In this edition of The Naked Scientists, it’s time for the conclusion of our summer series: Titans of Science. Chris Smith chats with England's former Chief Medical Officer and the current Master of Trinity College, Cambridge: Dame Sally Davies.
In this episode

00:47 - Sally Davies: finding a vocation
Sally Davies: finding a vocation
Sally Davies
Sally Davies was born in Birmingham on the 24th of November, 1949. She was Chief Medical Officer between 2010 and 2019, and also the Chief Scientific Advisor at the Department of Health from 2004 to 2016. Her father was an Anglican priest and a theologian. Her mother, a scientist. They both became academics at the University of Birmingham. She attended Edgbaston High School for girls in Birmingham, where she also excelled in science And the viola. Dame Sally's remarkable career has included working on treatment of diseases of the blood and bone marrow. She helped to found the National Institute for Health and Care Research, worked at the WHO and she's now master of Trinity College, Cambridge, where we are meeting today. Let's begin at the beginning then. Tell us about the early years. You ended up as a scientist and a medic. Was that always on the cards or did that happen by mistake?
Sally - I didn't know what I wanted to do. I wasn't very good at school. In retrospect, I've got some funny brain wiring akin to dyslexia. I failed the 11 plus and I only began to shine at O Levels, 15, and then A Levels. I loved playing my violin and viola. I played in the Midland Youth Orchestra. I did wonder when I was young whether I could be a musician, but I had a wonderful violin teacher who when I said 'I think I'm going to do the violin', she said, 'I don't think so. You'll be quite good. You'll be in the first violins, but you have the character to be a leader. Go and find the right thing to do because you're not going to be good enough as a violinist to satisfy what you could do.' So I waited until I got my GCSEs, looked at them and I'd done quite well across the board and sat there on a summer holiday saying, 'oh dear, what am I going to do?' And it was my parents who said, 'why don't you do medicine?' You like people, it's less academic. And of course I was still struggling a bit. So that's what I went for.
Chris - Do you think you do have a funny brain wiring your words or do you think you were just a bit slower to mature? Because we assume that everyone's going to mature and do well at certain stages. But some people do bloom a bit later when they really get into their stride.
Sally - It is true that some people bloom later. I do have some funny brain wiring. There's no doubt. And my daughters have inherited it and needed much more constructive help. I invert letters, I forget names. So what happens is you develop later because you learn to compensate and find ways around it.
Chris - You then decide medicine's going to be the track you take. How did you pursue that? Where did you go to medical school?
Sally - Well, I quite wanted to go to University College, which you went to for a while. But I was too young. My school said I would never get into Oxbridge. So I went to Manchester and had a good training and I stand by it as being excellent training. But it didn't develop me beyond medicine. So after a couple of years there, I gave up.
Chris - You gave up?
Sally - The first couple of years I found quite brutalising. I remember looking after a young woman whose kidneys stopped working, acute and then chronic renal failure. And there was rationing about dialysis and they wouldn't put her on dialysis because they thought she would not abide by the strict diet and everything else. And I found things like that. And the way we handled the interactions was quite brutal.
Chris - So this would've been when you were doing what we used to call house jobs. We're now calling this foundation year jobs. It was early, early junior dr-dom
Sally - It absolutely was. And of course it remains very difficult and the COVID years have been brutalising for that generation in a different way.
Chris - Do you think it was because there were fewer women in medicine at the time? Were you slightly isolated in that respect or was it purely just the emotional brutalising effect? Because it's not just the fact that tough choices have to be made, the hours are worse then than now, but the hours were pretty harsh as well.
Sally - The hours were ghastly, but people supported us in a way they don't do now. My professor was very worried about me at one point and his wife looked after me for a week. I mean it was quite different then. Being a woman was difficult. There weren't many. I still remember the ward's sister on my first ward saying, 'you're a woman, you're here to make my tea. Not the other way round.' But she did make the tea for the men. It was the emotional side that really got to me.
Chris - Yeah, I think many people can identify with that. But that must have been a real wrench then. You'd worked really hard, got through all that, got into a career you thought was going to be right for you, that your parents had endorsed that decision and then you walked away from it for how long?
Sally - Well, I married a diplomat and I went to Madrid for four years as a diplomat's wife and realised I'd made a mistake giving it up. But what a great way to discover that you've got a vacation, which I didn't know before. Meanwhile, I learned all about the civil service. I learned Spanish to ski, to cook. I mean I did lots of things.
Chris - And then, what, came back?
Sally - I came back with him to London. We later divorced, did a course to update my medicine and just got going and became a consultant at the same stage as my own peer group.
Chris - And what discipline was that in?
Sally - I became a haematologist with a particular interest in sickle cell disease in children.
