Leprosy goes under the microscope this week as we uncover the origins of one of the oldest known human diseases, recognised this week on World Leprosy Day. A quarter of a million new cases are diagnosed every year, but how is the illness spreading, what damage does it do to the body and can it be stopped? We also hear what archaeologists are unearthing about the history of leprosy and where it came from in the first place. Plus, why it's time to rethink the workings of the circadian clock, brain scans for bilingualism, cow-stomach bacterial genes for biofuels, and the engineering that lies behind the cat's eye...
In this episode
01:53 - Resetting the Circadian Clock
Resetting the Circadian Clock
Biological clocks play an essential role in physiology and in controlling behaviour - from regulating sleep cycles in animals to balancing photosynthesis in plants. Now, research published in Nature suggests that our model of how the clock works might be wrong.
There are two key features that define a biological clock mechanism: It must compensate for temperature, as chemical reactions will generally run faster at higher temperatures; and it must be able to synchronise to external stimuli such as light and dark.
 Current models of circadian clocks rely heavily on feedback loops based around transcription and translation - the "reading" of DNA and subsequent protein production. Essentially, the products of transcribing "clock" genes regulate how associated genes are expressed, and this leads to a roughly 24 hour feedback loop. Post-transcription contributions to the circadian clock have been observed, but the basic DNA-led feedback mechanism is still assumed to be the major driving force in biological clocks.
Current models of circadian clocks rely heavily on feedback loops based around transcription and translation - the "reading" of DNA and subsequent protein production. Essentially, the products of transcribing "clock" genes regulate how associated genes are expressed, and this leads to a roughly 24 hour feedback loop. Post-transcription contributions to the circadian clock have been observed, but the basic DNA-led feedback mechanism is still assumed to be the major driving force in biological clocks.
Now, John O'Neill & Akhilesh Reddy at Addenbrookes Hospital in Cambridge have shown that non-transcriptional mechanisms are capable of maintaining a clock in human red blood cells, which have no nucleus and are therefore incapable of transcription.
To study clocks in red blood cells, they looked to a family of antioxidant proteins called Peroxiredoxins or PRX. These are responsible for clearing reactive oxygen species like peroxide from the cell. A subclass of PRX molecules undergo an oxidation/reduction, also known as a "redox" reaction, with a regular cycle.
To assess PRX's suitability as a clock molecule, O'Neill and Reddy took red blood cell samples from healthy volunteers, and stored them in darkness and at a constant temperature. This enabled them to sample the cells every 4 hours, and confirm that the redox cycle did indeed take around 24 hours.
To see if this system fulfilled the other conditions of being a clock molecule, they attempted to entrain the cells to a cycle of high and low temperature - mirroring the temperature variations you or I might experience on a daily basis. After just 48 hours, the PRX redox cycle was seen to sync with the new temperature regime, making it an excellent candidate for non-transcription based circadian rhythm control.
PRX proteins are very highly conserved, and found in a huge range of species, including mammals, plants and algae. In a related paper, Andrew Millar from the University of Edinburgh, along with colleagues in Cambridge and France, show the same mechanism in action in Ostreococcus tauri, a single celled, eukaryotic alga. This raises some very interesting questions about our current understanding of circadian clocks, and raises some exciting prospects for our understanding of clock evolution.

04:46 - Chewing the cud (and how it got there)
Chewing the cud (and how it got there)
Researchers in America this week have dramatically enlarged the catalogue of known genes which allow an organism to break down plants. This new information could be very useful in producing biofuel from plant matter.
 Matthias Hess and colleagues found their new biomass-breaking genes and genomes swimming around in the rumen of a cow. The rumen is a fascinating part of the cow's digestive system in which lots of bacteria, yeasts and fungi live. These microbes break down all the grass and leaves that the cow munches through - so as you can imagine, a probiotic yoghurt means nothing to the host animals.
Matthias Hess and colleagues found their new biomass-breaking genes and genomes swimming around in the rumen of a cow. The rumen is a fascinating part of the cow's digestive system in which lots of bacteria, yeasts and fungi live. These microbes break down all the grass and leaves that the cow munches through - so as you can imagine, a probiotic yoghurt means nothing to the host animals.
Publishing in Science, Hess and his team were able to sequence a quarter of a terabase (which is an enormous amount - a trillion bases) of genomic information from many different microbes involved in digestion. They were also able to identify the very genes which were involved in plant degradation and the proteins which are thought to do the work.
Just in terms of the data generated, it's quite a step forward in sequencing large communities of different microbes. And the team have managed to demonstrate that it's possible to construct genomes of new, previously unknown organisms from the same mass of data. But the authors hope that this work will ultimately help other researchers in developing more efficient ways of producing biofuels.
