Are you one of the many people who take ACE inhibitors or ARBs to treat high blood pressure? Or to help with heart issues or diabetes? In the UK, this is about one in seven people, making these are some of the most common prescription drugs out there; and recently there have been worries that they might make a coronavirus infection worse. The link between the drugs and the virus is a molecule inside everyone’s bodies called ACE2. On today’s show, meet ACE2, the protein in the spotlight: the bastion of our defenses, that’s become the very breach in our walls. Protector, turned betrayer...
In this episode
00:43 - What is ACE2?
What is ACE2?
Josef Penninger, University of British Columbia; Patricia Gallagher, Wake Forest School of Medicine
There's a system of hormones in our bodies that controls blood pressure called the renin-angiotensin system. The crucial parts, for this story, are: a hormone called angiotensin; and some enzymes that convert it, aka angiotensin converting enzymes - A C E. This is what ACE2 stands for. One of the people who first discovered much of this is Austrian researcher Josef Penninger, and he explained it to Phil Sansom...
Josef - Because the system called the renin-angiotensin system and this system, for instance, regulates blood pressure, it regulates our heart functions, our kidneys. It's one of the most fundamental systems for our basic physiology and there are two enzymes which regulate this: ACE and ACE2. ACE constricting blood vessels, and ACE2 the opposite - it opens the blood vessels and keeps us healthy, keeps multiple of our organs healthy.
Phil - Can you help me picture what it kind of looks like?
Josef - Yes, so the ACE2 basically is produced inside the cells and then it goes to the surface of the cells. Part of it is still in the cell. The business end is outside of the cell. It sits on many, many tissues because the system has multiple functions in our body.
Phil - Why do viruses come into all this?
Josef - So the viruses came into this because after we had found it, then we found a totally novel system that ACE2 actually protects against lung failure. At this time when we start working on this, basically built an ICU for mice, which took us years to do.
Phil - Did you consider calling it a mice-CU?
Josef - That's a great idea. Mice-CU it actually is! So we built a mice-CU and found to our surprise that ACE2, like in the heart, is this good guy. Without ACE2 blood vessels started to leak, the whole lung became a full of water, full of inflammation. And then a group in Boston said that ACE2 could be a candidate receptor for the first SARS virus. That basically clicked because if ACE2 protects from lung injury and the SARS virus causes a very severe lung disease, maybe the two fit together.
Phil - What exactly is the relationship between these viruses and the ACE2? Is the ACE2 the thing the viruses are attacking?
Josef - ACE2 is the door into our body for the viruses. The virus can only live if it enters our cells in our body, and to enter the cells in our body it needs a gate. ACE2 is the central entry gate for the first and now the second SARS coronavirus.
Phil - Are you saying that this is the reason that these coronaviruses do the damage that they do because they're using this ACE2 which ordinarily would help against lung infection?
Josef - Correct. It's a really evil, you know, there's no moral for viruses, but it's a real evil virus to hit one of our essential protective systems.
Phil - And when they hit that gate, do they also sort of use it up?
Josef - Exactly. So they don't just open it, they actually take the gate with them inside the house. And that's why believe these two particular viruses became so dangerous.
Phil - So you're saying there's kind of this double whammy of both the damage inside the cell and the damage you get from losing this helpful ACE2, which is sort of why this current virus has been such a problem.
Josef - Correct. This double whammy. And because the gate doubles as a good guy in our body.
Phil - You mentioned that ACE2 does all this stuff to stop you getting, for example, high blood pressure. If the coronavirus is getting rid of that, are we seeing patients with the coronavirus who've got, you know, blood pressure issues or something like that?
Josef - Yeah. What's really interesting is, you know, if you look at the cases, people who died unfortunately of Covid-19, most of them have actually had a disease before. And the diseases they have before are diabetes, which affects the blood vessels, cardiovascular diseases, hypertension, exactly where ACE2 has actually a critical role. It's very suggestive. And now it turns out in the latest stage of Covid-19, there's this rampant infection of more or less old blood vessels. So it does explain a lot.
ACE2 is the doorway that the virus uses to get into our cells. But not everyone’s cells have the same number of doors, so to speak. To find out more, Phil got in touch with another biologist who’s long researched ACE2...
Patricia - I'm Patricia Gallagher, I'm a Professor in the Hypertension Research Center at Wake Forest University in Winston Salem, North Carolina.
