Shape matters for Helicobacter infection
Interview with
Chris - Also in the news this week, researchers in Seattle have discovered that at least as far as gut bugs go, you have to be the right shape to be a success. We knew that size was important in some context. Shape now turns out to be equally so. The bacteria in question is Helicobacter pylori and this bacteria lives in our digestive system, and it's also been linked to the formation of stomach ulcers and stomach cancer. Now intriguingly, it has a very distinctive spiral shape which scientists have thought was what helped the bacteria to survive and also move around in the gut. The new research has now shown that the spiral bacteria definitely do a lot better than if we straighten them out and make mutant forms that don't have that spiral shape. And so this suggests there might be a clue there as to new ways that we can fend off this infection. And joining us to explain how they've discovered this, from the Fred Hutchinson Cancer Research Centre in Seattle is Dr. Nina Salama. Hello, Nina.
Nina - Hello.
 Chris - Welcome to the Naked Scientists. Tell us, if you would first of all, what is H. pylori in a little bit more detail than I went into and how does it cause disease?
Chris - Welcome to the Naked Scientists. Tell us, if you would first of all, what is H. pylori in a little bit more detail than I went into and how does it cause disease?
Nina - Well, Helicobacter pylori is a bacterium that lives in the stomach and when it was discovered in the early '80s by Barry Marshall and Robin Warren from Australia, their finding was pretty revolutionary because people thought that no bacteria lived in the stomach because of its high acidity. But these bacteria live in this very thick mucus that protects our stomach cells from the acid in the lumen and these scientists cultured them from patients with ulcers because as you say, this bacterium is associated with the development of ulcers. But it turns out that about half of the world carries this bacteria in their stomach and what it does is it causes inflammation. Most people survive with this inflammation and aren't bothered by it, but some people will get ulcers and then a smaller number of people can actually get gastric cancer, and Helicobacter pylori is the only bug at this point listed as a carcinogen by the World Health Organization.
Chris - So obviously, finding ways to make it less likely that a person will become colonised and carry the bug would be very, very helpful because it means that then there'd be less prospect of at least some people developing those stomach pathologies that you mentioned. But tell us about the shape of the bacterium.
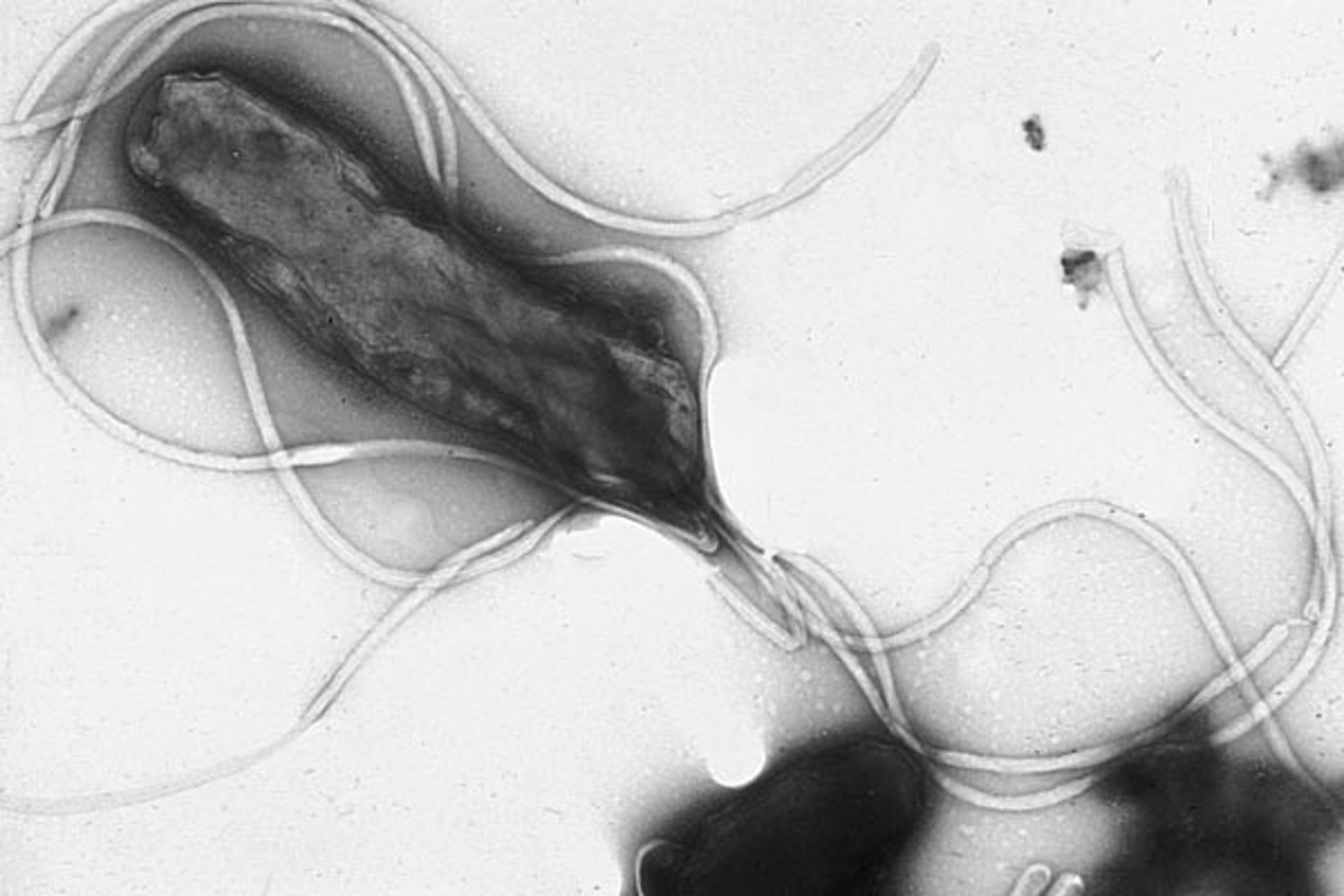
Nina - Well as you say, Helicobacter pylori, sort of evident in its name is a helical rod shape bacteria. It looks kind of like a spiral and what we wanted to ask was whether shape really was important for it to be able to colonise in its niche, the stomach mucosa. So, what we did was look for mutant forms of the bacteria; bacteria where individual genes had been inactivated that now had lost normal shape. And interestingly, we found quite a number of different bacteria inactivated in different genes, indicating that the bacteria have a whole program to enact this shape. So the study that we just published analysed four genes that seem to work together to make this normal helical shape by modifying the cell wall and basically taking this cage which wraps around the bacteria, and gives it its shape by making little snips in that cage to make it more flexible so that it can turn into this helix and have the appropriate twist and curvature to make the helical shape.
