Tomorrow's Tech: Biomedical Breakthroughs
This week, new ways to spot cancers much sooner, repair nerve injuries and fix hip arthritis: we’re looking at four major medical breakthroughs waiting to happen. Plus in the news, how advertisers can profile your personality online to boost their sales, and scientists dig up evidence of winemaking from 8000 years ago.
In this episode
00:54 - Resistance: bacterial defence against antibiotics
Resistance: bacterial defence against antibiotics
with Professor David Grainger, University of Birmingham
Antibiotics are at the top of the agenda; it’s been “World Antibiotic Awareness Week” and, as the WHO have put it on their website: “The world is running out of antibiotics. We need to take action to protect human health.” Well, right on cue, researchers at the University of Birmingham have used a new technique to uncover a host of potential new targets against which we may be able to produce new antibiotics to stem the rising tide of antibiotic resistance. David Grainger told Chris Smith what they've been doing...
David - The issue that we were interested in were the mechanisms that bacteria can use to protect themselves from antibiotics. One of the mechanisms that we’ve known about is a pump kind of mechanism, so if you imagine a sinking ship taking on water, a bit like a bacterial cell taking on antibiotics. A common mechanism is just to pump the water out of the boat, as it were, so the bacteria can pump the antibiotics out of the cell. So that was something we knew about, but we had an inkling that it was probably more complicated than that and that other things were happening at the same time and we wanted to try and figure out what those other things were.
Chris - So bacteria don’t just resort to one solution when someone throws antibiotics at them, you’re saying there’s probably multiple things that they do, one of which is to get rid of the antibiotics from within their cells, but there are others?
David - Yes, certainly. Bacteria very seldom rely on one line of defence. Broadly you often find that they’ve got multiple levels of a defence or a certain system to deal with the problem, so they’re very resilient.
Chris - What did you do to try and unpick, apart from pumping things out of their cells, what else bacteria can do?
David - We use a technique which is called chromatin immunoprecipitation and, I guess, you could think about it a little bit like a molecular fishing line, and we can use that molecular fishing line to hook out genes from the bacterial genome that are important for antibiotic resistance. An issue is, okay, we can sequence bacterial chromosomes, we can find out what all the genes are, but what we really need to know are which, out of those thousands of genes, which are the handful of genes that are important for antibiotic resistance. And that’s where this kind of molecular fishing rod came in so we could hook out the important genes and then work out exactly what they were doing.
Chris - What genes did you fish for?
David - We fished for genes that were a target for a protein called “the multiple antibiotic resistance activator.” That sounds complicated but it’s not. What this protein basically does is switch on the genes that you need to resist certain antibiotics, so by targeting these genes we could just identify the genes that we were interested in.
Chris - I see. So this gene turns on when it sees some antibiotics and that, in turn, triggers lots of defence mechanisms all at once by this master switch? So if you follow the scent of what that master switch is turning on, you can then work out what mechanisms the cells is invoking to defend itself?
David - Yes, that’s exactly right.
Chris - And what did you flush out?
David - We got, I think, it was just over 30 genes of interest, and two of them we focused on in detail. Going back to the analogy of the sinking ship, one of the sets of genes that we identified was important for kind of plugging holes in the cell. If you imagine the cell surface as being like the hull of a boat - it’s got holes in that’s letting in water or, in the case of the cell, letting in antibiotics, one of these gene systems, these sets of genes, was able to help plug those holes and stop the antibiotics from getting into the cell.
The other set of genes that we identified were important for repairing the DNA. Some antibiotics work by damaging the bacterial DNA, and we found that one of the sets of genes was important for repairing the damage that was caused.
Chris - Why does this help us in our present situation of facing an antibiotic apocalypse as some people have described it where we’re worried that, in the future, we may have not drugs left to treat things? Why does what you’ve found here help us to meet that challenge?
David - What we can probably do is that now we know about these defence mechanisms we can start to perhaps make new drugs that can target the defence mechanisms.So, if you knockout or hinder one of the defence mechanisms we would expect make the bacteria more sensitive to certain antibiotics. For example, if you take the genetic system that’s important for blocking the holes in the surface of the cell, you can imagine that if you could hinder that system, it might allow antibiotics to get into the cell more easily. It might allow different types of antibiotics to get into the cell more easily; perhaps ones that couldn’t get in there beforehand - things like that. So what we would like to do is target these defence systems and see if we can stop them from working.
Chris - Is that easy to do because is that not what antibiotic researchers have been trying to do ever since Florey and Fleming first came up with penicillin?
David - These are new target that we won’t have searched for drugs to hit before. They’re new system that we can screen for drugs against.

06:24 - Oldest evidence of drinking wine
Oldest evidence of drinking wine
with Andrew Graham, University of Toronto
Are you a wine buff with a penchant for a more mature vintage? If so, you may be interested to hear that archaeologists working in Georgia have discovered the world’s oldest evidence of imbibing. Shards of pottery dating back about 8000 years have turned up with wine residue still stuck to them. Georgia Mills spoke to Andrew Graham...