Phil - And I have to say you're sounding pretty good right now. Where in your house are you?
Patricia - I'm in a closet. You have put me in the closet.
Phil - I feel bad when you put it like that.
Patricia - That's all right.
Phil - So tell me about ACE2.
Patricia - One of the primary functions of ACE2 is to maintain the proper balance between two hormones: angiotensin 2, and angiotensin 1-7. Now these two hormones are coursing through your body as we speak, angiotensin 2 constricts or narrows blood vessels while angiotensin 1-7 dilates or opens blood vessels up.
Phil - That's kind of a funky naming system. Why isn't it angiotensin 2 and angiotensin 3?
Patricia - Well, angiotensin two is eight amino acids long, and ACE2 cleaves one of those amino acids to produce angiotensin 1-7. Angiotensin 2 also promotes inflammation. While angiotensin 1-7 has anti-inflammatory properties. ACE2 ensures that the levels of these two hormones are balanced, so there's proper defense against invaders and so that your blood pressure is not too high or too low, so it's kind of a ying and yang thing.
Phil - How important is it in the grand scheme of your body?
Patricia - Well, we think of ACE2 and angiotensin 1-7 as part of a pathway that protects against chronic diseases such as hypertension, heart failure, cardiovascular and lung disease, and diabetes. SARS and Covid have hijacked this essential protein as their host receptor and in the process wreaked havoc in the patient.
Phil - Does that mean then that if you reduce the amount of this ACE2 that you have that might protect you against the coronavirus?
Patricia - Well, it's a complicated issue. Before, or in the initial stages of infection, that might be a good thing. But later on when you've got that severe pneumonia, high levels of systemic inflammation, increasing ACE2 may be a good idea.
Phil - So you're saying that even though it's what the virus uses to get into you, it's still useful to have when you've got the virus because it does all these good things?
Patricia - In the later stages definitely, I would think high levels of ACE2 may be a good thing and there are actually clinical trials right now looking at drugs that cause an increase in ACE2 to give to patients in the latter stages of disease.
Phil - Now do different people naturally have different amounts of ACE2 to start with?
Patricia - There's a lot of data accumulating now on a few levels. There are studies showing that Asians, particularly Asian females, have high levels of ACE2 compared to other ethnicities. Men have higher levels of ACE2 than women. ACE2 also increases as we age. This increase in ACE2 with age may in part explain why Covid-19 has such devastating effects in patients over 60, but also these patients tend to have chronic disease. This is a complicated process.

10:07 - ACE inhibitors: protection against COVID-19?
ACE inhibitors: protection against COVID-19?
Hugh Montgomery, University College London
There’s a crucial distinction between ACE2, the star of our show; and ACE, as in ACE inhibitors. They’re both in the same system, and both first and foremost seem to affect blood pressure, but in opposite ways. Let's look now at ACE. Hugh Montgomery is an intensive care specialist at University College London, and he explained to Phil Sansom what ACE does, what ACE inhibitors might do, and what role the genetics seems to play in all this…
Hugh - We all have two ACE genes and we can have one of two flavours. One's known as the I or insertion variant, which has got a tiny little extra chunk of DNA in it. And one's called the deletion or D variant, which has that little bit missing. That changes how much of this protein the gene makes. Which is called ACE.
Phil - So this isn't something that breaks the gene and stops it from doing stuff. This just changes what happens.
Hugh - That's right. Essentially it changes how much of this active protein you've got. And for a long time we thought the only reason this system existed was to control your blood pressure and for that very reason a bunch of drugs are made. These are called ACE inhibitors and they lower the amount of ACE activity and that lowers blood pressure. Now these drugs are widely used now, but it is true that this turns out not just to be something that regulates blood pressure, but it regulates the growth of cells and it also regulates their metabolism. You DDs in the audience, a bit like me, are likely to find that you can stack muscle on very easily with training. Whereas the II people, the low ACE activity people are very much better generally speaking at endurance. The I version of the gene is much more common in long distance runners. Now the D version is much more common in power lifters and rowers for instance.
Phil - What's the version that's really, really good at sitting down for long periods of time.
Hugh - Well do you know what there are even genes that influence whether you want to sit down on your rear end and watch Netflix all day!
Phil - I better thank Joe Wicks now for helping me overcome that stuff. Now when it comes to the coronavirus, this is sort of related, right? Because ACE acts as part of the same system as the thing that the virus attaches onto.
