Getting under the Skin of Melanoma
Interview with
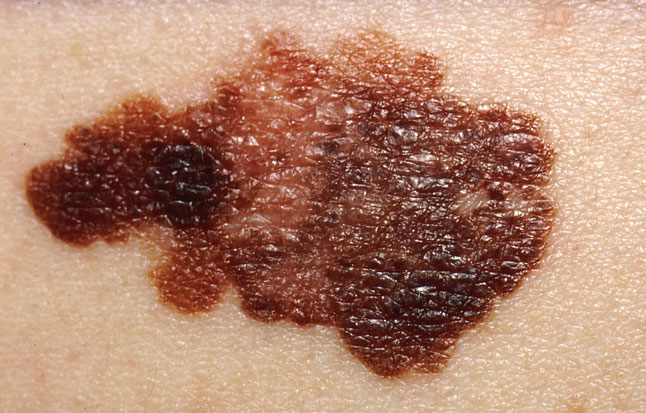
Diana - This week has also seen a breakthrough in the field of melanoma, a form of skin cancer that's becoming increasingly common; in fact, the incidence of the disease has doubled in the last ten years. But now there's some good news, because, with the help of a tankful of fish, scientists at Harvard University have discovered a key gene that drives the disease and therefore could hold the key to new ways to treat it. To explain more and talking to Chris, here's the author of the work, Leonard Zon.
 Leonard - Well, my laboratory has been focusing on melanoma which is a very deadly skin tumour and we had developed about 5 years ago a model of melanoma in the zebrafish. In this model, we took the human gene that's known to cause melanoma, a gene called BRAF and we over expressed it in the zebrafish, in combination with another gene, P53 which is the most common mutated form of a tumour suppressor gene in humans. That combination led to fish that develop melanoma. We were able to study those tumours and they really resemble very similar signatures of genes, to what you would see in a human tumour.
Leonard - Well, my laboratory has been focusing on melanoma which is a very deadly skin tumour and we had developed about 5 years ago a model of melanoma in the zebrafish. In this model, we took the human gene that's known to cause melanoma, a gene called BRAF and we over expressed it in the zebrafish, in combination with another gene, P53 which is the most common mutated form of a tumour suppressor gene in humans. That combination led to fish that develop melanoma. We were able to study those tumours and they really resemble very similar signatures of genes, to what you would see in a human tumour.
With that, we wanted to understand whether we could use this model to find new genes that cause cancer or find new therapies that might be used for the treatment of melanoma. We knew there was a region on human chromosome-1 that was amplified in about 30% of all human melanoma. We studied that region and found that there were 54 genes in that interval. We then looked at gene expression among 100 human melanomas and we found that 17 of those genes were expressed very highly. And so, we needed to figure out which was the driver gene, which was the most important to the cancer. And so, what we decided to do was to take each of these 17 genes and to inject them individually into our zebrafish embryos at the one cell stage, and then to grow up those fish and count how many fish developed a melanoma. What we found was that one of those genes, a gene called SETDB1, had the ability to greatly accelerate the melanoma, and this was likely to be the driver gene in this particular critical interval.
Chris - And is this representative of what you think goes on in humans? In other words, if you were to take human melanomas, real clinical tissue, do you see the same gene, this SETDB1 gene that you've now discovered to be involved also mutated in the human problem?
Leonard - Well that's right. So, 30 percent of human melanomas will have amplifications of SETDB1 and we went on to show in this paper that actually, 70 percent of melanomas will over express SETDB1. So it's something that's central to being a melanoma tumour is to over express this particular gene. So I think that over time, we'll be able to see that this gene also participates in other cancers too, and this region is also amplified in other tumours of humans such as lung tumours, and also breast tumours.
 Chris - We'll come on to what SETDB1 might be doing in a second, but first of all, if 70 percent have it, what about the 30 percent of human melanomas that don't? What's going on with them then?
Chris - We'll come on to what SETDB1 might be doing in a second, but first of all, if 70 percent have it, what about the 30 percent of human melanomas that don't? What's going on with them then?
Leonard - The way I think about this as an oncologist is, if I see a patient, I'll often describe their tumours as let's say, poorly differentiated or well-differentiated. What that means is that I can actually classify them by how the tumour looks under a microscope. We think that melanoma isn't a single disease, but there's actually different causes of melanoma. And so, there's different driver genes, depending on where the melanoma arises on your body and what types of exposures to carcinogens or light, sunlight is often thought as an instigator for the melanomas. So, with all these different options, the tumours could be heterogeneous and so, what we would say is that the 70 percent that over express SETDB1, that must be one category, and then the other 30 percent have a different classification and probably represent a different stage or a different location of those melanomas.
Chris - So what do you think SETDB1 is doing?
Leonard - Well, there's a new field that's blossomed over the past 5 years called epigenetics. Epigenetics deals with things that aren't inherited in a typical genetic manner. We're used to mutations, let's say, being inherited genetically, but in this particular case, DNA is actually wound around a spool and that spool is a set of proteins called histones. When DNA is wound too tightly, the genes are shut off. When DNA is wound loosely, the genes are on. This gene SETDB1 seems to wind the DNA a little bit too tightly and that shuts off particular types of genes that have an identity in the melanoma. So for instance, one class of genes that we found are a gene set called the hox genes which regulates the body plan normally of how embryos developed. But we think that somehow, this gene alteration in terms of expression leads to a change in the cell fate and that makes the tumours more invasive.
Chris - And does this in turn also give you new strategies for how to combat melanoma? The survival prospects for someone who's diagnosed with an advanced melanoma are really dismal at the moment, are we going to be able to do something about it with this discovery?
Leonard - So SETDB1 is an enzyme that actually methylates the histones and that regulates whether the DNA is tightly wound or not. And so, because it's an enzyme, it's possible to make inhibitors to this enzyme and so, we're in the process now of talking to drug companies to think about inhibiting this particular enzyme and we think this is a wonderful treatment for the patients, 70 percent of the patients who over expressed this gene who have melanoma.
Diana - Harvard Scientist Leonard Zon talking to Chris Smith there. He published that work he was discussing with me, this week in the journal Nature.








Comments
Add a comment