Andrew - What we have discovered is something that many people have suspected for quite some time for a number of reasons but that we have in the Shomu-Shulaveris culture in the Republic of Georgia during the neolithic, the earliest evidence of wine production in the world. If you want to use round numbers we’ll say 6000 BC, so 8000 years ago. So we’ve pushed the earliest evidence of wine back about 1000 years by this discovery.
Georgia - What did you find and how did you know it’s evidence of wine?
Andrew - Pat McGovern, who is one of our colleagues down in the United States. Pat developed a process by which to look at the residue left by wine on ceramic vessels, and one of the important things you have to remember is tartaric acid. Tartaric acid is produced in the process of making wine, so he developed a process by which he would look at the absence or presence of tartaric acid on the inside of ceramic vessels. We also test the surrounding soil so we can also test if there is tartaric acid in the soil in high amounts. It wouldn’t be a good sample because you could argue that the tartaric acid on the pottery is a remnant of the tartaric acid that is present in the soil. So looking at the soil and the residue give us the fact that the presence of tartaric means that they were storing wine, or wine was in this pottery vessel.
Georgia - Just thinking about what I’m like, how do we know these people just didn’t leave grapes out too long by mistake? Do we know they intentionally wanted to make this drink?
Andrew - Well yeah, it’s used other lines of evidence. Looking at the pottery specifically and the type of pottery it is; looking at the iconography on the pottery, one of the things that is on all of the news wires that is going out, there is a famous ceramic vessel from the neolithic site of Khramis Didi-Gora in Georgia and it’s an iconographic representation of a cluster of grapes on the rim of the ceramic vessel. And of all of the range of symbols and images they could represent on their pottery, they chose to represent grapes.
And to make wine that’s drinkable, and en masse to be able to provide for many people you can’t just leave it out. Anybody who’s left a glass of grape juice out knows that it doesn’t necessarily turn to wine - it will turn to vinegar. Do we understand how they made the wine? No, because what we have is just the residue, the evidence of the process. What we don’t have is a production facility; we don’t have where they were actually making and storing the wine during this period. So they were making and storing it somewhere, we just don’t know exactly where.
Georgia - Are you holding out hope you might discover a very aged vintage?
Andrew - Well I will say, and any archeologists listening to this programme, there’s an axiom in archeology that in any field project your greatest discoveries or the greatest challenges that you have normally appear on the last day. And certainly on our excavations last summer, on the very last day of excavation we were cleaning for site photos etc., and one of our students and Georgian colleagues was being a bit vigorous in their cleaning and did a little bit of excavation and uncovered the top of what appears to be a fully intact vessel. So we were like umm, because usually what we found on this site thus far are fragments of vessels. Unfortunately we had to rebury it because we just didn’t have the time to excavate it, so it’s a treat waiting for whoever is the lucky square supervisor to excavate next summer.
Georgia - Wow - you reburied this pot?
Andrew - We didn’t rebury it - we just recovered it. We put material on top of it, then we covered that with soil. We know where it is, no-one else knows where it is, and we’ll go and recover it.
Georgia - Brilliant! I hope it’s still there when you go back.
Andrew - Me too! Looting is an issue in all countries. We’re very fortunate however, the local communities around where we work. We have a problem of the local herders running their cows throughout site leaving us little treats every day as they move their cows through. But they keep an eye on things for us and so we’re pretty confident that everything will be as it is when we return.

12:27 - Social media: which adverts are targeted at you?
Social media: which adverts are targeted at you?
with Dr David Stillwell, University of Cambridge
If you have a presence on the internet, with a page on Facebook for example, every time you use it you leave behind digital footprints that reveal an enormous amount about your personality; because what you tend to like looking at is being logged. And now researchers have shown that advertisers can use this freely-available data to tailor-make adverts that make you 50% more likely to click on their products. David Stillwell spoke to Chris Smith...
David - What we previously showed is that just clicking on these things, just liking things on Facebook can say a lot about you. It can say how intelligent are you; what is your personality; what makes you unique. So that we’re asking in this study is, given that it’s possible to show those, very, very personal things about you, how can companies use this to advertise better, and how worried should we be as consumers in terms of privacy?
Chris - So if I see something on Facebook and I click “like” against it, you can extract data from what I have like or chosen specifically to flag up as of interest to me, to begin to make deductions about my personality and my likely life choices?
David - Exactly. If you like, for example, on Facebook computers, then obviously you can sell computers to that person. But actually it shows something more personal, which is that people who like computers tend to be introverted. Which means that if you’re selling something that isn’t anything to do with computers, you can use the fact that you know someone is more likely to be introverted to sell products in a way that means they’re more likely to be interested.
Chris - How have you proved that that’s the case?
David - What we did is we worked with a few different companies who were running adverts on Facebook, and we got them to target those adverts at people who we knew were more likely to be introverted or extraverted based on their Facebook likes. Then we changed the adverts to either appeal to introverts or extraverts.
So, for example, we worked with a cosmetic company and we had an extroverted advert, which was a dance like no-one’s watching. It was a picture of a woman in a club, she’s sort of got her hands in the air just dancing around and everyone’s looking at there because she’s the centre of attention, and that’s the ideal for an extrovert.
Then we had a different advert for introverts. This was “beauty doesn’t have to shout.” It’s a woman looking in a mirror; it’s about her own opinion of herself; it’s not about what anyone else thinks, and this is what an introvert looks for.
