This month - we’re riffing around the concept of “gut feelings”. In a digestive sense, an emotional sense, and asking whether these concepts overlap at all...
In this episode

01:10 - Understanding intuition
Understanding intuition
Valerie van Mulukom, Coventry University
We've probably all had one, but what do we mean by "gut feelings" in an intuitive sense? What is intuition, and why do we have it? Katie Haylor firstly asked the Naked Scientists office for their experiences, and then she quizzed Valerie van Mulukom from Coventry University...
Nadeem - If I'm driving to work and I think there's gonna be traffic in one direction and not traffic in another direction, I'll find that my gut feeling, it’ll tell me to go exactly the opposite direction and I'll go with that and it'll be correct. And I think my gut is picking up on things subconsciously.
Katie - Have you ever listened to your gut to your detriment?
Nadeem - Yeah, sure, especially as a teenager.
Katie - I love how you’re not gonna elaborate!
Amalia - I mainly rely quite a lot on my gut feeling when it comes to determining whether a situation is safe, as a woman. It happens with people, when it feels a bit aggressive or just unpredictable, then I think that's when my gut says ‘oh, this might be dangerous, you don't know how this will go’, so I go away.
Phil - I associate gut feelings with anxiety. Because that's where I think at least for me anxiety manifests butterflies in your stomach contraction, tightening, feeling like a little nauseous [sic].
Adam - So my biggest going-with-my-gut moment was when I proposed.
Phil - That's a good one.
Adam - So I had this big intricate proposal planned and then that little voice of my gut went ‘you could just do it now. You know, you could just propose tonight, just do it’. And there was about 15 minutes where my wife thought there was something desperately wrong with me, because she could see this internal struggle playing out on my face. But eventually the gut feeling won, I ran home, just grabbed the ring and went ‘do you wanna get married?’.
Katie - I assume she said "yes"?
Adam - Yes. Thankfully she did, in the longest three seconds of my entire life between asking and her saying yes..
Adam - Well as you can see, going with your gut has been pretty beneficial from where I'm standing, but thanks as well to Nadeem, Amalia and Phil. Well, what exactly are the so-called “gut feelings” they were talking about? Katie called up neuroscientist Valerie Van Mulukom, from Coventry University, to find out. Valerie told Katie that as the brain makes sense of the world, actually a lot of processing happens out of our conscious awareness and only a relatively small amount makes its way into our consciousness.
Valerie - If something really important happens but it doesn't reach our conscious awareness, this gives you sort of emotional response or a feeling of salience, something that we have to pay attention to. That is then translated as a gut feeling in our conscious awareness. So, it's almost as if some of this automatic subconscious processing that is happening just manages to catch your attention in your conscious awareness, if that makes sense.
Katie - There seems to be a bit of a spooky, mystical, uncanny, element to gut feelings. Do we know much about what these signals actually are?
Valerie - I think that the mystic aspect of intuition is that we don't know where it comes from. Normally we feel like we're in control, and when we suddenly are either reminded or we learn that sometimes, well actually lots of the processing of the brain happens not in our conscious awareness, that is a bit of an eerie feeling, it feels like we're not that much in control.
Katie - How much do we know about the neuroscience of gut feelings? Has anyone stuck people in a brain scanner and encouraged them to have gut feelings to see what's actually happening?
Valerie - Not that I'm aware of, because it's kind of hard to induce real strong gut feelings. They just come to us when we don't expect them, right. But what they have done is skin conductance testing. They put sensors on the palm of your hand and they test how much you're sweating, and they have this card game. So participants came into a lab, they had to turn over cards from one stack and they could switch between them. If you got a certain type of card, then you got a reward. And if you didn't get that card you could get punished. And the idea was to get as much money as possible, and then they would get the money after the end of the experiment. It was rigged, obviously. So there were stacks that progressively got worse, and there were stacks that progressively got better. And before people were conscious of it, their hands would start sweating as they would reach for the bad stack. So, basically your brain already knew that this was the bad stack but it hasn't quite reached your conscious awareness. So I think that might be the closest to what we've got so far, because it's really hard to measure intuition considering that it isn't in our conscious awareness.
Katie - People often say "you need to listen to your gut. What is your gut telling you if you're in a difficult sort of decision-making scenario?". I find this really difficult to actually know what my "gut" is saying. Do you have any tips to help people actually hone in and listen?
Valerie - Maybe the simplest way is to not immediately dismiss it. There's been a study that I know of where they simply told people to keep a journal every time during the week where their intuition led to a good outcome. And just doing this exercise helped them tune into their intuition. So, just paying attention. But then, I don't want to stress this too much because you can also have bad intuition. I wouldn't encourage anyone to blindly follow their intuition. Our brain is very biased. The brain has evolved to have lots of shortcuts, right. We have biases like cognitive dissonance bias, so if we read something that we agree with we're more likely to pick it up and we tend to ignore things that we don't agree with. This is why it is important to not just rely on your gut feelings and intuition, because it is an evolutionarily old system, it’s biased. This is why we need critical thinking as well and science.