Hugh - Yeah, so this is really exciting. We were doing some work with mountaineers. These people climb of course very high and there the higher you go, the less oxygen there is. And we found that the I version of the gene was very, very much more common, much, much more common even than in marathon runners. Having those same genes massively influenced your chance of surviving from severe lung injury. In fact, you were five times less likely to die, which is way beyond any impact on mortality I could have as a competent and hardworking intensivist. So there are a couple of questions. The first of them is if we just took this coronavirus set of patients with very bad lungs and low oxygen, would they benefit from us giving them an ACE inhibitor and lowering ACE levels? Would we find a similar reduction in mortality? We don't know, but the data is suggesting that it might. If we look at the distribution of the I and D versions of the ACE gene around the world, the places that have much more I versions of the gene do seem to have less severe disease with coronavirus. And secondly, there's a three fold reduction in mortality in people taking an ACE inhibitor or actually something that blocks the product base, this angiotensin 2. Now that's not enough to prove the effect, but these data fit together to suggest that low ACE activity might work and we think this may give us a potential treatment that works. In fact, we're just about to start those trials hopefully soon with using those very same cheap, effective drugs that treat blood pressure and heart failure. If there were no such trial and there were no other options, my money were I betting, would be that the ACE inhibitor would work, but we're going to find out.
Phil - This is all such a far cry for when people were worried that these drugs would make the condition worse.
Hugh - Yes, and of course that was the first story. So when we first heard that ACE2 was the protein receptor for the spike protein of the coronavirus, we were all a bit anxious - should we be stopping ACE inhibitors on all the patients? And as it turned out, we don't see any signal for harm at all. So if I was an ACE inhibitor now listening to this podcast, I would continue to take it.
16:16 - How genes affect COVID-19 risk
How genes affect COVID-19 risk
Ewan Birney, EMBL-EBI
Scientists are still trying to work out what makes one person’s coronavirus infection just a bad cough, and another person’s a life-threatening hospital visit. There are plenty of theories relating to your age, sex, health, and more. But what about your genes, such the gene for ACE discussed earlier? How much do they explain? And, like some have theorised, could this be why certain minority ethnic groups are disproportionately going to hospital with this disease? According to Ewan Birney, that’s unlikely. He’s director of the European Bioinformatics Institute, helping gather coronavirus patient DNA…
Ewan - Actually, most of the variation about whether you're infected with the virus will be due to your exposure, but some, perhaps of whether you progress or whether in hospital you have a mild form of the disease or severe form of the disease, those may well have genetic factors contributing to the variation that we see.
Phil - And do you have an idea for this coronavirus of how big a role genetics might play?
Ewan - No, we don't really. There's been some initial work using some twin studies that says that there's some evidence that there's going to be a genetic component, and our experience of of many other previous studies would argue there'll be some aspect. For me. I think in particular between mild and severe disease is going to be our most fruitful area to look at. But we're not, we can't say that for sure in many ways one has to collect the data set and do the analysis before one can be sure. The very early genetic analysis is not showing much variance being contributed by genetics, but we just don't have the sample size to be sure that that's the full story. We need to wait until we have more cases coming through the system.
Phil - If you do find something, what's the point? What can you actually do with that?
Ewan - Yeah, potentially it can point us to parts of the genome where different individuals in the population vary and if we're lucky that part of the genome is in a pathway that we've already got a drug for. That would be our best result. Now if we find something in the genome that there isn't a drug, there is a possibility of making a new drug that is a long, long road, though. A final possibility is that there are genetic components which are big enough that they really show the difference between different individuals in a way that we can actually use in terms of saying well you're very much at risk and you're not. Now I actually don't think that's going to be a likely outcome of the genetics: tends to be that genetics is very complicated, but it is a possibility
Phil - If you do end up finding patterns, are they likely to be with, you know, everyone or are they going to be patterns in specific groups of people or what?