Chris - And you know that do you that extroverts will engage better with the extroverted type advert, introverts with their focused advert?
David - Exactly. That’s the theory. What we found from targeting this adverts is when the extroverts see the extroverted add, then they are 40% more likely to click and they buy 50% more stuff. Same thing with the introverts but when they see the introverted ad.
Chris - So when you tailor the type of advert that a person sees to the personality of the potential buyer, they’re much more likely to engage with the advert and to complete the sale? Haven’t advertisers known this for donkey’s ages though, this is not new, or is it?
David - What’s different here is that whereas previously you might have a sort of an ideal consumer in mind. If you’re putting an advert on television then everyone who sees that advert sees the same advert. But now, with microtargeting on social networks or the internet in general, you can advertise to a specific person given that you’ve made a prediction about that specific person. So you’re really seeing a very personalised advert to you as an individual.
Chris - I suppose, in some respects, that may be beneficial because it means that I see things that I’m more likely to want to engage with more of the time. You could you use that for good because you could show me positive health messages, for instance, if you wanted to target someone who was at risk of depression, for example, or mental illness you could focus your advertising at that person, reach that person who needed that help. It could be exploited by nefarious operators though, couldn’t it?
David - Exactly. So what we’re saying is that you can essentially persuade someone better given that you’ve got all this information about them that comes from the internet. You can persuade people to do things that are in their benefit so encourage people to save money, encourage people to take advantage of a pension. You can also persuade them to do things that are not in their benefit. If you notice that someone has an addictive personality, you might try to sell them gambling products and that is not going to be in their interest.
Chris - The data that you were exploiting on these users on Facebook because looking at your paper it was huge numbers, like 3 million people is the sample size that you’ve looked at. That data’s freely available, it’s just out there, you can extract that as a third party?
David - Exactly. Any advertiser can go on Facebook and target people who like a specific single product so that’s what we’re doing here. So just given one like on Facebook you’re seeing a specific advert from us. But now imagine that you are Facebook, or you are Google and you’ve got all of the data about one individual, then you can target adverts or products based on everything that someone likes, not just one thing.
Chris - What does the legislation say about this - is this legal?
David - What’s interesting about the data protection act in the UK and also the General Data Protection Regulation that’s coming in across Europe, and coming to the UK in May next year is that one of the key planks is consent to share your information. But what’s missing here is the fact that I click on an advert, I am now telling that advertiser that I am an extroverted person, or I am intelligent person, or whatever information, and I don’t even realise what information I’m giving away by clicking on an advert. I’ve never consented to give that information away, I’ve just clicked it, and I don’t even know who that advert is targeted at, so I don’t know what information I have given away.
18:08 - Do we get a new body every 7 years?
Do we get a new body every 7 years?
For this week's mythconception, Izzie Clarke has been picking apart the myth that we get a whole new body on a cellular level every 7 years...
Izzie - You may have heard that we get a whole new body on a cellular level every seven years. A fresh start? Yes please! Who cares how much you drank in your 20s, before long you’ll have a whole body with new cells and the damage should be written off - right? Wrong.
Your cells are the fundamental building blocks of your body. You have about 37 trillion of them and around 200 different types. The cells on the inner lens of your eyes have been there since you were a foetus, and the neurons on the outer layer of your brain, which plays a key role in memory, attention, and language to name a few, are never replaced.
However, some cells in other parts of your body do regrow. Your skin cells, for example, refresh every two to three weeks, whilst the cells that line your gut are constantly bombarded with acidic gastric juices so don’t last more than three days.
But how did we find out how long cells actually last in our body? The atmosphere naturally contains low levels of a radioactive form of carbon called carbon-14. But during the mid 1950s and early 1960s nuclear weapon tests released large amounts of additional carbon-14 into the atmosphere where it combined with oxygen to form carbon dioxide. Plants have been taking this in, we then eat the animals that eat the plants and hey presto… this radioactive carbon-14 has worked it’s way into the DNA of our cells too.
And because it happened at a very specific point in history, and we know how the levels of carbon-14 in the air have been changing since, scientists in Sweden have been able to use this so-called ‘carbon-14 bomb bump’ to work out how old the cells in different parts of our bodies are. Because cells that are being replaced will have new DNA and, hence, a more recent carbon-14 fingerprint than a cell made longer ago.
The scientists in Sweden found that the average cells in the intestines of an adult in their thirties were about 10 years old, and skeletal muscle cells were about 15 years old showing they’d been replaced several times since those individuals were born. The same tests carried out on brain cells, though, showed that they were as old as the individual, so they weren’t being replaced and if you lose them you won’t get them back.
So there we have it... while some cells do replace themselves over time, you’re pretty much stuck with the body you’ve got. So look after it.

21:14 - Would you commute in an Iron Man suit?
Would you commute in an Iron Man suit?
with Peter Cowley, Angel investor
A British inventor, Richard Browning, who’s the founder of the company Gravity, has built a real-life jet-pack and flown it across a lake, getting into the Guinness Book of Records in the process. Katie Haylor spoke to business angel Peter Cowley - who invests in tech start ups - about the invention...
