Rheumatoid Arthritis
Interview with
There are many different types of arthritis and it can be caused by infection, trauma, autoimmune diseases, or just simple wear and tear with age. One of the more common forms is rheumatoid arthritis, but if you diagnose it early enough, it can be controlled well with drugs. Sadly rheumatologists often don't see these cases until a long time after the onset of symptoms. Speaking with Ben Valsler, Karim Raza, Senior Lecturer at Birmingham University, Consultant Rheumatologist at Sandwell and West Birmingham Hospitals explains...
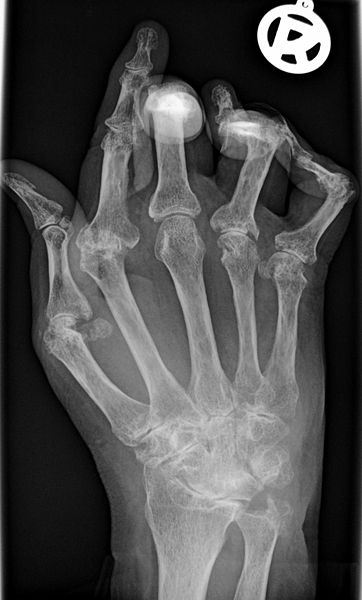 Karim - So rheumatoid arthritis is a common arthritis. It affects 1% of the population and is characterised by inflammation of the synovium. The synovium is a very thin layer of cells which lines most joints and it produces the synovial fluid, the lubricating fluid within the joint. In people with rheumatoid arthritis that synovium becomes inflamed and it becomes thickened. As a result of that people get pain, stiffness in the joints, and most importantly, that synovium actually eats into and destroys bone. So in the long term it causes damage and destruction to the joints which is irreversible actually once the destruction has happened, which is why it's important to catch people early before the damage sets in.
Karim - So rheumatoid arthritis is a common arthritis. It affects 1% of the population and is characterised by inflammation of the synovium. The synovium is a very thin layer of cells which lines most joints and it produces the synovial fluid, the lubricating fluid within the joint. In people with rheumatoid arthritis that synovium becomes inflamed and it becomes thickened. As a result of that people get pain, stiffness in the joints, and most importantly, that synovium actually eats into and destroys bone. So in the long term it causes damage and destruction to the joints which is irreversible actually once the destruction has happened, which is why it's important to catch people early before the damage sets in.
Ben - How does it affect quality of life? Obviously living with pain is not pleasant, but a lot of the time people find ways to cope. How does rheumatoid arthritis affect people's ability to work for example?
Karim - It has a huge impact on function. So within 5 years of a diagnosis of rheumatoid arthritis about 25% of people will have lost the jobs that they were in, and a proportion will clearly also be functioning less, and much less effectively in the jobs that they're in. So it does have a very big impact on function and quality of life.
Ben - What are our treatment options at the moment?
Karim - Treatment options that we have when we first see patients with rheumatoid arthritis are with drugs which modulate the immune system. So we want to dampen down the inflammation in the lining of the joint, and the most commonly used drug at our disposal is a drug called methotrexate. If you don't respond to methotrexate, we add in other oral drugs, and if you don't respond to those, which takes you down to about 10% to 20% of the rheumatoid population, then we have to move on to stronger drugs, which have been designed to specifically target particular components of the immune system.
Ben - Is it important to catch it as early as possible?
Karim - All the data that we have available suggests that the first 3 or 4 months after the onset of symptoms is a really critical time, and that if you can intervene at that stage you can really slow down the rate of progression of disease.
Ben - So what are the factors that are limiting early treatment at the moment?
Karim - One of the key factors that's limiting early treatment is the fact that we don't get to see our patients in our rheumatology clinics as early as we'd like. And if you think about what the determinants for delay are - say you develop inflammation in your joints - you'll spend a little bit of time deciding what to do about it and whether to go and see a General Practitioner. Then your GP will spend a bit of time deciding whether to refer you to the hospital, and then you'll get stuck on a hospital waiting list somewhere. So there are three levels of delay, and actually, when people have looked around UK at those three levels of delay, the main reason for delay in fact is delay on the part of the patient.
So if I told you that the average delay for a patient with rheumatoid was 6 months from when their symptoms began to when they saw a rheumatologist, if you break that down into this three components, three months tends to be delay on the part of the patient and the other 3 months is split between the delay on the part of the GP and the hospital. So the patient is accounting for the largest bit of it. And patients delay because they don't know anything about rheumatoid arthritis. They have no idea that it's a serious disease. They have no idea that there's treatment available for it. They have no idea that early treatment is important. In fact, when we've asked our patients, the vast majority have never even heard of rheumatoid arthritis.
Ben - So what should people look out for? How can they tell the difference between an ache or pain, or perhaps a bit of swelling because of minor trauma, and something that they do need to go and speak to their GP about?
Karim - So there are a number of key features in the story that we look for when we take a patient's history, and these are the kind of things that patients should be looking for. The first of them is morning stiffness. Often our patient is stiff for at least an hour in the mornings. They start easing up as they start using their joints, as they start doing things, but they're very, very stiff in the mornings. I'm not talking about the 2 or 3 minutes of morning stiffness which you probably all feel. When we're all out of bed, it takes us a few minutes to get going - I mean this is morning stiffness that lasts for at least an hour. The second thing is what joints are affected. So rheumatoid arthritis typically begins with the knuckles and the small joints of the fingers, the wrists, and the small joints of the toes. So patients may well notice pain, swelling, and stiffness in the hands, and in the feet. So it's the morning stiffness and the pattern in distribution of joint problems which are key features of new onset of rheumatoid arthritis. Anyone who has those should really be going to see their GP.
Dave - That was Karim Raza on the symptoms that suggest rheumatoid arthritis and how the biggest problem with catching it early, is actually the patients themselves.
Ben - And this is definitely worth thinking about because something else that Karim said to me off-mic was that having rheumatoid arthritis actually increases your risk of heart attack because chronic inflammation tends to lead to systemic problems. So if you do think you have those symptoms, if you do get stiffness for an hour in the morning, it's well worth going to see your GP.
- Previous Pi Time
- Next The Cultural Aspects of Sleep










Comments
Add a comment