The Genetics of Brain and Behaviour
Could genetics pave the way for developing schizophrenia or Alzheimer 's disease? Is there a genetic link between optimism and obesity? Is it ethical to screen people's DNA? Plus we find out what a nap might do for your memory, how a new study is turning addiction treatment on its head and we unravel what it means to be human. Plus we unzip whether DNA might make for an extremely high IQ!
In this episode

- Cure for carbon monoxide poisoning
Cure for carbon monoxide poisoning
A breakthrough therapy to rescue the tens of thousands of people killed or injured each year by carbon monoxide poisoning has been developed by scientists in the US.
Carbon monoxide is a colourless, odourless gas present in car exhausts and boiler flues. It's toxic because it binds tightly to haemoglobin in the blood and prevents it from delivering oxygen to our tissues.
Vulnerable organs, like the brain and heart, can suffer irreversible and often fatal damage owing to oxygen deprivation. Currently, the only therapy for the thousands of people poisoned each year is oxygen therapy, which can slowly drive off the carbon monoxide and restore oxygen levels in the tissues.
Sadly, this often comes too late for many victims, largely because it requires specialist facilities that are long distances away. Now a team at the University of Pittsburgh led by Mark Gladwin have developed an injectable molecule that loosens carbon monoxide's grip on our haemoglobin and allows the kidneys to dispose of it safely.
The new molecule is a modified form of a chemical found in the brain called "neuroglobin". This is a haemoglobin-like chemical used by nerve cells to defend themselves against biochemical stress and low oxygen levels.
Searching for a better understanding of its actions, Gladwin and his team switched a handful of the amino acid building blocks that form part of the neuroglobin protein. The resulting molecule turns out to be a chemical rottweiler that binds carbon monoxide 500 times more powerfully than haemoglobin.
Added to carbon monoxide poisoned red blood cells, the modified neuroglobin tears off the carbon monoxide and restores the haemoglobin to its former state within seconds. Normally it would take hours for carbon monoxide to relinquish its hold.
The results were so impressive that the Pittsburgh team then tried injecting the new molecule directly into mice suffering from carbon monoxide exposure. Compared with control animals, the treated mice all survived and there were no obvious signs of biochemical damage.
Measurements show that, once the modified neuroglobin sequesters a carbon monoxide molecule, it reverts to a form that can be filtered rapidly into the urine by the kidney and then exits the body harmlessly.
According to Gladwin, an intervention like this could be deployed aboard ambulances and with fire crews so that victims of carbon monoxide poisoning could receive rapid "at the scene" therapy, dramatically cutting the treatment times and improving outcomes. That said, he also acknowledges that a mouse is not a person, and they haven't yet determined whether their mice nevertheless still suffer brain damage despite receiving the treatment, so there's still work to be done...

- Is Alzheimer's genetic?
Is Alzheimer's genetic?
Dr John Rogers, Cambridge University - Well yes, there is some pathology around blood vessels in Alzheimer's disease. The main pathology in the brain is that there are abnormal proteins produced and deposited throughout the brain, but one of those is particularly deposited around blood vessels. We don't yet know whether that really makes significant contribution to the symptoms of Alzheimer's disease. Regarding the genetic control of it, yes, there is a gene which has significant influence on the incidence of Alzheimer's. it's called ApoE and people who have a particular version of this, an allele called ApoE4 are several times more likely to develop Alzheimer's disease than people with other versions of the gene. However, I have to say, at present, it doesn't seem worth testing for this because there's nothing we can do about it, but it is one more reason why we should generally keep a healthy diet and a healthy lifestyle because the main thing that ApoE does is to transport cholesterol into the brain. And there are some evidence that high cholesterol made from Alzheimer's disease as well as other ills that they affect us in our older years. There are many projects trying to use this kind of research to develop cures or prevention for Alzheimer's disease and some of these are in clinical trials, but nothing has been very successful as yet. So at the present, the best advice one can give is to keep intellectually active because it's known that people who are more intellectually active are less likely to develop Alzheimer's disease and to keep healthy lifestyles, keep physically active, and to try and keep one's cholesterol low.

01:05 - Stripping down Schizophrenia
Stripping down Schizophrenia
with David Porteous & Stephen Lawrie, Edinburgh University
Imagine your brain is being bombarded by information, coming in through all of your senses including hearing. You start hearing voices that other people can't, you can't filter them out. Your brain does its job and tries to make sense of them, tries to rationalise them...
