Hepatitis in the Clinic
Interview with
Ben - As part of World Hepatitis Day, we were taken on a tour of the scientific and clinical research facilities. This was a great opportunity to really understand the research in its proper context and a view behind closed doors for the Hepatitis patients who had come along. To understand more about clinical approaches to hepatitis, I spoke to Professor David Adams. David is a medical doctor as well as a Professor of hepatology and so ideally suited to explain how the scientific research impacts on clinical applications. David first explained the difference between the different kinds of Hepatitis.
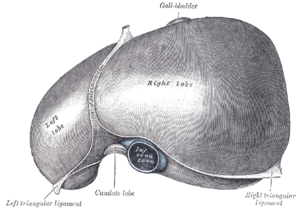 David - There are four different types of hepatitis that we commonly see; called A, B, C and E. D is a rare virus, which is an obligate parasite of B. But to talk about the four main ones, A and E are similar in that they are both transmitted via the oral route, so they are particularly at risk where you have areas or poor sanitation. Both of those viruses predominately cause acute infection, which resolves without long-term sequelae. A very small proportion of patients may unfortunately develop a really severe Hepatitis and go into liver failure but the majority of patients recover and don't have any chronic, persistent infection. That really sets those two viruses apart from hepatitis B and C , which can both be associated with chronic infection.
David - There are four different types of hepatitis that we commonly see; called A, B, C and E. D is a rare virus, which is an obligate parasite of B. But to talk about the four main ones, A and E are similar in that they are both transmitted via the oral route, so they are particularly at risk where you have areas or poor sanitation. Both of those viruses predominately cause acute infection, which resolves without long-term sequelae. A very small proportion of patients may unfortunately develop a really severe Hepatitis and go into liver failure but the majority of patients recover and don't have any chronic, persistent infection. That really sets those two viruses apart from hepatitis B and C , which can both be associated with chronic infection.
Hepatitis B, worldwide, is a huge problem in countries where it's endemic, that is where the virus is always present in a high proportion of the population. It tends to be contracted by children in the neo-natal period. Those patients tend to develop long-term, persistent infection without a lot of liver damage but later on in life that can cause a slow progression to chronic hepatitis and cirrhosis and liver cancer, so that's one of the main causes of cancer in the developing world. In the Western, developed world, hepatitis B is more usually contracted as an acute illness in adults, usually via sexual transmission, where it can present with an acute hepatitis that resolves but, in a proportion of patients, probably 20-30%, the virus persists and those patients become chronically infected and will need long-term follow-up and, possibly, treatment to prevent them going on to develop cirrhosis and liver cancer.
Hepatitis C is a different type of virus to hepatitis B. hepatitis B is a DNA virus, whereas hepatitis C is an RNA virus. It's also contracted via the breaking of a body barrier such as a mucosal membrane or, particularly, blood and is usually contracted through contaminated blood products either by treatment in the developing world with unclean needles, or intravenous drug use in the developed world. And the problem with hepatitis C is that probably in about 80% of patients who are infected, they will not get rid of the virus. They may not even know they've been infected. The acute illness is usually very mild but 80% will go on to develop chronic infection and of those 80%, a proportion, probably 20-30%, over a long period of time will go on to develop scarring, cirrhosis, liver failure and liver cancer.
Ben - So hepatitis leads to liver damage which, in turn, can lead to liver cancer. What are our options for treating it once the damage is there?
