Will We Beat Alzheimer's Disease?
Alzheimer's: A third of the population may be destined to develop this form of dementia, which robs people of their memories and independence. So what causes it, and what can we do about it? Plus in the news, NICE approves a new drug for an aggressive form of lung cancer, we've got the lowdown on the Nobel prizes, and how a computer code has been released online that could be using your devices to launch cyber attacks.
In this episode
00:58 - Osimertinib halts lung cancer
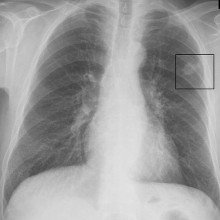
Osimertinib halts lung cancer
with Dr Alastair Graystoke, Newcastle University
A new drug to combat one of the more aggressive forms of lung cancer has been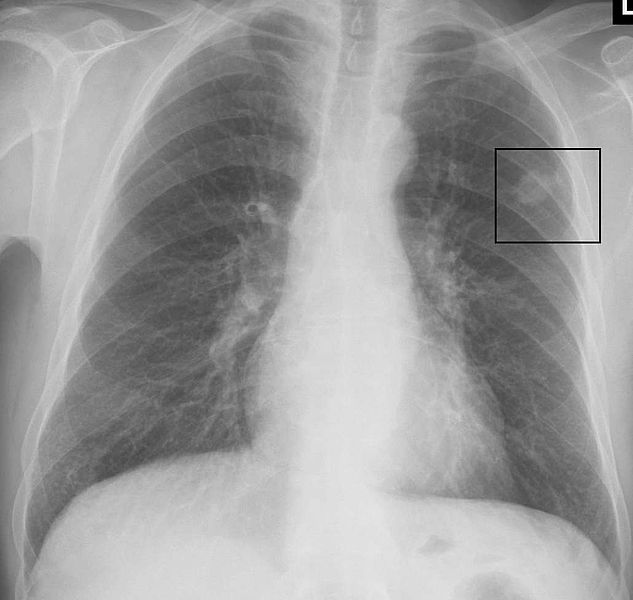 approved by NICE - UK's the National institute for Health and Care excellence. It's been developed at record-breaking speed by AstraZeneca and, in clinical trials, almost twice as many patients responded to the new agent, called osimertinib, compared with existing chemotherapy. Cancer specialist Alastair Graystoke, one of the investigators who has been testing the new agent, told Chris Smith how it works and who might benefit...
approved by NICE - UK's the National institute for Health and Care excellence. It's been developed at record-breaking speed by AstraZeneca and, in clinical trials, almost twice as many patients responded to the new agent, called osimertinib, compared with existing chemotherapy. Cancer specialist Alastair Graystoke, one of the investigators who has been testing the new agent, told Chris Smith how it works and who might benefit...
Alastair - Osimertinib is a new drug that's become available for patients with a rare type of lung cancer. It's lung cancer that's got a mutation in a protein called epidermal growth factor receptor. This protein is like a switch that turns on and then drives the cell's growth, makes it grow, makes it spread, divide, cause symptoms to the patient and this tablet (Osimertinib) goes in and blocks that protein and stops the cells growing. The lung cancer cells seem to be addicted to this - what we call oncogene addiction - and so, if you can block this signalling, you actually see the cancers shrinking and patients feeling better with a better quality of life.
Chris - How do you work out who might benefit from it?
Alastair - When patients first have their lung cancer diagnosed, then they have their cancer checked for a mutation in this protein. They can then go on to drugs that we have had for about four or five years that target this protein, but they only work for about a year and then this cancer becomes resistant. So what's neat about this new drug is we've worked out how the cancer becomes resistant, and the answer to that is it's developed a secondary mutation in this protein that blocks the binding of the drugs we used to have.
So what AstraZeneca have done is develop a new drug that targets the new mutation, the new switch, and is very effective. The other really neat thing about this tablet is that, at the same time in the clinical trials where they were looking at biopsies, they were also doing blood tests to look for the presence of tumour DNA in the circulation. And they were able to show that if you can detect the tumour DNA in the circulation, it's just as good as doing a biopsy. So in fact, there's some patients now who won't need a biopsy - we'll just do a blood test and show this is how their cancer has become resistant and now we can give them this new tablet with a good chance of responding.
Chris - And when someone is started on this sort of therapy, what sort of outcomes are you seeing with it?
Alastair - So, in about seventy per cent of patients we see what we describe as a good shrinkage, which is their tumour volume decreasing by about half. In some of the patients we've actually seen their cancer shrinking down so far that we're having really difficult seeing it anymore. It doesn't work for everyone and, at the moment, we're not really sure how long it works for but it seems to be about an average of a year and then the cancer can, unfortunately, become resistant again.
Chris - What about cancer that has spread to distant sites - metastasised to other parts of the body - does it work on those distant tumours as well?
Alastair - Most of my patients to have metastases; most of them present late with cancers that are already spread. But what's really interesting about this drug as well is that it's very common for patients with this subtype of tumour for it to spread to the brain and the spinal cord, and this drug seems to work very well in that setting as well.
Chris - How much does it cost?
Alastair - So the list price is between four and five thousand pounds a month. It's been made available to the NHS through the Cancer Drugs Fund because NICE didn't think that the data was mature enough; we don't know how long this tablet works for to work out if this is a cost effective treatment. So it has two years approval through the Cancer Drugs Fund and, hopefully, during that time we will develop enough data to show that it can improve patient's outcome, and that they do live longer, and that it's a cost effective treatment to use in the National Health Service.
Chris - Most of the cost, of course, comes from what's involved in developing a new drug, isn't it - tell us about the story of the development of this one?
Alastair - Well, the nice thing about this is that, on average before it's taken about ten years to develop a drug through clinical trials and that ten year process, and the costs behind it, is one of the main reasons that the drugs are so expensive when they come out the other side.
This drug first went into patients in 2013, and it got licensed in the US in 2016, the UK 2016. So it's only three years from first time in man to us having access to it in the NHS. Now if we can do that for all our drugs, hopefully it will bring down the cost of drug development and bring down the costs when they come out the other side.
Chris - Why was it so quick?
Alastair - I think because there was a really nice scientific rationale: we knew what the basic science was; the drug is very effective; has relatively little in the way of side-effects. And there's been new processes brought on by the FDA in America and the European Regulatory Authorities to fast track drugs like this which look to be very effective so we can give them to patients as soon as possible.