Katie - Can you tell us a little bit about the comparison with analytical thinking?
Valerie - It's not "either or". So, there is a lot of research in psychology where they try to say whether people are intuitive thinkers or analytical or rational thinkers, and I think that's just a little bit wrong because we definitely all use both. Even if we don't know it. We need both, right? But I have a feeling that with these past century or so, maybe even since the Enlightenment, we're starting to think of emotions as these fallible things that we should do away with, as I myself used to think, and I think that is wrong too. So if we could just see emotions for what they are - which is useful ways of your body telling you to pay attention to something - rather than thinking of whimsical things that should be ignored. Yes. Pay attention to your gut feelings, but don't just jump into them without critical thinking.
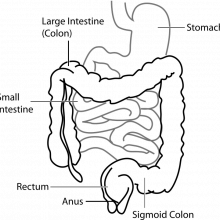
Stomach sensations
Jeremy Woodward, Cambridge University Hospitals
To explain what the gut can feel in a literal sense, Katie Haylor met up with consultant gastroenterologist Jeremy Woodward from Cambridge University Hospitals...
Jeremy - We talk about the gastrointestinal tract as being from the mouth to the anus. There's a lot of confusing terminology with this. People talk about the tummy when they mean the abdomen, short for stomach and the stomach is a key part of the gastrointestinal tract. But when you follow it down from the mouth you have a muscular tube, the gullet or oesophagus, which then leads into the stomach and the stomach then leads into the small intestine and then into the colon and then out into the toilet.
Katie - I've heard that the gut actually has its own brain.
Jeremy - Well it's not a brain like our head brain, if you like. We call it the gut brain because there are so many nerves present in the gut, about half a billion nerve cells which is the same as you'd find in the spinal cord. But the other reason which we talk about having a gut-brain, is actually the fact that it can function almost autonomously. We know that because if we transplant intestine, which we do here in this hospital, they actually function perfectly well when we move the gut into another person.
Katie - Provocative question - what makes the gut so special that it deserves its own brain?
Jeremy - Well one could turn that question around and say why do we have a head brain to be honest! The gut is the oldest organ in the body and the nervous system evolved around the gut in order to provide ways of helping it work, but also helping to fill it, in other words to get food into it. So when you look through evolution, all of the things that are developed on the outside of animals are really ways of actually getting food into the gut. And to a certain extent the head, where sensory organs are concentrated. The head brain if you like, for thinking and planning, to a large extent, when it comes down to the bottom line, it's about how we get food and how we fill the gut. In many ways, if you look at the evolutionary story, the gut brain came first and the head brain second as a result of basically the evolution of nerves in the gut.
Katie - Not that you're biased or anything.
Jeremy - Of course not.
Katie - Can you tell us a bit about how it's displayed in the gut?
Jeremy - Okay so it doesn't look anything like a brain. What it is, is just a network of nerve cells, long processes spreading out from the nerve cell body which are like the electric wiring if you like, that are able to transmit messages from one point to another. And in the gut that they're thinly spread between the layers of the muscle and also under the surface lining of the gut, the mucosa.
Katie - Can you tell us a little bit about how food actually progresses down the gut?
Jeremy - The gut works by a process called peristalsis and most people have heard of this. It’s a very clever mechanism where food goes in one direction usually - the gut senses a lump, it relaxes below it, and contracts above it and that way we get a moving wave of contraction moving down the gut. It's extraordinary to watch - it's the most the most beautiful thing, and there are even videos of people standing on their heads and you can see the peristalsis moving against gravity.
Katie - I was going to actually ask you what would happen if I stood on my head and ate my breakfast? I imagine you would not be endorsing that as someone who has to look after guts! But is this perhaps an example of what you were saying about the gut brain or enteric nervous system being able to work by itself?
Jeremy - So the gut actually is able to control its own movement entirely through the enteric nervous system. It's got a network of nerves responsible for contracting and relaxing below, and moving this wave down the gut and that's entirely independent of any nerves coming from outside and you wouldn't be aware of it. Interestingly, it is the oesophagus, the gullet, where the brain has actually in humans taken over some of the control of the muscle contraction. We don't see that in other animals. It seems to be specific to more recently evolved mammals, but further down in the stomach and the intestine this is all totally controlled within the nerves of the gut itself.
Katie - Can you tell me a bit about what the gut can feel and by that I mean sense or detect?