06:08 - Rapid Change in Bacterial Genome
Rapid Change in Bacterial Genome
with Dr Stephen Bentley, Wellcome Trust Sanger Institute
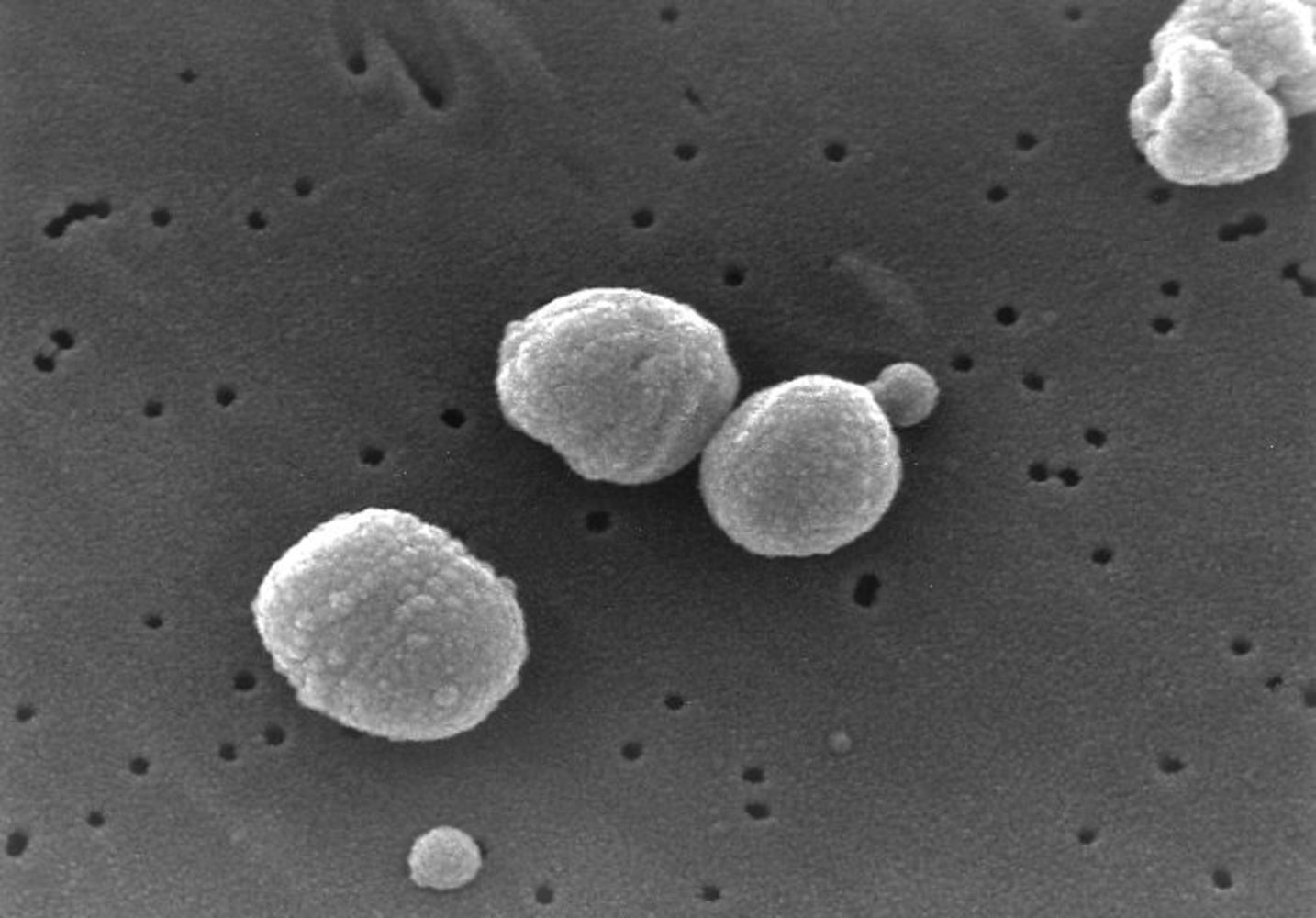
Ben - Also this week, researchers at the Wellcome Trust Sanger Institute who have been looking at changes in the genome of a troublesome pathogen, Streptococcus pneumoniae. This bacteria is responsible for a broad range of human diseases including pneumonia, ear infections, and bacterial meningitis. Fortunately, because this bacteria has been infecting humans for so long, we have samples from all over the world, going back many, many years, and this means, we can compare them genetically to see what has changed in response to modern antibiotic's and to vaccines. We're joined now by Dr. Stephen Bentley from the Wellcome Trust Sanger Institute. Thank you very much for joining us, Stephen.
Stephen - My pleasure.
 Ben - Now the idea that bacteria change genetically in response to drugs or vaccines isn't new, we've known about this for a while. What's novel about your work?
Ben - Now the idea that bacteria change genetically in response to drugs or vaccines isn't new, we've known about this for a while. What's novel about your work?
Stephen - As you say, we've known about these phenomena occurring over time since antibiotics have been in use, but the kind of breakthrough that we have in the projects that we're now able to do has been driven by our ability to sequence large number of genomes. Ten years ago, when we tried, when we sequenced the genomes of things like TB, Mycobacterium tuberculosis, one project to sequence the genome of one isolate, which was chosen to represent species, would have taken a couple of years and cost 1 or 2 million Pounds. The new sequencing technologies allow us to sequence hundreds or thousands of isolates at a cost of around 100 Pounds per isolate, and the turnaround of generating sequence data is down to a matter of weeks. That allows us now to exploit the collections of isolates that you mentioned earlier to really drill down onto the evolution of a population.
Ben - So, what samples have you actually been looking at? I understand they are from all over the world and actually going back quite a long time.
Stephen - The idea of project was to really use the whole genomes to analyse the evolution over the period since the introduction of antibiotics. So, when we tried to collect the samples we were looking for as much geographic and temporal coverage as possible. So, the collection we ended up with was 240 isolates, spanning the period of 1984 to 2007, and covering 22 different countries around the globe.
