In this NewsFlash, we find out how tumours suppress the immune system, to allow their growth to go un-checked. Plus, how brain zapping could improve mathematical ability, a trick to block the damage done by a stroke, and the bacterial immune system - how bacteria keep themselves safe from harm!
In this episode
00:25 - Electrical brain boost
Electrical brain boost
A small dose of electricity to the brain can boost mathematical ability, a new study has found.
Oxford University researcher Roi Cohen Kadosh and his colleagues, writing in Current Biology, tested the effects on the mathematical prowess of 15 volunteers undergoing a process called TDCS - transcranial direct current stimulation, which involves non-invasively passing a small electrical current through the brain. The stimulus was applied to the parietal lobes (the back part of the brain), the right side of which has previously been shown to be linked to mathematical function, for 20 minutes every day over a 6 day period.
The subjects were then trained to handle a new set of nine "numbers", represented by symbols, the values of which relative to each other the subjects initially did not know. Their task was to learn them. They were assessed using standard maths testing algorithms designed to probe the subjects' understanding of how the numbers related to each other.
The results were intriguing. Subjects in which the right side of the head was connected to the positive electrode did much better on the numerical tests than subjects wired up the other way around who performed worse.
Control participants, who did not receive any real stimulus, fell somewhere between the performances of the two groups. Even more surprising, when the same subjects were re-tested months later and without having received any electrical stimulus in the meantime, those that had benefited from the stimulus initially continued to outperform the others.
According to the Oxford team, up to one person in 5 has significant difficulty handling numbers in their head. This approach, they say, could therefore make a significant contribution to boosting mathematical brain power for the numerically challenged, or just the average joe who wants to buff up his mental arithmetic!
03:25 - Blocking brain damage, at a stroke
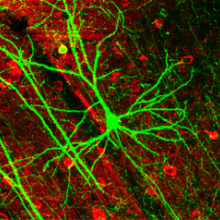
Blocking brain damage, at a stroke
Doctors may soon have a new weapon in their arsenal with which to combat strokes, which occur when the blood flow to part of the brain is interrupted.
Writing in Nature this week, UCLA-based researcher Tom Carmichael and his colleagues have found, using experimental mice, that surviving brain tissue surrounding an area affected by a stroke becomes electrically underactive. This occurs because the cells in this region increase their response to the inhibitory nerve transmitter GABA.
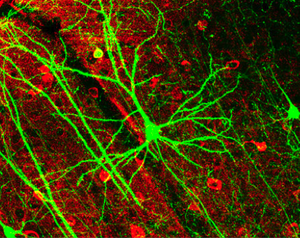 In the short term this is beneficial because, by suppressing the activity of these nerve cells the brain reduces their metabolic demands and therefore helps them to survive. But this state of electrical inexcitability seems to persist, which can hamper recovery in the long term. For instance, these brain regions can often take on some of the workload of the adjacent injured areas, helping to restore function.
In the short term this is beneficial because, by suppressing the activity of these nerve cells the brain reduces their metabolic demands and therefore helps them to survive. But this state of electrical inexcitability seems to persist, which can hamper recovery in the long term. For instance, these brain regions can often take on some of the workload of the adjacent injured areas, helping to restore function.
Reasoning that re-enhancing the activity of these cells might therefore boost recovery, Carmichael and his colleagues administered an agent called L655,708, which was able to block the aberrant GABA signals in the brain.
Animals that received this treatment, which was best administered from three days after a stroke, showed dramatically improved motor function compared with untreated controls. This suggests that stroke rehabilitation in humans should perhaps also include a pharmacological component, rather than solely a physiotherapy-based regimen as is currently the status-quo.
05:53 - Cancer's Own Immunosuppressants
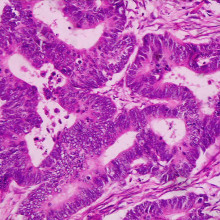
Cancer's Own Immunosuppressants
Professor Douglas Fearon, Cambridge University
Kat - Also in the news this week, scientists have made a breakthrough that could provide a new way to combat cancer and Cambridge University researcher Professor Doug Fearon has discovered that when cancers develop, they attract stem cells from elsewhere in the body. These stem cells, which carry a marker called FAP, seem to produce immune suppressing chemicals that prevent the immune system from attacking the tumour. But remove these cells and the cancer then becomes vulnerable to immune attack...
