In a special show from Cambridge and New Zealand, Hannah Critchlow investigates the research into Huntington's Disease. How has the search to correct a single gene enhanced our understanding of how the brain functions? How are sheep helping to unpick the pizzle of the human mind? Plus we visit a brain bank to find out how tissue donors are supporting the scientific research.
In this episode
01:21 - Living with Huntington's disease
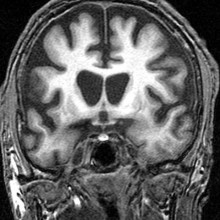
Living with Huntington's disease
with Richard Price
Huntington's disease is hereditary. A single gene change that can be passed down generations from mother or father to their children to cause a myriad of symptoms varying widely from person to person. But with typical age of onset in middle age. Because a single gene is to blame, a genetic test for diagnosis is available which lets people know if they will get Huntington's in later life. To find out more, Hannah Critchlow spoke with Richard Price, whose wife, Heather, started to exhibit symptoms of Huntington's 8 years ago...
Richard - My wife Heather is now in residential care. She started off with not being able to handle stress, even the smallest of issues can make her quite upset. Also, in terms of depression, she suffered from that a little as well. She has what has turned out to be a very aggressive form of Huntington's that has affected not only her cognitive side and her mobility, but also her mental state. So, from that perspective, it has changed quite a lot. She went into residential care about 2 years ago. But, just in the last 6 months, she's been declining in terms of her mental state. It was really just trying to get treatments. So, we're trialling a treatment to try and make her just more comfortable and less upset, and unsettled, which she currently is.
Where she currently resides there are between 4 and 6 people with Huntington's, and they all are so different. You've got one person that you just wouldn't realise, in fact, the GP probably won't realise that they have HD. You've got other people that have the movement issues and you've got people with the emotional and the cognitive issues. Unfortunately, Heather has had all three. Yeah, it's been real tough. Of course, Heather, having watched her mother go through what she's going through, it's been really quite tough on her. She's 43 now. She was tested when she was 18. At that stage, they'd only just discovered how to actually discover the gene and test for it. Heather is a very positive and proactive person, so she wanted to know whether she was going to have the symptoms later on in life. So, it was quite tough, but she got through it. In fact, that helped her knowing rather than not knowing.
Hannah - Did she ever mention that, as a result of having this test and knowing that she was going to develop Huntington's down the line, do you think she led her life a little bit differently because of that?
Richard - Definitely. In fact, that was her purpose. Everything from deciding to get a diploma rather than a degree, so rather than going to a university and really, just getting into the work force and really, just building up a nest egg. When the symptoms really started to appear, she was able to manage that, understand it, and then make some decisions around it. So, she always had planned on travelling. And for a Canadian from the east coast, it's not as common as we have in New Zealand. She sold her house and went travelling and I met up with her in London.
Hannah - Do you have children with Heather?
Richard - No, that was another sort of decision that she made quite early on because it seems that her family may be more prone to passing it down the line. Her brother has it as well. He does have a son. Heather had a lot of time to sort of process and accept that and we're both at the same mind. So, we had dogs instead of children!

06:30 - The gene for Huntington's
The gene for Huntington's
with Professor Russell Schnell, & Lynette Tippett, the School of Biological Sciences in the University of Auckland
Russell - Hi. My name is Professor Russell Schnell and I'm in the School of Biological Sciences in the University of Auckland. I was one of the members of the group that found the gene actually, now 20 years ago. I have to say that - so I'm going to witter on a little bit, but I have to say that the Huntington's disease research community is a little bit special because it's always had very direct input from people or families who were affected by the disease. And so, there's always quite a reality about our research meetings because generally speaking, there's somebody from a Huntington's family or a Huntington's patient who comes along to the meeting and presents in some way that is rather galvanising. It's great, so it's true partnership between the research community and the patients which is as it should be. Many years ago, when we found the gene, that was a collaborative group and great collaboration where we all shared the data prior to publication.
Hannah - We'll find out more about the gene and how sheep were involved in studying it shortly. But first, Associate Professor of Psychology, Lynette Tippett from Auckland University expands on how the Huntington's disease research community came about.