Ben - What sort of scale of changes are you actually seeing in the genome here?
Stephen - Substitution mutations which basically occur at random. One of those will occur approximately every 15 weeks. But there's another mechanism for variation which we call recombination, and that's basically where the bacteria are able to swap DNA with their neighbours. On the BBC website, there's a guy, James Gallagher, who's come up with a really nice analogy that's like doing down to the shops and swapping eye colour with someone in the queue at the checkout. But for the bacteria, that means they can generate enormous amounts of variation in their genomes and each variation that's generated then can be selected for possible advantage. So in a situation where the organisms are being exposed to antibiotics on a regular basis, which is what's happened in all bacteria since the introduction of antibiotics in the '60s and '70s, if they acquire a variation in their sequence which gives them advantage over the rest, then that's going to give them a good chance of proliferating.
Ben - Now obviously, the bacteria can't, as you say, meet down the shops and have a chat and say, "I've got these bright blue eyes. They've been really useful for me for survival. Why don't you have a copy?" There can't be a process by which they know that if they translate these genes from another cell that'll be useful. How does that process actually work? Is it quite random?
Stephen - It is entirely random. So, what happens with Streptococcus pneumoniae, they live in the human nasopharynx and, as far as we know, that's their only natural niche, but there are other bacteria that live there, some of which will be members of the same species but maybe only slightly-related, and then there are other species as well. As cells grow and divide and go through a cycle where there's actually death, some cells will lyse. Lysing the cells releases the [DNA] bacteria into the environment and that allows bacteria like Strep pneumo to potentially take-up that DNA. So this ability to take-up DNA from the environment is not ubiquitous in bacteria, it only happens in certain species. But Strep pneumo does that and is entirely random and some people have thought about whether it might actually be for nutritional needs and much as anything that they take up the DNA. So, the randomness is there but then selection kicks in, so it's really - if the variation you introduce is disadvantageous, then that will very quickly die out. If it happens to give you an advantage, then it will proliferate.
Ben - With all these random changes, do you see changes evenly across the genome or are there regions that are very heavily conserved and regions that are very highly variable?
Stephen - Yes. So we see these variation hotspots in the genome and it's interesting that those variation hotspots tend to be associated with surface antigens. So the major surface antigen in Strep pneumo is the surface polysaccharide and that's one region where we've seen frequent recombinations.
Ben - Now these are the sugars or the proteins that are on the surface of the cell that it actually presents to, say, our immune system.
Stephen - Exactly, yes. And what's interesting from the data that we've seen is that that region is a hotspot, so it's swapping in and out with its neighbours and changing its surface polysaccharide. But these changes were already in the population at fairly high levels, so that in around 2000, when we started to introduce a vaccine which targeted those surface polysaccharides, we could see that, in the population, there were already variants generated which we're going to be able to evade that vaccine because they didn't have the vaccine target.
Ben - So they essentially come preloaded to avoid our vaccine attempts.
Stephen - The population does, yes.
Ben - How can this help us to develop better vaccines or better antibiotics?
Stephen - Already, since the seven-valent vaccine was introduced, because these capsules have been spotted, new generations of vaccine have been generated where they now target 10 or 13 of those types. So, going forward, we would hope to be able to continue to monitor the population in very, very high resolution, using whole genome sequencing, so that we'll be able to understand better how the pathogens are responding to the clinical practices; and then maybe we can adjust those clinical practices to make them more efficient.

13:09 - Many heads are better than one
Many heads are better than one
Animals come to better decisions more quickly in larger groups, according to research published in the journal PNAS this week.
Group decision making is seen in many social communities - from ants to humans. It forms the basis of financial markets and the behaviour of the internet. It's clearly evolved many times over, but exactly how the decision making process in a group differs from that an individual is hard to determine.
 An international team of researchers, including Ashley Ward at the University of Sydney and Jens Krause at Humboldt University in Berlin, created a simple decision making task - a Y shaped chamber where one path contains a replica predator, and the other was safe. They then introduced mosquitofish, Gambusia holbrooki, to the task either alone, in pairs or groups of 4, 8 or 16.
An international team of researchers, including Ashley Ward at the University of Sydney and Jens Krause at Humboldt University in Berlin, created a simple decision making task - a Y shaped chamber where one path contains a replica predator, and the other was safe. They then introduced mosquitofish, Gambusia holbrooki, to the task either alone, in pairs or groups of 4, 8 or 16.
They then monitored how the fish moved, and which direction they chose to take, to see if group size would alter the speed and accuracy of the decision making process.
They found that lone fish took longer to reach a decision, swimming more slowly and changing direction often, but even then only chose the "safe" route little over half the time. As the group size increased, the decisions became more accurate and much faster - the larger group choosing the safe route up to 90% of the time, despite swimming faster and taking a more direct route.
The next step was to try to work out why groups are so much better at these decisions. As the variation between different lone fish was insignificant, this rules out the idea that particular fish are simply "experts" at spotting predators, benefiting the rest of the group. There is some evidence that the group does divides the responsibility of being vigilant - each fish needs to scan a smaller area, so the amount of direction changes made reduces in larger groups. Task sharing like this also means the fish must rely on social cues to make these decisions, as was seen when observing the fish closest to the leading fish.
This research suggests a high degree of cooperation, division of labour and rapid communication between members of a group, all factors that would promote the evolution of group decision making.
