In this NewsFlash, we'll hear how disguising cancer cells as salmonella could hold the key to producing anti-cancer vaccines, explore a link between the Y-chromosome and heart disease, and discover a new drug that can knock the cause of Alzheimer's on the head. Plus, a new Olympic effort to get school children to understand exercise and the body...
In this episode
00:17 - Y Chromosome yields heart disease clues
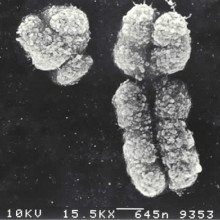
Y Chromosome yields heart disease clues
Although deaths from heart disease are falling, it's still a major killer. And men are more likely to suffer coronary heart disease than women of the same age. This has often been put down to chaps having unhealthier lifestyles, but an international team by scientists in Leicester has just published a paper in the Lancet showing that there may actually be a genetic component at work.
Although men and women share almost all the same genes, there's one important difference. Women have two X chromosomes, while men have an X and a Y. There are only a handful of genes on the Y chromosome, making a grand total of around 27 proteins, and most of these are thought to be important for sexual development and making men manly.
 But in recent years, there have been some intriguing links made between this tiny genetic estate and diseases including HIV and autism. So the scientists decided to analyse the genetic makeup of the Y chromosome in more than 3000 British men involved in three different heart disease studies.
But in recent years, there have been some intriguing links made between this tiny genetic estate and diseases including HIV and autism. So the scientists decided to analyse the genetic makeup of the Y chromosome in more than 3000 British men involved in three different heart disease studies.
Because Y chromosomes are passed down almost whole from fathers to sons, with little genetic muddling from generation to generation, there are only a limited number of different 'flavours', or haplogroups of Y chromosomes. Because of this, the Y chromosome is often left out of most large-scale genetic studies looking for links between gene variations and diseases.
In this case, the researchers found that all the men fell into just 9 haplogroups, and 90 per cent of the Y chromosomes came from only two different haplogroups. And when they looked at their history of heart disease, they found that men with Y chromosomes from one particular haplogroup had a 50 per cent increased risk of developing coronary heart disease than men whose Y chromosome came from the other haplogroups.
After a bit more digging, the researchers confirmed that this association wasn't linked to other risk factors for heart disease, such as lifestyle factors like drinking and smoking or other known biological risk factors. And when they looked closer at the activity patterns of genes in men from different haplogroups, they found clear differences between those from the high risk group and the other groups in the activity levels of certain genes involved in inflammation and autoimmune responses, both of which are thought to play an important role in heart disease.
At the moment this is still just an association - although it's the first study to robustly uncover an association between heart disease and the Y chromosome - and a lot more work needs to be done to confirm this finding and figure out exactly how the genes on the Y chromosome are having these effects. But in the future it might help to lead to new ways to reduce the risk of heart disease in men, or even potentially treat the disease. And because the Y chromosome is passed down wholesale from father to son, it also tells us that in some cases, susceptibility to heart disease may be handed down the generations in this way.
03:49 - Feed a cold, starve a cancer
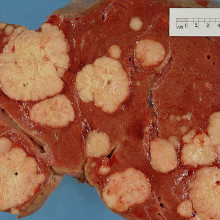
Feed a cold, starve a cancer
A self-inflicted fast might double the effectiveness of anticancer treatments, new research has shown.
Writing in the journal Science Translational Medicine, University of Southern California scientist Valter Longo and his colleagues have shown both using cells cultured in the dish and also in experimental mice that fasting sensitises cancers to chemotherapy drugs.
