Improving IVF
Interview with
Kat - This is the Naked Scientists with Dr. Chris and Dr. Kat and we're talking all about the science of pregnancy and conception. Now, many people manage to get pregnant doing it nature's way, when mummy and daddy love each other very much. But some people need a little bit of medical help and that's when they turn to in vitro fertilization. For some people, this is the only they're able to have their own children but at the moment, it is far from perfect and there's quite a high failure rate. This can leave people obviously very distraught and out of pocket and sometimes, because often multiple embryos are put into women, people who just want one baby can end up to slightly more than that. Now, in a few minutes, we'll be hearing how blood test could tell whether or not you're suitable for IVF. But first, we're joined Dr. Dagan Wells from Oxford University. Hello.
 Dagan - Hello there, Kat.
Dagan - Hello there, Kat.
Kat - Hello. Just for a start, talk us through the IVF process. What's it basically all about and what's going on there?
Dagan - Sure. Well, it's been an enormously successful technique since it was developed in a little over 30 years ago now. It's essentially a way that you can get around problems where maybe the egg is having difficulty making it through to the womb or sperm having difficulty making it to the egg or fertilizing the egg, and what happens is the woman actually undergoes a course of a hormonal treatment which allows her to generate multiple eggs in a single cycle, rather than the usual one that you would get in a typical monthly cycle. Those eggs are then taken out and outside the body their fertilized with her partner's sperm and so that's get around any possible difficulty that the sperm would have, reaching the egg and after that, several embryos are usually produced from these eggs and then the real challenge, and what we've really been working on, is trying to work out which of those embryos should actually be then transferred back to the mother. The idea is, ideally, that you transfer one back and then get one pregnancy and hopefully, one healthy baby out at the end. But the problem of is that actually multiple embryos are generated but they're not all equal. They don't all have an equal chance of making a baby and so, what we're trying to do now is to find out which we should transfer. At the moment it's bit of a luxury and just to increase the odds of success, it's not unusual for an IVF centre to transfer several embryos and certainly, in other countries, in the U.K. it's rarely more than two.
Kat - So, tell us a bit about some of tests that you've been developing because I've actually, in my previous life as a scientist, worked on human embryos and I am sometimes amazed that any humans get pregnant at all. How can you tell what are good embryos and what are bad ones?
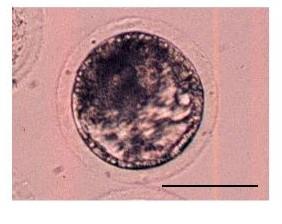 Dagan - You are absolutely right. It's amazing really, when you actually see what's going on in the human embryos, that we get pregnant as easily as some people seemed to manage. The primary way that's been used for many years is to just look at the embryo down the microscope. There were certain appearances of the embryo which may give you a clue that made the embryo isn't developing as well as it should. However, it's wide knowledge that really, that's only a very rough guide to embryo quality, the chance of them, making a baby. And so, what we've been looking at is in more detail on the genetic level. Specifically, we've been looking at the chromosomes. Now, as you probably know, every cell in the body ought to have 46 chromosomes with just a couple of exceptions and so, that's what you would expect to find. However, it turns out that in human embryos, this is incredible level of chromosome abnormality, having the wrong number of chromosomes, and the effect of that usually is that those embryos affect through these chromosome abnormalities, cannot actually produce a child. Either they just never initiated pregnancy at all or they miscarry early in pregnancy.
Dagan - You are absolutely right. It's amazing really, when you actually see what's going on in the human embryos, that we get pregnant as easily as some people seemed to manage. The primary way that's been used for many years is to just look at the embryo down the microscope. There were certain appearances of the embryo which may give you a clue that made the embryo isn't developing as well as it should. However, it's wide knowledge that really, that's only a very rough guide to embryo quality, the chance of them, making a baby. And so, what we've been looking at is in more detail on the genetic level. Specifically, we've been looking at the chromosomes. Now, as you probably know, every cell in the body ought to have 46 chromosomes with just a couple of exceptions and so, that's what you would expect to find. However, it turns out that in human embryos, this is incredible level of chromosome abnormality, having the wrong number of chromosomes, and the effect of that usually is that those embryos affect through these chromosome abnormalities, cannot actually produce a child. Either they just never initiated pregnancy at all or they miscarry early in pregnancy.
Kat - So, tell us a little bit about the way you've been testing because at the moment, they do a pre-implantation, genetic diagnosis on embryos when they're just, you know, a few cells. Tell us about the technique that you've been developing.