Peter - The suit primarily looks like somebody who’s on a motorbike racing track, so it’s lots of protection, padding etc. because the chap is carrying six small jet engines or gas turbines. Each gas turbine, which has got an exhaust gas temperature of about 600 degrees centigrade, so you don’t want to get too close to it, is providing enough thrust together about 130 kilos to lift him, his suit, and an amount of fuel with it. He looks like something out of space really; he’s got two on each arm and two on his back to stabilize him.
Katie - It sounds like something out of a comic book. Why make something like this?
Peter - Because he’s an inventor I think and he’s just enjoyed doing that. I had a look on the internet and find you can buy these gas turbines; they’re about £2,500 each. Anybody can buy them; they take jet fuel - kerosene or paraffin; they generate thrust, and they will then push you, lift you in the air, and if you point your arms backwards then they’ll send you forwards.
Katie - Amazing.
Peter - But he’s also admitted that he wouldn’t want to go too high because he has crashed a few times. So, if you look on the videos, he’s never more than about 2 or 3 metres high.
Katie - Yeah. I think on the video he got to about 32 miles an hour?
Peter - Yes.
Katie - But then he went into the lake on one of the attempts.
Peter - Well it’s great actually because that’s a great place to land! In fact, there are two things he’s working on. One is an airbag, so it’s a crash bag a bit like horse riders have and skiers have, so if he does crash then he’s less likely to damage himself. I think he’s probably broken the odd bone as well.
Katie - You mentioned a little bit there, but what kind of novel engineering is required to make something like this?
Peter - I think the most important thing is human courage actually, which isn’t engineering at all. So yes, you can buy the gas turbines, you can attach them to yourself. He’s worked out how to do it such a way that he’s fairly stable. It hasn’t got any auto-balancing so he’s having to do that by learning. The most important part, is protection of course, from these gas turbines otherwise almost anybody could do it.
Now he’s added things to that, so he’s now got a head up display. Because one of the things is if one of the gas turbine’s fuel supply is stopped, he’s suddenly unbalanced and will almost certainly, of course, hit the ground then.
Katie - Ah, oh dear. With that in mind, are these likely to become commonplace do you think.
Peter - I doubt it really because a) for safety reasons it’s unlikely that people will be using them in case they fail, and you certainly wouldn’t want to drop from 50 metres or 100 metres up in the air. And secondly remember there’s an exhaust gas there of 500 or 600 centigrade. Can you imagine what’s that going to do if you get too close to something?
Katie - Oh dear, yeah. It doesn’t sound like the ideal thing for a commute potentially if you’re stuck in a traffic jam or something?
Peter - No, no. There are a number of battery powered drones which is another way of looking at it. The great advantage of kerosene, is actually the fuel density is very, very high so you should, in principle, be able to go much further for a certain weight. Because, remember he’s got to carry the weight of fuel whether it’s the batteries or the kerosene than he would do with a drone.
Katie - Now this, and I think he says it in the video - it’s a bit of an indulgent toy at the moment, but could this sort of tech have more serious and long term applications?
Peter - Absolutely true in that we will have some sort of personal transport through the air. I’m absolutely confident about that. Earlier this year I talked about a battery powered drone in Dubai, which may happen or may not happen, so personal transport… Yes. Using kerosene powered jet engines… Probably not. I don’t know Richard - I’d happily talk to him on the telephone to find out what his view is.

25:53 - Shining light on early cancer
Shining light on early cancer
with Dr Sarah Bohndiek, University of Cambridge
First up, oesophageal cancer. Thousands of people are diagnosed each year with this disease. It’s the 14th most common cancer in adults; it mostly affects older people and tends to present late in the disease course, which can limit options for treatment. But if it could be detected earlier, outcomes are likely to be much better. That’s the approach that Cambridge University researcher Sarah Bohndiek is taking, and she spoke to Chris Smith...
Sarah - What we’re thinking about is trying to augment the vision of the endoscopist. What we mean by that is providing contrast for really early signs of cancer which are currently very, very difficult for the endoscopist to see.
Chris - What’s an endoscopist?
Sarah - An endoscopist is someone who uses a very long, thin flexible tube to look inside the body, and they typically do this in a way that replicates what your eye can see if you were able to peer inside.
Chris - You’ve got one on the table in front of you?
Sarah - I have.
Chris - I presume that’s the thing in front of us. So this is a long tube; you’re threading it down something. In this case you’re threading it down someone’s throat and you’d be looking at the lining of the intestines or the oesophagus but, critically, you’d be looking with what the human eye can see?
Sarah - That’s exactly right. Normally we’re looking with a white light camera that has red, green, and blue colour channels just like we have red, green, and blue cones in our eye. And that has strengths because we are able to signs of cancer, macroscopic signs as the disease is developing, but it also has weaknesses. When the disease is at a very early stage it’s usually flat so it’s quite close to the lining and also it’s often just a slightly different shade of pink from the normal tissue, so it makes it very difficult to spot with only three colour channels.
Chris - What’s your solution then?
Sarah - Our solution is to try to create what we call a multi-dimensional endoscope. So instead of just looking at three channels of colour, we look at a broad spectrum of colour beyond what the human eye can see. In addition to looking at a wider range of colours of light, we also introduce other properties of light. For example, light has a property of angle which is the angle at which it travels through the medium and what we can do with our new technology is also measure the angle of the light. All of these different properties interact with cancer in a different way than they interact with normal tissue. So by picking all of them up we hope to be able to enhance the contrast and augment the vision of the endoscopist.