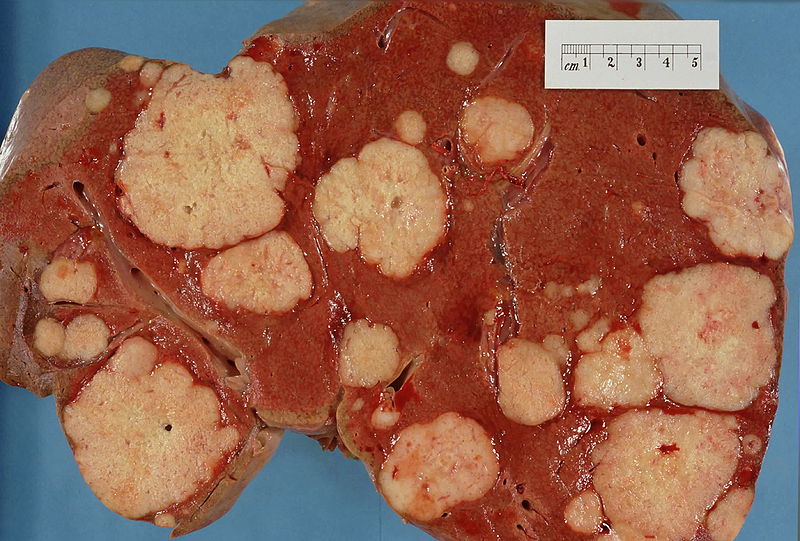 Initially using yeast cells genetically programmed to carry a genetic mutation that causes cancer in humans, the team found that starving the cells by replacing their culture media for 48 hours with water devoid of any nutrients triggered severe stress and increased the rate of cell death. Cells lacking the cancer-causing gene and subjected to the same treatment, however, were paradoxically much more resistant to the insult and were less sensitive to toxic chemicals like hydrogen peroxide. The researchers then grew cancer cells in growth medium made from the blood plasma of mice that were either fasting or fed normally.
Initially using yeast cells genetically programmed to carry a genetic mutation that causes cancer in humans, the team found that starving the cells by replacing their culture media for 48 hours with water devoid of any nutrients triggered severe stress and increased the rate of cell death. Cells lacking the cancer-causing gene and subjected to the same treatment, however, were paradoxically much more resistant to the insult and were less sensitive to toxic chemicals like hydrogen peroxide. The researchers then grew cancer cells in growth medium made from the blood plasma of mice that were either fasting or fed normally.
As expected, cells grown in the fasting mouse medium showed greater signs of stress, higher rates of death and were more susceptible to anti-cancer drugs than their normally-nourished counterparts. To find out whether this effect would translate from the dish to a real case of cancer, the researchers then treated mice carrying a range of tumour types including melanomas, gliomas (brain tumours) and breast cancers.
Mice that were fasted before receiving chemotherapy, they found, had a 40% reduction in the rates of cancer spread and a 42% long-term survival rate compared with 100% mortality in the normally-fed animals.
The mechanism underlying this extraordinary observation, the team believe, is that the very same processes that make cancer cells grow uncontrollably also prevent the cells from shutting down their activity and protecting themselves in the face of stress, including stress induced by fasting. And in this state the cells become much more vulnerable to chemotherapy drugs compared with healthy tissue. This, the researchers suggest, could be a way to boost anti-cancer effects in humans while simultaneously minimising side effects.
06:05 - Disguising Cancer as Salmonella
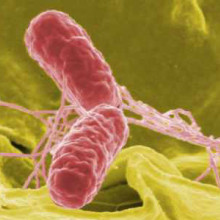
Disguising Cancer as Salmonella
Professor Julie Magarian Blander, Mount Sinai Hospital
Chris - Making cancer cells resemble the Salmonella bacterium might sound like an odd thing to, but oddly enough, it could hold the key to creating anti-cancer vaccines which trigger the immune system to actually attack cancers. And to explain how, we're joined by Professor Julie Magarian Blander from the Mt. Sinai School of Medicine in New York. Hello, Julie.
Julie - Hello.
Chris - So first of all, why doesn't the immune system attack cancer in the first place?
Julie - The immune system recognises its own tissues by a process called pattern recognition. So when it's searching for microbes, it's really searching for patterns that are associated with microorganisms and these patterns are absent from normal healthy tissues. Therefore, because tumour cells and cancerous cells are derived from normal cells, they don't have those microbial patterns that the immune system likes to see and target.
