Photo-therapy is the term used to describe treatments which use light to achieve their effects. Examples include the treatment of seasonal affective disorder (SAD) in winter by the controlled use of artificial light, and blue light exposure which is used to treat new-born babies with neonatal jaundice. In the case of the latter, blue light reacts with bilirubin, the yellow pigment responsible for producing the skin discolouration, and turns it into a more soluble form which is easier to excrete from the body.
Another application of photo-therapy, called photodynamic therapy (PDT), uses a combination of electromagnetic radiation (usually laser light) and a drug (given as an injection or in tablet form) to selectively target and destroy cancers. Conventional cancer therapies rely on removing or destroying the diseased tissue, usually with surgery, radiotherapy or chemotherapy, whilst attempting to spare the surrounding healthy tissue. But these approaches are often associated with significant side effects including pain, nausea, vomiting and infection. But PDT is much more specific, which means that there is less damage to healthy tissue, and it doesn't require a major operation. The process is outlined in figure 1, below.
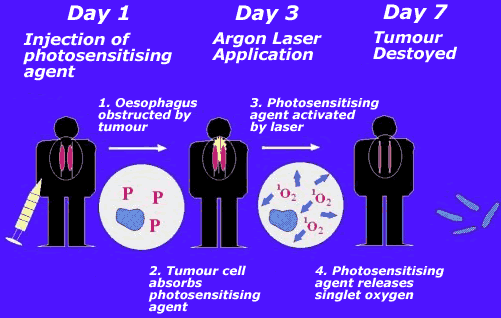 |
| Figure 1: The process of photodynamic therapy. A drug is given to the patient (1) which accumulates in the diseased tissue (2). In its inactive form the agent is harmless, but when it is excited by light (3) of the correct wavelength (usually in the form of a laser) it produces singlet oxygen which is highly toxic (4) and kills the cell. |
Photodynamic therapy (PDT) uses laser light for many reasons: the beam has a high power, high intensity and, unlike a normal house bulb, it can rapidly be switched on and off. Also, whilst white light contains lights of many different wavelengths, a laser produces light of only a single wavelength which can be adjusted to suit the required intensity, the degree of tissue penetration and the type of molecule that you wish to activate.
 |
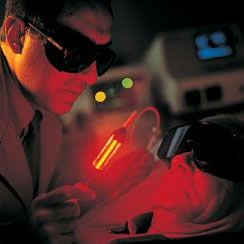
Figure 2 : PDT uses laser light to deliver light of the correct wavelength needed to activate the photo-sensitisive agent and produce singlet oxygen. |
The photosensitising agents used in PDT all have very similar structures and are often based on naturally-occurring molecules including haemoglobin (the substance that makes blood look red), Vitamin B12, and chlorophyll (the chemical used by plants for photosynthesis and which gives them their green colour). These compounds are all known as 'macrocycles' and contain nitrogen, oxygen or sulphur atoms locked inside a large hollow ring. In some cases the ring also contains a metal such as iron or magnesium. Examples of these molecules are shown in figure 3, below.
Photodynamic therapy currently makes use of a range of agents from plant extracts to complex synthetic macrocycles, but characteristically, they are all able to accumulate selectively in the diseased tissue. Verteporfin is being made by QLT Phototherapeutics and is being tested to treat blindness. The drug stops the abnormal vessels in the middle of the eye from leaking and causing retinal scarring. It is also being tested for the treatment of other diseases such as rheumatoid arthritis (which causes stiffness and soreness in joints) and skin problems including psoriasis. Temoporfin is being marketed by Scotia Pharmaceuticals for the treatment of head and neck cancers.
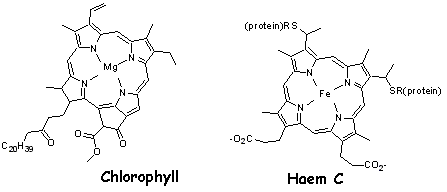 |
| Figure 3 : Naturally-occurring macrocycles |
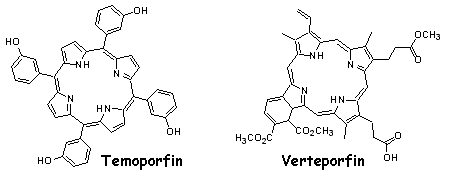 |
| Figure 4: Synthetic macrocycles Temoporfin and Verteporfin which are being applied in the treatment of head and neck cancers, auto-immune disorders including psoriasis and rheumatoid arthritis, and vascular proliferative disorders of the retina. |
 Crucially, these drugs cause fewer side effects than conventional cancer treatments because they remain in an inactive form until they are 'switched on' by shining light of the correct wavelength onto the diseased tissues. However, in order to work effectively they require the presence of oxygen, although this is rarely a problem in the human body. When designing newer versions of these agents, manufacturers aim to minimise the time that the drug remains in the body in order to avoid causing side effects, although it's important to select an agent which can achieve adequate tissue-penetration - if the drug cannot reach the diseased parts of the body in sufficient amounts, there will not be enough of the agent present to provide effective activity. It's also important to bear in mind that the skin can become sensitive to sunlight for some time after treatment, so patients are usually warned to avoid the sun for a while afterwards to avoid an untimely sunburn.
Crucially, these drugs cause fewer side effects than conventional cancer treatments because they remain in an inactive form until they are 'switched on' by shining light of the correct wavelength onto the diseased tissues. However, in order to work effectively they require the presence of oxygen, although this is rarely a problem in the human body. When designing newer versions of these agents, manufacturers aim to minimise the time that the drug remains in the body in order to avoid causing side effects, although it's important to select an agent which can achieve adequate tissue-penetration - if the drug cannot reach the diseased parts of the body in sufficient amounts, there will not be enough of the agent present to provide effective activity. It's also important to bear in mind that the skin can become sensitive to sunlight for some time after treatment, so patients are usually warned to avoid the sun for a while afterwards to avoid an untimely sunburn.
ACKNOWLEDGEMENTS - With thanks to Dr. John Reglinski, Strathclyde University.









Comments
Add a comment