16:02 - Brain activity can demonstrate how fast a second language is learned
Brain activity can demonstrate how fast a second language is learned
This week teams in both Hong Kong and Chicago have found that the levels of activity in two specific areas of the brain can be used to predict how well someone is learning a second language.
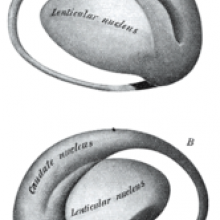
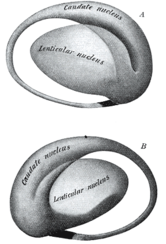 Li Hai Tan and colleagues found that the left caudate and fusiform gyrus areas of the brain displayed more activity the better the language student performed in their tests. The fusiform part of the brain is located at the back and base of the brain while the caudate is found closer to the centre and is shaped a bit like hooked headphones.
Li Hai Tan and colleagues found that the left caudate and fusiform gyrus areas of the brain displayed more activity the better the language student performed in their tests. The fusiform part of the brain is located at the back and base of the brain while the caudate is found closer to the centre and is shaped a bit like hooked headphones.
They used fMRI (functional magnetic resonance imaging) in between tests taken by 26 10 year old Chinese students who were learning English. They were given the first written test just before the fMRI scan and the second one year later. During the fMRI scan the children were asked to identify written English words. They found that those who'd demonstrated the greatest amount of activity in the caudate and fusiform regions during the scan performed better in the first and second tests.
Publishing in the journal PNAS, Tan and his team believe that the amount of activity in these two brain areas can therefore be used to predict how well a student will do when they learn a second language.

18:05 - Planet Earth Online - The Music Of Earthquakes
Planet Earth Online - The Music Of Earthquakes
with Brian Baptie, British Geological Survey, Edinburgh
Diana - A few days ago, a 7.2 magnitude earthquake hit Southern Pakistan. Fortunately, it caused limited damage, but in today's world, it can seem as if there were more earthquakes than ever before.
I say seem because scientists at the British Geological Survey in Edinburgh are often being asked whether earthquakes are becoming more frequent. Planet Earth Podcast presenter Richard Hollingham went to talk to seismologist Brian Baptie to find out if this was actually the case. The answer involves music and begins by comparing the number of earthquakes on Earth to throwing dice...
 Brian - Occasionally, you'll roll three sixes together. Earthquakes are a bit like that as well. You'll get times when there are a few earthquakes that happen together and then also you'll get pauses when there aren't so many earthquakes. If you look over the year as a whole, or a number of years as a whole, the numbers are all roughly the same.
Brian - Occasionally, you'll roll three sixes together. Earthquakes are a bit like that as well. You'll get times when there are a few earthquakes that happen together and then also you'll get pauses when there aren't so many earthquakes. If you look over the year as a whole, or a number of years as a whole, the numbers are all roughly the same.
Richard - Now you can prove this, can't you - with this computer program you've got up and the power of music?
Brian - We'll run through our sequence of earthquakes for the last decade and every time there's an earthquake, there'll be a noise, a little musical note, and what you'll be able to hear hopefully is that there'll be pauses, and then there'll be times when there are lots of notes all happening roughly at the same time.
Richard - Okay, so let's play this.
Brian - So each note is an earthquake.
Brian - And there are some pauses...
Brian - There's a longer pause now....
Brian - And you can hear how occasionally you get clusters or little groups of earthquakes happening at the same time and then we're in a longer pause...
Brian - And a few more...
Richard - So we had there South America, Indonesia...
Brian - These events are all happening in main global earthquake hotspots, if you like. They're big ones that are happening at plate boundaries and you can see on the map that they're clustering around in the Pacific.
Richard - Also several are there together.
Brian - So, this idea that you've got the clusters and gaps, earthquakes are not happening regularly. They're not like a person's heartbeat. They're not going to boom, boom, boom. They're going, babababum...boom, boom in that way.
Richard - Can we turn it off now?
Brian - Of course.
Richard - So we've switched that off. That could be one reason that you've got these clusters of earthquakes, even though the average is unchanged. What about the fact that there are more people living in the world now? Is that another reason that more people can be affected by an earthquake now?
 Brian - It's certainly true to say that there are far more people living in earthquake prone regions mainly because of increases in global population. So there's a huge swathe of Asia that can struck by big earthquakes starting from Turkey, Iran, through India, and into China where global populations are really increased in a big way. In those regions, earthquakes are capable of having far larger impacts than they have in the past. Also, there's a human perception thing going on here as well, because when earthquakes hit populated places, people look some more. Obviously, we're far more aware of the earthquakes that cause tragedies than the big earthquakes that happen in the middle of the pacific.
Brian - It's certainly true to say that there are far more people living in earthquake prone regions mainly because of increases in global population. So there's a huge swathe of Asia that can struck by big earthquakes starting from Turkey, Iran, through India, and into China where global populations are really increased in a big way. In those regions, earthquakes are capable of having far larger impacts than they have in the past. Also, there's a human perception thing going on here as well, because when earthquakes hit populated places, people look some more. Obviously, we're far more aware of the earthquakes that cause tragedies than the big earthquakes that happen in the middle of the pacific.
Richard - Could there be any reason though that earthquakes might increase? Is there any link between climate change and earthquakes, for example?
