Most people have heard of Shakespeare's 'Romeo and Juliet', and the majority know that it is a tragedy based on a love story, but you could probably be forgiven for missing the subtle reference it contains to one of mankind's most common infections:
O'er ladies ' lips, who straight on kisses dream,
Which oft the angry Mab with blisters plagues,
Because their breaths with sweetmeats tainted are:
Act 1. Scene IV
The blisters that Shakespeare refers to are in fact cold sores produced by the herpes simplex virus (HSV) which comes in 2 types, HSV-1 and HSV-2. Type 1 herpes is carried by over 80% of the population; it's the culprit responsible for causing recurrent cold sores, and most people pick it up in the first few years of life, usually in the form of a loving kiss from a parent or sibling. HSV-2, on the other hand, affects between 5 and 10% of the population (including many individuals who are also infected with HSV-1), and is more often associated with genital herpes, although either virus can cause a similar disease at both anatomical sites.
Part of the reason that herpes infections are so common, and so easy to transmit, is that up to 30% of people previously infected with HSV go on to periodically shed the virus in their saliva or genital secretions (depending upon the site of infection) without suffering any symptoms. These individuals are known as 'asymptomatic shedders' and can transmit the infection to other susceptible individuals but without showing any obvious signs of the disease themselves.
 Shedding, and recurrent lesions, occur because once a person is infected with herpes they carry the virus for life. This is because HSV has evolved a clever strategy, called latency, that enables it to escape from the immune system by hiding inside nerve cells. Then, in about 15% of people carrying it, the virus periodically reawakens producing recurrent, painful, infectious sores on the affected part of the body.
Shedding, and recurrent lesions, occur because once a person is infected with herpes they carry the virus for life. This is because HSV has evolved a clever strategy, called latency, that enables it to escape from the immune system by hiding inside nerve cells. Then, in about 15% of people carrying it, the virus periodically reawakens producing recurrent, painful, infectious sores on the affected part of the body.
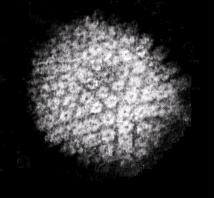
The herpes virus itself (left) consists of a tiny particle one five-thousandth of a millimetre across. It's so small that 100 million of them could fit on a pinhead. Each particle consists of a core, containing the viral DNA, wrapped in a protein-studded coat known as the envelope. These proteins are the viral equivalent of velcro and help HSV to lock on to, and invade, its target cells. Viruses are the ultimate parasite and comprise little more than infectious packets of genes. To reproduce they hijack healthy cells and turn them into viral production lines that churn out millions of new viral particles, which is how the infection spreads.
WHAT HAPPENS WHEN YOU ARE FIRST INFECTED WITH HSV ?
The first time someone encounters HSV, known as primary infection, they don't develop a classic cold sore like lesion, which is why many people often don't realise that they have been infected. Instead, most cases of primary herpes affecting the face present with a nasty sore throat, a sore mouth (which can occasionally ulcerate), swollen neck glands, and a temperature. Similarly, primary infection in the genital region usually produces a painful, red, ulcerating crop of lesions that can spread over a wide area and may involve the perineum and anus. Genital infection can also be associated with temporary numbness in the affected area, swollen glands in the groin, difficulty passing urine, and a temperature. Occasionally, primary infections such as these can also trigger viral meningitis.
WHY HSV INFECTION LASTS A LIFETIME
As HSV spreads through infected tissues it also penetrates nerve fibres which inadvertently provide the virus with the neurological equivalent of a getaway car. Indeed, as the immune system moves in to control the infection, the virus conceals itself within nerve cells and slips away from the scene by hitching a ride on a special transport system that nerves use to move materials from one end to the other.
In this way the virus is carried to the nerve 'cell body' in a swelling called a ganglion located close to the spinal cord. In the case of infection on the mouth or face this ganglion is known as the trigeminal ganglion, and in the case of genital herpes the 'sacral' ganglia are involved. When it reaches the cell body, the viral DNA is added alongside the nerve cell's own DNA in the nucleus. It remains there, hidden within the nerve cell and in an inactive state, for the lifetime of the infected individual. The purpose of this process is to provide a reservoir of virus within the body which can periodically be 'reactivated' to spread the infection to other susceptible individuals.
 SO WHAT CAUSES YOU TO DEVELOP A COLDSORE ?
SO WHAT CAUSES YOU TO DEVELOP A COLDSORE ?
