A Life with Marfan Syndrome
Being told you need heart surgery for the first time is a unique experience: a  moment that is now forever engraved in my memory. I'm usually good at handling bad news, or I'm at least used to it by now after already having three previous operations. It's a different experience though, understanding that you are treading a path that family members have gone before you, knowing they didn't get a happy ending. People tell you to 'stay positive' but when you learn that your aorta is creeping towards a life-threatening tear you reach a place in your mind you cannot get back from.
moment that is now forever engraved in my memory. I'm usually good at handling bad news, or I'm at least used to it by now after already having three previous operations. It's a different experience though, understanding that you are treading a path that family members have gone before you, knowing they didn't get a happy ending. People tell you to 'stay positive' but when you learn that your aorta is creeping towards a life-threatening tear you reach a place in your mind you cannot get back from.
When you get news like this, sometimes people say 'it's just one of those things', but in my case it definitely isn't. There's a reason behind my somewhat rocky childhood and teen years and that reason is Marfan Syndrome. It's a genetic disorder, which causes a variety of different symptoms in each case; I inherited it from my Mother, who hasn't had as many troubles as I have. Whilst the condition is usually passed on from parent to child it is possible to be the first person in a family to have the disorder; spontaneous cases are predicted to occur about 25% of the time.
Marfan is caused by a mutation in the gene that tells the body how to make a protein called fibrillin-1. This protein is important in making connective tissues, which are found throughout the body. The abnormal production of fibrillin results in parts of the body being able to abnormally stretch and can cause some bones to grow longer than they should. Since connective tissue is found across the whole body this means that there are a wide variety of problems that can occur as a result of having the condition. However, features of the disorder are most often found in the heart, blood vessels, bones, joints and eyes. The most common problem associated with Marfan are aortic aneurysms which can then lead to aortic dissection, a tear in the wall of the heart. This is a life threatening problem and the most common cause of death in people with Marfan.
It's estimated that around 1 in 5,000 people have this condition, so it is rare but not so rare that doctors shouldn't be aware of it. So often I will be met by a GP whose knowledge on my condition is lacking, and they simply Google it in front of someone who has much more knowledge and personal experience of the issue. The most common scenario, however, is that I will meet a medical professional who knows of the aortic involvement in Marfan and perhaps some of the key characteristics, but when it comes to some of the other symptoms that can arise as a result of this condition I often get back a blank stare. Many times have I been met with comments such as 'Marfan doesn't cause pain', in direct contradiction to my personal experience of an extensive history of severe chronic pain.
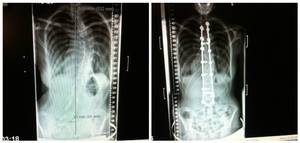
Marfan does affect everyone differently so it can be possible to have the condition and not suffer any significant pain, but unfortunately for me I definitely sit on the more severe end of the spectrum. Growing up, the pains started in my knees alongside swelling; it was labelled as 'growing pains' and every now and then they gave me six weeks of physiotherapy. That was over ten years ago and my knees still are swollen and painful most of the time: growing pains I think not. Then came my first proper secondary condition diagnosis, Scoliosis. Scoliosis is a sideways curvature of the spine, a common diagnosis amongst teenagers, however things get more complicated when you have a connective tissue disorder as well. My curve was small at first and my consultant predicted that I wouldn't need any intervention at all; he had wrongly assumed that I had already done most of my growing. In the space of just six months my curve progressed from 27 degrees to nearly 50 degrees, with my pain ever increasing as well. I was put on the waiting list for spinal fusion surgery; the plan was to straighten my spine using metal rods and screws. Things didn't go all that smoothly though, as just a few days after the operation I was having severe pains down my right leg, pains that I recognised as possibly being nerve related. They weren't investigated and were simply noted down as being a separate Marfan related problem. It took six months to look into it further, six months of me spending most of my time in bed as sitting and standing were far too painful. At nearly a year post op I was wheeled into the operating theatre once more to correct the problem, CT and MRI scans had shown that there was a screw sitting on a nerve. Luckily the surgery was much more successful that time and after a few months recovery I felt like I could return back to 'normal' life, I was looking forward to rejoining my friends at sixth form.