Squeaky Gate Male - My voices make me think I am someone that I don’t want to be. They tell me that I love somebody else instead of my wife.
Squeaky Gate Female - They're all looking at me.
Hannah - You’re not sleeping, your thoughts become more and more disorganised and confused. Your perception of the world around you has changed. You don’t want to socialise as much and the voices escalate and amplify, becoming more frequent and more insistent. Hallucinations, hearing things that aren't really there. You start to experience delusions as a result, strong beliefs in something that may not be true, causing you to act in a particular way.
Squeaky Gate Male Two - I thought they were trying to kill me and so, I ran away with my 4-year-old son.
Hannah - That were students at the local mental health charity, Squeaky Gate, speaking about their experiences. We’ll be finding out about the genetics and brain biology of Schizophrenia, a thought disorder that affects 1 in every 100 people worldwide. In order to do this, I visited Edinburgh University to talk to Cathy and Stephen.
Cathy was diagnosed with Schizophrenia over 30 years ago. It can be a debilitating disorder. 40 % of patients will attempt to suicide and up to 10 % of them succeed. These shocking statistics indicate that the medications currently on offer are not effective for every person, and it’s difficult to know which medication to put which patient on. So, more research is desperately required in this field. Cathy now volunteers for studies with Stephen Lawrie, Professor and Head of Psychiatry at Edinburgh University. They are trying to find out more about Schizophrenia to help improve treatments for the future. Cathy speaks with Stephen about her condition.
Cathy - Hello. This is my side as a patient. I actually had to be told, “You are ill.” I didn’t know I was ill. It took up to the age of 24 from age 18, to be told it was a Schizophrenic illness, and even then the psychiatrist diagnosed said that there's just looking in my case and they’ll give it that label because it helps the medical students to understand that it’s just a survey case.
I very rarely recall it but when the voices first started to talk to me they were accent less and they would penetrate in my eardrum and I was - got sick with fear. That is why I was put on medicine.
Stephen - So, can we talk about the voices a little bit because they're probably quite interesting for people to hear about?
Cathy - Yes.
Stephen - What sort of things do they say to you?
Cathy - Well, they give me an insight into just what humanity is all about. I am getting guided by voices. The UFOs got in touch with me. It was in the presence of a human form, and they were talking to me in my room for up to 4 months before I was admitted to the Royal Edinburgh Hospital with a suspected mental illness.
Because I hear them and nobody else does, what does that mean? I'm not imagining it. I'm on medication and I take the medication, and I still hear the voices. The medication does stop the voice from penetrating my eardrum to a point which is discomfort, and the voices go along with this
Hannah - That was Stephen, finding out from Cathy her experiences of Schizophrenia and the difficulties she had, getting diagnosed, and finding the correct treatment over the last 30 years.
And we’ll be speaking Professor Stephen Lawrie again shortly to discover what his research has told us so far. But first, I go in to search of a genetic contribution to Schizophrenia. I met with Professor David Porteous from Edinburgh University who tells me about some of his work, unravelling the role of genes in this disorder.
David - Some years ago, in fact in 2000, just at the turn of the Century, we were able to report that we’d identified a very unusual new gene, a gene that we knew nothing about before – that when it was damaged, led to a very high probability that individuals inheriting that damaged version of gene would develop a number of different possible types of psychiatric illness. So, some of the individuals within the same family developed Schizophrenia, some bipolar disorder, and others are a recurrent form of major depression.
Hannah - And what were the percentage risks for developing these psychiatric disorders then with this gene change?
David - About 2/3 of the individuals carrying the gene change developed a profound, clinically important psychiatric disorder, but a third didn’t. Now, that's quite interesting in itself. It reminds us that it’s not all to do with the genes. It reminds us also that the genes are important and not just for a particular type of psychiatric illness, but perhaps for a spectrum of illness. How might we understand that? Well, perhaps that's just chance, but perhaps more scientifically, perhaps it’s because there are other genes that were affecting whether or not you develop a very severe form of illness by Schizophrenia or a milder form like depression.
The other things that we have to take into account is that each individual is an individual with the different life experiences, with different life exposures. And that could also influence how a liability to a major mental illness actually develops over their life course.
Hannah - So, what's the role of this gene that you're working on? What does it do within the brain?