Lynette - It began really with Milton Wexler and Milton Wexler was a psychiatrist in Hollywood. His wife died of Huntington's disease, as did her 3 brothers. He had 2 daughters who are still alive today, Nancy and Alice Wexler. He decided he needed to find this gene and find a cure for Huntington's disease so that he could cure his family or save his family. And so, what he did was he started pulling together scientists from all around and just sort of putting them in a room and making them brainstorm, finding this gene and finding out how to cure Huntington's disease. It was unusual because instead of people fighting for grants and all the competitiveness that goes on in a lot of science, he managed to get these scientists in a room, get them all in the same page, and all just being open and brainstorming ideas. That's really how the Huntington's research field began. So, the gene was finally found in 1993. So, that's 20 years ago. That sort of legacy of a lot of collaborative and interactive and international groups working together, that legacy of collaboration I think continues today. I think it's down to that very unique start to focused Huntington's research that came from the efforts of Milton Wexler.
Hannah - Back to Russell to find out how this collaboration resulted in the successful identification of the gene involved in Huntington's disease.
Russell - Again, it was a partnership between researchers and the families. It was looking at families and looking at people - if you can imagine - like an upside down tree where the gene is inherited down the family. We can follow the inheritance of that particular piece of DNA in a family and look at individuals that got it and individuals that didn't. In doing it with molecular tools or DNA tools, we can narrow the region down until we narrowed it down to a single point. In Jemma Marcey's lab, they found an absolutely convincing mutation or variation in the gene which is like a lengthening of a piece of DNA particularly tract in the gene.
Hannah - So, that lengthening of that one section of DNA was being passed three generations and those individuals that were affected in generations then developed these symptoms of Huntington's and that's how you identified the genetic basis of Huntington's.
Russell - Yes, absolutely and there was one other piece of information that came along with it that really nailed it. It was that on average, if you inherited a longer repeat or this little track, you can imagine that it's like a bicycle chain that gets longer, where on average, when the repeat is longer because it varies between all of us, including people who don't get Huntington's disease. If the repeat is longer, then the age of onset is lower. So, you can draw a curve. If you're unfortunate enough to inherit a very long repeat, say, over 60 or 70 units, then the age of onset tends to be younger than 20. Again, there's a lot of variability with what convicted this gene as, the gene that causes Huntington's disease.
Hannah - And going back to the analogy of the bicycle chain, so the longer the bicycle chain, the less far you're probably able to ride before actually the chain slips off, you can't ride anymore.
Russell - That's probably where the analogy breaks down a little bit because Huntington's disease is a disease caused by - it's called a dominant disease. It means that you only need to inherit one copy of the expanded repeat. There's still debate about whether it contributes a gain of bad function or a loss of good function. The debate I think is falling on the side and this is what I believe as well, that there is a gain of dysfunction. So, almost like one is inheriting something that takes on a brand new but bad function for the cells in the brain.
Hannah - What does this gene usually do in the brain when it's the right length?
Russell - We don't really know. Even after 20 years, we know that it's absolutely required for embryo development. So, if you remove the gene in mice and they don't develop past day 7. We know that it's very likely to be involved in transport in axons. That's the nerves in the brain, so transport of molecules up and along these very long sticky outy branches in the brain. We also suspect it's involved in metabolism of the brain, so the feeding of the brain with glucose. Huntington's patients lose weight dramatically towards the end and on average, over life, they're slightly lighter. There appears to be some sort of metabolic deficit and I kind of favour this. I quite like this theory that in some way, for some reason we don't know, the feeding of these neurons in the brain, the supply of glucose to neurons in the brain is not operating that well. So, this is just another theory, but maybe these cells are being starved of food. But beyond that, we really don't know and I think the reason for that is because it's involved in so many things.
Hannah - Which is why you get this myriad of symptoms with the patients that have got this expansion of this gene.
Russell - I think the range in symptoms and the range of how the disease progresses or proceeds and the age that it presents is to do with, at least in part, how we are able to cope with the gain of dysfunction. I think some people are better able to cope with that because of what they inherited and their environment. Other people are least able to cope with it. A word that's quite often used is plasticity which is kind of a cool word and that it kind of means that how plastic, how malleable your brain is to cope with this - in effect - terrible insult that happens. We know that some people because there's quite a bit of cell loss in Huntington's disease in most cases that people can cope with different amounts of cell loss before the symptoms come on. It's quite remarkable. The brain is quite a remarkable thing.
Hannah - And you're studying this remarkable brain, this remarkable gene and how it's involved in leading to Huntington's with these expansions of the CAG repeats, you're studying it in quite unusual and remarkable animals I believe.