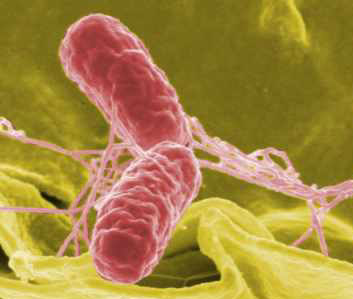 Chris - So that's why they escape normal surveillance. So what were you doing with Salmonella?
Chris - So that's why they escape normal surveillance. So what were you doing with Salmonella?
Julie - With Salmonella there is this protein called flagellin which Salmonella and other bacteria actually use for locomotion and therefore, we took this protein - the sequence of this protein - it's easy to express in cells because it's a protein in nature. We expressed it in tumour cells in order to make them look more microbial to the immune system. By doing so, we could target the receptors that recognise these patterns or structures that are associated specifically with microbes. In this way, you are tricking the immune system to think that tumour cells actually have a component that's derived from microbes and then they're targeted this way.
Chris - So the cells are made to look more like a bacterium. This gets the interest of the immune system via these special receptors it has to pick up pathogens. The immune system then attacks the tumour cells. That's all very well for the tumour cells that you have added the Salmonella-like gene to it, but what about the tumours elsewhere around the body?
Julie - So, in animal models, in mice, the strategy is to take the tumour cell itself, introduce this flagellin protein in order to target the receptors of the immune system and then irradiate the tumour cell and use that as a whole cell cancer vaccine. We have done two different sets of experiments where animals that do not have tumours have been vaccinated and then we tested their protection against subsequent challenge from a wild-type tumour that does not express the flagellin. We've also done experiments where animals that bear tumour already were vaccinated and then we monitored the immune response. In both cases, we were able to see that the immune system efficiently mounts a robust immune response - both the CD8 cytotoxic T-cell response and a helper response system important for making those CD8 T cells aggressive and capable of attacking the tumour cells.
Chris - So the immune system, once it's been primed using the Salmonella resembling vaccine cells, which are actually killed and don't go anywhere else once you put them in, the system then begins to attack the rest of the tumour. Presumably, there's some kind of crossover then. The immune system learns to recognise the cancer cells, having had its interest peaked by the presence of the Salmonella flagellin gene.
Julie - Yes, exactly. What we were able to show is that we can boost the memory response. The whole basis for vaccination for infectious diseases is, for example, you vaccinate with a particular component of a microbe and then the individual that's been vaccinated is protected, sometimes throughout their lifetime, against the infection itself. Here, it's the same idea. Because the microorganism has been seen the flagellin from the microbial components from Salmonella within tumour cells, the immune system can then make a response to that tumour and then subsequently that memory response is what protects against further development or growth of the tumour.
Chris - And there's no danger that the immune system might be led to start attacking healthy tissue because it gets interested in the cells and reacts to the wrong thing on them and then starts attacking healthy tissue.
Julie - Yes. This has been a caveat for whole cell cancer vaccines and many investigators do not prefer that, but there are also powerful mechanisms of tolerance that are inherent to the immune system. We have not addressed this in our study, but those mechanisms are so powerful that we think that we might be favouring the presentation of specific cancer derived molecules and those are the ones that are preferentially going to be targeted. So, cancer cells can share normal proteins with healthy cells, but they also have their own set of proteins that they express and there's a lot of efforts in identifying what those proteins are. Our hope is that by introducing flagellin, we can bypass the process of systematically identifying the individual proteins that cancer cells might have unique to them and not expressed on normal cells. In this way, we could, without knowing what those specific proteins are, we could prime the immune system to a whole slew of things that are going to be new to the immune system. And therefore, those normal proteins may not be targeted but it is something that we need to test in animals.