Brian - There isn't really a very strong relationship between earthquakes and climate change. There are some second order effects, if you like that might lead to increases in earthquake activity, but only in a really small way. One example of that is, as glaciers melt, as icecaps met, we get these phenomena called glacial rebound. It's basically when the ice goes, the lithosphere tends to rebound, it tends to push back up again, and that can result in earthquake activity, But generally, that won't be a big factor. And the reason for that is, that earthquakes are controlled by the motion of tectonic plates. You've got these plates that are moving around and that motion of the plates in turn is controlled by heat release deep inside the planet, and there's only a finite budget for this heat release which means the plates move at roughly the same speed. They're not speeding up or slowing down. So, the overall energy budget for earthquakes is roughly the same. So we wouldn't really expect earthquake activity to increase, unless the energy budget increased.
Richard - So really, there's no reason as far as you know, as far as you understand, how earthquakes happen, there's no reason for the number of them to increase.
Brian - That's right. As far as we understand at the moment, perhaps over much longer time scales once we have longer windows of observation if you like, it might become clear that there are these clustering phenomena happening for a reason, but at the moment, it's not clear to us.
Richard - It's like a radical jazz experiment gone wrong, isn't it?
Diana - That was Brian Baptie from the British Geological Survey talking to Richard Hollingham. You can download the latest Planet Earth podcast and find links to its host website Planet Earth Online at thenakedscientists.com/planetearth.
31:15 - Leprosy in the World Today
Leprosy in the World Today
with Professor Diana Lockwood from the London School of Hygiene and Tropical Medicine
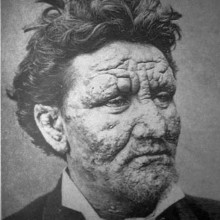
Ben - Leprosy is caused by an infection of Mycobacterium bacteria, the same family as the pathogens that cause TB. Most people here in the UK think of leprosy as a medieval disease, one long-since wiped out, but sadly, that's not the case. Leprosy still affects people worldwide and Professor Diana Lockwood from the London School of Hygiene and Tropical Medicine joins us now to tell us more.
Thank you very much for joining us, Diana. I wonder if you could start by telling us, how big a problem is leprosy today?
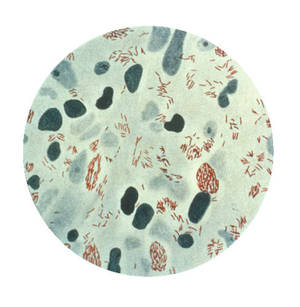 Diana L. - Leprosy is a very big and important problem. About 250,000 new cases are detected worldwide each year and that number is pretty stable at the moment. So that means that we've got a lot of new people coming in and the risk is that they will also develop disabilities that we associate with leprosy, and that will add to the number of leprosy cases that are around.
Diana L. - Leprosy is a very big and important problem. About 250,000 new cases are detected worldwide each year and that number is pretty stable at the moment. So that means that we've got a lot of new people coming in and the risk is that they will also develop disabilities that we associate with leprosy, and that will add to the number of leprosy cases that are around.
Ben - Where in the world do we actually find it? Is it like other diseases that we think are medieval and wiped out? I know that things like the plague are actually still around in certain parts of the world. Is it just hanging on in certain pockets or is it spreading around the world still?
Diana L. - 60% of the world's cases are in India and India is certainly the hotspot, and Northern India has more cases than anywhere else. Rather surprisingly, Brazil is the next most endemic country and particularly in Northern Brazil, again, associated with poverty. So Brazil has about 11% of the world's cases, but all through Africa, places like Ethiopia, Nigeria, Mozambique, Madagascar, these all have large numbers of new leprosy cases each year.
Ben - How is it actually transmitted from one person to the next?
Diana L. - What happens is that a very small proportion of people with leprosy are infectious. I want to emphasise that because you don't get leprosy from touching somebody and what happens is that the small number of people who are infectious cough and sneeze the leprosy germ out into the environment. It's a very hardy germ and it can survive in the environment for up to a month. Then people breathe it in, and most people who breathe the leprosy germ in then mount protective immune response to it. So, I've worked with leprosy in India and Ethiopia, and I've obviously met the leprosy germ many times and so I've presumably, although I've not tested myself, developed protective immunity to it. And that's what most people who live in leprosy endemic countries do.
Ben - So, it gets into our system through the lungs, but what does it actually do to the body once this bacterium is in there? What does it do?
Diana L. - Well, there are two critical things. Firstly, it has a receptor to bind to the nasal mucosa that crosses the nasal mucosa and then it binds to macrophages and also to Schwann cells in peripheral nerves. That's important because that's how you get the clinical signs of leprosy.
Ben - Schwann cells are the cells that actually make the protective coating for our nerves, aren't they? So if they're binding to these cells, they're stopping our nerves from being protected properly and our nerves will therefore break down.