05:28 - Nanomachines win chemistry Nobel Prize
Nanomachines win chemistry Nobel Prize
with Khalil Thirlaway, Naked Scientist
This week the top accolades in science, the Nobel Prizes, have been announced.  Khalil Thirlaway reports...
Khalil Thirlaway reports...
Khalil - The Nobel Prize for Chemistry has been awarded this year to Frenchman Jean-Pierre Sauvage, the British Sir Fraser Stoddart and the Dutch Bernard Feringa for their work on the world's tiniest machines.
You might think that computers, phones and other gadgets have become pretty compact in recent years, but that's nothing compared to what these three scientists have achieved. Their pioneering work has led to the creation of miniature machines the size of molecules!
Most molecules are held together by bonds which hold the atoms tightly together, but to make a machine you need parts which can move relative to each other, like wheels and hinges.
Sauvage took the first step when he joined two ring-shaped molecules together like links in a chain. This structure allows the two rings to move around just like chain links would. This showed that molecules could be joined and still retain their mobility, but two linked rings aren't in themselves a particularly useful machine.
Stoddart built on this idea and came up with a structure which looks and acts like a wheel on an axle. A ring-shaped molecule was able to rotate around a long, thin molecule. Stoddart had literally reinvented the wheel!
Feringa then took the field a leap further still when he invented the molecular motor. This extraordinary light-powered motor has sufficient power to move objects much larger than itself, and Feringa has even designed a so-called "nanocar", a four-wheeled molecular structure that can drive forwards when activated by light!
The field of molecular machines which Sauvage, Stoddart and Feringa pioneered is still in its infancy, but its potential applications could impact every aspect of our lives. The ability to create such miniscule machines opens up a whole world of possibilities in materials, medicine, engineering and many, many other fields.

07:35 - Biggest cyber attack ever launched
Biggest cyber attack ever launched
with Peter Cowley, Tech Investor
Last month saw one of the biggest malicious attacks the web has witnessed on  the French internet hosting company OVH. Hackers hit the system with data requests at the rate of a terabit per second at the site, swamping the servers and causing huge disruption. Now the code used to launch the attack has been released online. As a result there are fears that these types of attacks could be about to mushroom. Peter Cowley explained how they did it to Kat Arney...
the French internet hosting company OVH. Hackers hit the system with data requests at the rate of a terabit per second at the site, swamping the servers and causing huge disruption. Now the code used to launch the attack has been released online. As a result there are fears that these types of attacks could be about to mushroom. Peter Cowley explained how they did it to Kat Arney...
Peter - It's actually called a "distributed denial of service attack." The distributed means it's comes from various directions and denial of service means that it's been overwhelmed and, therefore, responds very slowly. So, if you went onto it as a normal user, something that would probably take a second to build might take hours, and hours, and hours, and the amount of data, as you said, is in the terabyte level.
Some of us will remember the Encyclopedia Britannicas which was a printed encyclopedia that was probably about three feet long on the shelf. It's possibly only for the older people because it's online now. But that actually works out at about three hundred and fifty-four sets of Encyclopedia Britannicas per second being shot at the server, which actually weighs nine tons as it turns out. So it's a huge amount of data.
Kat - This attack, so sending all these requests like: come on server, tell me, tell me, tell me stuff - that's coming from individuals people's devices that have been taken over and they might not even know it. How does that happen - what's going on there?
Peter - Yes. So what they did, they scanned the internet and found a hundred and fifty or so thousand webcams; not the ones that are built into a PC or laptop, that had not had their default passwords changed. And this is the biggest lesson you can learn from today - change your default password on these pieces of connected home kits. Then they alter the internal address from where the camera is sending its video data to the OVH server, presumably, and so it was streaming a hundred and fifty thousand sets of video at the same time. That is a huge amount of data.
Kat - So you've said "they did this." What do we know about who they are?
Peter - It's difficult to say. There's a guy called Krebs in the States, who's a journalist, who's well known for saying things about terrorists which, shall we say, they don't want to hear, and don't want to be publicised. His website was being hosted on OVH. Who was doing it? - don't know - that hasn't come into the public domain yet.
Kat - What risk does that have for us as individuals? Obviously, it's very, very inconvenient, potentially very bad for companies if their servers are under attack like this.
Peter - What's the risk? The risk is that something can be seen that you don't want to be seen. So, for instance, I had a look online and there's a website which actually shows a picture of the radio telescope array near Cambridge, which is off one of the cameras on the site there. Hacking into cars we've heard about, so there's a whole stack of things that potentially could go wrong. Of course, go back to what I said - change the default password.
Kat - So that's basically the key piece of advice here is if you have any device that's going on the internet, change the password. Do we need to change them regularly? What's the best way to protect yourself with passwords?
Peter - Well first of all, if you really are worried about this, don't buy one of these devices. But, on the basis that the benefits outweigh the risks, then the first thing to do is change it's default password and then secondly, is to trust the cloud system it's connect to to be good enough to protect you in that situation.
So, on the basis that we're moving towards a more and more connected life with our phones and then a billion or so connected devices in time, we have to trust the companies to protect us.

11:16 - Bagels and the Nobel Prize in physics
Bagels and the Nobel Prize in physics
with Khalil Thirlaway, Naked Scientist
Three Brits take the Nobel Prize in physics for their discoveries on abrupt  changes in the properties, or phases, of ultra-thin materials. Khalil Thirlaway reports...
changes in the properties, or phases, of ultra-thin materials. Khalil Thirlaway reports...
Khalil - This year's Nobel Prize in Physics was awarded to David Thouless, Duncan Haldane and Michael Kosterlitz for their work on exotic states of matter. All three of these scientists were born in the UK and Cambridge-educated.
In the matter which makes up our world, changes in temperature affect how particles interact. This affects properties like how well they conduct electricity, which tends to get better as they get cooler, because the particles are bumping around less so the electrons can flow more smoothly.
But at extremely low temperatures, close to absolute zero, things get a bit freaky. The effect of heat on the behaviour of the particles shrinks so much that it almost disappears, and the quantum effects, which are normally only visible on a tiny scale, are revealed.
It's one of these strange phenomena that Thouless, Haldane and Kosterlitz investigated. In systems close to absolute zero, some substances become what are known as "topological insulators". This means that they conduct electricity very well along their surfaces, but not at all through the middle. This means that the precise shape of the material can have dramatic effects on its electrical behaviour.
This strange effect is also seen in some very thin materials, ones that are so thin that they can essentially be considered two- or even one-dimensional. For example, a layer of tin one atom thick acts as one of these topological insulators.