A number of things can trigger the virus to reactivate including being stressed or run down, menstruation, drugs that suppress the immune system, and skin damage including burns caused by the sun, heat, or chemicals.
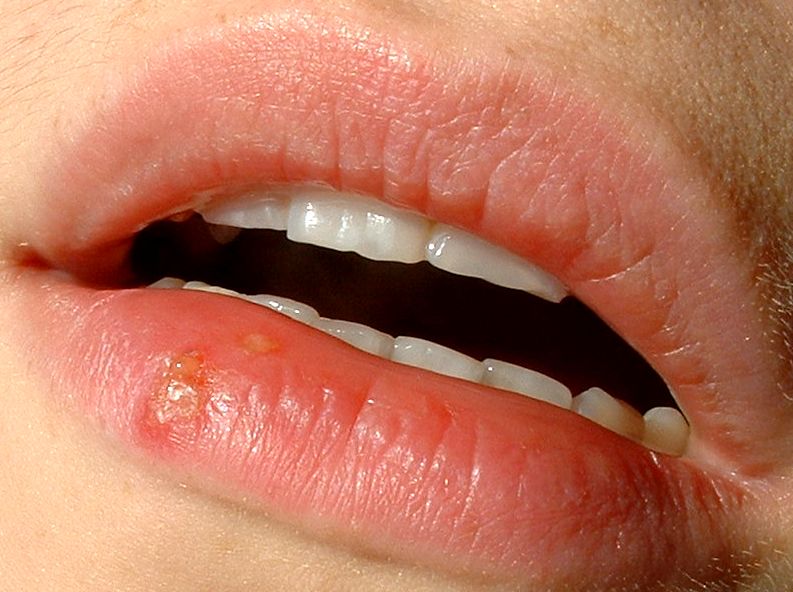
In some way these 'stimuli' reawaken the virus and it begins to make new particles from the recipe stored in the viral DNA hidden in the nerve cell. These newly-assembled viral particles are then shipped back down the nerve fibre to the region of the skin that it supplies - for instance around the lips. The virus 'buds off' from the nerve ending and infects the surrounding epithelial (skin) cells, producing a painful cluster of pale blisters which are crammed with herpes simplex virus and highly infectious.
When this process first begins to happen, and before the blisters appear, most people notice a mild tingling sensation on the patch of skin supplied by the affected nerve cell. Soon after they form the blisters break open, releasing their infectious cargo, leaving a red raw patch - the cold sore - which measures about half a centimetre across and takes about 7 to 10 days to heal up.
How often the virus reactivates varies from one person to the next but, as a general rule, recurrences tend to occur most often during the year following infection, and then they tail off.
Significantly, cold sores and genital lesions remain infectious until they have crusted over, so contact should be avoided during this time because the virus can be transmitted to other parts of the body, and to other people, especially between the mouth and the genitals. Cold sores and genital lesions also create a breach in the skin's natural defences, producing portals of entry for other infections, like HIV, so extra care should be taken to minimise the risk of any exposure.
Between 5-20% of the population of western countries are affected by genital herpes, and the prevalence is increasing, making this one of the commonest sexually transmitted infections. Traditionally, most genital infections were caused by HSV-2, but more recently there has been a large increase in the number of cases caused by HSV-1, mainly due to changing sexual practices, and particularly oral sex.
COMPLICATIONS OF HERPES INFECTION
Apart from cold sores and genital disease, herpes simplex viruses can also cause more serious infections, although fortunately these are relatively rare.
The most important are HSV meningitis (a form of aseptic meningitis), HSV encephalitis (HSV infection of the brain), neonatal herpes (HSV infection in the newborn acquired from the mother around the time of birth), corneal ulceration, scarring, and visual impairment following eye infection, and more severe generalised infections amongst those with weakened immunity. Such patients include people with HIV, and those on immunosuppressive drugs (for instance transplant patients), who tend to suffer worse recurrent disease, and are also more likely to develop drug-resistant forms of the virus.
DIAGNOSIS
Herpes affecting the face (orolabial herpes) is usually diagnosed clinically - that is, the diagnosis is made solely on the basis of the symptoms. But in the case of suspected genital herpes, HSV affecting the eyes, or more severe skin outbreaks, it can be useful to confirm the diagnosis by means of a variety of laboratory tests which are outlined below.
Traditionally, herpes infection is confirmed by taking a swab from an active lesion, growing the virus in the laboratory, and then using colour-coded antibodies to pinpoint whether HSV-1 or HSV-2 is the culprit. This method can be useful in confirming the presence of asymptomatic shedding of the virus.
