A new diagnostic technique is enabling scientists to listen to red blood cells for signs of disease.
By firing a high frequency laser at a sample of 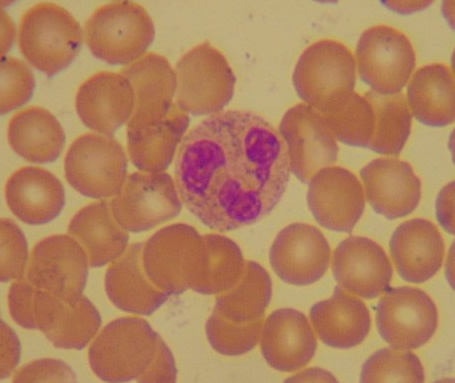 blood cells and measuring the frequency of the sound waves emitted, Ryerson University researcher Eric Strohm and his colleagues can construct a 3D map of the cell with hundredth of a millimetre resolution.
blood cells and measuring the frequency of the sound waves emitted, Ryerson University researcher Eric Strohm and his colleagues can construct a 3D map of the cell with hundredth of a millimetre resolution.
The pulses of laser energy momentarily heat the cell, causing it to swell slightly, and then contract again as it cools. As the cell relaxes, sound waves are produced, which are picked up by ultrasound detectors.
Repeated from various angles, the information generated is fed in to a computer, which builds a model of the red blood cells in the sample.
Dubbed photoacoustics, this technique is already used across a wide range of scientific areas including finding tumours: their blood-rich capillary networks are the giveaway, and, in the 1980s, by making use of the fact that nitric oxide resonates at different frequencies depending on the concentration, to prove that nitric oxide levels in the upper atmosphere were changing.
But, these applications used lower resolution photoacoustics, capable of giving only a rough overview of the surroundings. The high resolution delivered by the new technique is possible because the laser beam is very focused, delivering strong, short pulses of energy at very high frequencies of greater than 100 MHz.
Previously, the exact shape of an individual red blood cell had been worked out using light-scattering methods, electrical impedance - where a current is passed though the cell and its shape is determined by how much resistance is observed - or from looking at a sample of blood on a slide.
The most marked difference between these former techniques and Strohm's new approach is the cost. Once the equipment is set up, the running cost is relatively low. It also takes less time, the shape of the cell can be read in more detail and only a tiny sample containing as few as 21 red blood cells, is needed.
In theory, this could be used as a quick diagnostic test for blood disorders, which are frequently characterised by misshapen red blood cells. Malaria leads to swollen, almost spherical cells, while sickle cell anaemia gives rise to stretched "sickled" cells, and porphyrias can produce large or oddly-shaped red blood cells. The technique could even hunt out circulating tumour cells, enabling doctors to predict the likelihood that a cancer has spread.
According to Strohm, "we're currently developing a flow device where cells could be streamed through a target area rapidly, enabling measurements of thousands of cells in a short amount of time. We're also applying similar methods to detect circulating tumor cells in the bloodstream..."
- Previous Liver grown from stem cells
- Next Keeping an eye on diabetes










Comments
Add a comment