David - Well, that's a really interesting and very difficult question to answer because we’re actually still working out exactly what it does. But the thing that's very exciting about this particular gene which we call disrupted in Schizophrenia because that's what we’ve observed – is that it encodes for a protein, a building block in the brain, but that protein works with lots of other proteins in a way that it sticks them together and forms what we call ‘functional complexes’. And what those complexes do is help to determine how the brain develops in the very early stages of life, but also, how the brain signals one neuron to another, later on in life. So, it’s got this double feature to it. First, it is important in how the brain develops, and second, it’s important in how cells within the brain, the neurons signal one to another in adults.
Hannah - So, Schizophrenia has a neurodevelopmental origin, is that what you're saying and it’s also, there's some problem with communication from one nerve cell to another?
David - That's a very good way of summarising it. Yes, indeed, we have this notion that individuals at risk of Schizophrenia are born with that risk, but actually, the signs and symptoms tend not to develop until late adolescence and early adulthood. And so, they have a predisposition which is what we call neurodevelopmental in nature. Our hypothesis is that there are changes going on in the brain very early in life, but they are not manifest until later in life, and crucially at, and around the time of adolescence and early adulthood, and we have to try and explain that. And we think that in the discovery of this gene DISC1, and all the things that it does and regulates, that we’ve got a way to explain that.
Hannah - And you mentioned that families that have a history of DISC1 disruption in their genes, 2/3 of them will then go on to show some signs of psychiatric disorder. But how many people with Schizophrenia actually have this change in DISC1?
David - The answer to that is actually remarkably few and that’s been a bit of a puzzle, and it’s why some people have asked the question: Well, how important is all of these? And I think there are two answers to that. One answer is, actually, when you look at DISC1 alone, it perhaps only explains a small percentage of Schizophrenia, but when you look at the proteins, the other building blocks of the brain, the other signalling components of the brain that are influenced by DISC1, then the list gets much longer. And we’ve done some studies to suggest that perhaps as much as 5% of all of the risk of Schizophrenia could be ascribed either directly or indirectly to DISC1. So, when we think that 1% of the world’s population have a lifetime risk of Schizophrenia and we think that perhaps 5% of that 1% might be due to this one gene, that is a very, very large number of individuals. It’s more than that of course because this gene not only influences the risk of Schizophrenia, but also of bipolar disorder and of major depression. Now major depression carries about a lifetime risk of about 1 in 6. So we are talking about potentially a very profound influence on the risk of developing these illnesses in a very large number of individuals.
Hannah - That was Professor David Porteous from Edinburgh University, speaking about how genetic studies are telling us more about what's happening in the brain to give rise to Schizophrenia. These findings may be of help for patients in the future so they wouldn’t have to wait so long to get the right diagnosis and treatments as Cathy did. We now return to Professor Stephen Lawrie who describes what his studies with Cathy have helped to tell us so far.
Stephen - The research that we and other groups are doing has for example shown that we can predict Schizophrenia in those at high genetic risk because they come from multiple infected families, 2 or 3 years before people get the condition, because of changes in brain structure, reductions in the volume of particularly parts of the temporal lobe, 2 or 3 years before onset.
In terms of distinguishing features, Schizophrenia versus bipolar disorder, that looks like there might be simple differences in the volume of a structure called the amygdala which is an almond-shape structure at the front of your temporal lobe. But there are probably even more striking differences in terms of the appearances one gets on functional MRI, when one asks people to do a task in a scanner, you can get a variety of different patterns of blood flow in the two different conditions that look very promising in terms of being able to tease the conditions apart.
Of course, what you really want to be able to do is to use that kind of information to predict treatment response, who would need treatment, who’s getting it better anyway, who would need a particular type of treatment. And that work is really just getting started now.
Hannah - How sensitive are your techniques at the moment, particularly for differentiating between the different disorders of Schizophrenia or bipolar?
Stephen - They're about 70 to 80 % powerful in terms of being able to predict whether an individual who is going to go on to get Schizophrenia or in distinguishing groups of people with Schizophrenia from groups of people with bipolar disorder.
Hannah - So, given that we do seem to be getting there in terms of identifying scientific markers or biological markers for psychiatry, should these markers, these genes that David Porteous was talking about or the brain structure and activity changes that Stephen was talking about, or perhaps a combination of them all, should they be used to help screen people and start treating them even before they develop symptoms?
It’s a question that’s come in to play for breast cancer screening here in the UK recently and we discussed the ethical implications for this for psychiatry with David Porteous, getting his thoughts on the topic.