Another way, which is faster but yields less information, is to use an electron microscope to look for viral particles in fluid collected from the blisters.
More recently, however, many laboratories have moved to using a highly accurate DNA test which can rapidly pick up the presence of the virus in a sample, and at the same time tell whether it is HSV-1 or HSV-2. This approach is particularly useful in the diagnosis of viral meningitis, or encephalitis, caused by herpes infection. In these instances a sample of cerebrospinal fluid (CSF), the watery substance that bathes the brain and spinal cord, is collected by lumbar puncture, and analysed.
Doctors also sometimes take a blood sample, particularly in people with a history of possible herpes infection but no active lesions, in order to look for herpes antibodies. The benefit of this kind of blood test is limited, but it can sometimes be used to confirm whether a patient has been infected with herpes previously, and which type of virus they are carrying.
MANAGEMENT
Herpes causes a lifelong infection and there are currently no treatments capable of removing the viral DNA from the nerve cells that carry it. This means that treatment focuses on reducing the intensity of a primary infection, and the frequency and severity of subsequent viral reactivations.
COLD SORES
Prevention :
If you are prone to cold sores try to avoid the things that trigger recurrences - - When skiing or sunbathing use high-factor sun creams to avoid sunburn.
- Try to avoid becoming run down.
- Eat a healthy diet including plenty of fresh fruit and vegetables.
Treatment :
Uncomplicated orofacial herpes (cold cores) responds well to topical aciclovir cream (Zovirax), which is available over the counter. It is extremely safe (including during pregnancy) and can reduce the duration and severity of a recurrence. It should be applied as soon as the tell-tale symptoms heralding a cold sore appear. Warning signs usually include localised pain, or a tingling sensation on the lip. But remember, cold sores remain infectious until they have crusted over.
GENITAL HERPES
Genital infection with HSV also places partners and babies at risk, meaning that appropriate counselling, contact tracing, and exclusion of other co-existent infections play an important part in the management of this condition. For this reason, patients with genital herpes should be referred to a genitourinary (GU) medicine clinic for appropriate investigation and follow up. With any sexually transmitted disease it is always important to exclude the presence of other infections which may have been picked up at the same time as HSV, especially chlamydia which is very common, highly infectious, often symptom-free, and (left untreated) can lead to infertility.
Prevention :
- Always use barrier methods of contraception (e.g. a condom).
- If you have a partner with known genital herpes, try to avoid intercourse whenever they experience a recurrence.
- Avoid oral sex when you, or your partner, have a cold sore - the virus is readily transmitted from the mouth to the genital area, and vice versa.
- Like cold sores, genital lesions remain infectious until they have crusted over.
Treatment :
Initial (primary) infection with genital herpes can be extremely painful and very distressing, but prompt presentation to a doctor can help through the administration of antiviral drugs, and pain relief.
General measures to reduce discomfort :
- Bathing with saline - soaking the affected area in salt water can reduce pain.
- Analgesia - simple painkillers such as paracetamol provide effective relief.
- Topical anaesthetics - these can be very effective but should be used carefully owing to the risk of potential sensitisation to the agent.
ANTIVIRAL DRUGS
The drugs aciclovir, valaciclovir and famciclovir have all been shown to be effective at reducing the severity and duration of infection and, in general, they are more effective the earlier they are started. Ideally they should be introduced within 5 days of the start of the episode and continued for at least 5 days, or while new lesions are forming, whichever is the longer. On the grounds of cost, oral aciclovir is usually the drug of choice.
These antiviral drugs work by blocking the ability of the virus to copy its DNA, preventing it from growing. The agents themselves are active only in virally-infected cells, so healthy cells are not affected.
The drug molecules resemble one of the building blocks used to make new DNA but, critically, they lack a certain chemical group which is required for a DNA chain to continue growing. So when the virus inserts one of these drug molecules into its DNA, the DNA chain is prematurely terminated, stopping the virus from growing.
In general, oral agents are extremely well tolerated, have few side effects, and are more effective than topical agents. Trials have also shown that combining oral and topical medications is no better than oral medication alone.
IMMUNOCOMPROMISED PATIENTS
Patients with HIV, or other immune-disabling conditions such as organ-transplant recipients, are at increased risk of developing severe (and sometimes life-threatening) infections. They should receive prompt antiviral therapy which should be continued until fresh lesions have stopped appearing, and the existing lesions have crusted over. Lesions which are not responsive to therapy might be due to drug-resistant forms of herpes. Under these circumstances it may be necessary to switch to another class of antiviral drugs, and to collect samples of the virus for drug susceptibility testing.
