This episode of The Naked Scientists, as infected blood victims are finally promised compensation following the UK government’s cover up of the scandal, we trace the story back to the very beginning, and hear from some of the victims who now have justice...
In this episode
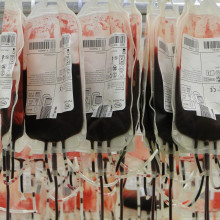
00:55 - How did the UK's blood scandal start?
How did the UK's blood scandal start?
Cara McGoogan
Between 1970 and the early 1990s, 30,000 people in the UK were infected with viruses such as Hepatitis B, Hepatitis C, and HIV after being given contaminated blood products and transfusions. These infections affected two main groups: those with rare blood clotting disorders - such as haemophilia - and people who had blood transfusions after childbirth, accidents and during medical treatment.
A long-awaited report into the scandal - which has been carried out by Sir Brian Langstaff - has just been published, and it doesn’t pull any punches. The inquiry has described the scale of the scandal as "horrifying" and Sir Brian added that "the infections happened because those in authority - doctors, the blood services and successive governments - did not put patient safety first."
How did what’s been called the ‘worst treatment disaster in the history of the NHS’ begin? Cara McGoogan is an investigative journalist and author of The Poison Line: Life and Death in the Infected Blood Scandal…
Cara - So at the heart of the infected blood scandal is people with haemophilia. This is a genetic bleeding disorder that often passes from mothers to sons. And what that means is people with haemophilia don't have a protein in their blood that they need to have a clot. So if you bash your arm, your blood will continue to pool into the space swelling and becoming very painful, because you can't form the sort of mesh needed to stop the bleeding. A lot of people think that might be kind of an external bleed, like if you cut yourself, but that was often the less common version of bleeds. And so in the late 60s, this miracle treatment for haemophilia became available called Factor VIII, and it was made from human plasma and it essentially replaced the protein that people with haemophilia needed in order to be able to live more normal lives, to be active and to be able to kind of go out with friends, run around the street and kick a football without the risk that if the football hits them, they're going to end up with a a very large painful injury as a result.
Chris - Indeed, I went to school with a young man who had haemophilia and he was not allowed initially to take part in many of the activities. It was a pretty isolating experience for him. But by the time we were leaving our first little person's school, this had come in and he was very much able to participate. So in some respects, being given these treatments was quite liberating for people who had haemophilia. I suppose that made it quite attractive as a proposition for doctors to give it to patients to have it.
Cara - Yeah, it was really seen as a sort of life-changing thing. Young kids spent their childhoods laid up on the sofa when they had a bleed. There was this older treatment called cryoprecipitate and you had to wait for it to defrost over hours, it was frozen, and then transfused very slowly and then took effect. And it had more bits of plasma in it than just the Factor VIII. So it took more of it to have as much of a result. So yeah, like your friend with Factor VIII, it was a white powder made by pharmaceutical companies and the NHS Blood Products laboratory. You mixed it with sterile water and injected it and you're almost ready to go again immediately. So, you know, people have told me that they would put it in their backpack and go mountain climbing, like it absolutely changed their lives.
Chris - So with that in mind, was this something that doctors began to actively push on patients because presumably their motives were good ones, they wanted their patients to live longer and have a better health span as well. Fewer debilitating bleeds, more activity effectively, better mental health as well.
Cara - Yeah, it was definitely pitched to patients in a big way. Doctors across the UK were prescribing this from 1973 when it was licensed, and they started to look at new ways to treat them as well. So not just when they had a bleed, which is how they used to have treated them, but also prophylactically to prevent bleeds. So rather than just when you'd had one, you would actually kind of inject a few times a week or a couple of times a month and keep your levels of Factor VIII higher so you could start to see a situation where you might not have those bleeds. And what that meant is we needed more and more Factor VIII in the UK as more patients were kind of brought onto this treatment and started injecting very regularly.
Chris - So where were they getting it from?
Cara - This is where the problems begin. We weren't producing enough of our own Factor VIII in the UK because here you can only donate plasma twice a month and it's a free service. You know, like you go and give blood, you're doing it altruistically to help people. In America they could donate twice a week and they were paid to do it. So America became this kind of centre of the plasma industry, people called it the OPEC of plasma. And they were making Factor VIII to feed the world essentially. So we were importing about 50% of our Factor VIII from America to meet the needs of our patients.