David - You're asking a question that often comes up and I'm actually rather on the side against this kind of approach even though I am very much a card-carrying geneticist. My view is that genetics is most important for trying to give us clues as to what might be going wrong in the brain, to understand better what’s going wrong in the brain, and then to be thinking about ways in which we might be able to think about the better use of medicines available to us today, and the way to make better medicines in the future.
But let’s not duck the question because this is an important one. So let’s use the example of identical twins. If we look at identical twin pairs and we have one presenting with a clinical diagnosis of Schizophrenia or bipolar disorder and we ask, “Well, what's the diagnosis in the co-twin?” And the answer is somewhere between 60 to 80% of the co-twins will have the same diagnosis, but not 100%.
So, are we thinking about treating an individual who might be at risk, but is not going to develop the illness? I think we’ve got to be very cautious about that and we’ve got to be very sure that the treatment really would be entirely harmless and also, fully protective.
I would rather see us thinking about more intelligent ways of making better medicines and have them available at the first sign of signs and symptoms. So, in order to try to dampen down the development of the illness and perhaps most importantly of all, one of the great problems we have in psychiatry is that the individual that turns up with the diagnosis will be put on the medicine that was last used that seem to work. And unfortunately, that choice is not always the best choice. So for many patients, not only does it take a long time to establish clearly what their diagnosis is, but also, it often takes a long time to find the medicine that’s best for them. If we could do that earlier, that would be a huge, huge advantage.
Hannah - That was Professor David Porteous and Professor Stephen Lawrie, and Cathy from Edinburgh discussing current gaps in knowledge of psychiatry and where science could help patients for the future.

15:60 - A Researchers Pick of Neuroscience News
A Researchers Pick of Neuroscience News
with David Weston, Cambridge University
It’s time to take a look at the top stories from this month, I join PhD student David Weston from Cambridge University. He’s been busy shifting through neuroscience research and comes up with his three favourite papers from the month...
David - So the first paper I’d like to talk about has really set the scientific community buzzing. It was published this week in the journal Nature by Luis Parada and his group over in the United States. The group were able to identify a specific subset of cells growing within brain tumours, a kind of cancer stem cell, and these cells are thought to be responsible for the regrowth of tumours after chemotherapy.
Hannah - So these cells could be the reason that tumours regrow even after chemotherapy. But how did the scientists find out about these new cells?
David - Well the scientists used a genetically engineered mouse model to fluorescently label this subpopulation of cells and track their survival during a course of chemotherapy and what they found was that while chemotherapeutic drugs managed to kill cells in the tumour, it failed to kill this small subpopulation. What they then went on to show was that when the tumour regrew the new tumour cells that were made were derived from these chemo-therapy resistant cells.
Hannah - So these cells are the parent cells of new tumour cells. Why do you think this discover is so critical in our understanding of cancer?
David - Well the results of this study seem to suggest that there may be a kind of cancer stem cell that could drive tumour growth, which has been a controversial idea in the field. Now that these cells have been identified we might be able to specifically target this them with drugs and stop the tumours from regrowing.
Chen et al. (2012) A restricted cell population propagates glioblastoma growth after chemotherapy. Nature, 488 (4709).
David - The next paper I want to talk about gives support to the idea that you can learn while you’re asleep. People have long thought that one of the primary purposes of sleep is the consolidation of memory, so the cementing of information in your mind, but this week Ken Paller and his colleagues at Northwestern University, have shown that this process of consolidation is enhanced if you also learn while you sleep.
Hannah - So learning while you sleep might not be a myth after all but how did Paller test this theory?
David - Well Paller and his colleagues taught 16 volunteers to play two different musical phrases using the keys on a computer keyboard and visual cues from a computer. They then let the subjects have an afternoon nap and when they entered a deep sleep one of the melodies they had been practicing that morning was played to them. Now when the subjects were tested after their nap they found that their accuracy for both of the melodies was better than before, but more importantly the accuracy for the melody that was playing while they were asleep was dramatically increased.
Hannah - So it seems that playing one of the melodies while the participants slept improved their abilities. Let’s hope that this kind of enhancement can carry over to other forms of information.
Antony et al. (2012) Cued memory reactivation during sleep influences skill learning. Nature Neuroscience, 15 (8), pp1055-1173.