Chris - And just to finish off, talking of animals, the mice that you tested in your study, how did they do? What sort of improvement or clinical outcome did you get with those animals that were treated with this vaccine?
Julie - We had several models where we had transplantable lymphoma cells and also melanoma cells that are metastatic. With the melanoma cells, it was really dramatic. These melanoma cells are injected intravenously into mice and they metastasise to the lung. Those mice that were vaccinated with the flagellin containing melanoma whole cell vaccine did not have any metastasis. Their lungs were completely free of metastasis compared to the control animals that were not vaccinated. And similarly, the subcutaneous growth of those tumours, lymphoma cells that we have transplanted subcutaneously into the immunised mice, all the mice rejected the tumour and were capable of mounting a robust memory response to that tumour compared to the wild type unimmunised controls.
Chris - Super! We'll leave it there but thank you for bringing this up to speed. That's Julie Magarian Blander from the Mt. Sinai School of Medicine in New York.
12:55 - Drug knocks Alzheimer's on the head
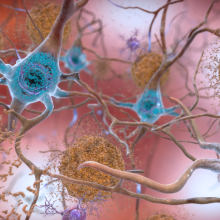
Drug knocks Alzheimer's on the head
A drug licensed for lymphoma and used to treat several forms of cancer may also be an effective anti-Alzheimer's agent, new research has revealed...
Bexarotene, marketed as Targretin, is licensed for the treatment of a disease called cutaneous T cell lymphoma, although it has also been used subsequently to suppress the growth of a number of other cancers including breast and lung malignancies. But owing to the way the agent works, by activating a signalling molecule called a retinoid X receptor (RXR), which is present on DNA and controls gene expression, animal experiments have now demonstrated that it can also dissolve the amyloid plaques that cause Alzheimer's and reverse some of the cognitive deficits associated with the disease.
Writing in Science, Case Western Reserve University researcher Gary Landreth and his team administered the agent to mice genetically programmed to develop the rodent equivalent of Alzheimer's. Treated juvenile animals showed a near immediate 25% drop in the levels of dissolved beta-amyloid proteins in the fluid bathing their brain cells. After 14 days of therapy, the number of amyloid deposits was down by 75% compared with controls. In older animals a 50% reduction in plaque number was achieved.
These structural changes were mirrored by functional improvements too, with treated mice recovering memory and cognitive abilities including being able to recall fearful stimuli, find their way around better and respond appropriately to smells.
The team think that bexarotene works by increasing the level of a substance called ApoE in the brain. This can dismantle the amyloid aggregates that are the neurological hallmark of the disease. Previous experiments in human subjects have shown that reducing the burden of these deposits can reduce the disease symptoms, suggesting that the agent might be able to achieve similar impacts in human subjects.
15:18 - Olympic Effort to get Children into Biology
Olympic Effort to get Children into Biology
Sir Steve Redgrave, British Rowing Team, Prof Mark Walport, The Wellcome Trust
A new project launched in London this week ahead of the 2012 Olympics to get school children across the country thinking about their bodies and how they work (if they needed any help with that) using sports exercise and a range of scientific experiments. Meera Senthilingam went along to the launch.
Meera - The pupils of St. Paul's Trust School in East London were treated this week to a range of experimental kits, helping them to explore their inner workings of their bodies during exercise. The kits will be delivered to schools across the UK as part of an initiative inspired by the 2012 Olympics and brought in by the Wellcome Trust to help pupils get active and in the zone as Mark Walport, Director of the Wellcome Trust, explains.
Mark - The Wellcome Trust has launched a series of kits for schools called In the Zone, teaching the next generation about their bodies and fitness which is designed for all stages of school, so it'll go out to more than 23,000 primary schools, to more than 6,000 secondary schools. And each of the boxes contains a series of experiments.
 Meera - So it's really focusing in on physiological traits that would benefit people perhaps during exercise.
Meera - So it's really focusing in on physiological traits that would benefit people perhaps during exercise.