Chris - And who were the donors?
Cara - So the pharmaceutical companies were setting up plasma centres in prisons, in the centre of impoverished areas of American cities. They had mobile trucks that were known to go and park up outside nightclubs in gay neighbourhoods. They were looking for people who were desperately in need of cash and so would be willing to sell their plasma twice a week to fund their lifestyles, whether that's to be able to buy some food or some alcohol. What you found was these people were more at risk of bloodborne viruses. That might have been because of intravenous drug use, sex workers in prisons. You also had people making penitentiary tattoos, which is where you'd sort of get a biro and a mechanism and give someone a tattoo. But you know, they'd use the same equipment across their friends. And so bloodborne viruses were just rife.
Chris - So we've got a situation emerging here where you have an organisation or organisations who are paying people in whom there is a higher prevalence we now know, but perhaps they began to get some insights at the time of bloodborne viruses because of various practices that were prevalent in those groups. What are they doing with those samples? Are they testing the people to make sure they're safe? And how are they then processing the samples to turn them into what they export from America to a range of countries, including ours?
Cara - Yeah, this is quite shocking. So it was deemed not cost effective and viable to be testing these donations for Hepatitis B, which was one of the bloodborne viruses that was known about at the time. They didn't want to stigmatise people, they didn't want to put donors off, and they also didn't want to make it too costly. And so there weren't tests for hepatitis B being done on this plasma. And what the companies did was they took these donations, they poured them into these massive stainless steel vats, and they mixed it together. And then they took off the fraction, the portion of plasma that contained just the Factor VIII, and made this treatment, this medical treatment. But they pulled tens of thousands of donations together and you only needed one person to have a blood borne virus to contaminate the whole batch. So what they were doing was really amplifying the risk of the blood products for patients.
Chris - And that was what was being bought by a number of countries, including the UK for treatment of their people with haemophilia.
Cara - Exactly. And this was known at the time. In the mid 1970s, there was an investigative documentary called World In Action broadcast in the UK. And it showed donors in America giving plasma who had been infected with hepatitis themselves. And so there were warnings here that this imported product was highly likely to give patients illnesses. And then you see school children in the UK turning yellow with jaundice after being treated with Factor VIII.
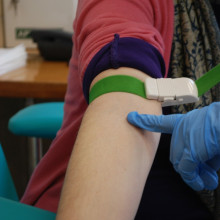
09:27 - Who did the UK's infected blood scandal affect?
Who did the UK's infected blood scandal affect?
Andy Evans & Joan Edgington
There was very strong evidence - both from America but also here in the UK - that the blood products that were being used were putting people at risk from both viruses we did know about at that time, but also ones we hadn’t discovered yet including HIV. So, what happened to some of the people who were infected with these blood products in the 1970s and 1980s? We put in a call to one of them…
Andy - Hi, I'm Andy Evans. I live in Worcester and I'm a haemophiliac who is infected at the age of five with HIV and hepatitis c. I developed full blown AIDS when I was 16 and went through four years of not having any treatment for the actual HIV and the AIDS, just firefighting the symptoms and the illnesses that came with that syndrome.
Chris - How old are you now, Andy?
Andy - I'm 47 now.
Chris - So when you were infected at the age of five, how did you find out that something was wrong?
Andy - I didn't know myself until I was 13 and I was told by my parents who in turn were told by my consultant. And the reason my parents told me was because my blood tests were showing that there were signs that HIV was impacting upon my immune system. So they use a count called CD4. They measure that immune receptor to measure what your immune system is doing in terms of HIV. And that was becoming dangerously low. And because they had to put me onto AZT, which was the only drug available at the time, they thought it would be <laugh> probably a good idea to let me know about that.
Chris - How did you manage to stay alive? You've bucked the trend because many people in your position have not been as lucky.
Andy - That's right. According to the figures that we have, around 1,250 people from the haemophilia community alone were infected with HIV and less than 200, probably about 175, are left alive now. So in that sense, I'm extremely lucky. I don't know why I have been selected out of all of those to be one of the survivors. And I ask myself that on a regular basis. I've been HIV positive now for 42 years. That's 90% of my life. And yeah, it's, it's a very strange thing to have to contemplate.