Chris - And what did you do with that?
Sally - Well, sickle cell disease is an inherited blood disorder. That means you are anaemic and you get pain crises and it's prevalent in people who come from sub-Saharan Africa and wherever they have moved to or have been moved to. So the privilege I had of looking after them was of knowing them for all their lives, knowing the parents, knowing the children. One family I looked after a grandmother, the son and his daughter. So I really got to know them and to help them learn to cope with their diseases as at that point there were no real treatments that are beginning to be now it's becoming optimistic.

07:14 - Sally Davies: becoming Chief Medical Officer
Sally Davies: becoming Chief Medical Officer
Sally Davies
Chris - How did you then cross the divide into, I want to say sort of politics, but it's sort of health policy, the road that took you towards being Chief Medical Officer?
Sally - It was a gradual thing. The first thing was I did quite a bit of research at my hospital about sickle cell disease with colleagues out of the blue. I got a phone call, would I go and sit on the Regional Health Authority Research Committee? I think they needed someone who had some laboratory experience. And of course I ticked the boxes of being a woman and various other things. So I went and sat on it and the joke of the secretary who later ended up working for me was I said nothing for a year as I sussed it out and learned how it all went. The next year I started to make comments. The third year I was quite strong because I can be. And so the fourth year they got me chairing it. I did have a bit of impostor syndrome and said, I don't know whether I can, my predecessors had been very famous professors and there I was working in a district general hospital. But that was how it started because then, as I always say, if you work hard and you deliver, then the next job comes along. I was made the director of research for all of North London and then for the whole of London. And eventually I became the director general for research and development.
Chris - Were you still doing much haematology work at that time or did this end up really taking over your life?
Sally - I went on that committee in the early 90s and I gave up seeing patients in 2006. So I managed to combine it for a long time. I didn't want to give up seeing patients, but I realised I could have a bigger impact by moving into R&D and later on the CMO Post.
Chris - And it didn't, well maybe it did, scare you a bit by taking on something of that kind of scale. Because it's a huge job being the Chief Medical Officer, isn't it?
Sally - Well that came in 2010. It is massive. Yes. But the thing about being chief medical officer, I think it holds true for any job. There's the job description and you have to deliver that. But once you're on top of that, you can then think, so how can I, as CMO, improve a lot of people? What can I do that will make a difference? And you have freedoms that most don't have.
Chris - I can remember listening to you on the radio talking about glasses of wine and cancer risk. Did <laugh>, did you expect that? I mean, just remind us what you said.
Sally - What I was doing was talking about the new Chief Medical Officer guidelines on safe drinking. And actually there is a direct relationship between the amount of wine drunk by women and their risk of breast cancer. I mean, it's a straight line. And so I explained that and said, and actually there's truth in it, that I actually often thought as I picked up a glass of wine, 'oh dear, breast cancer risk.' But it's a risk and you take your judgements. Unfortunately, it was interpreted very differently.
Chris - <laugh>. Yeah, I mean it turned into a bit of a joke, but at the same time it got the message out there, didn't it? I remember that. I can hear your voice in my head saying it and because people laughed a bit at what you said, it nevertheless made them think.
Sally - Well, that's true. And The Times published a wonderful cartoon of me being the nanny in Mary Poppins. So yes, we got the message over.
11:27 - Sally Davies: the antibiotic resistance crisis
Sally Davies: the antibiotic resistance crisis
Sally Davies
Chris - How do you pick your priorities though? When you are someone like the Chief Medical Officer, how do you decide what we are going to go after drinking, we're going to go after smoking? Is it just that you look at the statistics and you say, 'well, this is killing lots of people, this is putting lots of people in hospital, this is a problem, this is what we need to go for.' Or do you have a particular formula, or is it a pet passion? You think, 'well, I've wanted to sort this one out. That's going to be what I'm gonna make my mission as CMO.'
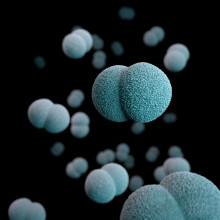
Sally - I think for some people it is their passion. My predecessor did wonderful work on patient safety and that had been a passion for him. For me, some things came round. The then Prime Minister David Cameron was asked in parliament for safe alcohol guidelines. So he said, 'yes, I'll tell the CMO to do them.' So I had to do them. Physical activity guidelines. No one had done them when I arrived and we just felt that we needed to give some guidance. The one which became very much mine and came out of the blue was antimicrobial resistance. So these are superbugs. It's when we misuse or actually use antibiotics properly. Actually, you can probably explain this better than me, <laugh> though I've been at this for years. The bacteria developed resistance in order to stay alive. And then of course people die of these resistant bugs. A lot of people think it's the person who's resistant. It's the bugs that are resistant. And I did with my first Chief Medical Officer annual report, realised that not only was antibiotic resistance and other bugs resistance going up and up and killing more people, but that we had an empty pipeline of drugs. So there wasn't a solution coming. And I've been working on it ever since, even since I stopped being CMO.