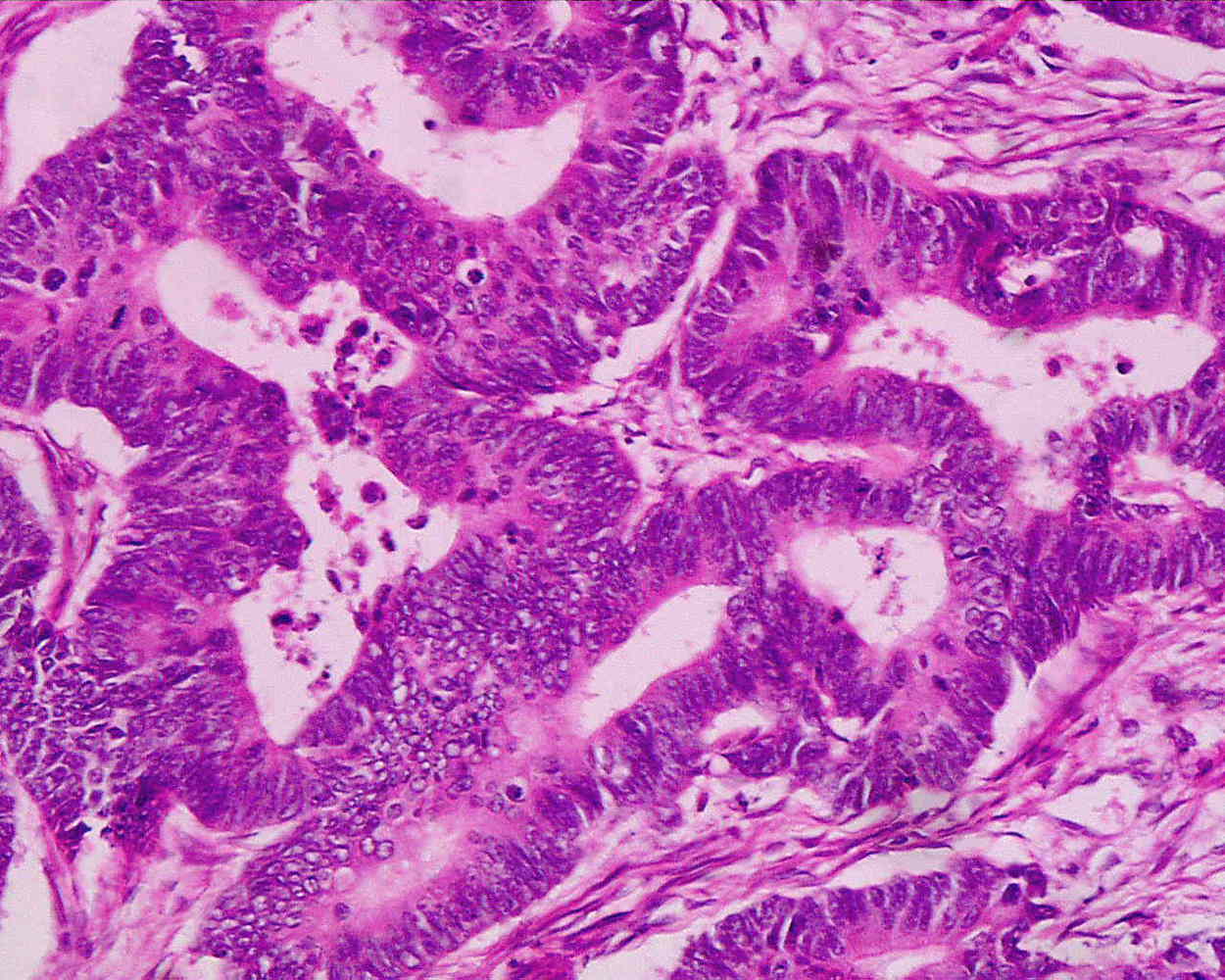 Doug - The problem that we wanted to solve was how did the tumour microenvironment prevent killing of tumour cells, cancer cells, by immune cells? We approached the problem by asking if there were cells in the tumour microenvironment that you actually would find in other places where we thought immune suppression would be physiologically reasonable like healing wounds or even the uterus and placenta. And it was a cell type that you could find in healing wounds, and in placenta that had first been described in 1990 by Lloyd Old, present in essentially all human adenocarcinomas. This cell could be recognised by its expression of a membrane protein which we'll call FAP, which is an acronym for Fibroblast Activation Protein. So using this as a membrane protein to identify a specific cell, we devised a genetically modified mouse strategy in which we could kill FAP expressing cells conditionally after tumours had formed in the mice, to see what would the effect be on immune killing the tumour.
Doug - The problem that we wanted to solve was how did the tumour microenvironment prevent killing of tumour cells, cancer cells, by immune cells? We approached the problem by asking if there were cells in the tumour microenvironment that you actually would find in other places where we thought immune suppression would be physiologically reasonable like healing wounds or even the uterus and placenta. And it was a cell type that you could find in healing wounds, and in placenta that had first been described in 1990 by Lloyd Old, present in essentially all human adenocarcinomas. This cell could be recognised by its expression of a membrane protein which we'll call FAP, which is an acronym for Fibroblast Activation Protein. So using this as a membrane protein to identify a specific cell, we devised a genetically modified mouse strategy in which we could kill FAP expressing cells conditionally after tumours had formed in the mice, to see what would the effect be on immune killing the tumour.
Chris - So your theory is that something is stopping the immune system attacking a cancer and that these cells that appear to be recruited from around an animal's body - these ones that are FAP positive, they make these fibroblast activation protein - they're the cells you believe that are suppressing the immune system. So if you get rid of them, the immune system should be able to attack the tumour.