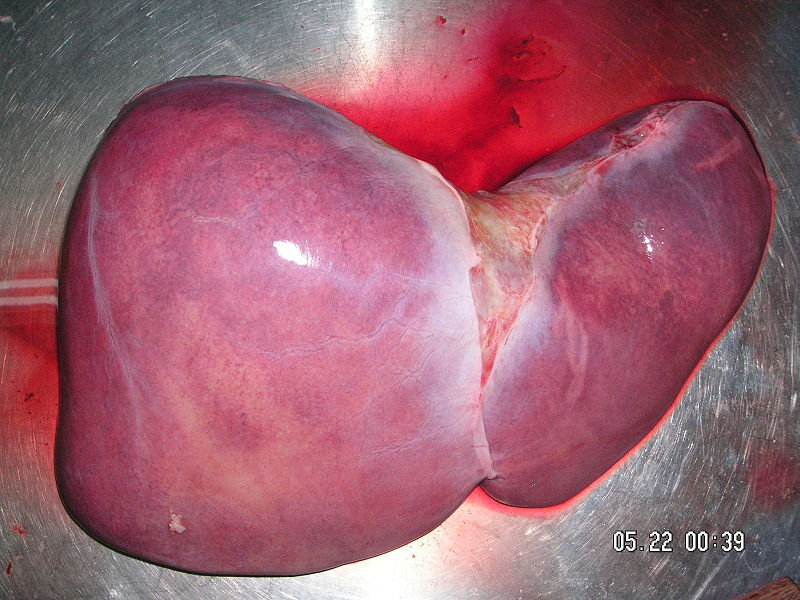 David - Once the damage has been done and the patient has got cirrhosis and end-stage liver disease, either in the form of liver failure or, as you say, the development of liver cancer, then we don't really have any medical options and the only option is liver transplantation. There are several problems with liver transplantation; one being that there is a shortage of donors, so there's a waiting time and there aren't enough donors for the number of recipients we would like to transplant. The second problem is the transplant doesn't, unfortunately, get rid of the virus because the virus seems to hide in other sites in the body, we're not quite sure where, but almost invariably after the transplant the liver gets re-infected with the virus so the recurrent infection and recurrent hepatitis disease is a real problem. Many of these patients will end up needing to be re-transplanted because the disease has recurred. As far as liver cancer is concerned, transplantation is a problem because we know that we can only successfully transplant somebody with liver cancer if we catch the cancer early enough. Once it's grown beyond a few centimetres in diameter we know from experience that after the transplant the cancer will rapidly come back. So it's very important that patients with cirrhosis, with end stage liver disease, are screened. We have blood tests and ultrasound scans that we can do to screen for liver cancer and if we pick it up in early stage then get them, if appropriate, onto a transplant waiting list as soon as possible so we can transplant them before the cancer has spread too far. But it's going to be important in the future to combine transplantation with drugs that prevent the replication of the virus and the re-infection of the liver with the virus and this has been very effectively done nowadays in hepatitis B so that hepatitis B infection was a contra-indication to liver transplantation because the patients all got re-infected and died. Now, actually, with antiviral therapies, which are very effective, it's one of the best indications for liver transplantation. So hopefully we'll be saying this about hepatitis C infection in the future.
David - Once the damage has been done and the patient has got cirrhosis and end-stage liver disease, either in the form of liver failure or, as you say, the development of liver cancer, then we don't really have any medical options and the only option is liver transplantation. There are several problems with liver transplantation; one being that there is a shortage of donors, so there's a waiting time and there aren't enough donors for the number of recipients we would like to transplant. The second problem is the transplant doesn't, unfortunately, get rid of the virus because the virus seems to hide in other sites in the body, we're not quite sure where, but almost invariably after the transplant the liver gets re-infected with the virus so the recurrent infection and recurrent hepatitis disease is a real problem. Many of these patients will end up needing to be re-transplanted because the disease has recurred. As far as liver cancer is concerned, transplantation is a problem because we know that we can only successfully transplant somebody with liver cancer if we catch the cancer early enough. Once it's grown beyond a few centimetres in diameter we know from experience that after the transplant the cancer will rapidly come back. So it's very important that patients with cirrhosis, with end stage liver disease, are screened. We have blood tests and ultrasound scans that we can do to screen for liver cancer and if we pick it up in early stage then get them, if appropriate, onto a transplant waiting list as soon as possible so we can transplant them before the cancer has spread too far. But it's going to be important in the future to combine transplantation with drugs that prevent the replication of the virus and the re-infection of the liver with the virus and this has been very effectively done nowadays in hepatitis B so that hepatitis B infection was a contra-indication to liver transplantation because the patients all got re-infected and died. Now, actually, with antiviral therapies, which are very effective, it's one of the best indications for liver transplantation. So hopefully we'll be saying this about hepatitis C infection in the future.
Ben - So what are our current treatment options?