Russell - Yeah, why sheep? I grew up in a farm in South Otargo. Sheep docile, but they're also intelligent. They've got big brains. I could see models wondering around a paddock, eating grass and living an ordinary sheep life until we wanted to look at their brains. And so, it seemed to me, at least for these late onset neurodegenerative diseases or Huntington's disease, is that we could make an ethical model where they live a normal sheep life until they don't, if that makes sense. So, that is just the ethical line that I draw. We knew something about the sheep brain structure and actually, how to manage them in a farming situation. We're good at looking after sheep. We're good at understanding sheep. So, it's a combination of things. The sheep genome or the sheep gene is a little bit closer to human. Also, we knew that we could do behavioural things for sheep because sheep have behaviours or we imagine we could but Jenny has really taken it to a major different level. Well, she's done an incredible job there.
![Sheep Flock of [[sheep]]. These particular sheep belong to a research flock at the US Sheep Experiment Station near [[Dubois, Idaho|Dubois]], [[Idaho]], [[United States|USA]] Image taken from http://www.ars.usda.gov/is/graphics/photos/ (Image Number...](https://www.thenakedscientists.com/sites/default/files/styles/medium/public/media/Flock_of_sheep.jpg?itok=WFw1eqL6)
16:44 - Huntington's in sheep and mice
Huntington's in sheep and mice
with Jenny Morton from Cambridge University, Russell Schnell, Auckland University, Dr. Ailsa McGregor from Auckland University
Hannah - I wanted to find out more about this sheep and how they behave, so I  met up with Jenny, a professor back in my hometown of Cambridge, UK.
met up with Jenny, a professor back in my hometown of Cambridge, UK.
Jenny - Sheep in a flock have a poor reputation. They follow each other, they do daft things if one sheep get stuck in a fence, another sheep will get stuck in a fence, and they also look a bit silly. But I always liken them to teenagers. Teenagers in a group don't always behave perfectly, but you get a teenager by themselves, and they're usually really quite civilised. It's the same with sheep. Sheep in a flock can be very silly. You get a sheep by itself working under controlled conditions. They perform very well. They're very intelligent, a little bit moody, but they understand things. They learn very quickly.
Hannah - So, the kind of experimental tests that you do...
Jenny - We're trying to design experiments that will test cognitive function in decision making in particular. Sheep can do tasks where the rule changes and they can figure out that there is a new rule and what the new rule is and perform accordingly.
Hannah - So for example, if I go down a corridor, I know at the left hand side, there's going to be a little treat for me, a little chocolate bar. And so, I keep going down the left hand side and then suddenly, you might switch that treat to the right hand side corridor and then I'll learn to get on to the right instead of the left. That's the kind of thing you do with your sheep?
Jenny - Yeah, that's almost exactly what we do, except we use coloured buckets. So, we'll say, "If you go to the yellow bucket, there will be a reward. If you go to the blue bucket, there won't be a reward." So, the sheep learn very quickly to go to the yellow and then you can switch colours so you can suddenly present them with a new pair of colours and they have to make a new decision. First, they have to go, "Oh, that's just the colour bucket test. I'll choose one of them and then I can learn what the new rule of these new colours is." What we now do though is we actually use computer screens. So, we don't need to have buckets and they don't have to walk in. We actually just use computer screens and choose symbols off a computer screen.
Hannah - And this type of decision making, it's important isn't it in everyday human life and as we're hearing, it can be affected in Huntington's disease.
Jenny - It's absolutely critical. In fact, that's why I started with two choice discrimination tasks because Huntington's patients can learn to do these sort of tasks that they have trouble with the sort of reversals that you were talking about. So, they learn something, but then when the rule changes, they perseverate on the old rule. So, they'll stick to the same thing they knew and they have great difficulty with flexible thinking. That's why I chose to develop that task for the sheep.
Hannah - I've heard that you've even managed to get some of your sheep playing games of football with proper goal posts and are the sheep counting the goals as well? Are they able to know who's the victorious team?
Jenny - The sheep don't play football with each other but I did teach sheep how to kick a ball into a goal because again, I'm looking for tasks of skill and motor coordination. I also wanted something that sheep didn't normally do. Now, sheep don't normally kick a football. If they see a football on the field, they would be afraid of it because it was weird. But I taught the sheep how to kick a football because I know that it's a good test of balance, coordination, and skill that might be useful for testing balance coordination and skill in the HD sheep.