 |  |
|---|
Marfan was about to strike again though, less than six months after my second surgery I found myself at the doctors trying to get my GP to listen to me about ongoing hip pains I'd been having. He did a few movements tests and decided that my hips were apparently normal; I had a gut feeling though that something was wrong so I pushed for a referral. Luckily I managed to get referred to a hip surgeon who had a pretty decent knowledge of Marfan and some of the secondary conditions that could occur, one of them being protusio acetabuli. It's an uncommon defect of the acetabulum, which is the socket that holds the femoral head to make the hip joint. This defect simply causes the socket to be too deep and it may protrude into the pelvis, a condition that is linked to Marfan. X-Ray scans quickly revealed that I had this in both hips and further CT and MRI scans found that my right hip was more severely affected. I was told that both hips would need replacing but since the right side was more damaged and had more severe cyst formation it was decided that it would need operating on first so, at the young age of 18 I sat in a ward full of elderly people waiting to undergo my first hip replacement. Hip replacements don't last for life though and whilst my surgeon cannot predict how long this one will last it is entirely possible that it will need replacing several times throughout my lifetime.
 |
|---|
It wasn't until I started getting more and more Marfan related diagnoses, like the hip problem, that I decided to look at the extensive list of possible secondary conditions that can arise due to the syndrome. Marfan is more than just what it says on the tin, the list of linked conditions and symptoms is long and my most recent related diagnosis is dural ectasia and a large sacral tarlov cyst. It's estimated that the majority of people with Marfan also have dural ectasia which is the ballooning of the dural sac surrounding the spinal cord. Most people probably won't ever suffer any symptoms but it can cause lower back pain, headaches, weakness and numbness. Tarlov cysts are less associated with Marfan but are equally as linked as I found out recently when a CT scan revealed that I had a large tarlov cyst in my sacrum area that had eroded away a lot of the bone. This gave me a reason as to why I had been suffering with severe lower back pain for well over a year, pain so severe that it had left me needing to use a powerchair and being unable to even sit up comfortably for more than half an hour, sometimes less. Both problems are difficult to treat, and I've got to the stage with Marfan where my treatment is based on managing my pain and increasing my quality of life, rather than striving to solve the problems.
This is usually the case when it comes to a lot of the symptoms that can arise due to the syndrome, problems are managed the best they can be, as and when they arise. When it comes to the cardiac side of this condition though, the involvement of the heart and blood vessels, things are tightly monitored and it isn't about waiting for something to happen, it's about catching the problem before it arises. The most serious and life threatening part of Marfan is the potential aortic aneurysms that you can get and the only successful treatment is major surgery. Right now we don't have any other treatments that make a significant difference but new research is hoping to change that.
For the first time
researchers at the University of Cambridge have been able to create blood vessel tissues in a petri dish which mimic Marfan syndrome in human arteries. They have used these blood vessel models to gain more of an understanding as to how the condition can lead to such catastrophic and fatal aneurysms. The researchers have found that the pathway initially thought to be responsible for the development of aortic aneurysms in people with Marfan actually only makes up part of the picture, they were able to tell that a separate pathway was in fact more critical in causing them. We hope that this new research will enable them to go on to use the vessels to test drugs which target this new pathway, looking at their potential to prevent people with the syndrome from developing these kinds of aneurysm.
This new research comes too late for me, as I know that major open heart surgery to replace my aortic root is unavoidable, but this does give me hope for the next generations. These findings could mean that people with Marfan in the future won't have to undergo heart surgery at such young ages; they might be able to continue to live a healthy live without major intervention for longer. The research could prove to be life changing for people with the syndrome and it could totally change the way we look at such serious complications and the treatments that can be offered to people. For now though this gives myself and others with the condition hope, having a rare condition can often be isolating and frustrating so just knowing that there are people out there trying to improve our lives is enough for many of us, I know that it is certainly enough for me.




Comments
Add a comment