David - The final paper I’d like to talk about describes what happens to the brain when you learn a second language. Now a lot of people say that it’s easier to learn languages when you’re younger because your brain is much more adaptable but the authors of this next paper, working at Dartmouth College, show evidence that even learning a second language as an adult can make big changes to the brain.
Hannah - So learning a new language can cause structural changes in the brain. How did the authors of this paper actually measure the changes in the brain?
David - Well Peter Tse and his colleagues used a brain imaging technique called diffusion tensor imaging which is a type of MRI scan that measures the diffusion of water in the white matter nerve tracts of the brain. Now the scientists took monthly images of the brains of 27 people. Of those 27 people, 11 people were put on an intensive Modern Standard Chinese language course and what the researchers found was that the brains of the people learning the new language had changed over the 9 months of the course compared to the control group.
Hannah - What was so different about the brains of those on the language course compared to the others and why is it important?
David - The language learners showed changes in areas of the brain associated with language acquisition, as they had expected but they also found that areas of the frontal cortex, the area right at the front of the brain were changed. This finding really challenges the idea that the adult brain is not adaptable and shows that changes to the brain are important for acquiring new information in the form of learning a new language.
Hannah - Exciting results showing that at any age we can exercise our brains by picking up a new skill, like learning a new language, and this changes the connectivity of our brains. That last paper was published by Chlegel and collegues in Journal of Cognitive Neuroscience.
Chlegel et al. (2012) White matter structure changes as adults learn a second language. Journal of Cognitive Neuroscience, 24 (8) pp1664-1670.
That was David Weston from Cambridge University with his favourite papers from the month.

20:08 - Neuroscience News Flash
Neuroscience News Flash
Are you Gleefully Gargantuan?
If so, it may be in your genes. The stereotype of rotund, jolly people full of mirth may have biological rational!
Researchers at McMaster University analysed 17,200 DNA samples from people in 21 countries. They found a gene called FTO that is associated with a significant eight per cent reduction in the risk of depression. This gene is also linked with obesity. 
So instead of trying to convert addicts by highlighting the dangers of drugs, due to their brain biology it might be better to emphasie the benefits of staying clean.
Neuroimaging study: Negative messages less effective on those who are substance dependent DOI: 10.1037/a0030633
Unraveling what it means to be human
Published in PLoS Biology, short DNA strands, previously thought to be 'junk DNA' may be key to understanding how human evolved their higher cognitive functions, like reasoning, flexibility in thinking and planning. It may also explain why human specific brain diseases like autism and alzheimers, appeared according to researchers from Mount Sinai School of Medicine,
 Hundreds of regions throughout the human genome show different 3D helical looping structure in the DNA of nerve cells in the prefrontal cortex,, compared to non-human primates. These regions do not code for proteins, which is why they were thought to be junk DNA, but instead determine how the DNA helix packages up intro a loop structure, and this may affect how other genes are regulated and expressed, plu play a critical role for human brain development.
Hundreds of regions throughout the human genome show different 3D helical looping structure in the DNA of nerve cells in the prefrontal cortex,, compared to non-human primates. These regions do not code for proteins, which is why they were thought to be junk DNA, but instead determine how the DNA helix packages up intro a loop structure, and this may affect how other genes are regulated and expressed, plu play a critical role for human brain development.
Human-Specific Histone Methylation Signatures at Transcription Start Sites in Prefrontal Neurons. doi:10.1371/journal.pbio.1001427
Boosting brain power with a diabetic drug already on the market
An FDA-approved drug initially used to treat insulin resistance in diabetics could be used to treat cognition in Alzheimer's disease, according to a multi-disciplinary study by researchers at University of Texas Medical Branch.
Published in Journal of Neuroscience Professor Larry Denner and colleges found the anti-insulin-resistance drug rosiglitazone also enhances learning and memory by reducing extracellular signal-regulated kinase (ERK), a protein involved in communication between nerve cells. Well, that's according to a study in mice anyway.
Cognitive Enhancement with Rosiglitazone Links the Hippocampal PPARγ and ERK MAPK Signaling Pathways. doi:10.1523/JNEUROSCI.2153-12.2012

Genes for intelligence?
Dr John Rogers, Cambridge University, answered this question...
First of all, it’s not just genes that affect intelligence. It’s strongly affected by environment as well as by genetics, and the two of them interact. And the stimulating environment in infancy is certainly important in influencing intelligence. But there do appear to be genes that determine intelligence, but searches for specific ones have not yet come up with very much.