Chris - Will this be a sort of laser source then so when the gastroenterologist does the endoscopy, they’ll thread the tube down into the person, they can see what they’re doing but, at the same time, you’re able to inject say laser light, or some other light source down the endoscope so it reflects all the way down, comes out the end, and they’re then inspecting the lining of the oesophagus with this extra light added?
Sarah - We can do more clever things with the existing light that they send down. They normally send broadband light down and they bin it into these different channels, so we can already use the existing light source and collect more interesting properties from it. But, as you say, we can also introduce additional light sources, such as laser light, which have nice properties in terms of how they travel into the oesophagus. By using that and pulling out additional information, and combining those two things together, the endoscopist will have their normal white light image which is easy for the eye to interpret. And what we’d really like to do is have an overlay which has a colour channel which essentially has a big arrow saying - “biopsy here, this is a suspicious area”.
Chris - I was going to say, are you going to sort of feed back onto the image that they’re seeing, what your system is interpreting, so it comes out of the endoscope, goes to a computer, that crunches through all the other information coming in and then represents that over the top of what the surgeon can see, or the gastroenterologist can see in plane light, and then you can highlight the bits that you want?
Sarah - That’s exactly right. It’s really important for adopting new technology into healthcare that you think about how it’s going to fit into the existing standard of care. If we’re able to use that existing standard of the white light and feed in all of our information into one really useful image to the endoscopist, it just makes their workflow really, really easy and adds information and adds value.
Chris - What is it about the cancer cells that means they’re different in a way that you can see with these additional light investigations?
Sarah - There’s actually a number of different things. The simplest one is just that the microstructure changes. If you imagine a normal tissue, it has a very ordered structure of cells, as the cells become abnormal and turn towards cancer they proliferate more which means they divide very rapidly. That means they tend to push out and dislodge the normal tissue around and that disorder will interact, for example, with laser light, to depolarise the light which means that it changes and removes the property of angle, and if we measure that angular property we can see that change.
But there are also other properties that change, for example, metabolism. Imagine if cells are dividing really rapidly, they need more energy to be able to do that. There are certain molecules in the body that are related to their energy which you can actually visualise using optics, and we can also probe those if we look at more colour channels.
Chris - We had Gareth Corbett on the programme a month or two back; he’s a gastroenterologist; he’s working on a camera you can swallow. The idea is that rather than people having to have tubes like the one you’ve got in front of you shoved where the sun don’t shine, which isn’t everyone's cup of tea, you can just swallow this thing and it makes it’s own way through your gastrointestinal tract taking photos on it’s way through. Then it beams the pictures wirelessly to a belt that you carry and then you bring that back to the hospital and the doctor can see all of the images as it made it’s way through you, and you don’t even have to retrieve the camera - that’s the other added bonus! Could you take your technology and engineer it into something like that so that you’re not tied to a endoscope because, obviously, the benefit of your approach is that you can perhaps pick up cancer earlier, but that’s only as good as someone regularly getting investigated with an endoscopy, which isn’t ideal, is it?
Sarah - The small device architecture of having a capsule is exactly compatible with our technology. In fact, the projects that’s just been funded develops a new set of optical filters which could be miniaturised and placed into a capsule format if we wanted to. For the oesophagus that’s a bit of a challenge because when you swallow something it travels really fast.
Chris - It doesn’t hang around no.
Sarah - So you do have to think about how you can do that and one approach is to put it on a tether. Other people have shown that if you put the pill on a string and don’t allow it to go too quickly, that allows you to get better quality images.
Chris - But you could use the same approach, albeit perhaps with different filters or a different sort of interrogation of the tissue, for anywhere that you could stick an endoscope. So would this work, for instance, for lung cancer?
Sarah - You could, yes. You could look in the lung, you could look in the colon. It’s very flexible and, in principle, we imagine that we would see similar sorts of contrasts for very early cancers, and there are similar challenges in those diseases as well.
Chris - Cervical cancer as well? That’s a big problem we’re trying to do a lot of screening for that. Could it work in the same way?
Sarah - Yeah, very much so.
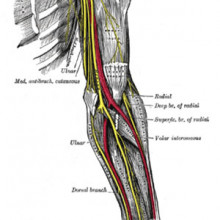
32:36 - Peripheral nerve injury: bridging the gap
Peripheral nerve injury: bridging the gap
with Dr Becky Shipley - UCL, Mr Tom Quick - Royal National Orthopaedic Hospital
Nerves are specialised cells that carry information between the brain and spinal cord, and the rest of your body, including your skin and muscles. They carry electrical signals that enable us to feel things and to move. But if we injure nerves, we can be left with permanent disabilities. When injuries like this happen, often to people’s arms, sometimes the only way to repair a nerve and restore its function is to remove a healthy segment of nerve tissue from another part of the body - usually the leg - and use this to patch up the damage. The injured nerve then regrows using the patched-in nerve tissue to guide it back to the skin and muscles it needs to supply. Of course, this is the neurological equivalent of robbing Peter to pay Paul, because it leaves part of the leg lacking a nerve supply instead. Now Becky Shipley, from University College London, is developing a modelling system to discover how best to grow new nerve graft tissue in a dish so that patients don’t have to get a numb leg to restore functions in their arms and hands in future. Katie Haylor spoke to Becky, and also to peripheral nerve surgeon Tom Quick...
