We hear more than ever about the secrets hidden in our genes, from our risk of diseases to traits such as intelligence or even sporting ability. But can we really test for them? And just because we can, does that mean we should? Plus, an extremely popular - and extremely distracting - gene of the month. This is the Naked Genetics podcast for October 2016 with Kat Arney...
In this episode
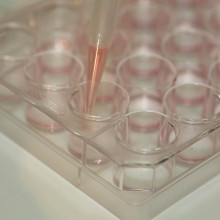
01:04 - Nazneen Rahman - Cancer gene screen
Nazneen Rahman - Cancer gene screen
with Nazneen Rahman, The Institute of Cancer Research
Over the past few years we've witnessed the rise of personalised or precision treatments for cancer - drugs that target the products of faulty genes in cancer cells, as revealed by genetically testing tumours. But what can genetic information tell us about cancer risk, and the chances of developing the disease in the first place? To find out, Kat Arney spoke to Professor Nazneen Rahman at The Institute of Cancer Research and the Royal Marsden hospital, who has spent her career studying the genetic faults and variations that influence the risk of many types of cancer...
Nazneen - Well the first thing that makes it difficult is cancer is so very common. About one in two, one in three people will get cancer. So everybody has cancer in their family and that's not usually actually due to genetic factors. There are all sorts of different things that lead to us having an increased risk of cancer. So the first thing we're doing when we're sort of doing that is trying to work out how likely it is that inherited factors are going to be relevant. That depends firstly on the type of cancer and then also, of the patterns of cancers in the family.
Kat - So, what would be some kind of classic hereditary cancers that you can pick out?
Nazneen - Well, probably the ones that people know about most are the breast and ovarian cancers. Ovarian cancer in particular, around about one in five ovarian cancers is due to inherited factors usually in the BRCA genes. A lot of people know about that because of Angelina Jolie.
Kat - Yes, the Angelina Jolie gene I believe we must call it.
Nazneen - Don't call it that! So ovarian cancer is one in which genetic inherited factors are making a big impact. Breast cancer is only about 3 or 4 per cent that are due to these inherited factors. But because breast cancer is so common, it ends up being about the same number of cancers per year. About 2,500 of both ovarian and breast cancer per year in the UK are due to inherited factors.
Kat - What else can we tell about an individual's cancer risk from their genetics because we sort of hear about those - if you like to call them, the strong gene factors - things like the BRCA genes? Surely, there are other things in our DNA that maybe more subtly increase or decrease our risk. Can we look for those? What do they do for us?
Nazneen - Yes, we can. I think it's probably more helpful to think about what gives us cancer overall as a whole spectrum of things - genetic, environmental, lifestyle. All of these things are working together to make it more or less likely that a person will get cancer. And there are also chance events in it. so, I think the importance of thinking about those very strongly acting genetic factors particularly in terms of prediction is that if you're at a very high risk of having a particular disease then you're more likely to act upon that than if there's just a slightly increased risk. Again, particularly if you're at a high risk anyway because one in two people will get cancer. So, in terms of really having an impact on the choices that people can make and giving useful information, the higher the risk is, the more likely that's going to lead to meaningful actions for people.
Kat - If say, I was worried about my genetic risk of cancer, what could I find out? How can I go about finding out is there anything in my DNA and what might it mean for me?
Nazneen - I think what we're really trying to do in the UK to really try and give that information through the individuals who first got cancer in the family. So, we're trying to get more and more of this testing happening for cancer patients. One, that allows us to give the cancer patient themselves better tailored information because they've got their cancer because of this genetic risk. But in turn, that means that we can then go out to the people in their immediate family and then more beyond who are at risk of having inherited it so that we can have a much more effective way of getting that information out to the people that needed it. If you actually tested the whole population, that would be pretty ineffective because they're overall in the population. They're sort of rare, only about 1 in 300 of the individuals would have that. So, I think the way in which we're trying to get people to have that information is really by trying to get as much testing done for cancer patients first and then going out through the family through that way.
Kat - So, is it going to be likely at any point that there's like a national cancer screen where everyone can have all their genes looked at? I'm thinking that there are already products where you can get a lot of information about various things in your DNA, how they affect your risk of health. Are we not really at a point of using genetics for widespread population screening?
Nazneen - Not in terms of cancer. There are two reasons for that. One, it doesn't make sense even economically or even scientifically really. There's only a certain number of these mutations in the population. So to survey the whole population to find them is a very inefficient way of doing that. Equally importantly and possibly even more importantly, we don't really know at this point what the risk of cancer is and that's the critical information. So, if you just test a random member of the population and find they have a mutation in a gene that can increase the risk of cancer, the natural question is, "how much is my cancer risk now?"
