Any old bacteria won't do: to be healthy, an animal requires a unique 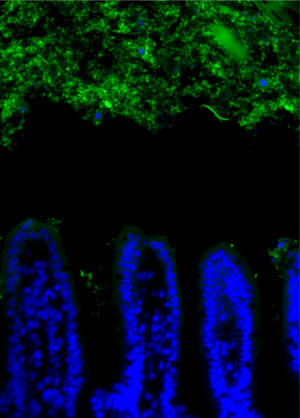 consortium of microbes in its intestines, US scientists have revealed.
consortium of microbes in its intestines, US scientists have revealed.
It's been known for some time that mice raised in a sterile environment, meaning that their intestines remain uncolonised by microorganisms, are paradoxically less healthy than equivalent animals reared in a natural, germ-laden environment.
Some species even depend absolutely upon microbial colonisation in order to develop and reproduce at all. Without the help of the cholera-relative Vibrio fischeri, certain tissues don't develop in squid, for instance, and tsetse flies that fail to team up with the bacterium Wrigglesworthia glossindia lack key vitamins required for fertility.
These and other observations have led to the formulation of the human "hygiene hypothesis", which holds that rising rates of allergy and autoimmune diseases amongst western populations reflect an obsession with sterility and a failure to engage effectively with the microbial world. This, scientists say, hampers the development of the immune system, putting people into a pro-allergic state.
But now, new research presented this week in the journal Cell by Harvard scientist Dennis Kasper and his colleagues suggest that just mere exposure to a microbial milieu isn't sufficient. Instead, what organisms require is colonisaton by a unique collection of highly-specific microorganisms unique to a given species.
The team made the discovery by colonising initially germ-free mice with either normal mouse or human intestinal microbes. A third group of animals were left uncolonised as controls.
Both colonised groups developed similar levels of bacterial loads in their guts, the team found. But when they compared the immune systems of the two, the animals colonised with human flora had fewer white cells known as lymphocytes in their small intestines, they secreted lower levels of defensive antibodies and proteins, and they had fewer immune presenting "dendritic" cells in the gut lining.
And compared with the animals colonised with normal mouse bacteria, those carrying human microbial flora were also highly vulnerable to Salmonella enterica infection. In fact, the human-bug colonised animals were equivalently unhealthy and as vulnerable as the germ-free uncolonised mice.
As Hachung Chung, one of the research team puts it, "Despite the abundant and complex community of bacteria that were in the human flora mice, it seemed like the mouse host did not recognise the bacteria."
The interaction also appears to be highly specific since repeating the experiment even with rat, rather than human, bacteria produced the same result, suggesting that millions of years of co-existence between microbes and hosts has produced animals pre-programmed to depend upon the presence of certain bugs for the immune systems to develop and function normally.
"This raises serious questions regarding our current overuse of antibiotics, as well as ultra-hygienic environments that many of us live in," says Dennis Kasper. "If the bacteria within us is specific to us and necessary for normal immune system function, then it's important to know if we are in fact losing these vital bacteria. If that is the case, then this is yet further evidence that the loss of the good bacteria is partly to blame for the increased rates of autoimmunity that we are now seeing."










Comments
Add a comment