Hannah - Thanks to Jenny Morton from Cambridge University. And Russell and colleagues developed a Huntington's disease flock of transgenic sheep that he's called the Kiwis. They've been genetically tweaked to contain a short number of CAG genetic repeats. Looking at their brains, they show the same pathology as very early stage Huntington's. Russell is using the kiwi model to help find out how to safely stop full Huntington's progressing by preventing the bad Huntington's protein from accumulating in the brain as he explains...
Russell - So, the central dogma of molecular biology is that a gene in the genome is read and it is read and copied into the stuff called RNA or messenger RNA and then that's get read and copied into protein. If we could remove the messenger RNA, then the message won't go forward and be translated into a protein. Actually, that is the language we use. If you make small molecules of RNA that could stick to the copy carrying the mutation, then the cell has this wonderful mechanism of recognising when two RNA molecules are stuck together and comes along with an enzyme called dicer. It nibbles it and chops it up and then removes it. So, if we can get those small RNA molecules into the brain and they're going to do that by injecting a virus, and, if that virus gets taken up by the vulnerable cells, expressing or producing these small molecules which will stick very specifically to the aberrant or mutant RNA and just chop it up.
Hannah - Thanks to Russell Snell. Exciting studies and the results are expected in the summer of 2014.
As well as sheep, genetically tweaked mice are also being used to study Huntington's. This time though, to accelerate the disease and discover drugs that could help patients in later stages of Huntington's. To find out more, I spoke with Dr. Ailsa McGregor from Auckland University.
Ailsa - So, our mice have also an increased CAG repeat length, but it's 120 repeats. So, it's much, much more than you would see in a human patient because we need an accelerated pathology in the animals to fit with the lifespan of a mouse.
Hannah - So, what are you seeing this mega long CAG repeats of this Huntington gene?
Ailsa - So, we see there's really classical motor impairments that human patients see. We also see very early cognitive problems. So, these mice are not able to learn how to do the motor test that we usually use to assess coordination in these animals. They also really have a lot of problems with what we call delayed dependent memory. So, can you remember this one piece of information in 5 minutes time or in a day's time? They also are very poor in recognition memory. So, recognizing that there is a new object in their environment. We also see psychiatric impairments in these animals which are much more difficult to measure, but we have ways that we can assess that type of behaviour in animal models and our transgenic mice also show a depressive-like behaviour from about 6 months of age. There is a very specific way that we look at depression in mice because they obviously can't tell you how they feel about things. We typically use swim test and the mice will either swim or they're immobile. In this environment, it's quite small environment and they can't generally get out. So, we can correlate time spent immobile or floating with depression and that actually uses a screen by a lot of pharmaceutical companies to look at anti-depressant activity of new drugs. It has a real correlate with human behaviour I guess. So, if you imagine the time spent immobile, like despair or helplessness, we see a lot less of that following our drug treatment that we've been working on so the animals are swimming much more and they're much more active. Another interesting correlation with human patients because other tests that we used to look at shifting strategies or cognitive tests where you have to change the way that you do something. Normally, we survey that strategy shifting type behaviour. It's how they find food. They alternate between different ways of doing things. Our Huntington's disease mice are very bad at that and they persevere with the same strategy over and over again even when it's not successful. The types of compounds that we are interested in are involved in cholinergic transmission which is involved in attention and memory. These compounds, even in normal mice are what we call cognitive enhancers. So, they improve performance in memory tasks and attention to do these tasks. We're also seeing really significant improvements in motor function in very, very elderly Huntington's disease mice. So, we had really expected that by then we would be beyond the point where we could see any benefits, but we're actually restoring motor function in these aged Huntington's disease mice back to a normal aged mouse's performance which is great.

25:38 - Brain Bank
Brain Bank
with Dr. Maurice Curtis, Malvinder Singh-Bains, Auckland University
Professor Richard Faull and Dr. Maurice Curtis from Auckland University have set up a bank of frozen human brains. This contains hundreds of brains from Huntington's disease patie nts and also, healthy controls from the general population. Their PhD student Malvinder Singh-Bains took me on a tour of the research facilities.
Malvinder - Okay, and now we're going to go into the Neurological Foundation of New Zealand Human Brain Bank. Long title but we call it the Human Brain Bank over here. If you just walk this way, through the music and we have all our brain bank freezers isolated in rooms.
Hannah - We've entered into the brain bank room. So, it's got a massive freezer in here which is humming away. You might be able to hear it and there's also a fume cupboard over there where I'm presuming some dissection can take place under very clean conditions. Can you open up the brain bank and show us some of the samples?
Malvinder - I can, indeed.