These strange and exotic states of matter found in very cold or very thin systems are currently being investigated for potential applications in the development of advanced electronics and quantum computers which could revolutionise our lives, as well as having other far-reaching implications in the worlds of maths and physics.
13:00 - Myth: Why we get white spots on nails
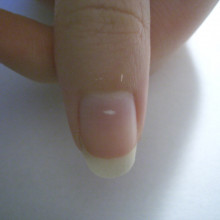
Myth: Why we get white spots on nails
with Kat Arney, Naked Scientist
This week Kat's got her finger on the pulse to get to the bottom of why we get white spots on our nails...
Kat - We're a glamorous bunch at the Naked Scientists, and while comparing manicures Graihagh noted that she's got quite a few white spots on her fingernails. All of us had a vague memory that they're something to do with calcium deficiency - after all, calcium is good for your teeth and bones, so surely it's good for nails, right? Actually, we were wrong.
There are plenty of folk-lore explanations for white spots - for example, that a white spot means you'll get a present when it gets to the end of your nail, or that the number of white spots on your left hand tots up the number of lies you've told. I've even seen the suggestion that white spots is the result of eating too much mayonnaise! None of these are true, and what's more - white spots have nothing at all to do with calcium. More formally known as leukonychia, white spots in the nails are incredibly common and are the result of damage to the base of the nail - that's an area known as the matrix - rather than any nutritional deficiency. Nails are made up of specialised cells containing large amounts of a sturdy protein called keratin, which grow outwards and form fingernails and toenails. Damage to the matrix prevents newly-formed keratin-packed cells from bonding together properly, leaving a tell-tale white blotch.
This damage could be the result of an injury like a knock or bang - it doesn't have to be slamming your finger in a door, even smacking it on a table could do it - or even an overly-vigorous manicure. But because nails grow so slowly, cranking out just a few millimetres in a month, it can take a good six weeks for a patch of damage in the matrix to grow up and manifest itself as a white spot in the nail. And by that time you've probably forgotten all about the original incident.
Simple white spots are harmless, and will eventually grow out, although this can take up to eight months. Sooooo slow! But your fingernails are actually a useful window on your internal health in many ways, and there are other conditions that can cause more dramatic changes to the shape and colour of fingernails, including arsenic poisoning, chemotherapy for cancer, heart disease, kidney failure, low protein levels in the diet, eczema and psoriasis, and general poor health. For example, if your fingernails turn completely white, you should be worried, because that's a sign of liver disease. And although calcium levels don't seem to have any impact on nails, other minerals do. For example, a lack of iron in the diet can lead to spoon-shaped dips in the nails, while a lack of zinc is also thought to lead to brittle nails and white patches.
Fungal infections can cause brown or pale patches under the nails, and allergic reactions to nail products such as polishes or varnish removers can cause changes and discolouring. And one colour change that you really don't want to ignore is a persistent black or dark brown patch under the nail - especially toenails, and particularly if you have dark skin. That could be a sign of acral melanoma - a rare type of skin cancer, so it's worth getting anything like that checked out by your doctor. And finally, one major cause of damaged patches on the nails is good old-fashioned fingernail-biting, so get those fingers out of your mouth!
16:47 - Medicine Nobel goes to how cells recycle
Medicine Nobel goes to how cells recycle
with Khalil Thirlaway, Naked Scientist
This year, the Nobel Prize for Medicine goes to research done on how cells  recycle, also known as autophagy. Khalil Thirlaway reports...
recycle, also known as autophagy. Khalil Thirlaway reports...
Khalil - This year's Nobel Prize in Physiology or Medicine has gone to Yoshinori Oshumi, who identified the mechanism behind one of the key processes going on inside all of our cells through a series of experiments in his lab at the University of Tokyo.
Living cells undergo a constant cycle of breaking down old or worn out parts and recycling the building blocks to make new components for the cell. This process is known as "autophagy", from the Greek meaning "self-eating".
This constant renewal protects the cell from damage as well as wear and tear. Problems with autophagy, which can occur because of aging, lead to damage not being repaired, and a build up of potentially dangerous debris inside the cell. This has been linked to a range of problems, including Parkinson's disease, diabetes and cancer.
Oshumi wanted to find out how this crucial process is controlled, and carried out a series of experiments to find out. He exposed yeast cells to a chemical which introduces random mutations, changes to the DNA instructions inside the cell, and identified those cells which could no longer carry out autophagy. By looking for the genes that had been mutated in these cells, he identified the genes responsible for controlling the process. In follow up experiments he went on to identify the proteins encoded by these genes, which actually carry out autophagy.
Oshumi showed us just how important this cellular recycling system is, and how it works on both a genetic and molecular level. Important medical research into new medicines for a raft of serious conditions is based on his work uncovering the hidden mechanisms behind one of life's most important housekeeping functions.

18:31 - Fat or sugar? Genes may decide for you
Fat or sugar? Genes may decide for you
with Professor Sadaf Farooqi, University of Cambridge
Given a choice, which would you prefer: a creamy korma, or a sugary eton  mess? Your genes may well be making your mind up for you: a new study out in Nature Communications this week has shown for the first time a direct link between our DNA makeup and our food preferences. Naked Scientist Graihagh Jackson went to chew the fat with the author of the study, from Cambridge University, Sadaf Farooqi...
mess? Your genes may well be making your mind up for you: a new study out in Nature Communications this week has shown for the first time a direct link between our DNA makeup and our food preferences. Naked Scientist Graihagh Jackson went to chew the fat with the author of the study, from Cambridge University, Sadaf Farooqi...
Sadaf - Well really what we're interested in doing is trying to work out why some people gain weight much more easily than others. And we know that whilst for all of us the amount of food we eat, and the amount of activity that we undertake are really important, some people gain weight much more easily than others and find it very hard to lose weight and, for those people, genes play a major role in their weight problem. And so what we been doing for many years really is trying to find some of those genes and work out what they're doing and here we were focused on one particular gene called MC4R.
Graihagh - And what does that gene do?
Sadaf - Well we know from quite a lot of work, including work that's been done in mice, that that gene is key to regulating weight and it does so by affecting appetite. And here what we were looking is whether the gene also might affect food preference: which foods you choose.
