Scar tissue in injured hearts can be converted back into healthy cardiac muscle using gene therapy, US scientists have shown.
Following a heart attack, some of the muscle tissue that 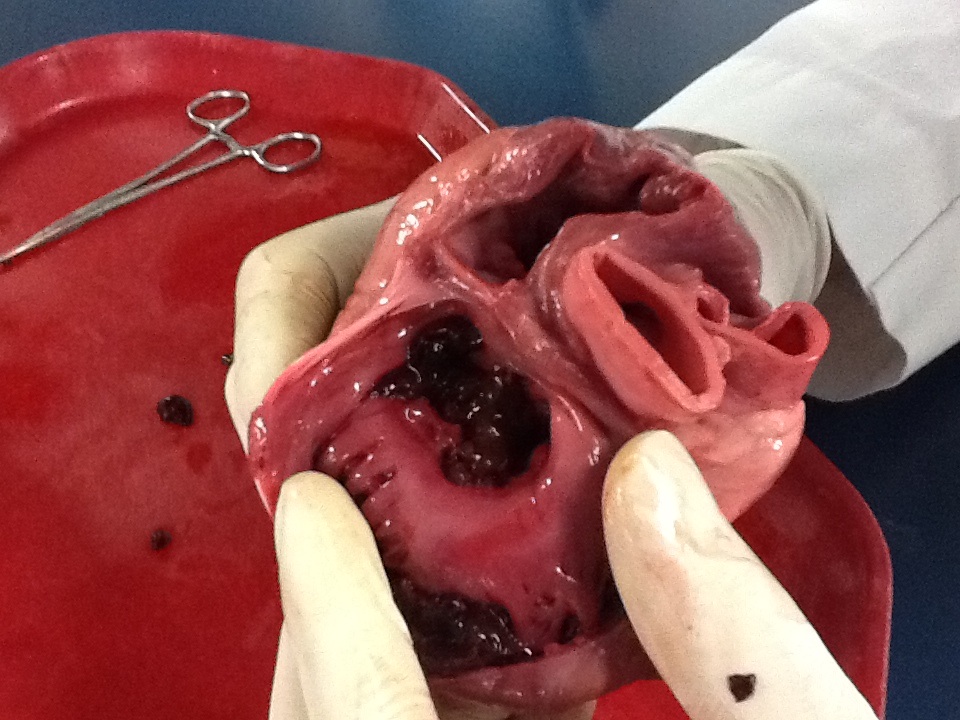 generates the pumping action needed to push blood around the body is replaced by an immobile fibrous scar.
generates the pumping action needed to push blood around the body is replaced by an immobile fibrous scar.
If it's sufficiently extensive this can compromise the function of the heart, causing heart failure. The scarred areas may also affect the way that the electrical signals that coordinate the heartbeat travel through the tissue, triggering abnormal rhythms and even cardiac arrest. And because heart muscle doesn't naturally replace itself after an injury, these consequences were thought to be permanent.
Now, writing in Nature, Deepak Srivastava and his colleagues at the Gladstone Institute of Cardiovascular Disease in San Francisco may have found a way to convert the fibroblast cells that form scar tissue back into beating heart cells, in-situ.
The discovery hinges on three genes called Gata4, Mef2c and Tbx5; these are known as "GMT" and have been shown previously to operate during the embryonic development of the heart to direct the formation of heart muscle cells known as cardiomyocytes.
By engineering these genes into disabled viruses, which were then injected into the damage parts of the hearts of experimental mice that had had recent heart attacks, the team successfully reduced the sizes of the scars that subsequently formed in the animals' hearts and demonstrated that, compared with controls, the animals had improved cardiac function as a result.
A dose of about 100 million virus particles was able to hit about 300,000 cells, converting about 12% of them into new cardiomyocytes. And because the technique labelled-up the newly-re-programmed cells, the scientists were able to confirm their origins and test their function.
The cells wired themselves apropriately to adjacent cells and contracted when electrically activated. They also had the correct appearance, genetic and biochemical profiles.
In their paper the team conclude, "The ability to regenerate adult heart tissue from endogenous cells is a promising approach to treating cardiac disease that may face fewer obstacles to clinical translation than other approaches..."










Comments
Add a comment