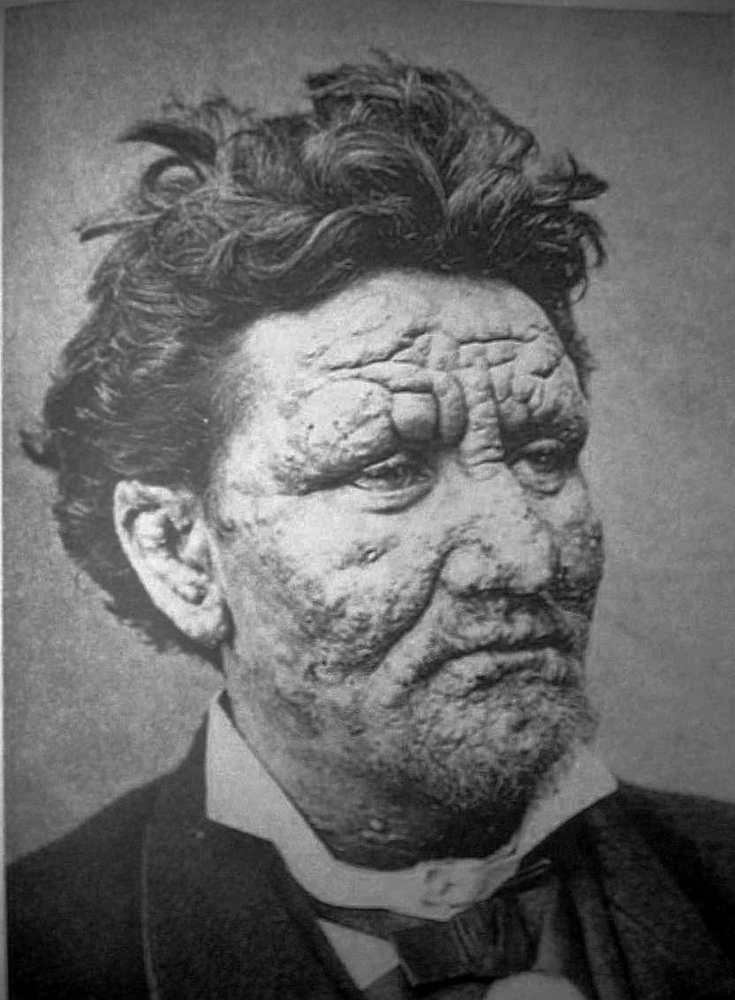 Diana L. - That's right, yes and so, one of the very important signs of leprosy is loss of nerve function which is manifest as either losing sensation in your hands and feet, or losing power in your hands and feet. People have this idea that leprosy eats away your body, but it doesn't actually eat away your body, what happens is that you lose pain sensation in your hands and feet, and then you don't feel injuries, and so, you get what we call traumatic injuries.
Diana L. - That's right, yes and so, one of the very important signs of leprosy is loss of nerve function which is manifest as either losing sensation in your hands and feet, or losing power in your hands and feet. People have this idea that leprosy eats away your body, but it doesn't actually eat away your body, what happens is that you lose pain sensation in your hands and feet, and then you don't feel injuries, and so, you get what we call traumatic injuries.
Ben - So, the stereotype that leprosy causes your fingers to drop off is not actually because your fingers drop off as a direct result of the presence of the bacteria, but because you injure your fingers so often because you don't feel the pain there any more, that you're quite likely to lose fingers, toes, and other extremities through that mechanism.
Diana L. - Yes, that's right and so, when you diagnose a new patient with leprosy, it's really important that you do a careful examination to find out if they've got undetected loss of sensation in their hands and feet, and then institute a kind of health education programme with them, which obviously will be very much guided by the kind of activities that that person does. So, for instance if you're a farmer in Africa, you might be at risk by walking too far or holding your hoe too tightly; but if you're an Indian housewife, your danger area is the kitchen, and it's very easy to burn yourself in the kitchen.
Ben - So, how is it actually treated? Can we use standard antibiotics?
Diana L. - Yes, we've got very good antibiotics for treating leprosy and the key is a drug called rifampicin and every patient with leprosy will get a combination of either two or three drugs, antibiotics against leprosy, and they will take them for either 6 or 12 months. The beauty of the rifampicin is that you only have to take it once a month because, again, the Mycobacterium leprae is a very slow growing organism and so fortunately, we only have to take the rifampicin, once a month. The other antibiotics you have to take every day.
Ben - Is this a cure for leprosy or is it merely a case of, once you've contracted it, we have drugs that can manage it, and you get to end up with these drugs for the rest of your life?
Diana L. - No. It cures you of the infection. What it doesn't cure you of is the inflammation that goes with this. We talked about the Mycobacterium going to the Schwann cells and the skin macrophages, and what happens then is that the body then mounts an inflammatory response. That is far more difficult to switch off and that can go on for a long time. So, patients will quite often need to have a course of steroids along with their antibiotics to try and switch off that inflammation because it's that inflammation that's destroying the nerves.

38:18 - Leprosy in the Past - the Story in the Bones
Leprosy in the Past - the Story in the Bones
with Professor Charlotte Roberts, Durham University
Diana - Now, to help us understand leprosy, it's important to look into the past and see what evidence we can find from when and where it's prevalent. One way to do this is to look for the marks it leaves on the bones. Joining us now is Professor Charlotte Roberts, a bioarchaeologist from Durham University; she studies evidence for disease in skeletons that are excavated from archaeological sites... Hello.
Charlotte - Hello.
Diana - So what is the evidence of leprosy in bones? How do we spot it?
 Charlotte - Well, it primarily affects the bones of the face, the nasal area where the bacteria, as Diana [Lockwood] has just said, is inhaled and you get destruction of those areas of the face. It also affects the nerves, again as Diana has said, where you get loss of sensation, and loss of proper function of the muscles or the nerves supplying the muscles. And so, all these manifestations of leprosy can affect the bones, so we get the loss of bone from the upper jaw, loss of front teeth, perforated palette bones in the skull, and then because of development of ulcers on the hands and the feet due to lack of sensation in those areas, you'll get involvement to the bones of the hands and the feet, and you'll get loss of parts of those bones.