Kat - Will it happen? That's the big one.
Nazneen - And that sort of information we haven't got because we haven't done studies on the population at large. What we do knowledge is that cancer risk is not a definitive value. It's in itself very changeable. So the risk of cancer, even of the same mutation, will vary depending on all sorts of contextual things about that individual. So we actually haven't got enough information to give, clear information to people if they were having testing in that context. We still need to do these studies.
Kat - In terms of your own work, you're particularly focusing on ovarian cancer. What are you trying to do to unpack this disease more?
Nazneen - Well ovarian cancer actually for us is a kind of exemplar really of the whole system. The system really is about making genetic testing routinely and easily available where it can have a beneficial impact for cancer patients and their families. The reason that we chose ovarian cancer was firstly because genetics is important. As I say, one in five individuals with ovarian cancer will have had their ovarian cancer because of an inherited gene mutation. Secondly, it is a disease where there's still a high mortality. And so, anything we can do to try and reduce that and prevent cancer from occurring is very important. And so there, what we're trying to do is making sure that all ovarian cancer patients can have access to the genetic testing so we can find out who has the inherited cause. And that impacts to their treatment, also the ones who don't, that also has impacts on their treatment, so it allows to personalise their treatments. But then also, we can go out to their family members. They can potentially have testing. If they're at higher risk, prevention of ovarian cancer by keyhole surgery after people have completed their families is a very effective way of preventing the cancer occuring in the first place.
Kat - So just removing the ovaries so they can't become cancerous.
Nazneen - Yes, absolutely. So, prevention is always better than cure. Often prevention is extremely difficult because either you can't remove all parts of the body.
Kat - You can't take someone's whole bowel out.
Nazneen - You can't, absolutely. So, sometimes if the risk is high enough, people do have their bowels out. But again, it depends on your risk. It has to be incredibly high for that to be a reasonable strategy. For ovarian cancer, as I say, once people have had their families you can have the ovaries removed by keyhole surgery. And in a situation where you still got a very high mortality and there's no useful screening, a lot of women, over 80 per cent of the women we see if they're at high risk, will choose that option.
Kat - Nazneen Rahman from The Institute of Cancer Research.
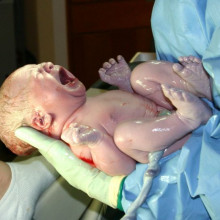
08:46 - Tony Gordon - Genes, embryos and babies
Tony Gordon - Genes, embryos and babies
with Tony Gordon, Genesis Genetics
Kat - We've just heard how genetic testing for cancer patients -if not the general population at large - could be useful. But what about taking things back to the very beginning of life? At a recent conference run by the Progress Educational Trust, called Testing, testing, 123, scientists, genetic counsellors and ethicists debated the issues around genetic testing on early embryos, created through IVF. One of the speakers was Tony Gordon, UK lab director of Genesis Genetics, so I caught up with him in his lab in London to find out more about the ways in which he and his team can test embryos and fetuses for genetic disorders.
Tony - We are involved in what we call the reproductive genetic health spectrum. So, we can test embryos basically for their chromosomes to ensure they had the right number of chromosomes which is called pre-implantation genetic screening. We can also test embryos to make sure that they have the correct inheritance of single genes - that is pre-implantation genetic diagnosis. Also, we do here prenatal diagnosis using maternal blood which is known as NIPT - Non-Invasive Prenatal Testing. And that tests for Down Syndrome, Edwards Syndrome, Patau Syndrome, and sex chromosomal aneuploidies.
Kat - So, let's go to the embryos first. What sort of stage embryos are we talking about, like the big ones, little ones, how many cells? what's going on?
Tony - We can test for day 3 which is called the blastomere stage. That's eight cells and you can take one cell from that eight cells. Increasingly, that's becoming less tested for because you're taking an eighth of an embryo and sort of rationally, that's possibly not as good as testing at other stages. Primarily, we test now at day five. The embryo is kind of formed, almost what looks like an egg if you can imagine. So, the inner cell mass is the yolk and then on the outside is the trophectoderm which is the shell. The trophectoderm goes on to form the placenta. So it's not actually called the embryo and we can take 3, 5, 8 cells from that day 5 trophectoderm and test that.
Kat - What sort of things are you testing for when you're doing say, the pre-implantation genetic screening, and the pre-implantation genetic diagnosis? What sort of conditions can you look for?