The challenge of course is humans are not mice and we needed to find a way to test food preference using regular meals. And, so what we did, we did lots of tests ourselves, and I personally volunteered to try all of the food, and what we did was we found that chicken korma and rice was a really useful food to use. And the reason it's useful is we could make a chicken korma and rice that was twenty per cent fat, forty percent fat, and sixty per cent fat. The key thing really we wanted to do here is you need to make sure they look exactly the same and they taste the same.
So the study involved normal weight people, people who are overweight but have a normal MC4 gene, and people who are overweight but have a faulty MC4 gene. And what we found is that when we asked everybody just to do a little taste test and try out the three types of chicken korma, they couldn't tell them apart. But then, when we left them in a room with a large tray, a buffet style approach, we found that the people with the MC4R gene that was defective ate ninety-five percent more of the high fat food than the normal weight controls, and they eat sixty-five percent more than the obese controls. So really a very marked food preference.
Now what was interesting was the total amount they ate at that meal was exactly the same in all three groups. So it's not that people necessarily ate more, but they switched their preference towards high fat.
So what we thought originally is that they may be both fat and sucrose preference in these folks because both things will give you plenty of calories. Interestingly, while we were doing the study on sucrose preference, mouse data came out suggesting that mice have less of a preference for sucrose, they don't like sugar.
So we set out to test that out in people as well. Originally we tried yogurt; that didn't work very well because nobody really like the sweetened fruit yoghurt, so we ended up with Eton Mess. And what we found is that the lean people; the obese people do what most people would do is that they like the sweeter things but, actually, the patients with the MC4R defect actually really didn't like the high sucrose Eton Mess. In fact, they hardly ate any of the Eton Messes that we gave.
So it suggests really that we have a pathway in the brain that can pick up the fat content in the food, even when we don't realise.
Graihagh - That's really intriguing because you would have thought, evolutionary speaking, you want to put on as much weight as you can for those feasts and famines, so why would you choose fat over sugar?
Sadaf - I think the possible explanation, but we would have to test it, is that this pathway is there to defend us against starvation. So, in people where the MC4R gene is defective, effectively that pathway's on the whole time; their brains and their behaviour is like as if they're starving; they need food. So I think it would make a lot of sense is that if you're starving you want to get more fat because fat has twice as many calories per gram as carbohydrate or protein. So that bit, I think, makes quite a lot of sense.
The bit that was confusing is the sucrose because, surely, that's got calories in it. Why wouldn't you eat sucrose? But then actually, what we thought about is that if you eat quite a lot of sucrose, you can only store a certain amount in the liver and actually, after that, it's waste. Whereas fat, of course, you can keep storing in your fat tissue so it would make a lot of sense that if you're starving, the thing you need to is fat and, actually, you need to make sure that you don't waste time eating sucrose because you can't store very much of it, whereas you can store the fat.
Graihagh - As many of us I'm sure know, myself included.
Sadaf - Exactly. And I think this is what's interesting is that whilst this finding came from studying a relatively rare group of people who have this gene problem, actually its relevance is much broader because we all have this pathway. And it's part of understanding really that you know what, our biology will influence our behaviour.
Graihagh - Does that mean, in some way, we're powerless, we're predetermined to always want to put on weight or does this mean we can perhaps harness this and work with it a bit?
Sadaf - So, of course, I often get asked that question. And I think the main thing is the assumption that something like eating and eating behaviour is purely down to free will is something that is challenged by this research. I think this research, and the work that's been done in animal models before this clearly shows that biology has an important part to play. But, of course, human beings are complex creatures and we work with our environment so there are potentially ways of modulating, or controlling, or influencing this behaviour, so I don't really think it's deterministic but I think it's important to recognise there's a biological component too.

24:16 - Smokefree this Stoptober?
Smokefree this Stoptober?
with Jamie Hartmann Boyce, Cochrane Tobacco Addiction group, Joe Allen, Harvard University and Amanda Sandford, ASH
For many smokers across England, this October is... Stoptober! That's the  campaign urging people to quit smoking this month, and hopefully even kick the habit for life. If you're one of those brave quitters, you might take inspiration from Public Health England's recent announcement that more people are quitting than ever before. Part of this success is thought to be down to the use of quitting aids, and among them, e-cigarettes. But, there have been some confusing reports about whether vaping really does help people kick the habit. To find out more, Laura Brooks sat down with Jamie Hartmann Boyce, researcher with the Cochrane Tobacco Addiction group and lead author of Cochrane's recent review on e-cigarettes....
campaign urging people to quit smoking this month, and hopefully even kick the habit for life. If you're one of those brave quitters, you might take inspiration from Public Health England's recent announcement that more people are quitting than ever before. Part of this success is thought to be down to the use of quitting aids, and among them, e-cigarettes. But, there have been some confusing reports about whether vaping really does help people kick the habit. To find out more, Laura Brooks sat down with Jamie Hartmann Boyce, researcher with the Cochrane Tobacco Addiction group and lead author of Cochrane's recent review on e-cigarettes....
Jamie - In Cochrane, what we do, where we can, is collect evidence from randomised control trials and, in the case of electronic cigarettes, we found two of these and results showed, when we combined them, that electronic cigarettes with nicotine did appear to help people quit.
Laura - There are growing concerns, aren't there, about the risks associated with vaping? Based on the evidence that you've seen, how safe are they?
Jamie - It's a really interesting question. It's hard to quantify safety for a number of reasons, partly because we don't have long term data. They haven't been around really for all that long and they certainly haven't been in common use for all that long. Another issue with assessing their safety is that the devices are changing all the time. Usually these changes are for the better but that also makes it difficult to assess.
Now, when we think about electronic cigarettes, what we really are comparing them to is regular cigarettes and everything we do know from the evidence suggests that electronic cigarettes are really considerably safer. We didn't find any evidence of any serious side effects that were associated with their use, but the studies we have in our review only went up to two years.
Laura - Right, and that's an important point, isn't it - does that mean we don't know what the long term effects could be?
Jamie - We haven't seen the data on the long term effects but we know from our studies of cigarettes a lot of the things that happen in your body that mean, in the long term, those cigarettes are likely to cause disease. And when we've measured those things in users of electronic cigarettes, the studies that we found in our review, found that they appeared much safer than regular cigarettes.
Laura - E-cigarettes might be safer than tobacco, but does that mean they are actually safe? Some scientists have expressed alarm about certain flavourings, because, while these chemicals might be harmless to eat, it doesn't necessarily mean they are also safe to inhale. Harvard Public Health scientist, Joe Allen...