Ewan - Human genetics is very mixed and very messy and so they're likely to be weak and distributed across all humans on the planet. That's the way most human genetics works out. It's important to realize that although we, in society, we have a lot of casual use of self identified ethnic groups. So if you're presented with a form where you're asked to tick who you are, whether you're a European American or an African American or a white British or white Irish or these other terms, most people feel confident about ticking those boxes. That process of ticking boxes is less aligned to genetics than people's intuition thinks. So it's unlikely that there's going to be big differences between these self identified ethnic groups. Now you might be aware that it's reasonably clear both in the UK and the US that many people in minority ethnic groups, African Americans in the US and Afro-Caribbeans and South Asians in the UK, seem to be disproportionately represented in hospitalizations of Covid-19. But what you have to remember is two things. Firstly, the biggest outbreaks are happening in dense urban city centres, London, New York, and these spaces which have a much higher level of of these groups. And secondly, many of the things that we know are involved with causing severe disease such as type two diabetes and obesity, cardiovascular issues, are related to socio-economic status, which is related to how much money you have. And that is distributed in a very skewed way in our society. So I'm relatively confident that there is not a big genetic component explaining the observed differences we see of ethnic group labels with Covid-19.

21:15 - 50% heritability for key COVID-19 symptoms
50% heritability for key COVID-19 symptoms
Frances Williams, King's College London
The evidence is starting to come in on whether host genetics - in this case, the genetics of human hosts - changes the response to COVID-19. Here in the UK, Kings College London rolled out a popular COVID-19 Symptom Tracker app, and they’ve recently released their heritability findings: using twins to figure out how big a role genes play in key symptoms. Katie Haylor spoke to one of the team, Frances Williams, about what they’ve found...
Frances - We've done what's called a classical twin study in which you can compare symptoms among the twin pairs. Because we know that identical twins share a hundred percent of their genetic material, while non-identical twins share on average 50%, we can compare between the identicals and non-identicals and work out roughly what the contribution is of genetic factors.
Katie - And what symptoms specifically are you talking about?
Frances - Cough, fever, delirium, loss of taste and smell, shortness of breath, chest pain, abdominal pain, diarrhea, that sort of thing, all the commonist symptoms associated with many different viral illnesses. We could combine the symptoms in a mathematical model to determine the best combination of symptoms that predicts being positive on a test for the virus. So it's a combination of those symptoms, such as the loss of taste and smell and fever with persistent cough and fatigue, and age and sex are also in the model. And interestingly, that model has the highest heritability of all the symptoms that we looked at: 50%. Which means that roughly 50% of the difference in expression of those symptoms is accounted for by genetic factors.
Katie - What does that mean for an individual?
Frances - Well, it's difficult to extrapolate to an individual because heritability is all about the group differences in the population if you like. But I think what this is telling us is that while many people consider infections to be an entirely random event, in fact it's not entirely random. It is to some extent influenced by the individual, but we know that many symptoms of viral illnesses actually occur because of the host immune system reacting to the presence of that virus rather than the damage that the virus itself causes directly.
Katie - Do you think this could go any way to explain why some people seem to be relatively mildly affected whereas other people are severely affected?
Frances - We know that the people that end up with a major illness requiring hospitalization often developed high levels of inflammatory proteins in the blood. And it may well be that what we're seeing in our study is reflecting the fact that somebody's genetic makeup can impact how their immune system responds to viral infection and whether or not it responds by making very high levels of those inflammatory markers.
Katie - What's the value in understanding to what extent the symptoms or risks are heritable?
Frances - Firstly, it's a better understanding of how genetic variation influences people's susceptibility to the disease. So it might be possible if we developed, for example, a test which would advise people better about their risk of developing (FULL?) Covid-19. So rather than just have a blanket rule about by age or by sex, everybody has to stay indoors, you could make it more personalized. And the second big value I think for this app is being able to collect large volumes of data real time about how this infection is spreading across the country.
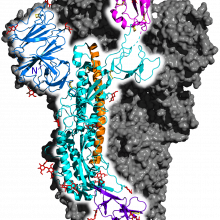
25:18 - ACE2 variation may affect spike protein binding
ACE2 variation may affect spike protein binding
William Gibson, University of British Columbia
Human genetics seem to affect COVID-19 infections; but what about the gene for the crucial protein, ACE2? Does variation in the ACE2 gene make the coronavirus see you as a bullseye - or even the opposite, might it protect you? Medical geneticist William Gibson at the University of British Columbia tried to find out, using a big database of people’s DNA called the gnomAD, and told the story to Phil Sansom...
William - There's just over 141,000 people represented in the gnomAD database.
Phil - And are you looking at this ACE2 gene? What it's like for all of those people?
William - We did. Not every person had reliable data at every part of the gene. Fortunately, the gnomAD database gives us data on the quality of each person's DNA sequencing at each specific site, so we were then able to look at the number of X chromosomes in both males and females that had reliable data at each of the sites that we were looking at.