Hannah - And the freezer is opening up now and it's minus 80 degrees centigrade. So, it's keeping the brains in a very cold condition to preserve the tissue and all the proteins and the genes that are there.
Malvinder - Absolutely and we have a few of these freezers. So, we have the tissue stored in these columns that are kept in the minus 80 freezer and they're all designated with a number and they're all coded specifically. We don't know who these cases belong to for security purposes and also for patient confidentiality. The tissue is kept in these biohazard bags. I'll just open up one of them. So here, we have one tissue block. We've designated it a case of H131. So, in this case, I've picked out a normal one and we've also got the block number on it. So, SM4 stands for sensory motor block 4.
Hannah - So, that's sensory motor cortex. So it's the band of your brain which runs kind of from ear to ear. If you imagine having a hair band on, or an Alice band, that's roughly about where the sensory motor cortex would be. The sensory motor cortex is involved in processing all of the sensory information that comes in through our bodies. So for example, sense of touch, sense of temperature and sense of self as well I think.
Malvinder - Absolutely. Sensory motor cortex is probably one of the most important cortical regions.
Hannah - So, can we open the sample without jeopardizing the integrity of the tissue, but open it and just have a quick look?
Malvinder - Absolutely. So, we have each of our blocks that are wrapped in foil. So, we snap freeze them using dry ice. I think this one has a few layers on it.
Hannah - We're unravelling now the block of human brain tissue.
Malvinder - So, this is a fresh piece of tissue and you can actually see the gyri.
Hannah - Yeah. So, the human brain has these folds in it which almost make it look like a walnut and I can see now all of the gyri. So, those like little folds coming into the brain which almost look like - I don't know - like a river bed that's flowing into the brain with little bits of blood which - that's how the brain gets its blood supply and the oxygen rushing to it and I can see that really intricate details there in this frozen block of tissue. It's quite awe-inspiring actually.
Malvinder - It's very real. When you see the brain this way, you know that this is such a precious gift from a person. You can even see the little tiny vessels on the top of the meninges. If you look very carefully, you can see the little capillaries.
Hannah - And that's how the brain gets its oxygen through this vasculature which lies on almost the surface of the brain.
Malvinder - You can even see the separation between the grey and white matter. The grey matter contains all the bodies of the cells of the neurons and then the white matter contains all their processes. So, all of the connections come through the white matter here and it's just very distinct. We haven't even stained the tissue. You can get so much information just from one block.
Hannah - It's beautiful. Would you donate your brain for medical research for this type of study?
Malvinder - Absolutely. I think the care that we take into the processing of every single block of tissue and just the brain as a whole, we treat these brains like as if it was our grandparents or our parents and I would certainly donate my brain with the knowledge of how well we treat the tissue here.
With the Indian culture, certain different cultural groups amongst Indians, the Indian population, we have beliefs that the blood of our body is sacred and our organs are sacred, that the tissue is sacred. This is why when a person passes away, we practice the art of cremating so in other words, giving everything back to the earth, so sending our ashes into the ocean and then passing on to the other side. So, the sensitive topic of tissue donation i.e. leaving a part of yourself on Earth is very, very different for Indians. So for me, I've actually had an internal cultural battle as well. I actually wasn't allowed to donate blood at a point.
Hannah - Because of your family's wishes.
Malvinder - Yes, because of the cultural commitments and also, the family understanding that blood is sacred. I've brought my parents to the centre and shown them firsthand what we do and also, my parents can see how precious the information is, it's as almost as if that knowledge has armed them with the understanding that we can actually learn so much from what we have.
Hannah - Thanks, Malvinder. Now, over to Dr. Maurice Curtis, Deputy Director of this brain bank on some of the results from the samples to date.
Maurice - One of the things I've been interested in are the stem cells in the brain. These are cells that have the capacity to divide and become any other cell type in the whole body actually. But in this case in the brain, they would normally go on to become either glial cells which are the supporting cells of the nervous system or neurons which are kind of the active unit of the brain. These stem cells we'd always thought were very important during the development of the brain. In fact, it's those stem cells that produce about 160 billion neurons in the course of about 4 or 5 weeks when we are developing in utero. But once you're born, the thought has always been that you don't have any more stem cells in the brain.
Hannah - So, the number of cells in your brain that you are born with, people used to think that that was it for life. So, if you have any trauma or if you do any damage to your brain then you can't replace those cells. That was the traditional hypothesis.