Chris - So the obvious thing to do is to identify what those genes are, then you can go in and deactivate them. What happens to bacteria if you switch off the genes that normally make them like a cork screw shape?
Nina - It's kind of interesting. If we grow them in the lab in broth, they are just fine being grown normally, they swim normally, and they appear to be no more sensitive to stresses like acid or some of the defence molecules that our bodies secrete to kill bacteria. They seem to be just fine. But if we take them now and try to infect them into the mouse stomach because that is the model that we use since we don't do experiments on humans. Now, these strains with an abnormal shape cannot colonise the stomach.
Chris - Do you know why?
Nina - That is a really good question. We don't know exactly why. So, the previous idea in the field was that it might help with motility - the ability of the bacteria to swim out of the acid part of stomach in the lumen, down into this mucus layer and next to the cells. But what we found is that they appear to swim normally, both in regular broth and in conditions where we make a gel-like matrix to mimic the thick mucus gel that overlies our stomach and we watched the bugs by live video microscopy. We basically can't find any differences in velocity. So now, we're left to try to figure this out. So the good news is that we have this animal model where we can see a difference in the way the bacteria colonise. And so now, we're trying to go in and look where the bacteria go, how that differs from the normal spiral shaped bacteria, and try to get to the bottom of it.
Chris - And finally, Nina presumably, because you found that these genes, if they're not working and you know how they work which is helpful, they seriously disable the bug. This presumably means you can now start to look for potential drugs that could target those genes and the things that those genes make because that might be a new way to treat or potentially disable them and decolonise people who are carrying H. pylori?
Nina - Yes. In fact, a very exciting thing about our findings, is that three of the four proteins that our work uncovered appear to have a very specific biochemical activity, and that they can cleave a peptide bond. And so, having an enzyme as it were, that's functioning in your process makes it a real possibility for screening for inhibitors of these enzymes that presumably then could render the bacteria unable to colonise. And another good thing is that these enzymes aren't found in human cells so that's the other trick when you try to develop a drug against bacteria. You want something that's specific to the bacterium but that's not going to hurt our own cells.
Chris - So you can make it highly selective. Nina, thank you very much. We have to leave it there. Dr. Nina Salama from the Fred Hutchinson Cancer Research Centre in Seattle. She's published that work this week in the journal Cell.
- Previous Ready, Steady, Stop!
- Next RHS Chelsea Flower Show 2010










Comments
Add a comment