Charlotte - Well, it primarily affects the bones of the face, the nasal area where the bacteria, as Diana [Lockwood] has just said, is inhaled and you get destruction of those areas of the face. It also affects the nerves, again as Diana has said, where you get loss of sensation, and loss of proper function of the muscles or the nerves supplying the muscles. And so, all these manifestations of leprosy can affect the bones, so we get the loss of bone from the upper jaw, loss of front teeth, perforated palette bones in the skull, and then because of development of ulcers on the hands and the feet due to lack of sensation in those areas, you'll get involvement to the bones of the hands and the feet, and you'll get loss of parts of those bones.
Diana - Okay, so it sounds like it's mostly skull, hands, and feet.
Charlotte - That's right, yes.
Diana - But do you see any other diseases which affects bone in a similar way that could be confused with leprosy?
Charlotte - Yes. In the skull, you may get people with tuberculosis or indeed, syphilis where you'll get similar changes, but what we're always trying to do when we're looking at skeletons, is to look at the distribution pattern of the lesions that we see in the bones, which helps us make specific diagnoses. And so, if you got a complete skeleton, I'll have to admit it's not often in archaeological sites where the whole skeleton is preserved, you can look at the distribution pattern and you can be pretty safe when you have someone who's been suffering from leprosy.
Diana - So the more of the body you've got, the better.
Charlotte - That's right.
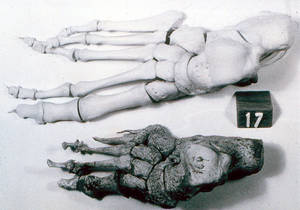 Diana - So, can we confirm a diagnosis just from the bones or can you use other techniques? Has DNA been used on them?
Diana - So, can we confirm a diagnosis just from the bones or can you use other techniques? Has DNA been used on them?
Charlotte - Yes. Since 1994 actually, people have started to extract the DNA of the bacteria that causes leprosy from bones of the skeleton quite successfully. In many cases, this has confirmed a diagnosis where we have seen the bony changes that we would recognise as leprosy and then the DNA has confirmed that diagnosis. People have also taken histological sections from bones and found particular patterning in those histological sections that are recognisable as leprosy. So, yes, there are other methods that we can use, but most people don't have access to that methodology and tend to just look at the visual signs of leprosy in the skeleton.
Diana - Yeah, I suppose that the beauty of looking at the bones is that you can almost identify it in the field on site.
Charlotte - Yeah. I mean the other thing to say is of course, depending on how resistant you are to the bacteria, you'll develop a different patterning of bony changes in the skeleton. So if you're very resistant to the bacteria, depending on your immune system strength, then you may not develop the very obvious signs, but if you're not very resistant to the bacteria, it'll be very obvious in the skeleton.
Diana - Okay, so when do you get the first evidence of leprosy? What's the oldest skeleton that's been found?
Charlotte - Well, there've been suggestions that we've got evidence from about 2500 BC in Turkey and in Nubia, and in India about 2000 BC. There is a suggestion that a child skeleton from a Scottish site dated to 2000 BC, but that hasn't been confirmed yet.
Diana - So it's pretty ancient then?
Charlotte - It is pretty ancient, but it doesn't really increase in frequency until about the 12th to 16th century in Europe, and then it really seems to increase in frequency, along with the introduction of leprosy hospitals which were founded around that time.
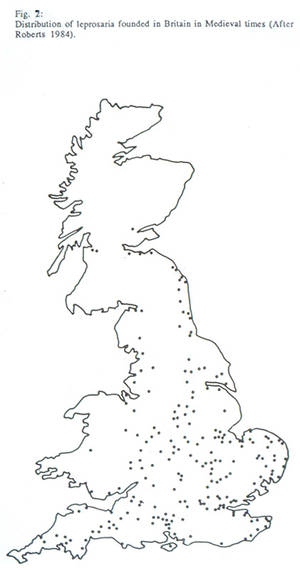 Diana - Of course, in the leprosy hospitals, I think most people will have heard about. So, can you tell us a bit about hospitals? How many were there, just in Britain for example?
Diana - Of course, in the leprosy hospitals, I think most people will have heard about. So, can you tell us a bit about hospitals? How many were there, just in Britain for example?
Charlotte - Just in Britain, probably over 300 in England alone and mainly founded in the south and east, and this was between the 11th and 16th centuries. They tended to be founded by wealthy benefactors who were really concerned about their own salvation, and they really controlled admissions. Whether you got admitted, if you were diagnosed with leprosy, depended on how rich you were and maybe your religious affiliation, and maybe sex. You know, maybe the males got admitted more than the females.
Diana - Most people say that these leprosy hospitals were sort of built outside cities and that people with leprosy were kind of sidelined or marginalised from mainstream society. So, do you think this is true?
Charlotte - I don't think so, no because recent evidence that I've looked at suggests that the majority of individuals with the bony changes of leprosy were not actually buried in leprosy hospital cemeteries. They were buried in the normal community cemetery and that, I think, suggests that perhaps, our assumption that everyone was stigmatised in the past doesn't hold true, and that communities actually accepted these people.