Maurice - That's right. That's what I was taught when I first started at the university. Only a few years later and I can still remember where I was standing when I read the paper in 1998, which indicated a paper that showed unequivocally that the brain produces new brain cells. That was staggering to me and I thought I have to know more about this. And so, we were actually interested in the Huntington's disease brain for the reason that the area that the stem cells reside is exactly next door right - they're neighbours - right next door to the area that actually degenerates in Huntington's disease.
So, you've got this interesting situation where in Huntington's disease, the regenerative area and the degenerative area are neighbours. They're right next to each other. So, the areas that we're referring to when we say the stem cell area is an area called the subventricular zone, it sits right next to the lateral ventricle in the brain that's the fluid-filled space in the middle of the brain. Just next to the subventricular zone is the caudate nucleus. The caudate nucleus is the area that degenerates in Huntington's disease and it normally is involved with mood and movement and hence people with Huntington's disease of problems with movement and also, they can have mood disturbances. And so, we were interested to see whether or not the area that is responsible for regenerating the brain at least during development was upregulated or whether more stem cells were born in that area, in response to the area next door, the caudate nucleus degenerating. And so, we used some special stains and what we found was that the more degeneration that was occurring in the caudate nucleus, the more regenerating cells or the more stem cells we found in the area next door, the subventricular zone.
Hannah - So, it's kind of almost the opposite of what you might expect.
Maurice - Yeah, that's right. So, you might naturally think it would go the other way, but if you think about how skin repairs itself, when you cut yourself, you'd think, well, that's going to kill off the cells. But actually, what it does is it gets the stem cells engaged and they come along and they repair it and within a few weeks, you're left with just a small scar, but not an open wound anymore. Of course, the brain isn't nearly as able to cope with insults, but the process is similar just on a smaller scale.
Hannah - So, what's going wrong with the patients with Huntington's disease then? So, they're having more degeneration in this particular area of the brain, but they're trying to compensate with this regeneration. But why isn't it happening properly so that those regenerating cells are properly getting down into that region, making the circuits and replacing those lost cells?
Maurice - Yeah, so there's a couple of problems there I suppose that the brain has to overcome. Unlike skin which are relatively simple cells, the neurons are highly specialised, very, very specialised and they've actually done their job successfully for 40, 50, 60 years, and they've learnt it. We're then asking stem cells to come along and just replace these cells that have done their job well for a long time and asking these stem cells to find the right place to connect up with is actually quite a big ask. It's a case of too little too late. So, we don't really get the true regeneration that would be nice to be seen there.
Hannah - Is it also something to do with this CAG repeat that Russell was mentioning earlier? Is there some genetic reason for why these new regenerating cells aren't re-circuiting or getting into the circuit properly as well? Is that something to do with the genetics of Huntington's?
Maurice - We don't know. We certainly don't have a lot of information about that. What we do know is that some of the abnormalities that occur in cells with Huntington's disease actually affects stem cells less. So for instance, the Huntington protein which abnormally accumulates in Huntington's disease, that normally is a real problem for neurons. It accumulates because the neurons are very old and they don't have such good ways of being able to get rid of those abnormal proteins, the Huntington. In stem cells, they actually don't accumulate the Huntington. Cells that are dividing don't seem to accumulate these abnormal proteins that occur later in life with diseases like Alzheimer's, Parkinson's and Huntington's. So, the stem cells seem to have a window of being immune to these problems and part of it is just the fact that they're regenerating.
Hannah - So is this finding, will it lead to maybe a treatment where you can start using these stem cells which wont accumulate these misfolded or improper proteins and somehow make sure that they do make the proper connections and kind of get themselves in place in the circuit properly in order to help cure or treat Huntington's and other disorders as well like Alzheimer's?
Maurice - That's certainly always been the desire, is to be able to get new cells in there, a cell replacement therapy essentially. What I guess we've learned from other cell replacement therapy approaches is that getting one group of cells that you put into the brain to connect up with the right target cells is actually quite tricky. It certainly has been done a lot in the past and the hope is that using endogenous stem cells, the brain can direct it themselves and we just help the brain out. So, that's certainly one of the goals. We want to know more about how is it that you actually get the brain cells to do what they would naturally do and connect up in the right places. But part of that is actually understanding what it is that drives a stem cell to make a projection to actually look for a place to connect up with elsewhere. And so, we're studying those features currently.