Doug - Yes. That was a hypothesis we wanted to test was, if we were to kill that cell and only that cell in the tumour, could the immune system then control tumour growth? The outcome of the experiment was that when we did deplete the tumour microenvironment of these cells, the immune system did indeed kill the tumour or reduce the number of viable cells in the tumour within 48 hours.
Chris - How did you get rid of the FAP positive cells in the cancers in the mice?
Doug - That's been a very nice development over the last few years, where you can target the expression of human diphtheria toxin receptor, to particular cell types genetically in modified mice, because mice don't have a diphtheria toxin receptor. And if you give diphtheria toxin, the receptor internalises that toxin, a toxin turns off protein synthesis in the cell, and the cell dies within 24 hours. So the experiment is based on the fact we made mice in which the diphtheria toxin receptor would be expressed only in FAP positive stromal cells and nowhere else.
 Chris - So you put tumours into a mouse, they get these FAP positive cells in there, you delete those cells using this diphtheria toxin technique, and the tumours then regressed?
Chris - So you put tumours into a mouse, they get these FAP positive cells in there, you delete those cells using this diphtheria toxin technique, and the tumours then regressed?
Doug - They did in 48 hours - either didn't grow or actually got slightly smaller. In addition, the number of viable cells that we found in the tumour was decreased by about a half to 2/3. So, there was, overall, maybe about 80% fewer viable cells in that tumour than in a controlled tumour, just 48 hours after the addition of diphtheria toxin.
Chris - Is this exclusive to the experiments you've done or would you find the same population of cells in any kind of cancer, and therefore, the technique would generalise to other tumour types?
Doug - Well, as I said, this cell was discovered by Lloyd Old in 1990, published in a PNAS paper, showed that it was present in essentially all human adenocarcinomas. So, if the FAP expressing cells in humans have the same function as they appear to in mice, then potentially, if we could get at that cell in humans, most human adenocarcinomas might become more susceptible to immune control.
Chris - And do you know why those cells stop the immune system attacking the tumour?
Doug - The only insight we have now, which is pretty limited, is that we know we can block the tumour killing by giving neutralising antibodies tumour necrosis factor and interferon gamma, two cytokines made by immune cells, interferon gamma, particularly by T-cells. So we presume somehow that FAP expressing cells are inhibiting the tissue response to these two cytokines.
Chris - So the next step will presumably be to ask, can you ubiquitously get rid of FAP in the long term and see what happens to these animals? Will they stay healthy?
Doug - These cells are found in bone marrow, bone, adipose tissues, skeletal muscle, retina, olfactory epithelium of the nose, tongue - so a variety of different normal tissue sites, which has not been appreciated before, and it's looking like they have some important functions in these tissues, but we're still working on that. So I don't think it'll be a therapeutic option to simply kill these cells all over the body. I think somehow, we have to interfere with their function selectively in a tumour, so we need to be a little more sophisticated. We need to know and understand what these cells do. Do they make a protein that we could inhibit in some way? Can we inhibit how they accumulate in the tumour? Those are the approaches we have to develop. We can't have a blunderbuss approach of killing them off in the entire individual.
Chris - So is that the next step then, to try and work out how you can target just those cells in just the tumour environment and not have ubiquitous killing throughout the body because there probably will be consequences.
Doug - So, what we are doing is that we've looked at the genes that are being expressed in FAP expressing cells in adipose tissues, skeletal muscle, bone and tumour. And then we go to the tumour and say, what are the genes uniquely expressed in the tumour FAP cells? Might they be related to immune suppression? Might there be targets that we could have some therapy directed at and we're right in the middle of that.

12:20 - Bacterial immune system probed
Bacterial immune system probed
Bacteria have a clever gene-based immune system that helps them fend off attack, researchers have found.
Writing in Nature, Quebec-based scientist Josiane Garneau, from Laval University, has shown that when Streptococci and other bugs come under attack from bacteria-hijacking viruses called bacteriophages or even trnamissible pieces of DNA termed plasmids, they add a piece of the genetic code from the invader to a special region of their own DNA.
 The molecular equivalent of a DNA trophy cabinet, this microbial library consists of many short chunks of genetic material garnered from previously-encountered attackers. It's been termed the CRISPR region, short for clustered regularly interspersed short palindromic repeats.
The molecular equivalent of a DNA trophy cabinet, this microbial library consists of many short chunks of genetic material garnered from previously-encountered attackers. It's been termed the CRISPR region, short for clustered regularly interspersed short palindromic repeats.
This region, Garneau and her colleagues have discovered, serves as an immune memory for the bacterium. If the same bacteriophage turns up again, its DNA sequence is compared with the version lodged in the CRISPR region. If there's a match then a set of cellular scissors, directed by one of a family of genes called cas, chops up the invader's genome before it can do any damage. Understanding how this system operates could hold the key to "vaccinating" biotechnologically significant bacteria such as those used in the cheese and dairy industry to make the bugs less vulnerable to bacteriophage attack.










Comments
Add a comment