Chris - I think I've quoted you more than almost any other scientist, doctor and so on in my career communicating science and medicine because you used extremely frank language and said, 'look, the threat from this is worse than the threat from terrorism.' Which, given what had been happening over the course of the time that you were CMO, that was really saying things. And I think that startling statement helped to crystallise it in many people's minds.
Sally - I've started calling it the Grand Pandemic. After all, we know in 2019, 1.3 million people died of AMR, these superbugs. It's the third most important underlying cause of death in the world. So the idea that infectious diseases are no longer important, COVID scotched, but actually there are all these others which we used to be able to treat very effectively and increasingly we're having problems.
Chris - Did we sleepwalk into this a bit because I'm a bit younger than you, but when I applied to university, I applied to, it wasn't your College Trinity, it was a different Cambridge college. And the 17 year old me sat in their medical school interview and this bloke said to me, 'what do I think the big problems are going to be in the future facing the medical profession?' And I said, bearing in mind I was 17 years old, I said, 'well, I think based on my reading and understanding, we've got a crisis of antibiotics coming.' And I said, 'and I think we are looking at a situation where we might not be able to treat some diseases.' And this guy laughed at me. He told me, I think we're a bit more ingenious than that young man.
Sally - Well, he was wrong and you were right. How very perspicacious of you, I must say. Yes, we've sleepwalked into it. And some of that is the way we'd pay for antibiotics. That most of them are what are called generics. They're made by companies often in India, very well. They do the trick unless there's bacterial resistance, but they're so cheap that it means that health systems, not just ours but around the world, are not used to paying enough money for new drugs that it's worth the companies making them. They make a loss on the research and development. It's not even that it doesn't make them money. And yet it's stupid. We will pay £100,000 to give someone who's got cancer an extra few months of life. But we baulk at £10,000 to save a life from an infection. We just have not thought through our priorities.
Chris - One person who first put me onto the reason why this might be, I sat down with Mene Pangalos from AstraZeneca and he pointed out to me, 'look, we might have to sink 10 billion into making a new drug. We might fail 90% of the time, not because we're no good, but because we're so good that we only fail 10% of the time.' But he said, 'if we come up with a wonder drug and, and we get it on the market, it comes to someone like you pointing his finger at me as a microbiologist and said, what do you do with it? You put it on the shelf and you don't use it because someone like Sally says, you need to keep these drugs as drugs of last resort.' He said, 'either way, we don't make any money. So we're just not able to recoup our 10 billion risk that we've taken or more.' They must have come to you with those sorts of points. So were you able to try and come up with a way to deal with that because it's a broken business model as you've just pointed out?
Sally - Absolutely. So what I persuaded both the NHS and our government to do was to try a new methodology for paying for antibiotics. And we did a couple of pilots that were very successful. Essentially, we put in place an evaluation using NICE but also academics from York University to evaluate the impact of new antibiotics to specific ones on the patient. That's normal. But in addition, on the insurance value of that antibiotic as a fire extinguisher. The value of protecting the whole of that community, that hospital, the community society from that infection. And in that way came up with a larger valuation than you would for an individual. And then multiplied it up by how much we should fairly pay related to our English GDP to the rest of the world. And we've managed to sign contracts with both those companies that each get £10,000,000 a year for the next 3-10 years because it can be renewed after the first three years. And it doesn't matter how much we use it. So we can use as much as we need, but if we don't use it, they still get £10,000,000 a year. The NHS and the patients win. The companies have a steady income. The Americans are looking at something similar. The Japanese announced a pool mechanism, that's what it's called. And if we can get all the G7, the rich countries to do that, then we will have a flow of new drugs.
Chris - One of the problems with superbugs is that, just as we saw with COVID, we've seen with flu, microbes do not need passports. They don't observe borders. They go where we go and sometimes where other animals that carry them go. Antimicrobial resistance is no exception. Therefore, we need a sort of joined up strategy around the world. Have we got buy-in from many countries? I remember going, when I was in America, I went across the border into Mexico early in my medical career and was gobsmacked to walk into a pharmacy and I could buy any antibiotic I wanted off the shelf. That is not going to help.