Tony - Pre-implantation genetic screening is a fertility test, as it were, in terms of we are looking to ensure that the embryos that we look at just have the right numbers of chromosomes. You're not looking at anything in terms of genes at that point. But that is just to try and ensure that we've got an embryo that is more likely to produce a healthy birth. PGD, Pre-implantation Genetic Diagnosis is different because we're looking at genes there and we can test for the inheritance of about 240 different conditions. PGD patients aren't infertile. They have an inherited condition that they want to avoid.
Kat - So, that might be something say, like cystic fibrosis or a severe genetic condition that one of the parents is carrying and they don't want to pass on.
Tony - Yeah or both parents of course because it could be a recessive disease where they're both carrying it. But there's also oncology disorders like BRCA and then there's also some late onset disorders like the Huntington's which you have to be very careful about how you look at the parents because you need to test without informing them that one of them has a late onset disorder. So there are special protocols for how we do that. So there's quite a wide spectrum of diseases with different inheritance. And then finally, under the PGD umbrella, there are people who are carriers of chromosomal translocations that we can test for as well.
Kat - These are all embryos that are being created through IVF. So they've been made in the lab from mixing an egg and a sperm together?
Tony - That's absolutely correct.
Kat - So let's move on to the foetal testing. So this is when the baby is already growing inside the mum and you can test her blood. What are the conditions that you're looking for? How are you looking for them?
Tony - When the foetus grows within the woman, the placenta forms and the placenta is kind of slightly leaky and it leaks small amounts of DNA into the bloodstream. We can test for some fairly straightforward chromosomal abnormalities and changes in the sex chromosomes as well.
Kat - What's the purpose of doing this? Is it just so women can decide, "I don't want to have this baby. I want to have a termination." What do people do with this information? How does it help to know this?
Tony - Every patient that we have that has a positive result is screened by one of our genetic counsellors. It is a personal decision. You could quite feasibly have a Down Syndrome positive result and then go on to have a Down Syndrome child. That's perfectly reasonable outcome. Different people have different desires for what they want to do with their pregnancy. We help with our genetic counselling to give them the information as to what the outcomes might be. Down Syndrome, it has a very large different amount of penetrance, so presentation of phenotypes. We can't predict that. So that's something that the patient and genetic counsellor has to discuss.
Kat - So, some children could be very, very severely affected and some children could be very high functioning.
Tony - Absolutely and quite a lot of Down Syndrome pregnancies don't actually progress to full term as well. So, there's a really big spectrum of presentation of Down Syndrome.
Kat - When you think about genetic testing, you think about like, "is that there? Yes, no." But the more we understand about genetics, it's becoming clear that it's not quite as simple as one gene, one fault, one disease. Is this kind of testing capturing that kind of complexity? Are there some areas that are a bit challenging for the link between the gene and how you come out?
Tony - It's a fascinating area because the more advanced our genetic testing gets then the more interesting and sometimes complicated difficult questions we come along to. So you're absolutely right. None of this is straightforward and that goes right through to prenatal testing where actually, we're testing the placenta sometimes isn't representative of the embryo itself so, these interesting questions that you have to consider at that point as well.
Kat - There's a lot of questions that are raised by this kind of technology - some of them technical, some of them ethical, some of them societal. Where is the debate now about how this technology moves forward? What's acceptable? What can we look for? What should we look for? What should we do with this information?
Tony - I think we're very fortunate in the UK that the HFEA, The Human Fertility and Embryology Authority, they have a very good programme that looks at these future questions, whether new conditions should be licensed. So any new condition you want to bring forward has to be licensed. So, there's very vigorous debate about where this can go and I think as science progresses faster than legislation, as always, there's new ethical questions of genome editing, CRISPR, things like that. I think already, we've begun to address them and really, I think we're in a pretty good state in the UK in terms of being ethically very considering every view of the new ethical issues that are coming up. It's a fascinating area.
Kat - And to sort of run the sci-fi thing to its logical conclusion, would this technology end up with a perfectly homogenous population of perfect humans where every single disease is screened out?
Tony - No and the reason is that if you do PGD for a single recessive disease and you also test for the viability of the embryos, half of the embryos roughly would be suitable for transfer if you just looked at a single gene. If you add in chromosome with the normal embryos, you get to about a quarter of the embryos. If you add in another disease, it gets to about 12.5 per cent, and if you start to look for more than one or two things, you would never have any IVF embryos to transfer. So, we can only look at serious disorders that we know about upfront. We could sequence embryos but frankly, nobody would ever transfer an embryo at that point because there'd be too much information and too much risk. So, we look at really specific medical questions before anything is transferred.
