Evolution of cancer drug resistance
Interview with
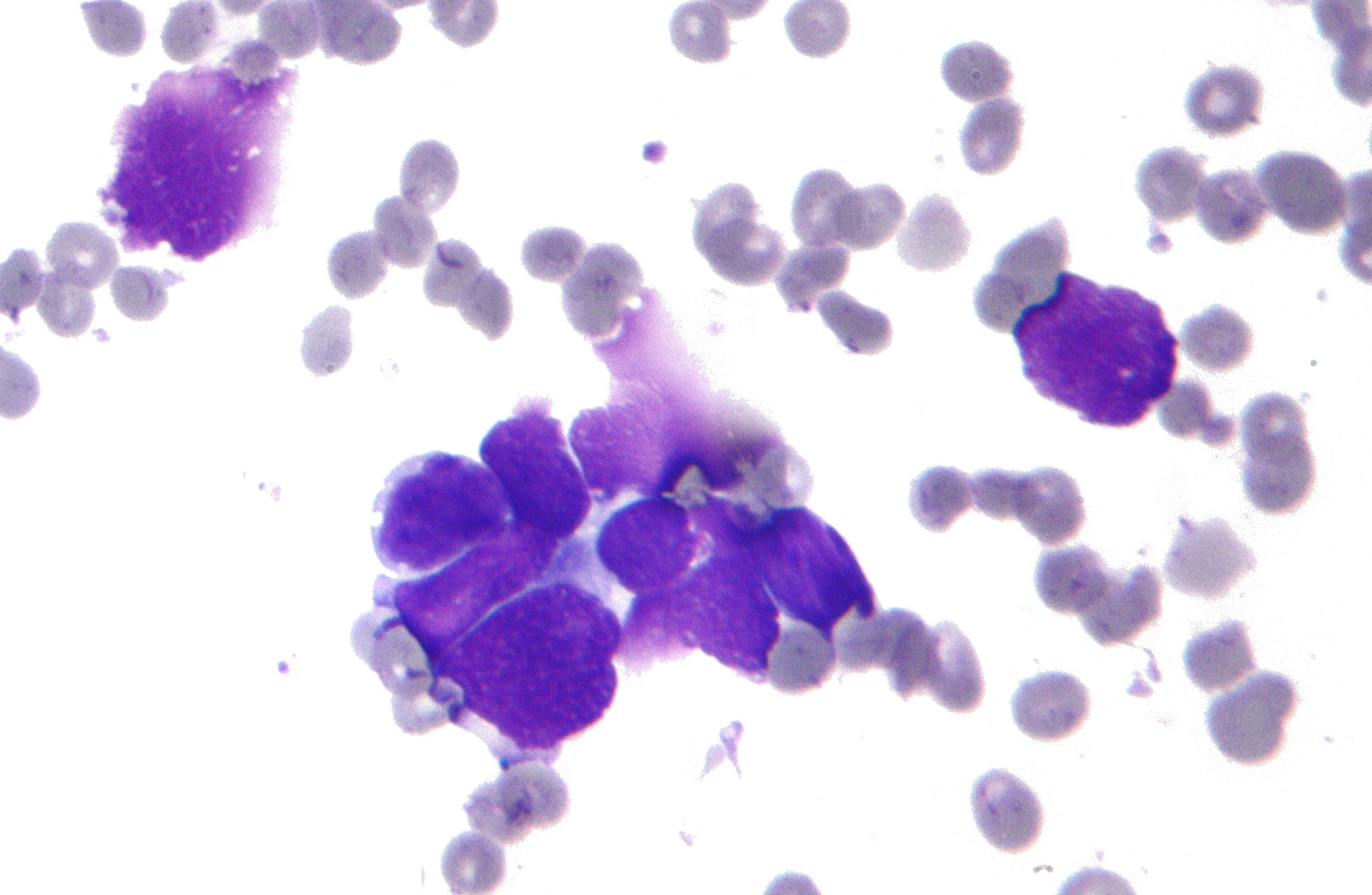 Cancer researchers and doctors all over the world are getting increasingly excited about the new era of molecular therapies designed to target specific gene faults in tumours. But while these drugs tend to show impressive results, their effectiveness soon wanes and the cancer comes back after a number of months or years, as it evolves resistance to the therapy.
Cancer researchers and doctors all over the world are getting increasingly excited about the new era of molecular therapies designed to target specific gene faults in tumours. But while these drugs tend to show impressive results, their effectiveness soon wanes and the cancer comes back after a number of months or years, as it evolves resistance to the therapy.
Kat Arney spoke to Martin Nowak, Professor of Mathematics and Biology at Harvard University, who has been using mathematical models of tumour evolution to try and understand why this happens. His results could change the way that these new treatments are used.
Martin - The initial effect of the drug is often amazing and doctors see a decline in advanced cancers to an extent that they have never witnessed before in any situation. So, this is extremely promising, but many of these therapies exactly as you say, they are short-lived and the reason is because the cancer cells develop resistance.