Becky - The gold standard at the moment for treating large gap peripheral nerve injuries is to graft one of these healthy sections of nerve from another part of the patient’s body, and implant it back into the gap between the severed ends of the injured nerve. Although that’s the gold standard, there’s obvious limitations to that in terms of having damage to a healthy nerve for the patient, a second surgery and beyond that, that approach actually only restores full function to the damaged nerve in about 50% of cases.
So instead, what we’re trying to do is to engineer living replacement nerve tissues in the laboratory that we can then implant into the patient instead of using their own tissues. That could be really powerful both in terms of reducing the number of surgeries for that patient but also in how successful the nerve repair actually is.
Katie - Why is it that this hasn’t been done before?
Becky - In this area there’s been a huge amount of research that’s done in labs across the UK and internationally that has explored a very broad range of different materials, so bio-materials and exciting new stem cell technologies, and tried to use them in combination to repair damaged nerves. But, in a sense, it’s almost been too successful so now we’re in the in the position where there are so many different options that it’s hard to try and optimise them using physical experiments in isolation as these experiments that we do in the labs are so expensive and time-consuming.
So what we are trying to do instead is to use a combination of all of this exciting experimental work with computational modeling, so computer-based work as part of the design process to refine how we put together these tissues in the lab.
Katie - Can you talk us through the process of ‘growing’ this nerve tissue? You’ve got cells that you’ve taken from the patient, what else is in that mixture?
Becky - In the most fundamental sense, you can think of it as a combination of cells and materials. So, like you say, we have cells which can be from the patient themselves. We combine them with what we call a ‘matrix’ which is actually a combination of different proteins. We put those together to make what we call a ‘cellular gel’ and it’s like a piece of jelly and that is, essentially, your living tissue.
What we do is we combine them in different ways, and under different physical stimuli to be able to replicate the kind of mechanical and chemical environment that these cells would experience in the body.
Katie - And it’s that that will be bridging the gap that you can’t otherwise bridge?
Becky - Exactly. That’s what we create in the lab and that’s what we would then implant into the repair site. What’s really exciting about our approach is that by introducing the computational modeling we have this whole new framework by which to streamline the design process. In the long term, we’ll be significantly reducing the costs associated with engineering a really effective and transformative nerve repair solution.
Katie - But, as peripheral nerve surgeon Tom Quick points out, there are numerous other costs to having an operation…
Tom - Theatre time is a very expensive resource and quite limited. The time to take these nerve grafts is quite considerable, but then the cost to the patient themselves having lost that function, so having lost the sensation, having extra scars. There’s an awful lot of work yet to be done on exactly the impact of having a scar on the leg when you’re having your arm repaired and how these scars affect people’s body perception and image of themselves. So cost, I think, can be looked at on a number of levels, not just financial.
Katie - So what difference could growing a patient’s nerve tissue outside the body instead of using this grafting process have for someone who’s had a traumatic nerve injury?
Tom - Certainly from my point of view as a surgeon it would give me the ability to have greater options to help patients. A number of times we look to reconstruct nerve grafts and we don’t have the ability to take enough tissue to reconstruct that as we would like.
The ability to have a product that is entirely designed for the patient, to give us everything that we want from a nerve graft from a tissue to fit a nerve gap would be amazing. The tissue that we use currently and we say is a gold standard, we’re actually using sensory nerves to reconstruct mainly motor tissue deficits and we know that that isn’t ideal. We could design it better than what we have now and actually get the right cells to do the right job from the patient themselves, so it could open up a whole new area of clinical treatments.
Katie - So is it fair to say that it might not necessarily be a difference between not being able to use your arm or being able to use your arm, but it could transform the way in which that is done and the consequences on other parts of the body?
Tom - We know from clinical research at the moment that patients’ assessment of outcome doesn’t really relate directly to individual muscle responses, how strong they are and how they recover, but it’s more a global appreciation of how their life has changed. So what we’re trying to do here is give us an awful lot more options to improve the patient experience. It may not make an arm normal; many of the injuries are actually un-reconstructable to bring it back to normal. Sort of a “humpty dumpty” injury, you can’t make it back to what it was before, but it will improve the overall experience of having a nerve injury.
39:57 - A step forward for hip replacements
A step forward for hip replacements
with Dr Sophie Williams - University of Leeds
One of the most successful surgeries ever invented is the total hip replacement; this replaces the ball and socket joint at the top of the leg with an artificial implant. It’s performed in people with severe and debilitating hip arthritis. The downside is that these devices only have a limited lifespan before they wear out and need replacing themselves; and as people live longer and remain active for longer, more patients are needing replacement hip replacements, which tend to be more complicated than performing the surgery the first time around. So is there a better approach? Chris Smith spoke to medical engineer Sophie Williams from the University of Leeds, asking firstly how many people have total hip replacements...