Dagan - Yes, that's exactly right. There is an existing technique where a single cell is removed from the embryo, three days after fertilization. At which point, it usually is only consisting of about six to eight cells. So, at that point, you can take one cell and you can test it and you can look at about half of the chromosomes that are in there. And people have used that for a number of years. Some people have said that it's helped considerably with pregnancies, but other people have said it doesn't work at all and may actually would reduce the chance of the embryo making a baby. Now, the difference of what we're doing now is we're waiting an extra two days. Might not seem like much, but in those two days the embryo goes from just a handful of cells up to over a hundred cells. And that means that at that point, we can actually take several cells. Now, the effect of that is that we get a much more reliable test.
Kat - And that doesn't presumably do too much damage to the embryos. So if you've got a woman that the test says it's all right, you are not going to be hideously harming it?
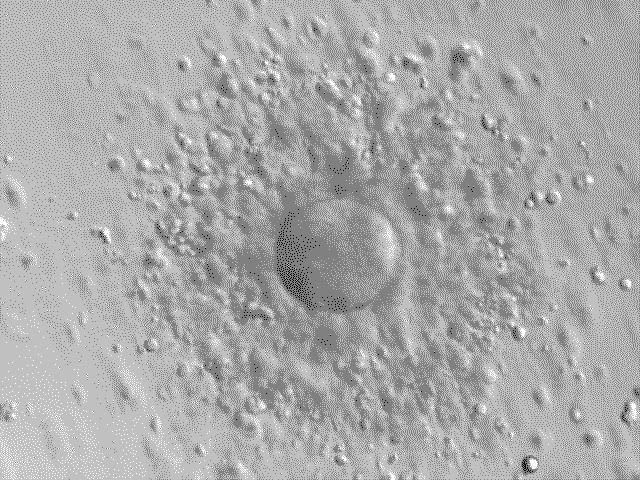 Dagan - Exactly. Again, if you do the traditional test, looking on day three after fertilization, there is accumulating evidence that, that may have some impact on the embryos ability to form a pregnancy. It's not that it's going to give rise to a child with, you know, a body part missing or something like that. It's a more all or nothing thing. It may just simply not make a pregnancy. Now, if you look at the stage that we look at, known as the blastocyst stage, two days later, that's a very robust stage and the embryo tolerates the biopsy beautifully, almost as though nothing had happened to it. The other thing we're doing is rather than just looking at half the chromosomes, we're looking at the full set. So, we're really getting a very comprehensive idea of what's going on.
Dagan - Exactly. Again, if you do the traditional test, looking on day three after fertilization, there is accumulating evidence that, that may have some impact on the embryos ability to form a pregnancy. It's not that it's going to give rise to a child with, you know, a body part missing or something like that. It's a more all or nothing thing. It may just simply not make a pregnancy. Now, if you look at the stage that we look at, known as the blastocyst stage, two days later, that's a very robust stage and the embryo tolerates the biopsy beautifully, almost as though nothing had happened to it. The other thing we're doing is rather than just looking at half the chromosomes, we're looking at the full set. So, we're really getting a very comprehensive idea of what's going on.
Kat - And how are you actually looking on the chromosomes? What's the technique that you're using?
Dagan - Well, we're using a method that was originally developed for looking at chromosome abnormalities in tumors which are of course, very common. They have a similar problem to what we have and that is very hard to actually get a cell, to show you its chromosomes from some cancers and certainly, from the cells of the embryos. So what we do is we actually take the DNA that makes up the chromosomes out of the cells and we actually colour it in, we label it with a fluorescent colour, and usually, we label the embryo cell DNA green. We then take some DNA from someone who we know has a normal set of chromosomes, they're exactly the right number and label their DNA with a red colour. We'll mix those green and red DNAs together and we apply them to some chromosomes that are stuck on a microscope slide. Now what happens is the red and green DNAs kind of fight it out to stick down to these chromosomes. If they fight it out equally, all of the chromosomes get equally covered with red and green DNA, and you get kind of yellow colour from the mixing of those two colours. But if our embryo for example had one chromosomes too many, it's going to have relatively more green DNA than it should, just because it's got one chromosome more than it should. And so, one of chromosomes on the microscope, down on the microscopic slide, will end up looking more green than they ought to and that's what gives away that there's been an abnormality.
Kat - Fantastic and so, just very briefly, are you actually using this to get successful pregnancies? What's the success rate like when you do this test?
Dagan - Yes, it's a great question. That's the real acid test at the end of the day. Well so far, we've done a prospective trial of this and this is in association with a centre in America called the Colourado Center for Reproductive Medicine. Now this isn't a randomized trial, so it's not really the gold standard study, but what it is, is a prospective trial which I think, is indicative. We've done about - well, over a hundred cycles now and the pregnancy rate is actually about 90% which is way higher than you would ever normally expect in IVF. Now, that has to now go ahead and be verified in a well controlled study which is what we're going to be initiating actually in London in September of this year.
- Previous The Future of Scientific Journals
- Next Blood Tests for IVF Success









Comments
Add a comment