38:58 - Networking Brain Cells
Networking Brain Cells
with Professor Mike Dragunow, University of Auckland
So, we can examine what's gone wrong in the brains of patients that have had 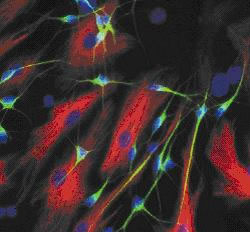 Huntington's and donated their brains after passing away. But there's also other ways that scientists can study the samples. Professor Mike Dragunow is able to culture stem cells that he gets from the brain bank. He also gets brain tissue donated from epilepsy patients who have elected to have surgery to cut out small parts of their brain to help control their seizures. He harvests this tissue and grows the adult human brain cells in a Petri dish to form a network of brain cells.
Huntington's and donated their brains after passing away. But there's also other ways that scientists can study the samples. Professor Mike Dragunow is able to culture stem cells that he gets from the brain bank. He also gets brain tissue donated from epilepsy patients who have elected to have surgery to cut out small parts of their brain to help control their seizures. He harvests this tissue and grows the adult human brain cells in a Petri dish to form a network of brain cells.
Hannah Critchlow asked him, how similar are these cells to a conscious, real living brain. Is this a better approach to studying the brain than by looking in sheep or rats? And can you really compare a culture system to how a fully functional living brain actually works?
Mike - Well, it's always a challenge actually because once you grow them in a dish, you already have a very much artificial environment. But what we can do is we can use markers for the di fferent cell types that we know are present in the brain and see whether those markers exist in the cells in the dishes, and they do. And so, what we're trying to do really is understand how those human brain cells function, their basic biology, because we can test that. So, we're looking at understanding how human brain cells that are involved in a number of neurological disorders, how they behave, their biochemistry. And also, we're testing compounds directly on those human brain cells. Now, one of the big problems in the neurosciences really is that compounds developed in model systems haven't actually translated to humans. So, you have medications that work wonderfully in transgenic models of Alzheimer's disease in mice for example that cure the mice of Alzheimer's and yet, so far at least, none of those compounds have worked effectively in humans with Alzheimer's.
And the approach we're taking I suppose is to try and take a more direct approach if we can actually understand first the biology of the cells and secondly, use those cells to test drugs. The drugs that work on the human brain cells in the dish may - we don't know if they will, but they may be effective in real humans that are living and walking around. So, what we've been doing really is learning how to grow the cells, defining the different types of cells and some cells grow better than others - the dividing cell population that we do freeze down because they bulk up, it turns out that these dividing cells - we're not 100% sure. We're about 95% sure now through a number of different genetic techniques in fax sorting...
Hannah - Sorry, fax sorting. Is that fax as in like faxing something, f transfer of information there?
Mike - No, it's a sort of flow cytometry. It allows you to actually sort cells on the basis of certain markers on their surface. We use that to try and identify what sort of cells you have. Using these approaches, we think that pretty sure these cells that we're growing in bulk here are called brain pericytes. Now the pericyte actually is a very old cell, but a very, very understudied, and under understood cell really because what it does, it actually lines blood vessels. In the brain actually, there's actually a large number of pericytes and one of their functions in the brain to line blood vessels is to maintain the blood-brain barrier. Now, this barrier is very important because molecules in the body and the blood, there are certain molecules you don't want to get into the brain. And so, the brain has this privilege, this blood-brain barrier, the pericytes maintain the barrier and we now know through work by a number of researchers around the world that the blood-brain barrier breaks down in a number of neurological disorders especially in Alzheimer's.
Hannah - So, these pericytes in this blood-brain barrier really stops any toxins entering the brain that might cause damage to the brain and therefore, cause any behavioural problems like seen in Alzheimer's or Huntington's for example.
Mike - That's right, yes and so, people think that once that barrier breaks down, toxins can get into the brain. They can actually add directly to the nerve cell degeneration but they can also activate immune cells in the brain to cause inflammation. We need to study more of the human versions of these inflammatory cells in the brain, the microglia and the astrocytes directly.
Hannah - Which is why it's so important to get these samples from the human brain bank tissue and also from the surgery.
Mike - It's amazing really and our work really is driven by the amazing generosity of the patients who are undergoing surgery and also, the donations that people with fatal brain disorders give to the brain bank. It's incredible and their families. They really drive our work and they also motivate you as a scientist. When you're studying the human brain or human brain cells, you're much more motivated to try and understand and provide some useful answers. And so, that's our approach really, by studying human brain cells by testing drugs directly on them. Our hope is to identify molecules that will work in humans to help reduce and stop the progression of some of these terrible disorders.
