A drug that can block the process in the brain that leads to Alzheimer's has been uncovered by UK scientists. 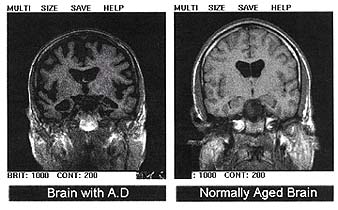
Alzheimer's Disease, which progressively robs sufferers of their mental faculties and independence, currently affects about 44 million people worldwide.
The effects of a rapidly ageing population, however, mean that by 2050 that number will have tripled. And in some countries more than one third of the elderly population will be diagnosed with the disease.
The disease is caused by the build-up in the brain of harmful aggregates of a protein called beta-amyloid, which is toxic to nerve cells.
Beta amyloid is a breakdown product of a larger chemical known as beta-APP, the role in the brain for which is currently not known, but it appears to be produced in increased amounts in response to brain injury and biochemical stress.
Treatments for Alzheimer's tried so far largely aim to tackle the symptoms of the disease, which chiefly include memory and cognitive problems. have included using the immune system.
Now scientists at Cambridge University have developed a technique to enable them to discover promising drug candidates that may be able to prevent the disease occurring in the first place.
Likening their approach to the use of statin medicines that reduce blood cholesterol and thereby cut stroke and heart attack risk, Michele Vendruscolo and his colleagues went looking for "neurostatins" that could stop beta-amyloid forming in the first place.
Their approach was highly novel. They began with a collection of 88 molecules that they knew would interact with beta-amyloid. From their 88 molecules, they identified 164 fragments or regions of the molecules that might be responsible for the interaction.
They then mined a chemical database extracting molecules known to contain one of the 164 fragments they had identified. Of the 16850 hits they achieved, 386 were drug molecules already approved for human use by licensing agencies.
As a proof of principal they selected two of these agents, one an anti-cancer agent called bexarotene and another called tamiprosate, for further characterisation using a test they have built in the lab to follow how beta-amyloid plaques are formed.
Their in-vitro test uses a fluorescent marker that binds as the amyloid aggregates begin to assemble, enabling the team to quantify how much beta-amyloid is forming, at what rate and whether or not a drug is affecting the process.
Tests on cultured cells showed that tamipirosate, of the drugs selected for testing, was not functional, but bexarotene appeared to be highly potent. The fluorescent test showed that it appears to bind to the smallest clusters of beta-amyloid and prevents them from building up further or promoting the formation of further amyloid aggregates.
Given next to microscopic worms called C. elegans, which have been programmed to develop an Alzheimer's-like condition, bexarotene treatment prevented the worms developing the same neurological abormalities that were rapidly manifest within the untreated animals.
The researchers acknowledged that, while bexarotene is unlikely be helpful in the reversal of established Alzheimer's symptoms, the discovery, published this week in Science Translational Medicine, could usher in an era of preventative management instead whereby drugs like bexarotene, uncovered using the technique announced by the Cambridge researchers, block the development of the disease in vulnerable populations.
"You wouldn't give statins to someone who had just had a heart attack, and we doubt that giving a neurostatin to an Alzheimer's patient who could no longer recognise a family member would be very helpful," said study co-author Chris Dobson. "But if it reduces the risk of the initial step in the process, then it has a serious prospect of being an effective preventive treatment."










Comments
Add a comment