Phil - Oh, okay. So you've got all your people, you've got twice the number because all the women have two X chromosomes, and then you've whittled down to get all the ones that are definitely accurate. What differences did you find in this sort of final amount of data?
William - In the final analysis, we found that there are differences in the ACE2 protein and these differences seem to be distributed differently among different human populations and predicted to be at different levels between males and females.
Phil - Talk me through this. What kind of variants can you get?
William - You can get genetic variants that are predicted to stop the protein from being made. They either break the protein or they make a protein that's too small to do anything. You can also get variants that are predicted to change the shape of the protein but not break it so the protein likely works pretty well and we call those missense variants. We're looking at a small number of the variants that are specifically predicted to bind to the virus as opposed to all of the missense variants overall.
Phil - How many of these types of variants did you actually end up finding?
William - Between 14 and 15 missense variants in the ACE2 protein that were predicted to bind the virus. Some of them were predicted to bind the virus more tightly and some of them were predicted to bind to the virus less tightly.
Phil - How common are these differences overall?
William - Uncommon but not unheard of. Among males of European descent, around 1 in 170 males would be predicted to have one of these variants. It's about 1 in 80 females. Interestingly enough, these variants were more frequent in individuals of Ashkenazi Jewish descent, and they seem to be less frequent among Latin Americans, South Asians, people of African descent, people of Finnish descent, people of East Asian descent.
Phil - Really what does that mean?
William - It's not entirely clear what it means. What we're looking into now is whether these variants actually affect susceptibility to disease and disease outcome. We're not sure about that yet.
Phil - Did you find that, for example, the Ashkenazi Jewish population had more of the variants that bound the virus better or more of the variants that bound the virus worse or neither?
William - I confess, we haven't actually split out the numbers that way. Partly because we're not really sure how good our prediction software is. In other words, do the predictions that we make using the software actually correlate to actual binding of the protein or not?
Phil - If they did, is there anything you could do about it?
William - Theoretically, if someone were found to have a high susceptibility variant, then that be very useful for them to know in terms of either self isolating or of course for their healthcare practitioners if they were found to then contract the virus. That's someone who would need quite carefully managed care.
29:55 - Common ACE2 variants: no effect on physiology
Common ACE2 variants: no effect on physiology
Serena Sanna, Italian National Council of Research
Evidence on host genetics in is coming in all the time, from different methods and sources. A study from the Italian National Council of Research seems to show that common variation in the ACE2 gene doesn’t seem to affect much in the way of bodily traits like blood pressure - at least for healthy people. Phil Sansom spoke to Serena Sanna, one of the researchers...
Serena - We found that none of the common genetic variation in this gene are associated with physiological variation between individuals. So there's no impact in regulating cholesterol level or your weight.
Phil - Nothing at all?
Serena - No, not among all the 150 different measurements that we considered.
Phil - How did you figure this out?
Serena - So we looked at more than 30,000 volunteers. They all live in the North of the Netherlands. So we have genetic information of those individuals. So we looked at this ACE2 gene and there are roughly 1000 variants in that gene that are common, means they are present in at least 1 person in every 100. We compare the different variation to their corresponding level of blood pressure or glucose or cholesterol and so on.
Phil - If you found no associations, what's the most surprising? Were there any that you thought might be there that you just found nothing for?
Serena - Well, the first question was, is this gene involved, for example, in blood pressure or glucose? Because we are seeing a lot of coronavirus patients that also have hypertension or diabetes. But in reality this was not. So, if there is any explanation for this, probably comes from other genes or from some other factors.
Phil - So out of all these like a thousand different versions of this gene that a few people have, it doesn't seem to affect any of your physical stuff at all.
Serena - Yes.
Phil - What does this mean for people?
Frances - This means that for the coronavirus infection, this gene is probably not having any role in making symptoms worse in terms of hypertension and diabetes.
Phil - You've been talking about common variants specifically. Does that mean that they're rare ones that you didn't look at?
Serena - Yes, correct. There are rare variants in these genes that we did not look at because we looked at 30,000 volunteers, but for rare variants, so variants that are present in 1 in every 10,000, we really didn't have enough numbers. So we did not look at this specific category of genetic variant, which might still play a role and infection. And usually rare variants in the genome have a higher impact than common variation.
Related Content
- Previous What are the thin bones in chicken wings for?
- Next High anxiety










Comments
Add a comment