Hannah - So, a whole host of brain disorders show an altered immune system, where the brain is effectively being attacked by its body's own defence system. Cases of Schizophrenia, depression, Alzheimer's, and Huntington's all involve the brain being almost on fire with inflammation. And Mike is now working on trying to come up with molecules that will dampen down this heightened inflamed response and repair the brain in the hope that this will lead to new treatments for patients. Next, I speak with Professor Richard Faull who set up this brain research centre at Auckland University to find out how researching Huntington's disease is also helping us to grasp the incredible scale of complexity of the human brain. He tells us what decades of research into the disease have taught him.
Richard - So, Huntington's disease was generally thought to be a simple disease because it was caused by one gene and why there has been so much attention on this gene scientifically and on this disease, was the simple idea that if we could solve this disease by working out what this one gene defect caused, then we could solve diseases like Alzheimer's, Parkinson's, and Motor Neurone Disease which are multiple gene diseases. Well, it just so happens that we now know that this single-gene disease, Huntington's disease is a very complicated disease because it actually causes disregulation and upset of at least a quarter of all the genes. We have 45,000 genes in each cell and depending on what part of the brain it is, will upset different combinations of these other genes you see, that's why you get all the different symptoms. And so, genetics is a very complex science now. We thought it was a simple science when I was at school and that this gene would do just one thing. It doesn't. The gene makes a protein, that protein interacts with other genes, and causes them to change their function or change their pattern of protein production. So, there is a sort of an effect which spreads like wild fire in variable ways. And the variation is affected by the environment. And so, we know that people in different environments, even with the same gene will result in different patterns of brain degeneration and symptoms. And Huntington's disease has taught us the fundamental principle that the human brain is more complex than what we ever, ever imagined. We can't explain a human thought. We can't explain what a sudden burst of genius is, billion neurons talking to one another in complicated ways gives us the conscious personality and gives us and makes us what we are, and we're beginning to unravel that. But it's almost as if we climb to the top of Mt. Everest, thinking we're going to solve this disease and then we see all the Himalayas before us which are even higher. And that's the challenge of doing brain research. It's going to be several lifetimes of work to unravel the human brain. And this disease has actually led us along that path.
Can I donate my living body to research?
Hannah - So, we know that once dead, you can donate your brain and body to science, but what about getting involved in research whilst your still alive? For the answer, we turn to Kate McAllister, a doctoral researcher at Cambridge University...
Kate - So, there are loads of ways in which you can donate your living body to science.
In the most, kind of, straightforward way, you can donate your time to take part in research studies. So, that can be as simple as filling out a questionnaire, helping take part in psychological studies. People are always looking for help with that. The easiest way to go about that is to contact your local university psychology department, and the good thing about that is that most volunteers are also paid for their time for that.
If you wanted to be more literal and, "Can I donate my body to science?" you can definitely donate tissue to some research studies. So, part of the project that I'm doing just now, I'm interested in cellular energy - how our bodies make energy - and how that can later link to dementia, the onset of dementia. So, the best way to look at cell energy is to look at tissue that really is highly dependent on energy. So, what we look at is muscle. So basically, we set this up with the ethics committee and we make sure we go through all the right procedures and then we get people to come up to the hospital and to donate a tiny, tiny bit of their muscle in a sort of outpatient procedure that takes half an hour.
Another way that you may be able to donate your tissue to research is if you're for example in hospital having a diagnostic procedure done, the surgeon may ask beforehand if you wanted to consent to, whilst they're in there, grabbing another little bit of tissue and then that can be sent to a tissue bank and later used for research. So, for example, if you were to have surgery for cancer on a tumour, the surgeon may ask to take an extra piece, or to use a piece of that, in research and that would all be anonymised.
Hannah - Thanks, Kate. So yes, you can donate your living body to research by participating in a study, getting your brain scanned whilst solving a puzzle for example or simply sitting next to a computer and taking part in a survey. Quite often, you'll be paid for your time and you can walk home with a momento, so a snapshot of your brain perhaps.
You can even volunteer to take part in a clinical trial, acting as a guinea pig to help test out new pharmacological drugs. Again, you'll be paid for this or you can donate tissue as part of an existing surgical procedure that you're already having or as a special one-off. You can find out more about donating both your living and dead bodies to research by looking at your local university's science and psychology websites for details or by visiting the website hta.gov.uk.
- Previous Prolactin: Chemistry in its element
- Next Inside Alzheimers










Comments
Add a comment