Diagnosing abnormalities from a Cervical Smear
Interview with
Meera - This week, I've come along Northwick Park Hospital in London to find out the basics of the cervical screening program. Here to fill me in on this process is Tanya Levine, Consultant Cellular Pathologist here at Northwick Park Hospital. First of all, who should be screened?
Tanya - Women between the ages of 25 and 64 are invited for screening.
Meera - And when somebody comes in for a sample, we know that the sample is taken from their cervix, but what part of the cervix is the sample taken from and why that particular area? 
Tanya - The sample should come from an area of the cervix, which is the neck of the womb, and this area is called the transformation zone. And it develops at about the time of puberty and what happens at that stage is that under the influence of oestrogens, the cervix increases in size and bulk. And in so doing, some of the surface layer of cells undergo a process of squamous metaplasia, and what this really means is that the cells change their appearance, and this is a normal physiological process, but it can be hijacked if you get human papillomavirus onboard. The cells can be converted from this normal physiological pathway to the pre-cancer sequence of events.
Meera - Okay, so you have a sample and you have a slide of the cells from this transformation zone around the cervix. What changes are looked for?
Tanya - Of the many cells that you can see on a sample, there are two basic type of cells that we are particularly interested in as cytologists. One are called squamous cells and the other are called endocervical cells. Now the squamous cells look not a little unlike fried eggs. In that the yolk of the egg is a nucleus and the white of the egg is a vision of the cell that we call the cytoplasm. We're looking to see the consistency of the nucleus or consistency of that yolk, if you will. And in so doing, we will grade those cells as mild, moderate or severely diskaryotic cells.
Meera - Okay and so, in order to just show me how clear some of these differences can be, you've got some slides here with samples taken from patients in the past.
Tanya - What I thought I'd show you is a normal sample, just to get your eye in on what we're looking at down a microscope, and Meera, if you look down the field at the moment, what you can see are normal squamous epithelial cells. Now these are the fried egg cells that I was talking about earlier.
Meera - And looking through actually, the nucleus is very small compared to the overall size of the cell.
Tanya - These are entirely normal. If you look at this sample now, there's actually a 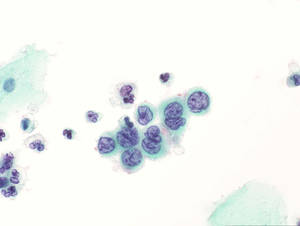 range of appearances that we can see here in these squamous epithelial cells. The nucleus is taking up much more of the surface area of the cell. In fact in this cell, it's virtually filling it and this is a severely diskaryotic cell.
range of appearances that we can see here in these squamous epithelial cells. The nucleus is taking up much more of the surface area of the cell. In fact in this cell, it's virtually filling it and this is a severely diskaryotic cell.
Meera - How many of the samples that come through are abnormal?
Tanya - In our laboratory, we process just under 60,000 samples a year, and about 93% to 94% will be negative.
Meera - So of those 6% to 7% that are abnormal, what's the next step?
Tanya - Someone with low grade abnormalities may have repeat smear. For women with moderate or worse abnormalities, they will be referred to the colposcopy unit.
Meera - That was Tanya Levine, Consultant Cellular Pathologist at Northwick Park Hospital. The presence of abnormal cells in a cervical smear doesn't mean that a treatment will be needed. The next step as we've heard is to have a colposcopy to investigate the area further. So I'm now at the Sloane Street Clinic in London with gynaecological surgeon, Thomas Ind.
Thomas - Some abnormal smears just need to be repeated. If you have another abnormality, you would come for a colposcopy which is an examination of the cervix using a specially designed microscope with some dyes. If there is an area that we can see suspicious or pre-cancerous change, we would take a local biopsy.
Meera - What's the next step then if any abnormality is confirmed?
Thomas - Most of the time, your body has the natural ability to clear these cells, but what they can do is they can form abnormalities at the bottom part of the basement membrane which is the area of the cervix that lines the cervix. Now with only the bottom third of that basement membrane is affected and has had cellular change in the nucleus, we would call that CIN1 and most of the time, that goes away on its own unchanged. If two-thirds to three-thirds of that area is affected, that would be CIN2 and CIN3 respectively. There is a good chance if we don't treat those abnormalities, that it would progress to cancer in the future. So women with those abnormalities generally have treatment. 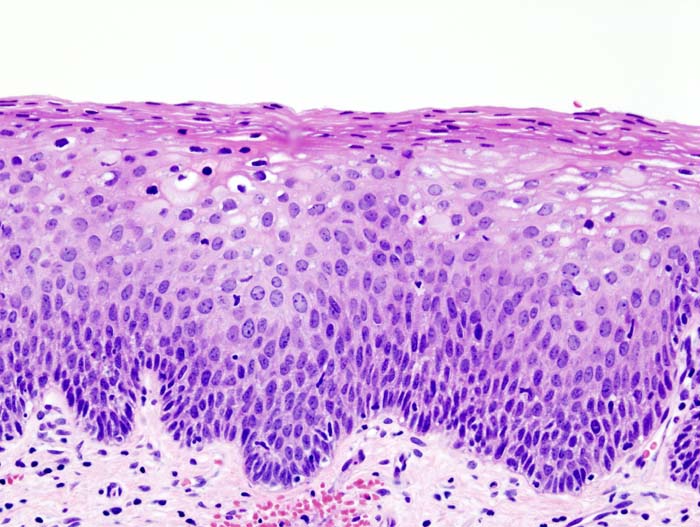
Meera - And what does CIN stand for?
Thomas - Cervical Intraepithelial Neoplasia. What that really means is cervix in the skin, new cells.
Meera - So a patient has come in and been found to have say, CIN levels 2 or 3, what are the options available to them?
Thomas - The most common treatment in the UK at the moment is something called a loop cone biopsy. It's also called a LETTS procedure and in the States, they call a LEEP procedure, and what normally happens is that during a colposcopy, a small sugar cube sized piece of tissue is excised from your cervix, removing the area of abnormality. We now use a form of energy called diathermy which is a just a very high voltage electrical instrument that removes the piece of tissue a bit like a cheese wire and it's done very swiftly in a few minutes.
Meera - What would you say the success rate is for people that come in for these treatments to not need them again or to actually prevent them from getting cancer?
Thomas - If you have a treatment, it's generally about 95% successful and by that, I mean, you will never have another abnormal smear again.
Meera - And just lastly, how would you summarise then the benefits of the screening process as a preventative measure against cervical cancer?
Thomas - Well I think most people would agree that the National Health Service Cervical Screening Program is probably one of the best cervical cancer prevention programs in the world. It's all about getting people to attend and in this country, nearly 80% of people attend for their cervical smears. It's attendance which is the key issue, not the process that you go through afterwards, and this is the problem that we've encountered with the vaccine is that if people don't attend for the vaccine, it doesn't matter how effective it is, it's not going to prevent cervical cancer.
Chris - Thomas Ind from the Sloane Street Clinic and before him, Tanya Levine from Northwick Park Hospital and they were talking to Meera Senthilingam about the importance of cervical screening.










Comments
Add a comment