Diana - I wonder where this idea comes from then...
Charlotte - Well I think it's a view that was actually forwarded in the 19th century and that was based on their medieval evidence. I think the historical data that's been looked at by people like Carol Rawcliffe at the University of East Anglia, and myself looking at the skeletal evidence for leprosy, has really turning those assumptions we have about how people were treated with the leprosy and the past over.
Diana - Well, as my director of studies used to say, "History is the handmaiden of archaeology."
Charlotte - Certainly.
Diana - That was Professor Charlotte Roberts and she's from Durham University. Thank you.

Does leprosy interact with TB and other diseases?
Charlotte - Well, we see evidence for both leprosy and tuberculosis in skeletons, and the suggestion is that, in Europe, leprosy declines [after] about the 14th century while tuberculosis takes off as a major infectious disease and there's a belief that that's linked to increasing urbanisation and close-living between individuals. Leprosy and tuberculosis are both caused by Mycobacteria, but different species; so Mycobacterium leprae versus Mycobacterium tuberculosis; and there's a suggestion that increasing exposure to tuberculosis will reduce the chances of contracting leprosy. And it's actually quite interesting to see that evidence in skeletons early-on in that medieval period tends to be the low-resistant form of the disease. People are expressing the disease in their skeletons very obviously and as time goes by when you get into the 16th and 17th centuries, they're getting a less severe form of leprosy, something called tuberculoid leprosy, suggesting that they're more resistant to the bacteria. But there's also less evidence of leprosy during those periods too.
Diana - I suppose one of them might kill you a bit faster than the other....
Charlotte - Yes and in fact today, one of the major causes of death in people with leprosy is tuberculosis.
Ben - Well that of course, brings me on to the modern clinical perspective. Diana, do you see these infections together very often?
Diana L. - You certainly see them together, but not very often, no.
Ben - And are there any other interactions between different diseases? Of course, there are things like HIV which are in the same parts of the world as you were saying, we still see leprosy. That knocks your immune system almost totally dead. Does that mean that leprosy runs absolute riot?
Diana L. - We were very worried at the beginning of the HIV epidemic, that we would see a lot more leprosy and a lot worse leprosy cases. But what's actually happened is that having HIV doesn't seem to make you more likely to get leprosy. Paradoxically, what we have seen, now that people have antiretroviral treatment, is that when they do get leprosy, they get leprosy with a lot more immune activation and the inflammation that I was talking about earlier, occurs in a very florid form, and it's quite difficult to switch off again.
Ben - So it actually complicates the issue quite a lot.
Diana L. - Yes, it does.
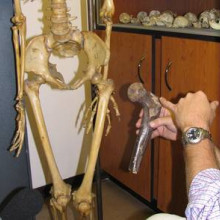
Can one saw somebody's femur in half, and figure out how old the person was?
Charlotte - Well we try not to saw femurs in half to find out age. We normally look at degeneration, particularly of the pelvis and the ribs and the skull, particular features that we recognise as being associated with age. However, having said that, it's not a very accurate science, because people age and degenerate in different ways and at different rates, but you can actually look at the microscope structure of bones like the femur, and looking at a particular picture gives a closer correlation to the age at death of that individual. But you can also look at teeth and you look at the roots of teeth. As you get older, they become more translucent if you put a light behind them, and that's better correlated with age at death too, but that's not a destructive method like you would do for the femur.
Diana - I understand that once adults start dying after the age of 35, that's when it's really difficult to assign an age to their body. So, which is the best method for doing those adults?
Charlotte - Well, it's looking at the cut femurs and the teeth really, but most people again really don't have access to the technology to do that. But I think the idea that everyone died young in the past doesn't hold true because I don't think our methods are really well-developed enough to pick out those people in the older age groups yet.

49:02 - What happens if you use 99.9% effective sanitizer twice?
What happens if you use 99.9% effective sanitizer twice?
We put this question to Jane Greatorex from the Health Protection Agency in Cambridge:
Jane - Well, it's not a straightforward answer. The 99.9% claim that manufacturers put on their products is true based upon the tests that they carry out, but these are carried out under laboratory conditions in test tubes and on plates. It's a little bit more complicated than that in real life and it really depends on what we're talking about here. If we're talking about a cough droplet, a cough droplet might contain about 200 million 'flu germs in the winter season and about a million or so bacteria; and if you use that hand gel, then you will indeed get the numbers of viruses and bacteria down probably to levels below that which is infectious. However, you will not remove all of them and that's because of two things. One, your hands are very good at retaining bacteria and viruses, and two, the numbers of bacteria and viruses that you start with are such that even 0.1% is still a big number of bacteria and viruses. If you kill even that 0.1% with another hand wash, you'll still be left with some remaining.
Now if, for instance, we were talking about faecal contamination - not a nice subject, but then we're talking about much larger numbers of viruses and bacteria, and the big complication there is, you need fewer of those to cause an infection. So, the straight answer is, you won't remove all the bacteria and viruses, and that's in some situations, it's really not very good news.
Diana - Two scrubbings will remove more germs, but 99.9% of a lot is still going to be a lot. It all depends on what the infectious doses of a specific pathogen. If you only need one bacterium to infect you and sometimes even the most thorough washing isn't enough.
- Previous Better Biofuel? Ask a cow...
- Next Retroflectors










Comments
Add a comment