Joe - For over a decade we've known about severe lung diseases associated with inhaling flavouring chemicals because of workers in the popcorn packaging industry, many of whom developed severe and irreversible lung disease after inhaling these flavouring chemicals. In particular, one of the chemicals that got the most attention, called diacetyl, and we detected diacetyl in over seventy-five percent of the flavoured e-cigarettes we tested. And this is the chemical that, in the United States, the investigating agency said that it's highly likely that diacetyl contributed to the occurrence of fixed obstructive lung disease, also known as bronchiolitis obliterans, also known as popcorn lung.
So we don't know much at all right now about the hazard associated with these flavoured e-cigarettes and that's one of the goals of our study is to be sure that when we start talking about e-cigarettes, and safety, and risk, is that flavouring chemicals are part of that conversation.
Laura - Joe Allen, who also believes that e-cigarettes should be regulated as carefully as tobacco cigarettes. But how are e-cigarettes currently regulated? Amanda Sandford works for the charity ASH (Action on Smoking and Health)...
Amanda - Really, virtually all the e-cigarettes that are on the market now in the UK are governed by the European Union Tobacco Products Directive. That means that there are restrictions on limits of the amount of nicotine per product, there's essentially a ban on the advertising and marketing that crosses borders, so sort of mass media type advertising, and there are other rules such as requiring a health warning on them. But, otherwise they are still classed essentially as consumer products so they are a separate category, they're treated differently, from tobacco products.
Laura - And we heard earlier from Jamie that e-cigarettes are thought to be a lot safer than smoking tobacco but, presumably, there is still some level of risk? No-one is recommending that we inhale chemicals into our lungs if we can avoid it.
Amanda - I mean, yes, that's a fair point. The Public Health England conducted a review of the evidence last year, which complements the Cochrane review, and they found that e-cigarettes were about ninety-five per cent safer than tobacco products. But you're right, there is going to be some small risk from continually inhaling a vapour and we certainly don't know what the long term risks are, particularly to the lungs. But we always come back to the comparative, which is tobacco smoking, because these products are not by and large used by non-smokers, and they are being used by smokers and recent ex-smokers and we know the harm from smoking is so great that, undoubtedly, e-cigarettes are a safer alternative.
Laura - Amanda Sandford. So, where does this leave us? We've heard evidence that vaping is much less harmful than tobacco smoke so, if you are a smoker looking to make the switch to e-cigs, the consensus is that it's probably a good move. But consumers should also be aware that there are still some safety concerns, and future trials will be needed so scientists and policy makers can better assess the risks.
But, if you're quitting this Stop-tober remember, there are many options out there to help you, but the place to start is to get advice from your Doctor or local Stop Smoking service who can help you find the best strategy to go smoke free for life!

30:31 - Alzheimer's: What we know
Alzheimer's: What we know
with Dr Louise Walker, Alzheimer's Society
Search for Alzheimer's Disease on the internet and you might be lead to believe  that we're on the cusp of conquering one of the most puzzling diseases of our time and indeed, there have been some 'big' breakthroughs out in recent months. So today on the Naked Scientists, we're going to be taking a closer look at these developments and ask when, and if, we'll be able to defeat the disease. First, what do we know about Alzheimer's? Louise Walker took Chris Smith through the pathology...
that we're on the cusp of conquering one of the most puzzling diseases of our time and indeed, there have been some 'big' breakthroughs out in recent months. So today on the Naked Scientists, we're going to be taking a closer look at these developments and ask when, and if, we'll be able to defeat the disease. First, what do we know about Alzheimer's? Louise Walker took Chris Smith through the pathology...
Louise - Alzheimer's was first described in 1906 by a German neuropathologist and psychiatrist called Alois Alzheimer. And what he did, he examined the brain of a lady called Auguste D., and she's been experiencing symptoms such as memory loss, aggression, and delusions, and when he examined her brain he found that she had two proteins in her brain that were not usual. So the first one were clumps of a protein called amyloid, which are now known as amyloid plaques, and another one were tangles of a different protein called tau.
Chris - And he could see all of that over a hundred years ago?
Louise - Yes, he stained them with a special dye and he was able to see these two abnormal proteins and realised they weren't normal parts of the brain, yes.
Chris - And today, what do we understand about the role of beta-amyloid and these tau tangles in causing Alzheimer's?
Louise - The role of these two proteins is actually not fully known. So we know that they exist in the brain of people who are affected by Alzheimer's disease and that amyloid seems to appear first and tau appears a little bit later, and they're thought to cause damage to the cells. So amyloid appears outside of the cell and tau appears inside of the cell and in some way they cause the brain cells, or the neurons, to stop working properly and that causes them to become stressed and die. But currently the exact link between the two proteins, the way that they affect the brain cells, is not fully known.
Chris - What sort of tempo does it follow then - once you start to see these symptoms how quickly can a person expect it to progress?
Louise - It varies a lot from person to person so people will experience these symptoms differently. Not everyone will experience the symptoms I've described and the prognosis and the progression of the condition varies a lot from person to person, so it depends on their age and the type of Alzheimer's that they have. If they've got early onset Alzheimer's they may progress faster than somebody who gets it in the later stages...
Chris - By early onset, you mean someone who's young when they start getting symptoms?
Louise - Yes. By early onset Alzheimer's, we mean somebody who is diagnosed before the age of sixty-five, which Auguste was actually, she was fifty-six when she passed away. So it can progress over five to ten years but I have heard of cases of people living with it for over twenty years.
Chris - At the moment, what can we do for someone who has this?
Louise - At the moment, if somebody is experiencing memory problems we will encourage them to go and see their GP and to get a diagnosis, because a lot of people feel that they don't want to, or they think there's nothing that can be done. But, if they go to their GP, you will have the comfort of having a diagnosis and there are some treatments that can be given to that person. They don't treat the underlying causes of the condition but they do help to manage the symptoms for a short period of time.
Chris - Now can you just define, because I think some people may be worried about what we call memory loss? Because I went out this morning and I forgot to pick up my keys but that doesn't mean I've got Alzheimer's disease so what do we define as memory loss in this context?
Louise - It's when memory loss begins to interfere with your day to day life. So said you've forgot your keys, that's obviously normal - everybody does that, but maybe if you start forgetting what your keys are, or what they're for, that would be a time to get concerned.