Chris - What would the alternative be if you hadn't had the treatment that you had, which unfortunately infected you, what would the outcome for your haemophilia have been?
Andy - Fortunately, even though I'm a severe haemophiliac, I've never really bled very much. I have been on haemophilia treatment for all of my life, but I've never had it in a prophylactic way. Really, it's only ever been on demand and I've been told that I use a lot less Factor VIII than the average severe haemophiliac. My joints are in good condition, which is not something that can be said for a lot of haemophiliacs of my age. I have to say that really, had I not received that Factor VIII at that time, I don't think it would've had a massive impact on my haemophilia prognosis.
Chris - Did you know that you'd been infected? As in, did anything happen to your health that your parents in retrospect think 'Yeah, there was this time when Andy suddenly went off color and had a whole bunch of symptoms and looking back, that's probably when it happened.'
Andy - We think that maybe before I was infected with the HIV, there was a period where I was jaundiced. We think that was possibly down to hepatitis B, which I self cleared luckily. But obviously my parents were on the lookout. My dad had read in the New Scientist that there may be HIV coming through blood products from the United States. And so he actually told me at one point, please look after yourself so you don't get a bleed. We don't know what's in this blood. But I don't remember becoming ill and my parents have never told me about it either. So it was not really until they were told about it that it was confirmed that I had got HIV through it.
Chris - And how did they cope?
Andy - My parents were pretty good. They tried to shield me from their own worries as much as possible, but of course as my illness progressed they were impacted financially. My mum had to give up work as a teacher to look after me. She spent most of the time in hospital with me at the Children's hospital while I was in for those four years. My dad still worked, but he would come visit me at all hours of the day and night. My sister, who was younger by four years than me, was very much left to bring herself up and that's carried consequences into her adult life as well. It really has impacted the entire family around me, and I know that's the same for a lot of people involved in this scandal as well.
Chris - And what about you personally? What was it like being a teenager? Seeing the world through a teenager's eyes, but also knowing I have AIDS, that this may be life shortening, probably will for me. You didn't realise that science was going to ride to your rescue. So what was going through your mind?
Andy - I think I'd come to terms fairly quickly with the fact that I was going to have a shortened life. But it's strange because when you become a long-term patient like that and you start suffering opportunistic infections and then worse, fever starts climbing to extremely high levels. I mean, I was blue-lighted into the hospital every couple of weeks really for one infection to the next. I mean, you adapt to it. And all I could think about during that time was trying to reach the next day and what I'd have to do to survive, whether it be putting a nasogastric tube down my nose into my throat and into my stomach to make sure that I didn't lose too much weight, whatever I had to do. It was just a case of firefighting for those four years. And that was the only task that I had in front of me. And so I got to it.
Andy Evans from the Tainted Blood campaign. And luckily Andy managed to hang on for long enough for the modern combination drug regimens we now have for HIV to become available, which suppressed the virus and restored him to full health, which he’s enjoyed since. But , this is actually a story of two blood scandals. The second of which saw people contract viruses - predominantly infection with a previously undiscovered hepatitis virus called hepatitis C - following blood transfusions. But this too was avoidable because the lessons emerging from the people with haemophilia should have sounded the alarm loud and clear much sooner to policymakers. I’ve been speaking with Joan Edgington about what happened to her after she became ill following a routine surgery that required a blood transfusion in 1991…
Joan - I was in my thirties. I was a single parent of two girls, and I had a full-time job as a youth worker. So lots of demands, but still, you know, had been very <laugh> fit and expected to return to that level. And then it was in 1994, I had a letter from the transfusion service inviting me in for a screening blood test connected with a transfusion I'd had. So I went and I think in a way I just assumed it was a sort of general check then waited for the results and was invited back to the hospital. A gentleman in a white coat took me into an anteroom, sat me down and said, 'we do have to confirm that you have Hepatitis C, and it was from a contaminated blood sample.'
Chris - And how did you react when you were given this news?