Sophie - If we look at England and Wales, about 90,000 are having hip replacements every year, but if we look at the people who have hip osteoarthritis and may need one of these hip replacements we’re talking about 11% of over 45 year olds.
Chris - So very common; very, very frequently performed surgery which, as people live longer, is going to become even more common?
Sophie - Absolutely, yes. One of the drivers for my research is actually about hip replacements, seeing what we can do to make those better so only one is needed. But, also, if we can go into these patients earlier on and we can make it so that they’re less likely to need a hip replacement.
Chris - But if someone’s hip has worn out and they have arthritis, how can you avoid that happening?
Sophie - We’re starting to see increasing amounts of evidence that some people have hips that aren’t quite as round, aren’t quite as spherical as they should be, and they seem to be more likely of developing osteoarthritis. This is a condition called femoroacetabular impingement. Already now, surgeons are going in earlier when patients present with some early onset of pain and they will start looking at how they can make that hip more round again so the progression to osteoarthritis won’t be as rapid.
Chris - Right, so if you could intervene in these people and not do a complete hip replacement, but you do some kind of resurfacing or refashioning to the hip you could, potentially, prevent the need for a hip replacement and you could do it in people earlier so that they wouldn’t progress to full blown arthritis?
Sophie - Yeah, that’s exactly the case. The thing is, at the moment, whilst surgeons are very good at doing this surgery they don’t really have the scientific evidence to tell them which bits of the bone they should be removing. The problem with these hips when they’re a funny shape is that they impinge. If you imagine going into some sort of extreme of motion - and I’m not talking gymnastics here - I’m just talking maybe leaning down to tie your shoelace, that will cause an impingement between the outer round bit of your head and then the rim of the cup and that outer round will start to cause some damage. So, if we give the surgeons sort of a road map of what they need to remove to make sure we don’t get that impingement, then it’s going to be better.
Chris - How are you able to model what’s going on in a person’s hip then in order to give the surgeon that information?
Sophie - For quite a lot of years now in our labs at the University of Leeds we’ve had hip simulators. These effectively we’ve been putting total hip replacements into them which we’ll continue to do, and we can load them and put them through motion cycles. Previously, we’ve just tended to put these through walking cycles to see how they perform, but what I want to do in this grant is actually starting to take tissue that mimics the tissue in the human body and go to extremes of motion to see when you get the damage so we can then make changes to the hip as the surgeon would do and see if that actually, in reality, really does reduce the amount of damage that we get.
Chris - Will you, ultimately, end up then with a computer model where you could take the scan of the individual, plug it into your computer model, and it will then work out where all of the forces are travelling through their joint and when they were to move in certain positions when it’s likely to impinge or wrinkle up the cartilage in the joint and, therefore, you could make predictions for the surgeon without actually having to lay a finger on the patient?
Sophie - Yeah, that’s absolutely what we want to do. It’s very much about creating a bespoke sort of package for each individual patient because everyone’s got a different shaped pelvis, they move in different ways, etc. The bit we’re missing at the moment is we don’t actually know how the tissue physically behaves so we need this physical experimental simulator in the lab. We need to physically do it and cause this damage in the lab.
Chris - What have you got then: something that resembles a hip joint but it’s sort of sitting with mechanical devices attached to it so you can see exactly how it’s being loaded when it gets moved around?
Sophie - Yeah, pretty much. The exciting part of this grant is I’m going to be collaborating with some manufacturing engineers, so they’re really good at coming up with smart materials that will mimic materials that we have in the body. We can also put various sensors on that so we can look at the forces that are going through the hip. And then, as the shape is changed, we can look at what causes this optimum amounts of change and differences in that. We can actually start to use some tissue in the lab as well - human tissue - and look at the changes you get with that and the damage that’s caused.
Chris - What will you do then; three dimensionally print the structures so that you can get something which is really quite a precise and accurate representation of what’s going on in a real hip?
Sophie - Yeah, that is what we’ll do. We can create the funny shaped bits and we can start to change that shape, and then we can use natural tissue as well on the other side to see what damage you get as you start to apply those loads and motions.
Chris - And you do think the surgeon doing this kind of refashioning and resurfacing maneuver will be easier, less traumatic than doing a total hip replacement?
Sophie - Yeah. I think we'll still need total hip replacements, but it means that we can put them off and we won’t need to use them in so many patients quite so early.

45:47 - Treating diseases wirelessly
Treating diseases wirelessly
with Dr Frankie Rawson - Nottingham University
The human body is intrinsically electrical and almost every one of our cells generates a voltage across its cell membrane that’s used by the cell to communicate with other cells - which is what nerve cells do - or to carry out other important functions, like pumping food into cells and pumping waste out. And as our knowledge of this field grows, scientists are realising that many diseases are associated with a disruption in these electrical processes. So if we can reverse those changes, it might be possible to slow down some diseases; or, by exaggerating these changes, it might be possible to kill off harmful cells, like cancers. Frankie Rawson from Nottingham University is developing new ways to manipulate these electrical effects in the body; it’s a field called “electroceuticals”, and he spoke to Katie Haylor about it.