34:03 - Why Alzheimer's drugs keep failing
Why Alzheimer's drugs keep failing
with Professor Simon Lovestone and Jennifer Lawson, University of Oxford
If we know tau tangles and amyloid plaques are the cause of Alzheimer's, why  can't we just blitz them? Kat Arney put this to Simon Lovestone...
can't we just blitz them? Kat Arney put this to Simon Lovestone...
Simon - We now know how the amyloid that forms the plaque gets formed and there have been drugs designed to prevent that formation or, indeed, to clear that plaque once it's already formed. They've gone through clinical trials; so far none of those clinical trials have worked. I think there's a different reason why they haven't worked; I don't think it's just because the drugs are no good.
Kat - What is that reason? You can't give me that teaser and not tell me.
Simon - The trials are done too late. So one other thing, and this is surprising; we didn't know this until a few years ago but those plaques and tangles start to form ten, perhaps twenty years before there are any clinical symptoms. So this is not doctors not picking up dementia, that's another problem; this is there is no dementia, there are no clinical symptoms and that's probably because the brain is such an amazing organ. It's plastic, it's able to cope with a certain amount of damage without causing symptoms. So there's this long period, up to twenty years, where the disease is happening but there are not symptoms. Now the trials, they're done in people with dementia. I think, and I think the majority of the world thinks, those trials are done way too late. It's too much to ask these particular drugs to have a substantive effect after twenty years of disease.
Kat - What we need to do then, is spot the disease earlier. But that's not easy, especially since people don't have symptoms until very late on. However, Simon and his colleague Jennifer Lawson have won a huge Medical Research Council grant for a clinical trial that they hope will change that by finding biomarkers. Much like a blood test can reveal a high levels of antibodies, and therefore whether you have an infection, Simon and Jennifer hope to find some similar marker for Alzheimer's. Here's Jennifer...
Jennifer - We're going to take about two hundred and fifty volunteers and ask them to take part in the study. These are people who might have a range of health profiles; some people might appear be more at risk of getting Alzheimer's disease than others and what we want to do is track the really early changes that happen in the human body before we see memory changes.
Kat - So these are people who don't have Alzheimer's and also you don't know that they're going to get Alzheimer's?
Jennifer - That's right. We don't know if they're going to get Alzheimer's. At the moment, we know there are various genetic factors that make somebody more at risk of getting Alzheimer's. But we know that's not the whole picture and we urgently need to find other ways of tracking Alzheimer's well before people end up with memory problems so that we can target treatments at people, at that stage, and we can run clinical trials in that population as well. And that's the stage at which we think it's most likely to make a difference to people's lives.
Kat - So with this study you've got these two hundred and fifty people. What are you doing with them - how are you studying them to try and find these markers that may show that they are or aren't going to develop the disease?
Jennifer - We are going to use every test we can think of that might show us something valuable in this population. So we will do a whole host of tests; they'll be about fifty tests on people over a twelve month period, so it's quite intensive. We're going to do MRI scans, there'll be MEG scans, and PET scans, so three different types of brain imaging in the same population in the same volunteers.
Kat - That's a lot of brain scanning!
Jennifer - That's a lot of brain scanning - yes. And there'll be blood tests, there'll be cognitive tests alongside which tests people's memory, reasoning, and thinking skills. We'll also do eye tests looking at the retina at the back of the eye; we think we might be able to detect some changes in the morphology of the blood vessels at the back of the eye there and possibly pick up some early degeneration well before you see any other changes. We're also looking at wearable technologies, so there's lots of things to look at people's gait and movement. Really subtle things that you wouldn't pick up yourself with your fitbit; these are like more highly specialised pieces of equipment that are being used to detect really subtle changes, so that needs to be analysed by some proper science in a lab.
Kat - So say you come up with this profile; this sort of set of measurements that you can say okay, this person is getting worse or this person is getting better. What happens next?
Jennifer - Once we have a set of biomarkers that we're quite confident will show us how someone is progressing with Alzheimer's disease, we can then start to trial Alzheimer's drugs in a more effective way. In recent years, ninety-nine per cent of clinical trials in treatments of Alzheimer's disease have failed. It might be that many of those drugs actually would be effective if only we could target people at the right time. So we might be able to retest some of those compounds that previously haven't worked or we might be able to generate new compounds at the areas we have picked up from this trial.
Kat - If we can pick up the disease much earlier on, then, could we also screen for it? I put this to Simon Lovestone as my grandmother had Alzheimer's and I was keen to know if I, or my parents could be tested...
Simon - The short answer to that is no. And I'm not sure that we'd want something either. Right now we don't have any drugs for dementia and really you don't really want to screen until you've got something you can do if you find out you're screened positive. We are though trying to work on tests or biomarkers for dementia and the reason why we aren't though is not to screen populations but to help in the diagnostic process.
So when an older person comes to the GP and says they've got memory problems right now, it's almost impossible to tell whether that is just the memory problems that happens as people get to be elderly, or whether it's the start of the dementia process. So we really like tests to help that clinical practice but, even more than that, we need biomarkers or tests to help do clinical trials earlier in the disease process more effectively. That's what we really want to test for, not for screening.

40:25 - Aducanumab: A promising new treatment?
Aducanumab: A promising new treatment?
with Dr Laura Phipps, Alzheimer’s Research UK
Last month, a paper was published in Nature that demonstrated how a drug  called aducanumab appears to destroy amyloid plaques in people. Now, larger studies are underway. But, several other drugs have reached this stage and have failed, so why are scientists, like Laura Phipps from Alzheimer's Research UK, excited about aducanumab? She explained to Chris Smith...
called aducanumab appears to destroy amyloid plaques in people. Now, larger studies are underway. But, several other drugs have reached this stage and have failed, so why are scientists, like Laura Phipps from Alzheimer's Research UK, excited about aducanumab? She explained to Chris Smith...
Laura - Aducanumab is a drug; it harnesses the science of the immune system. So it's an antibody that tags the amyloid protein in the brain and really marks it for destruction. So the mechanism through which it really works, it isn't totally clear yet, but maybe through stimulating our body's own immune system to help clear away that protein.
Chris - How do the antibodies get made and how do they get into the patient?
Laura - They're given by a monthly infusion; this is what we call passive immunotherapy. So rather than giving somebody the amyloid protein themselves then letting their immune system do all the work...
Chris - Like a vaccine?
Laura - Yes. The antibody itself is made externally; it's pre-made and it's given by a monthly infusion, so the effects are shorter term. They're not a one off injection so it would involve somebody going for monthly injections of that antibody treatment.