Sally - Unfortunately, there's still far too much of that. But we are getting traction around the world. I think 115 countries have now got national action plans following work the British government has done with the World Health Organization, Food and Agriculture, Organisation for animal health across the world. And they're beginning to get funding and do things, but still you can go to Africa or Asia and buy antibiotics from a market stall. They may be worthwhile antibiotics, they may be counterfeit. You may only buy one day. All of that drives even more resistance. So we really need to continue to work on this. And I'm very excited because next year on September 24th, there's going to be a high-level meeting. So in the week of the heads of state at the United Nations in New York, we're having a whole day meeting on AMR. And I hope we can really make progress there.
Chris - Has this begun to bear fruit though? Are we seeing that pipeline that was woefully empty begin to be replenished? New drugs coming, new prospects on the horizon to treat some of these superbugs?
Sally - So we've got biotech companies around the world beginning to develop them. So I'm optimistic, but unfortunately we've even had a biotech, who got a licensed antibiotic, go out to business, go bust, because no big pharma bought them because they said, 'huh, we won't make money from it.' So we still have a broken model, though there's some good research coming through. We can do this, but it needs more money. But I promise you prevention and doing this will be so much cheaper than losing all the lives and the cost of not doing it.

20:51 - Sally Davies: master of Trinity College
Sally Davies: master of Trinity College
Sally Davies
Chris - We're sitting in Trinity College, you are master of Trinity College. I think you are the first female master. You are the first person who came in as Master who wasn't a Cambridge person. So it's the first on many levels and you did it in what must be the best timing ever in sort of policy and politics and so on. You dodged the bullet of COVID because you stepped down in 2019 as Chief Medical Officer and came here. You must have thought, my goodness, didn't I get that right?
Sally - I do. I dodged the bullet. So I'm very privileged to be here and I'm delighted that Chris Witty was CMO, not me.
Chris - <laugh>. Why, because you didn't like him? <laugh>
Sally - Actually, I'm very fond of him and we're good friends. I think he's wonderful. I think he did a good job. And he also is much younger. He's got more energy and he's an infectious disease doc. He's great.
Chris - When that kind of thing happens, how long does someone stay as Chief Medical Officer did, did you go, because you said, 'I'm done here. I've done what I wanted to do. I've made my mark. I need a new challenge.' Or do people begin to say in the nicest possible way, again, a bit long in the tooth, you need to look for a new challenge or something.
Sally - So there's a renewal process and that for me was no problem. But I always said it's wrong to stay longer than 10 years. And I was coming up for 10 years when Trinity invited me to come here. And you should go when you are still doing well. You should never overstay your welcome in a job.
Chris - One of my long-term friends said to me, she used to run radio networks and stations, and she said ‘you need to go after a certain period of time because otherwise the problems become your friends.’
Sally - <laugh>. I hadn't heard that one, but I think there is something about going on a high. I had a boss in R&D who after five years left and I said, 'but you're doing a fantastic job. Why don't you stay?' That's the perfect moment to leave. And I took it to heart.
Chris - What are you going to do here in Cambridge? What's in your 10 year game plan here at Trinity?
Sally - Well, I won't stay 10 years. I have eight years maximum as a master for this college. What I want to do is leave us even stronger than we are now. It's not about me, it's about what a wonderful place it is for fantastic students. How to make sure we're giving them the best.
Chris - But you can use this presumably as a springboard to realise a number of things and keep going. Some of the other important work you've been doing. So are you keeping a hand in the CMO work and the other projects you've had cooking as well as bringing to bear other things here?
Sally - Yes. I'm still overworking. So I continue unpaid as the government's special envoy for antimicrobial resistance. And I really do a terrific amount. I'm on the United Nations Global Leaders Group on AMR and things like that. Proselytising. Actually more pushing and shoving and shouting and squeaking anything that'll get action. I want to save lives. I want to look, if I ever have them, grandchildren in the face and be able to say, 'I did my best'. Even better, 'I pushed hard and we sorted the problem.' So I do that, but I'm also co-chairing with Ara Darzi, a commissioner at IPPR, on the links between health and productivity in the economy. It's kind of common sense, but we're beginning to put together the data to prove it. So therefore you need to look at health and people need to see health as an investment rather than a drain on the country.
Chris - So did you know they were going to approach you about coming here and how did that go down. When the offer came in, what went through your mind?
Sally - No, I didn't. I got a phone call out of the blue one August. You know, 'we're looking for a new master.' I said, 'yeah, I know you are.' Because my husband's here. And I said, 'well, yes, you normally have a Nobel Prize winner.' And I started listing people and then this colleague who is a fellow said, 'well, what about you?' And I roared with laughter and said, 'you'd never have me. I'm female. I'm not from Cambridge, let alone Trinity. No, I hope you find someone good.' And so there were repeated phone calls until eventually I said, 'oh, okay, I'll think about this' <laugh>. And here I am. Aren't I lucky?










Comments
Add a comment