting across species or human individuals which could lead to rejection and possible transmission of illness.
- Previous What is Heart Disease
- Next Make your own hot air balloon









Comments
Add a comment