Chris - Now, the blood is kept separate from the brain, so have we any idea how this antibody given into the bloodstream can affect what goes on in the brain and get rid of this protein we don't want?
Laura - So you're right. The brain is a really protected area and it has what we call the blood-brain barrier that's really selective about what goes in and what goes out. And that's why drug development in Alzheimer's has been such a challenge because not only have you got to find a drug that hits your target, but you've got to find one that goes into the brain as well. But the research suggests that this drug, and others in development, are able to do that; they are able to clear this protein out of the brain and we need to then see see whether or not that's effective and whether that has a benefit for patients.
Chris - Now when you say "whether it's effective," you mean as in we know it gets the stuff out of the brain but whether that makes a difference for the outcome in the patient?
Laura - Yeah, exactly. Amyloid has been in researchers sights for many years as potentially the idea that if you could stop the buildup of amyloid, you could slow or halt the progression of Alzheimer's disease. And we've heard in previous interviews on the show tonight that, actually, there have been some quite high profile failures in this area where, perhaps, the drugs have been unable to look like they're clearing the protein but hasn't benefited patients. And so, we really need to try to understand whether or not we're hitting the right target, whether just the timing is wrong.
Chris - What's the evidence that it will work?
Laura - So, the study was promising, even though it was a relatively early clinical trial. It showed evidence from brain scans that the amyloid protein was being cleared out of the brain. But, obviously, they need to be taken forward into big phase three clinical trials before we can see robust statistical evidence that this makes a benefit for people.
Chris - How did the patients get on because in a previous trial, I think it was Wyeth the drug company, made a vaccine which was designed to stimulate the person's own immune system to do something similar. A number of patients had inflammation in the nervous system; we had to stop doing that. How has this been tolerated and is the outcome better?
Laura - So, with these anti-amyloid treatments, there is this side-effect called ARIA, which stands for amyloid related imaging abnormality, and some people have this and they don't have any symptoms at all; other people will experience confusion, or dizziness or headaches and it can bee seen on MRI scans. So it's basically a leakage of fluid out of the blood vessels into the brain, so an oedema in the brain. Obviously, that's not an ideal side-effect and what the researchers found is people who were on the higher dose were more likely to experience this. And this is something researchers are facing all across the anti-amyloid field.
Chris - There are two things that Louise Walker mentioned: one is that people begin to accumulate this stuff long before they actually have any symptoms, and the other is this protein tau, which Alois Alzheimer also spotted in the brains of people who have the disease. Now a) do we need to start the treatment very early in order to defer the buildup in the first place before it does damage, and two, what about the tau?
Laura - Yes, that's a really good question. Amyloid has been the major player in drug discovery because of some of those very early discoveries, and genetic discoveries that have really implicated amyloid as driving Alzheimer's disease. But then, in recent years, scientists have understood that, actually, amyloid may just be a trigger; it may be a judge and not an executioner and perhaps tau plays that ultimate role. But that means because the focus for a long time has been on amyloid, those anti-amyloid treatments are much further through development and so we are seeing tau treatments come through the pipeline of drug discovery, but they're not as advanced as amyloid.
But the advantage of tau against amyloid is that we know that amyloid is one of the first changes in the brain; it's one of the earliest changes in the brain. And so some of the clinical trials with anti-amyloids potentially have failed because they haven't been given early enough. So, in order for them to really work, you'd have to find people in the very earliest stages of Alzheimer's disease, which then gives it a diagnostic challenge; how do we find these people?
45:55 - A 'silver bullet' for Alzheimer's?
A 'silver bullet' for Alzheimer's?
with Rosie Freer, University of Cambridge
A lot of focus has been on blitzing these amyloid plaques and there is now a push to target tau tangles but what if we could find a 'silver bullet' which could stop these proteins forming a sticky mess in the first place? Rosie Freer published a paper in Science Advances this summer that was looking at why some areas of the brain are resistant to build ups, whilst others aren't. And in this, holds a clue into this 'silver bullet', as she explained to Kat Arney...
to target tau tangles but what if we could find a 'silver bullet' which could stop these proteins forming a sticky mess in the first place? Rosie Freer published a paper in Science Advances this summer that was looking at why some areas of the brain are resistant to build ups, whilst others aren't. And in this, holds a clue into this 'silver bullet', as she explained to Kat Arney...
Rosie - We know that the hippocampus is one of the most vulnerable tissues to Alzheimer's disease. And what we also know is Alzheimer's spreads in a very specific spatial temporal pattern through the brain and there are some tissues in our brain that will always be very resistant to the diseases. And, as you mentioned, what I wanted to understand was why some tissues were vulnerable and why others were resistant.
Kat - So it seems to have this route that it likes to take from the hippocampus around different bits of the brain?
Rosie - Exactly. And what I did, I looked at the protein composition of tissues that were vulnerable and those that were resistant, and I identified a set of proteins that characterised vulnerable tissues and were able to predict the progression of Alzheimer's disease through the brain.
Kat - So there's certain characteristics then that make it more easy for these tangles, these plaques to form?
Rosie - Exactly. So if you look at a vulnerable tissue you'll see very high levels of the proteins which promote the aggregation of these plaques and tangles, and you'll see very low levels of the proteins that protect against this clumping process.
Kat - This isn't completely surprising to me because, obviously, different bits of the brain do different things but, was it a surprise to find these particular proteins seem to be in different levels in different parts of the brain, and does that seem to then tip when Alzheimer's kicks off?
Rosie - I think the interesting thing about these results - you're right. I think we would expect to see different levels of proteins in different regions of the brain because different regions of the brain have different functions. But the interesting thing about the results is they suggest there's an underlying biophysical basis to the disease. And they also suggest that there's a wider network of proteins which are responsible for vulnerability to disease beyond amyloid-beta and tau.
Kat - And is this just Alzheimer's where this is important? I mean there's lots of different types of dementia; there's lots of diseases that affect nerve cells; I'm thinking of things like Parkinson's or Motor Neuron disease.
Rosie - This is the really interesting thing about our results is if our hypothesis is correct, then we should be able to apply our results to other neurodegenerative diseases associated with aggregations such as: ALS, frontotemporal dementia, and be able to detect similar signals which define vulnerability to those diseases.
Kat - Okay. Put it all together: we've found that tipping the scales, tipping the balance of proteins in the brain is the problem; if we can find a way to tip it back then that could lead to a new treatment. How do we go forward from here?