Frankie - All your cells are electrically active in one form or the other. In your central nervous system it’s based on ion movement, but also cells shuttle individual electrons around just like electrons moving in a copper wire that powers a lightbulb. One thing to note is, in disease there’s a malfunctioning in your electrical communication systems. What changes in those electrical signals is not very well understood. And we’re starting to understand that which means we can now start to develop the technology to modulate that to try and negate problems associated with disease.
Katie - Bioelectric devices are already available: from the well-established pacemaker to the bionic eye that’s not yet currently on the market. But these devices require invasive surgery to get them to where they’re needed in the body which has it’s drawbacks…
Frankie - Doing invasive surgery is not necessarily a good thing: 1) it leads to chances of infection, 2) the electrical components doesn’t necessarily last long so it needs replacement. So if we can develop wireless tools we can avoid the detrimental effects associated with invasive surgery.
Katie - By exploiting the electrical conductivity of cells in the body one of Frankie’s aims is that these electrochemical based wireless tools can be applied to treating diseases including cancer…
Frankie - There’s changes in the way that cancer move electrons around during their disease so what we plan on doing and addressing is if you can control that electron transfer and those electrical communication systems in cancer, you can also halt cell proliferation or even induce cell death to actually kill the cancer and treat it.
Katie - One way Frankie plans to control cancer cell’s behaviour is by the use of conductive nanoparticles. A kind of conductive pill will be taken by the patient, spreading gold nanoparticles throughout the body, and then the ones that reach the cancer cells would be activated by an electromagnetic field being induced in a particular area of the body…
Frankie - We functionalise and synthesise these gold nanoparticles - we’re terming them “nanobombs”. You put them inside the body; they’re taken up by a cancer cell; you apply an external field and that electric field switches on that gold nanoparticle to induce cell death.
Katie - Another proposal is to grow conductive wires within living tissue around cancer cells to enhance the effect of the electromagnetic field when it’s targeted at the cancerous area..
Frankie - We plan on wirelessly growing conductive wires around cells so when you apply your external field, you get an enhancement of that electrochemical effect.
Katie - So how do you ensure you’re hitting the right area of the body with your electromagnetic field, as electroconductivity is so wide ranging, getting this wrong could pose serious problems?
Frankie - The reason that they have to implant electrical devices, so do that invasive surgery, is because the need that electrical device to be close to that area of the tissue that they’re targeting. The idea that we propose, and we’ve already got some preliminary data for this, is to actually use additive manufacturing to build 3D electronics, which enable you to actually target the geometry of your electric field so you can target where that field is going into those tissues so it gives you a degree of selectivity in terms of targeting a specific area.
Katie - So besides cancer, could there be other applications for this wireless electrochemical technology?
Frankie - There certainly are; it’s extremely broad. Just to give you a flavour of where the state of the art is. Of course, we’ve already mentioned the cochlear implant and the potential bionic eye, so that’s controlling neurosignals. But there’s also the work by Professor Kevin Tracey over in the Feinstein Institute in the States, where he discovered there’s a reflex arc that modulates your immune system. So there’s a whole host of treatments now being currently developed for treating arthritis, gut inflammation using electronics. So there is certainly scope to treat a whole host of diseases.

50:39 - Why do we pick our noses?
Why do we pick our noses?
Lewis - Well Patrick, you’ve really got us baffled by bogies. None of the behaviour our evolution experts we contacted wanted to touch such a sticky question. Luckily, Liverpool GP, Dr Laura Wark knows a few things about noses…
Laura - Our noses have two main functions: firstly to improve the quality of air we breath in on it’s journey to our lungs, and secondly to house receptors that provide our sense of smell. Air is filtered, humidified, and warmed on its journey through the nose. Airborne particles are trapped by hairs and the paranasal sinuses produce mucus to keep the nasal cavity moist. Both of these contribute to the buildup of debris in the nose - or snot.
Lewis - Okay. So now we know what the nose does, but what is it that makes Patrick so eager to go digging for gold.
Laura - There isn’t much research into why we pick our noses, but nose picking is common practice amongst most kids and adults. In a 1995 study of 254 people in Wisconsin, 91% admitted to being current nose pickers. Practical reasons may be relieving an itch, or removing nasal obstructions which can affect breathing and smell. However, as 12% of teenagers in an Indian study of adolescent nose pickers pointed out - many people do it just because it feels good.
Although considered an habitual habit in most cases, similar to nail biting for example, extreme nose picking may be considered pathological if it becomes obsessive - medical condition branded “rhinotillexomania,” and picking isn’t without it’s risks. Over-picking can result in septal perforation and the nasal carriage of the bacteria Staphylococcus Aureus is increased in those that enjoy a regular rummage.
Lewis - What about those people who love munching on their mucus?
Laura - A Canadian biochemist has recently hypothesised that the nasal mucus has a sweet taste which may encourage its owner to eat it, thereby introducing pathogens into the body and bolstering the immune system. However, this theory has been refuted by other scientists who point out that humans swallow around a litre of nasal secretions a day anyway, so snapping on snot wouldn’t confer any additional benefit.
Lewis - Thanks Laura; you really ‘blew us’ away.
Next week we’ll be tackling this rocket riddle from Anthony…
Would a rocket launched from a tube, like a bullet from a rifle barrel, be assisted or hindered by that?










Comments
Add a comment