Joan - It was a very straightforward, not unkind, but a very straightforward businesslike 'this is a bloodborne virus. Do not share toothbrushes, do not share razors, and be careful of blood spills,' which for women, it's a harder thing to manage. I guess it was over sort of 10, 15 minute chat and I left and I remember sitting in the car park for a good half hour just thinking, what on Earth does this mean? And, in my story, I'm very fortunate that I had a very kind, supportive GP. And I do remember eventually making an appointment by which time I had got round to thinking a bit more rationally about it. And I just had a whole load of questions. And he was very upfront with me and said, 'I don't know, but I will help you find the answers.' And it very quickly became evident that this virus had the capacity to kill people. And I do remember, as I say, as a single parent, just thinking that just mustn't happen to me. My mother had died when I was in my early twenties, and I didn't want that sort of thing to happen to my daughters.

19:28 - When did doctors notice the problem with infected blood?
When did doctors notice the problem with infected blood?
Tim Wreghitt
The NHS website says that: “If you had a blood transfusion or blood products before 1996, there's a chance you may have been given infected blood. This could mean you were infected with hepatitis B, hepatitis C or HIV.” It adds: “Today, all blood donated in the UK is screened using very rigorous safety standards and testing to protect both donors and patients.” So, when did health professionals become aware of the dangers of contaminated blood? And are investigators satisfied that measures are in place to stop such a healthcare disaster from unfolding again? I went to speak with Tim Wreghitt, a retired consultant clinical virologist at Addenbrooke's Hospital and was working professionally when all this was happening...
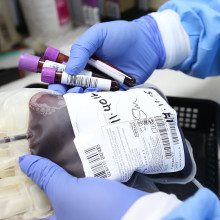
23:56 - Are victims satisfied with the blood inquiry findings?
Are victims satisfied with the blood inquiry findings?
Andy Evans & Joan Edgington
What have the victims of the UK blood scandal - who have been campaigning for decades - made of the inquiry’s findings? Here’s Andy Evans…
Andy - It almost seemed that everything that we had been telling people and shouting from the rooftops for the last 30 to 40 years had been written down by this ex high court judge and signed off as part of the inquiry process. I feel vindicated for all the years that we've been pushing the injustice that has happened to us. We hope now that people will start to think that they can actually have a voice, whereas they felt they couldn't before.
Chris - And where now for you? What will you do next?
Andy - I don't know. I think there's going to be a little bit of digging into both the report, which is enormous. So we're going to have to take time to read through that. And we'll be working with Sir Robert Francis, who's heading up the infected blood compensation authority over the next few weeks to see if we can iron out any ambiguities and the levels of compensation that will really allow people to use this as a turning point in their lives and maybe start to heal from it. But what comes next? I don't know. I think I'm going to take a break for a couple of weeks now. We're going to Portugal for my mum's 70th birthday. When I come back, hopefully I'll have a bit more energy to decide what to do with everything. But people are still wanting prosecutions for people who were involved back in the day who made these decisions, particularly licensing authorities and the ministers that declared that there was no comprehensive proof that there was a link between haemophilia products and HIV when the warnings were there. So there's plenty to get our teeth into. I really hope at some point though, I'll be able to let this go and put it down and maybe think about trying to live the rest of my life for me and my family.
Andy Evans. Let’s conclude with the thoughts of Joan Edgington who told us about her hepatitis infection a little earlier on…
Joan - The first time I was in the room with thousands of people who'd been through similar experience, who validated all the issues and struggles, that in itself was worth everything to me, to then find out that the inquiry team were tackling it with full heart, total integrity, have absolute admiration for Sir Brian and the whole team. We then come to the recent publication of the report, and it's more than we could have hoped for. He has gone into such detail and has pulled no punches. And the key word that so often is repeated amongst us is validation. We were telling the truth all along.
Chris - And where does this leave you? What will you do next?
Joan - <laugh>, that is such a good question. You can tell by my voice I'm really, really tired. Immediately I will rest up. I then think I will take time to grieve. Too many people died. Too many friends died. And then if needs be, I would gladly join another campaign that's looking at holding those in power to account and getting them to use honesty, integrity, transparency, and all those wonderful words. The system has to change. Nobody should go through this kind of inquiry again, even though we had the very best team behind us, it has been a long, exhausting, and often traumatic process.










Comments
Add a comment