Rosie - I think one promising approach that's been suggested by our results as well as may other studies would be to enhance the natural capabilities of our cells - it's called the protein homeostasis system - and create an environment which is really resistant to the type of clumping process that results in plaques and tangles.
Kat - It feels like it's just coming at it from a different angle, instead of focusing on the molecules, you're focusing on the process?
Rosie - Exactly, yeah.
Kat - And in terms of the treatments, are we still talking about something that's five, ten years away or is it even to early to talk about that?
Rosie - That's the golden question, isn't it?
Kat - It's almost like how long is a piece of string?
Rosie - Exactly, exactly. I think we're making great steps at the moment towards understanding the disease, and I think that will be the key to finding an effective treatment, and so I think it is on the horizon.

50:04 - 5 ways to reduce your Alzheimer's risk
5 ways to reduce your Alzheimer's risk
with Dr Louise Walker, Alzheimer's Soceity
Although all this research sounds promising, drug development takes time. From the discovery of a potential compound through to drugs hitting the market, it can take decades. In the meantime then, we need to be thinking about what you and I can do to reduce our risk. Louise Walker talked Chris Smith through her top 5 tips...
the discovery of a potential compound through to drugs hitting the market, it can take decades. In the meantime then, we need to be thinking about what you and I can do to reduce our risk. Louise Walker talked Chris Smith through her top 5 tips...
Louise - Yes. To start off with I want to make clear that the biggest risk factor for Alzheimer's disease is age, and that Alzheimer's disease is thought to be due to a complex mixture of age, genetics, lifestyle and environment. However, there are things that people can do to reduce their risk of the condition. My number one tip is physical activity. So do exercise as much as you can, particularly if you're in mid-life.
Chris - But why does that help a brain problem?
Louise - It's thought to help things like induce blood flow to the brain, maybe to help boost the immune system. And there is some quite exciting research that indicates if you exercise it might help to clear them out of the brain although, obviously, the research is still ongoing there.
Chris - That's your number one tip - take up exercise, which is good for a range of different health disorders and potential health risks. What's number two?
Louise - Number two is eat a healthy, balanced diet. The one that we think there's most evidence for is the mediterranean diet. So, this is one that's high in vegetables, high in fruit, cereals, legumes, quite a lot of oily fish, and low in red meat, dairy and sugar. And, again, that's generally thought to be because it might help to boost brain activity through boosting the immune system - just improving blood flow, things like that.
Chris - And those things are more likely to fur up blood vessels aren't they? So if you reduce them.
Louise - Yes. High sugar....
Chris - What about this claim that people in India who eat a lot of curry and, therefore, have a lot of turmeric, which has got the anti-oxidant curcumin in it - what about the claim that that's protective against Alzheimer's? Is that a myth or is that true?
Louise - At the moment there's not a lot of evidence for turmeric as a way to prevent Alzheimer's disease. People have made that observation but...
Chris - I was just hoping you see because I'm quite partial to a curry.
Louise - People have made that observation but it hasn't shown any benefit. But there are things that curcumin has quite low bioavailabilities so, if you eat it, it doesn't really get into your brain very much. So there's currently not much evidence for that. And there's things about cultural aspects of living in India which might be why Alzheimer's appears to be lower in that population.
Chris - And the next thing on your list?
Louise - The next thing on my list is to stop smoking. This is mostly because smoking is very damaging to blood vessels and there's a lot of evidence showing that blood vessels raises your risk, particularly of vascular dementia, but maybe of Alzheimer's disease as well. So, if you are a smoker, there's evidence actually that if you stop at any age, it will help to reduce your risk.
Chris - And the next one?
Louise - The next one is to manage certain conditions. These include diabetes; if you do have diabetes make sure that you manage your condition well. And another condition you should keep in check is high blood pressure, because high blood pressure, again, it increases your risk of dementia, particularly vascular dementia, possibly Alzheimer's disease as well. So, if you know you have one of these conditions, make sure you manage them, make sure you get your blood pressure checked regularly, particularly again, if you're in middle age when you're most vulnerable to these processes that cause Alzheimer's disease.
Chris - And number five?
Louise - Number five is one that's a little bit less evidence-based but it's quite a nice one. So, if you try and keep as mentally and socially active as you can: doing maybe crossword puzzles, jigsaws, make sure your go out with your friends a lot. There's a few specially tailored brain training games that - lots of trials have been happening now - and they're starting to show that maybe there's some evidence that if you do these on a regular basis that you might be able to reduce your risk of dementia. I should just point out that these are very particular games made by scientists, not your average brain training computer games.
Chris - It works in mice though, and rats, doesn't it? If you give them a rich environment in which to grow, and you give them toys to play with, they succumb to these sorts of brain-eroding illnesses at a later date than if they have a boring existence with less mental stimulation.
Louise - Yes, but we always have to remember, as always, in these kinds of things, how things work in mice doesn't necessarily work that way in people. So there's quite a lot of work going on now to try and found out if people keep mentally and socially active, whether they reduce the risk or delay the onset of Alzheimer's disease. So it's quite exciting research and we are hoping to see some results coming out on some of those trials soon.

54:28 - Does handwashing really work?
Does handwashing really work?
Connie Orbach put this to Cheryl Trundle from Addenbrooke's hospital...
Cheryl - When you're talking about hand washing, the important things to know are when to do it, what sort of soap or what agent to use to wash your hands, and how you do it. And really, of those three, the most important is the good technique so it's how you do it. Any soap will be sufficient, any soap will work, but it's important you cover all the surface of your hands and you do it for the required length of time, and you need to do it before you touch a patient and after you've touched a patient. Connie - The required length of time? I always thought depended on how much of a rush I was in. Cheryl:: Generally we say between ten and thirty seconds. About the time it takes you to sing Happy Birthday fairly slowly. Connie:: So far Dale, it seems your cleaning lady may have been telling porkies. What about that gesture though? Cheryl - It's just so they're not tempted to touch anything. So they just hold them where they can see them so they're not touching anything dirty to contaminate them again. Then the water can wash down to the elbow so that the fingertips, which are the important bits, remain clean. It also lets the hands drain a bit so it doesn't take quite so long to dry them. Connie - Well, there you go Dale. There's some method to the madness but don't ditch the soap just yet.Next week we'll be defying time with Troy's question... Troy - If you were to live on Jupiter for fifty years and then return to Earth, what would the time difference be back on Earth due to Jupiter's increased gravity? Thank you.
- Previous Hospital Histories
- Next Roving Over Mars










Comments
Add a comment