Kat - And also, for many diseases, there are many, many different small subtle variations that all add up. So, I guess something like a test for heart disease isn't really going to work.
Tony - Well, I mean multigenic disorders are very prevalent. Yeah, we can only do single gene disorders. People come to us and ask us to do autism testing. It's a multigenic disease with no known genes that are really clearly loss of function from the majority of autism patients. There's a small subsection of autism patients that have clear genetic disease. That's classic example. You can't and you probably will never be able to do PGD for autism. There's questions that we won't be able to answer and unfortunately, you're back to the old fashioned way of producing children at that point.
Kat - Genesis Genetics' Tony Gordon. And you can find out more about the work of the Progress Educational trust - who aim to raise the public understanding of science, law and ethics around genetics, at
progress.org.uk

18:30 - Mike McNamee - Sporting genes
Mike McNamee - Sporting genes
with Mike McNamee, University of Swansea
Most of us have probably wondered at some point what our kids might be like - whether we want to actually have them or not. But could a genetic test predict their ability on the football pitch, in the art room or in the orchestra? The latest direct-to-consumer kits promise to tell eager parents whether their kid is cut out for certain sports and activities. But, according to Mike McNamee, Professor of applied ethics at Swansea University, they're wasting their money. Kat Arney spoke to him at the recent British Science festival, also in Swansea, to find out why...
Mike - Well, they make a number of claims but I think essentially they come down to this: that we can identify the predispositions of your child towards certain kinds of athletic activities. It's my belief and those of my scientific colleagues that they're predicated on an evidence base that's nowhere near robust enough in order to make those kinds of claims.
Kat - What sort of traits are they looking at to make these claims? What sort of things are they analysing for?
Mike - Well, they're looking for genes which predispose people for example to endurance activities. So they would hope to predict the volume of oxygen uptake or for example, a gene which has been associated with speed and power, ACTN3. But I think in each of these cases, one might query what the precise relationship is between forms of gene expression and the activities to which they're supposed to be predisposed. So, take sprinting. ACTN3 is the gene that's talked about as a gene for speed. But certainly, there's a world famous case of a Spanish world class long jumper who did not express the gene ACTN3. So, can it be a necessary precursor to sprint based activities? It seems not. But even if you do have that gene and lots of us might express it, being a world class sprinter requires a million other things. So, do you have the motivation, dedication, the commitment?
Kat - Do you like sprinting?
Mike - Actually, I chose that one because I think people would say, there is more robust evidence for the association between that gene and the output in terms of the athletic activity. For the others, here's a case of a world class distance runner who had like a 28 per cent output versus 72 per cent output for sprinting activities. So, let's say I was the parent of said world class world record holding distance runner. I'd take my child along to do this genetic test and say, "Okay, sprinting is the future for you. The world would be without this world record if that were the case, in long distance running." So, one has to be careful generating dialogue and discussion from a single case but this is a profoundly damming case offered up by the direct to consumer genetic company themselves.
Kat - How much do these tests cost? And if they can't really tell us that much, it doesn't seem like they're terribly good value.
Mike - Well of course, it's a market. In a market, there are lots of different operators. Certainly the one that I've just shown on the slide there was 100 bucks. That strikes me as an awful lot of money to get something, the results of which are not desperately robust or precise. So if you have a 100 bucks to spare and you wish to do it, that's absolutely fine. I myself, wouldn't.
Kat - There are direct to consumer genetic tests that can tell you about all sorts of things - your risks of different kind of diseases, your ancestry. There are some tests that are now talking about traits like which sport you should do. How do people kind of find their way through this and work out, "is any of this worth doing? What can I get that's actually telling me useful information and what is kind of genetic astrology?"
Mike - Just stepping back for a minute and thinking as a philosopher as it were, the idea that complex human activities are in some way reducible to some particular genetic makeup strikes me as fallacious. To excel in any human activity and let's just think whether it's painting, art, sprinting, whatever, requires such a combination of human characteristics and traits that it strikes me as preposterous that one could reduce these to single genetic expression markers or whatever. So for me, they're an interesting aside. I think any geneticist or sport scientist working within genetics would say for example if you want to be a sprinter, "have a look at the kid and see how they run. You'll get more information from that than you're going to get from the test of one of these swabs?"