Mark - Yes, that's part of it and it's also partly about teaching people how their body responds to exercise. So, if you think about the brain, reaction time is important, so there is an experiment that can measure reaction time. Your muscles are obviously hugely important in exercise and so, for primary children, there are simple experiments like, can you jump further if you have longer limbs? For secondary schools, we've got experiments that teach people about lung capacity. Obviously, if you have big lungs you're much fitter, potentially. Your heart rate is a very good measure of your fitness and how your heart rate changes in exercise and so, we've got pulse oximeters. It's a whole series of experiments which are, on the one hand, linked to the curriculum so they're relevant to science. On the other hand, they're specifically about health and exercising.
Meera - Have you had a go, Mark, on the equipment yourself?
Mark - Yes, I've had a go on some of it but I'm not sure I'd like to tell you the results!
Meera - Wellcome Trust Director, Mark Walport. Although Mark wasn't keen to share his results, many students were, as they publicly performed some of the experiments out on display, including one measuring lung capacity...
Cusomo - Hi. I'm Cusomo Baker. I'm 13 and I'm in year nine.
Meera - So Cusomo, you've got one of the experiments from the kits here which is a long plastic bag with lots of numbers down it...
Cusomo - Basically, it's got litres on the bag. You have to blow in it and that will show you how much you can breathe into it from your lungs.
Meera - So this looks at your lung capacity.
Cusomo - Yes, lung capacity. It's to do with your height, whether if you're longer, you will blow higher or if you're shorter, you will blow lower. So that depends on that.
Meera - Okay, so how tall are you?
Cusomo - I'm 5 foot 3.
Meera - Okay, let's see how much air you can let out.
Cusomo - Okay, I'll try it then.
Meera - ...you breathed out a litre and a half!
Cusomo - Yeah.
Meera - One man able to fill the entire 6 litres of the bag and more was 5-time Olympic gold medallist Steve Redgrave, though he is 6 foot 4, and the kits help you learn that height can greatly benefit this particular physiological attribute.
Steve - Hi. I'm Steve Redgrave and here with the Wellcome Trust today, having a lot of fun doing some experiments.
Meera - What would you say are the main physiological traits that people need to succeed at rowing?
Steve - The physical side is the length of levers. You don't really get very small people competing at the highest level. You can get short people to a reasonable level, but when it actually comes down to athlete size, they're all very tall. It's all about long levers in some ways.
Meera - Being tall is good. You've got those levers to get you through the water quite quickly, but what about your internal organs & phisiology?
Steve - Rowing is an endurance based sport. So you've got the physical side, you've got the right specimens leverage wise. They also have got to be trained to be be very efficient. If you don't have the lung capacity, the VO2 uptake transferring oxygen into energy that goes into red blood cells to feed the muscles, from that point of view, you're not going to be very efficient. So the science behind it becomes immense - training, preparation, monitoring, trying to improve levels all the time.
When I started back in the '70s, there was none of this. I remember one of the chief coaches wanting to do a muscle biopsy on me. I'd worked for a number of years building up my muscle and they wanted to stick a little needle in and pull a bit out just to find out if I was more fast twitch or slow twitch fibres! Endurance sport tends to need slower twitch, faster speed tends to be more fast twitch. I was a reasonable sprinter so I must have a reasonable amount of fast twitch fibres within my makeup but endurance wise, you can train it. So having that ability of natural speed and then trained for endurance, so the best of both worlds in some ways.
Meera - Did you learn a lot about how your body actually works through all this training and through the scientific methodology and did that help you then to get better?
Steve - I think it does. In sport, everyone seems to get faster all the time. They may not get faster every time they go out or within a year or even an Olympiad, the 4-year cycle. But over a period of time, times get quicker, athletes go quicker. You've got to use every aspect so diet, training, the science behind it - it all plays a part to being a better and faster athlete than we were before.










Comments
Add a comment