Kat - They kind of evolve don't they and change to escape the drug.
Martin - Yes, exactly. So, we are witnessing here an evolutionary process on a pretty fast timescale and here's also where the mathematics comes in because the mathematics of biology is very developed to understand evolution. So, evolutionary dynamics can be described with exact mathematical equations. We can describe how populations get a resistance, get mutations and then how mutations respond to selection pressure. This is what we're doing for cancer here.
Kat - How do you go about starting to model what seems like such a complex biological process?
Martin - The first question would be an estimate of how big the population of cancer cells in the body is. So, if you look at the particular lesion of a certain size then very often we're confronted with approximately 1 billion cancer cells. And then we give the treatment and the observations suggest that there are single point mutations that can actually confer resistance to the treatment. So the first question that would arise is; at the time to start treatment, are the resistant mutations already present in the patient, or do the resistant mutations emerge once therapy has started.
Kat - So, that would be single changes to a gene that would make the cells resistant to a treatment or not, to find out whether they're there at the start or whether they kind of come on later.
Martin - Yes, that's exactly right. So now, the question is; supposed, there are a number of point mutations in the oncogene that can do this between say, 1 and 10 or so. The point mutational rate is fairly well known approximately 10 to the minus 9 per base per cell division. So, given this point mutation rate, given the population size, we can fairly accurately estimate the probability that the resistant cells are already there before you started treatment.
Kat - So, by doing some maths, you can kind of figure out the rate at which these cells are mutating and evolving, and kind of track back to work out whether they were there at the start.
Martin - Yes, exactly. So, if you are telling me basically there are 10 possible point mutations, the population start is 10 to the 9, the point mutation is 10 to the minus 9 then there's some very high probability that we can conclude that the resistant mutations are already there by the time the doctor starts the treatment. So maybe 1 in a million cells has the resistant mutation and this is below clinical detection. So, if you examine the cancer, you would conclude that there's no resistant cell present because the frequency is so small. But then you start treatment and within approximately 20 to 30 weeks, you observe that the treatment fails. If you now look and analyse the genetic composition of the oncogene, you will find that the resistant mutations have emerged.
Kat - This seems to me to be incredibly significant for treatment because at the moment, with these targeted treatments, we tend to test one at a time. So, you do an analysis of a patient's tumour. You say, "Okay, you need this drug" and then you give it to them for a bit, it works and then it fails, and then you try another one. What conclusions can you draw from your research about how we should use these drugs now?
Martin - So, what we have done in this paper is really to ask the question, supposed that you are in a situation where you have two targeted therapies against the same cancer. If you now lose two therapies at the same time then what is the probability that the cancer is now cured. This really depends on whether or not there exist single point mutations in the genome that give simultaneous resistance to both drugs. So, if you are in a situation where there is even only a single point mutation in the whole genome that confers resistance to both drugs at the same time, the situation again is very gloomy and the chances for curing patients with this type of combination therapy are fairly small. So, what we really need to design are drugs that work against the same cancer and moreover, there's not a single point mutation in the genome that keeps rise to resistance to both drugs at the same time. Then the cancer has to respond by developing at least two-point mutations. One that gives resistance for drug A, one for drug B, and that is not so easy for the cancer.
Kat - Cancer cells only have a limited range of ways they can get around these drugs. They're not completely immortal so you would think that eventually, if we had enough targeted drugs, we would be able to have enough ways to hit cancer so it couldn't get round the treatment.
Martin - Yes, this would be the idea, but always keep in mind, it doesn't matter how many drugs you have, if the cancer cell has a mechanism to give resistance to all those drugs simultaneously. So, you really must develop drugs that do not have resistance mutations in common and here the surprising observation of our current study is that a single point mutation of the genome that would give you resistance to both drugs would defeat the treatment. The very important aspect is that whatever combination therapy you use, do not use it sequentially because to use first one drug and then wait until it fails, and then another drug is a certain recipie for complete treatment failure. To use two drugs simultaneously as opposed to sequentially is a much better idea and this is rare in the clinical practice of cancer treatment at the moment.
Kat - How quickly do you think you can get this message out to people who are treating cancer patients and for example, running clinical trials of these new targeted drugs? It seems like an incredibly important thing for doctors to know about.
Martin - Yes, I think it can happen quickly. I was involved in a similar study in 1995 for HIV virus and there, we actually were able to show that single drug therapy of the HIV virus gives rise to complete resistance in approximately 4 weeks depending on the drug because there's a very rapid turnover of the virus. This moved the field very quickly, I mean within in a year to combination therapy. I mean, for me, it's fascinating to see and to hope that mathematics can really help to inform experimental scientists and doctors in the clinic. And so, my hope would be that in a few decades from now, our understanding of cancer will be engineer-like and then we can really use an engineering-like approach to actually design and use the optimum therapies and prevent many, many people from dying from cancer.










Comments
Add a comment