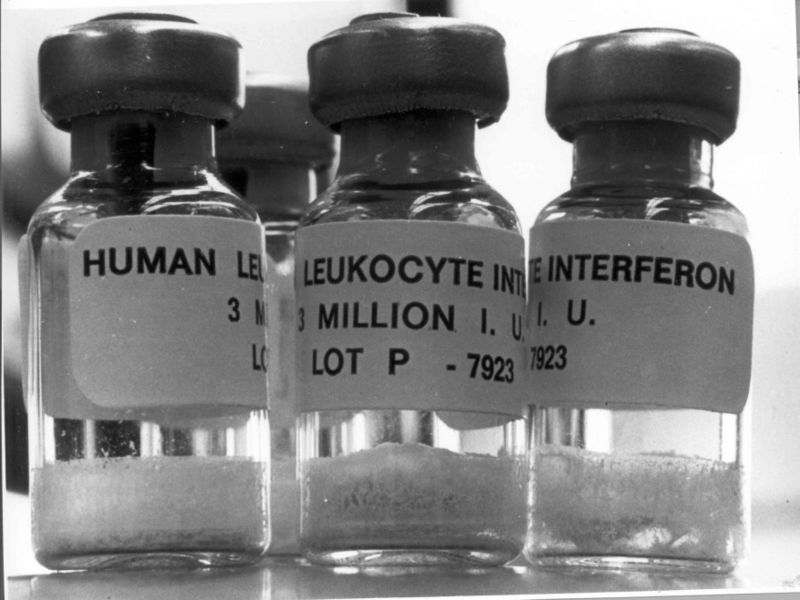 David - So the current treatments are based around interferon, which is a naturally occurring antiviral factor produced by the patient's own body when infected by a virus. Particularly a form of interferon called pegylated interferon, which means it's linked to a chemical which makes it last longer in the body than it would otherwise. And that's given by injection and that's combined with a drug called ribavirin, which has some weak anti-viral properties but seems to work very well in combination with interferon. So those are the current, standard treatments and there are a range of new treatments coming into clinical trials at the moment. We hope that these will come into clinical practise in the future but our mainstay at the moment is interferon and ribavirin.
David - So the current treatments are based around interferon, which is a naturally occurring antiviral factor produced by the patient's own body when infected by a virus. Particularly a form of interferon called pegylated interferon, which means it's linked to a chemical which makes it last longer in the body than it would otherwise. And that's given by injection and that's combined with a drug called ribavirin, which has some weak anti-viral properties but seems to work very well in combination with interferon. So those are the current, standard treatments and there are a range of new treatments coming into clinical trials at the moment. We hope that these will come into clinical practise in the future but our mainstay at the moment is interferon and ribavirin.
Ben - Interferon works by encouraging the body's own defences to kill off infected cells. What are the side-effects?
David - The side effects are really, pretty much, that it makes you feel like you've got flu because when you get flu it's interferon that's released, so patients can get headaches and feel agitated. One particular side effect which can be really quite profound is depression. Many people, when they get a bad viral infection, such as influenza, do feel profoundly depressed before, during and after the infection so some patients just can't cope with the interferon because of the effect it has on their mental well-being. The side-effects tend to go off with time and they can be treated but they're not inconsiderable and some patients just can't tolerate it and have to stop treatment early.
Ben - So killing off infected cells with interferon seems a bit like taking a hammer to the problem. Are there no more subtle ways around it? Can we stop the virus replicating or can we stop it getting into cells in the first place?
David - Well that's the aim of the new generation of drugs, to be much more specific and to tackle different parts of the hepatitis C machinery that blocks its ability to reproduce or, as you say, even better than that, that's blocks its ability to actually get into the cells. Those drugs are potentially very exciting and some of the early trials look very promising, but as with all antiviral drugs, one of the concerns is always that the virus will mutate and become resistant to these agents, so we need to look out for that very carefully. And at the moment none of these drugs are licensed for routine use; they're all still at the trial stage but I think the next few years is going to be an exciting time for new therapies.
Ben - That was Professor David Adams, who's confident that we'll see developments in hepatitis therapies in the next few years.










Comments
Add a comment