In fact only recently, the first such gene was identified and it just has a small effect on IQ. If you have a particular version of this gene, it increases IQ by about 1.3 points which really isn’t very much. And this gene is a gene that’s generally in the nucleus to operate on expression of other genes and it seems to affect the size of the brain. So that may be why it’s affecting IQ.
Otherwise, we might expect there’ll be other such genes which contribute in a rather general way to brain development or to brain function, and there may again be some variance of them which allow for more effect to development to the circuits which integrates and interpret experience within the brain.
In addition to general intelligence as it were, there will also be genes that contribute to specific learning disabilities and there's been some progress in finding some of those recently, and there are some genes which seem to influence the chance of developing dyslexia and also other psychological conditions such as autism.
There are genes that influence the chances of developing those and those tend to be rather rare variance of genes which affects just a few people, but seem to predispose to those conditions in those people.

Genes just for the brain?
Dr John Rogers, from Cambridge University, answered this question...
Well, yes, there are a lot of genes expressed in the brain. Most of the genes are expressed in the brain and there is a lot of overlap between the expression there and elsewhere in the body.
That’s largely because the cells in the brain all need the same as it were housekeeping functions that other types of cells do, and there are thousands of genes expressed for that purpose throughout the body.
And also, in the development of the brain, many of the signals that are used are the same as in developing other organs of the body. There are genetic control systems that are used for many different purposes in different organs. One reason why the brain has so many genes expressed is, it has so many different types of nerve cells and so, most of these genetic control systems are used somewhere in the brain.
What is unique about the nervous system is the collection of ion channels and neurotransmitters which allow nerve cells to transmit signals and to receive signals. And the genes for these account for many of the genes that are specifically expressed in the nervous system.
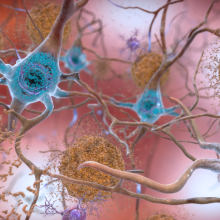
Is Alzheimer's genetic?
Dr John Rogers, Cambridge University answered this question...
Well yes, there is some pathology around blood vessels in Alzheimer's disease. The main pathology in the brain is that there are abnormal proteins produced and deposited throughout the brain, but one of those is particularly deposited around blood vessels. We don’t yet know whether that really makes significant contribution to the symptoms of Alzheimer's disease.
Regarding the genetic control of it, yes, there is a gene which has significant influence on the incidence of Alzheimer's. it’s called ApoE and people who have a particular version of this, an allele called ApoE4 are several times more likely to develop Alzheimer's disease than people with other versions of the gene.
However, I have to say, at present, it doesn’t seem worth testing for this because there's nothing we can do about it, but it is one more reason why we should generally keep a healthy diet and a healthy lifestyle because the main thing that ApoE does is to transport cholesterol into the brain.
And there are some evidence that high cholesterol made from Alzheimer's disease as well as other ills that they affect us in our older years.
There are many projects trying to use this kind of research to develop cures or prevention for Alzheimer's disease and some of these are in clinical trials, but nothing has been very successful as yet.
So at the present, the best advice one can give is to keep intellectually active because it’s known that people who are more intellectually active are less likely to develop Alzheimer's disease and to keep healthy lifestyles, keep physically active, and to try and keep one’s cholesterol low.

28:03 - What keeps a Professor up at night?
What keeps a Professor up at night?
with Barbara Sahakian, University of Cambridge
I find out what areas of neuroscience are keeping a professor excited and up at night…
Barbara - I'm Barbara Sahakian. I'm Professor of Clinical Neuropsychology at the University of Cambridge.
Well, there's many exciting things about the brain, but I suppose two areas that really excite me is the fact that learning is so fast that children especially are just programmed to learn and pick up everything and imitate, and I find that really exciting that the brain is just so essentially programmed to learn new things about the environment and how to interact with it.
The second thing that I'm very excited about is really resilience in terms of brain function because we go through life and many of us have very unfortunate experiences from time to time, and there are many people who experience really horrific environmental circumstances and yet, we can frequently overcome that.
So, the emotional brain can be quite resilient in many ways and I find that remarkable and I think we need to understand more about resilience, and how we overcome these things so that people who end up unfortunately with post-traumatic stress disorder, we’re able to help them and we’re able to instil resilience in young people.
Hannah - That was Professor Barbara Sahakian from Cambridge University.
Related Content
- Previous Cancer genetics - When good cells go bad
- Next Dealing With Debris










Comments
Add a comment