Kat - Who are these tests aimed at? Why would someone want to find out these things about a child?
Mike - One might have an idea that one wants the best kind of possible future for one's child. But that's a very, very abstract concept. Moreover, Kierkegaard, the Danish philosopher wrote, "life can only be understood looking backward. The trouble is, you've got to live it forward." How do we know what our children for example would be best suited to until we know what kind of people they are? It's a complex one, isn't it? Because the choices we make early on in life as parents will help to shape a child's future. In that shaping, will open up certain possibilities, will foreclose others. My big worry about these tests is that people will think they have a greater precision and reliability and therefore power, and use them to shape children's lives at such a young age in a naïve belief about early specialisation in its powers that they may have foreclosed all sorts of possibilities that would've made that child's full and meaningful and valuable. And so, the idea of a right to an open future, although it's a liberal idea - you know, there may be other kinds of communities and social forms of organisations in which this doesn't have such a space - but it has a really widely applicable, acceptable, wise - I want to say - fulcrum. That is, don't foreclose opportunities too early. Have a chance to explore not merely what a child is capable of being good at but what they enjoy, what gives meaning to them? And that may well be partly a social kind of thing. What do their friends do? Who are their parents? What were their families doing? In which part of country do they live? I mean, what's the point for being predisposed to be a great skier - whatever that might mean - if you live a million miles from a mountain? So, the idea of these rather complex decisions being somehow tracked back to or reducible to certain genetic markers or predispositions strikes me as a folly.
Kat - Obviously, with something like sport or even art, or music, the instrument you play or the kind of art that you like or the kind of sport that you like, as you say, there's many more factors in it. Are your mates doing it? Is there a running track or a rowing lake near your school? Are there any kind of things we can predict from the genes or should we just let kids try out stuff to see what they're like?
Mike - The latter would be the case for me, but I would want to make the following kind of distinction that the possibilities of finding genetic precursors to certain kinds of clinical conditions, that might be a much richer possibility for these tests. It may be the case that there are some conditions which have so strong a genetic component that we are much more confident about identifying those at an early stage and at least having the opportunity to intervene. Now, it might be the case that you might find the genetic predisposition to a particular condition and not want to intervene. It doesn't follow from any particular genetic test that you must do X, Y, or Z. That will be a human and an ethical choice based upon particular sets of circumstances. One family might choose for example that they did not want to have a child with a particular disabling condition. Another might say, "We don't have a problem with that." So, even when tests are reasonably reliable and valid, there is always a kind of human choice and very often, that test must coincide with some kind of genetic counselling which advices the people making decisions whether it's parents or the individual themselves, as to how best interpret this data in the round.
Kat - In some ways, maybe having a thing on a piece of paper that says, "Go this way. Don't go that way." It's kind of a direction in life rather than this, "Oh my goodness! What do we do? Where do we send you?"
Mike - Well, it would be for people who don't like thinking for themselves. Being a philosopher I'm rather against that kind of predisposition but yeah, I suppose that's part of it, the idea that we can go to some kind of technique or technological expertise which will make the decision for us. That will be attractive to a good group of people. That kind of disposition has to be understood against a much broader canvas about the role of technology in our society, about how we use technology to kind of shape our futures in a way that we think will have greater control. Human life is contingent at its core though. I suspect that that's the kind of sobering one liner for any company that wants to sell their genetic technologies.
Kat - Mike McNamee from Swansea University, speaking to me at the British Science Festival.

27:59 - Gene of the Month - Pokemon
Gene of the Month - Pokemon
with Kat Arney
And finally it's time for our Gene of the Month, and this time it's Pokemon. First described in 2005 in the journal Nature, no less, and found in mammals such as mice and humans, the name Pokemon stands for "POK erythroid myeloid ontogenic." It makes a type of molecule known as a transcriptional repressor, which shuts down the activity of certain genes - sadly, it doesn't make cells look like Pokemon characters, but it does make them behave very badly. High levels of Pokemon can turn healthy cells into cancerous ones - and it's been implicated in many human cancers, especially lung and liver tumours - while cells lacking the molecule are completely resistant to tumour transformation, so there's a lot of interest in developing drugs based on it. Sadly, because games manufacturers don't have quite the same sense of humour as scientists, the company Pokemon USA threatened a lawsuit over the use of their trademark for the gene and it's now referred to as the much more boring Zbtb7. All is not completely lost, however, and another Pokemon-based gene - Pikachurin - seems to have slipped through the net. Gotta catch 'em all!










Comments
Add a comment