RECURRENT GENITAL HERPES
Most HSV recurrences occur in the year following infection, and then the frequency of reactivation tends to tail off. But for some patients recurrences remain a problem and they may require regular use of antiviral agents.
For patients with infrequent herpes reactivations the condition can be controlled effectively by using oral antiviral medications, chiefly aciclovir, whenever they experience a recurrence. When used in this way, known as episodic therapy, antivirals have been shown to reduce the duration of symptoms by 1-2 days, and the clinical severity of the outbreak.
But patients with more frequent recurrences (6 or more per year) often benefit instead from 'suppressive therapy', which means taking antiviral medications every day to prevent the virus from producing clinical symptoms. In other words, whenever it tries to reactivate, the virus is immediately switched off by the antiviral agent. Again, aciclovir, valaciclovir, and famciclovir have all been shown to be effective at preventing recurrences, but this course of action must be balanced against the inconvenience and costs of taking regular medication. Again, on cost-grounds, aciclovir is usually the agent on choice.
Most doctors advise stopping suppressive therapy after a year in order to re-assess the activity of the disease, and to reduce the risk of developing viral resistance to the antiviral drugs. Because the clinical course of the condition varies between patients, treatment is tailored to the requirements of the individual, and based upon the severity and frequency of their symptoms.
GENITAL HERPES IN PREGNANCY
Genital herpes can be dangerous for the newborn, but the risks can be minimised by careful medical management. All women who develop new genital herpes during pregnancy should be referred to the genitourinary medicine clinic in order to exclude the possibility of other infections, and for advice on treatment. Aciclovir has been used extensively during pregnancy, it is well tolerated, and in over 20 years of use there have never been any reports of foetal toxicity or birth defects. It is not contraindicated in cases of primary genital herpes occurring during pregnancy.
All women with first-episode genital herpes lesions at the time of delivery are advised to deliver by caesarian section because the risk of transmitting the infection to the newborn under these circumstances is 40%. But caesarian is not recommended for women who contract HSV during the first or second trimesters, or for women with a past history of genital herpes but without any signs of recurrence, because the local infection will have cleared by the time of delivery, and protective antibodies will have been produced against the virus. These antibodies will be passed to the developing baby before it is born, greatly reducing the risk of transmission. The baby should, however, be monitored closely when it is first born for any signs that it may have picked up the infection, in which case treatment with intravenous aciclovir should be started immediately.
EYE INFECTIONS
Herpes infection involving the eye usually presents as single, sore, red eye which is extremely sensitive to the light. Often the virus attacks the cornea producing a dendritic ulcer which doctors can see by adding some coloured drops and examining the eye with a slit lamp. If these ulcers are allowed to recur (like the ocular equivalent of recurrent cold sores) they can lead to corneal scarring, opacity, and blindness. They should be treated aggressively with pain relief and aciclovir (or a topical equivalent), which can also be used to prevent recurrent lesions.
MENINGITIS AND ENCEPHALITIS
HSV can occasionally trigger aseptic (viral) meningitis. Patients usually complain of a severe headache, neck stiffness, nausea, fever, and a dislike of bright lights. Unlike meningitis caused by a bacterial infection there is usually no skin rash. Anyone with these symptoms should see a doctor urgently. Cases of HSV meningitis usually resolve rapidly with intravenous aciclovir therapy, and without long term consequences.
A very rare manifestation of HSV is encephalitis in which the brain tissue itself becomes infected by the virus. There are very few warning signs, but patients with encephalitis tend to become confused and drowsy. Without prompt treatment with intravenous antivirals (usually aciclovir) the condition is often fatal, and even when treated rapidly often causes long term neurological problems including memory loss and epilepsy.
ON THE HORIZON
Scientists are currently trying to identify the chemical signals responsible for providing the wake up call which causes the latent (inactive) viral DNA to reactivate and produce recurrent disease. Pinpointing these cellular messengers, or the means that the virus uses to detect them, would provide scientists and drug manufacturers with new targets to aim at in their search for novel antiviral agents capable of preventing reactivation, shedding and transmission of herpes infections.
But with no solution presently on the horizon, we will just have to cross our fingers, and possibly our legs, and hope that the answer is not too far away.










Comments
Add a comment