Jeremy - Well you name it, effectively. There's no end to what the gut can do. It's an extraordinary organ. I've already mentioned that it can sense the presence of a lump or a bolus of food, but the lining of the gut can actually even taste specific chemicals. So if there's a lot of fat in the meal it will affect the way the gut works into more of a churning motion. Fat is also detected by cells that secrete hormones that make us release bile to help us to absorb it. And this is all regulated within the gut itself.
But the gut can also sense noxious things. The feeling of nausea and sickness when we've eaten something we shouldn't. The Yew tree berry for instance which looks very attractive but is highly toxic. The gut will be able to sense that and it will automatically make us vomit. The gut can recognise the difference between particles and fluid, that's part of the way that peristalsis works. It can sense the presence of bacteria and even specific bacteria. It's capable of responding to stretch and even probably to be able to tell apart the consistencies of different foods going through it.
Katie - I'm glad I can respond to stretch, because isn't that how I managed to eat my Christmas dinner or a couple of Christmas dinners, right?
Jeremy - Well effectively, yes.
Katie - I'm curious. As a gut expert, what do you think looking forward are the more interesting questions to ask around how the gut is controlled or innervated?
Jeremy - For me as a clinician, understanding a lot more about the afferent nerves, these sensory nerves from the gut to come back to the brain, and what fires them. How the gut is sensitive to things - I have to deal a lot with people who have a lot of sensations from the gut, pain and nausea. These sensations can be extremely unpleasant and we as yet are very limited in our ability to understand the mechanisms for how they are occurring in these patients but also how to make them better.
14:41 - Hacking the gut-brain hotline
Hacking the gut-brain hotline
Katerina Johnson, Oxford University
How is the "gut brain" connected to the "head brain"? And what have bacteria got to do with it? Katie Haylor asked Oxford University neuroscientist Katerina Johnson...
Katerina - We think that a strong link between our gut and our brain evolved because, ultimately, a lot of information about our environment comes from our gut. So if we eat something dodgy or something, our brain really needs to know about it and needs to respond to keep us safe. Our gut can affect our brain, but also how we feel and our emotional state can in turn affect our gut.
Adam - That's Oxford University neuroscientist Katerina Johnson.
Katerina - And one of the ways that this happens is that there's a vagus nerve, so this is a major nerve that travels between our gut and our brain. And interestingly actually 90 percent of nerve fibres in the vagus nerve communicate in the direction from our gut to our brain. And so this really suggests that our brain is actually more a receiver of information in terms of gut-brain communication.
Adam - One aspect of the gut not yet mentioned is the incredible abundance and diversity of microorganisms surviving and thriving down there in your intestines. They do vital jobs for us in exchange for taking up residence inside us, like helping to break down our food or to produce vitamins for us.
Katerina is interested in whether the different types of gut microbes can tap into this communication to affect the brain, and maybe even our mood. So how exactly do these microbes hack the gut-brain hotline? Katie asked Katerina.
Katerina - One of the messages is by neurotransmitters travelling along the vagus nerve. Also other messages as well. So for example we think that our immune system plays an important role, so the types of bacteria living in our got are very important for regulating our immune response and how we deal with infection. And it's good to have an active immune response. But if we have an overactive immune response, this in turn has been linked to low mood and depression.
So one of the interesting things at the moment we're looking into is that our gut bacteria can actually produce neurotransmitters - a chemical used to send signals between nerves. And we typically think of neurotransmitters as being in our brain, but really that's kind of a misnomer. Neurotransmitters are more just chemicals that help cells communicate with each other. So things like serotonin, dopamine, histamine, acetylcholine. And so one of the things we're interested in now is understanding whether these neurotransmitters produced in our gut can affect our brain. It may be that these neurotransmitters can trigger the vagus nerve and send signals to our brain that way, or perhaps the neurotransmitters or their precursors can travel through the blood and affect our brain.
Katie - It seems to be that there are multiple lines of communication. There's this vagus nerve so electrical impulses being fired up from the gut to the brain, but also there's the bloodstream, right, where perhaps particular metabolites are going up to the brain. Have I got that right?
Katerina - Yes. So for example in terms of metabolites, we know our gut bacteria produce fatty acids when they break down our food, and in particular sht chain fatty acids. These can actually travel through the blood and into our brain directly. But bacteria produce such a wide range of chemicals that we're only really starting to understand. And a lot of these chemicals may be able to influence our immune system, you know perhaps through our bloodstream. And, like I said, the neurotransmitters they produce, they might just stay locally in the gut. But that doesn't mean that they can't affect the brain. Because they may well trigger the vagus nerve. And in fact there's some new research at the moment looking at whether electrical stimulation of the vagus nerve may help with things like depression. That does suggest that maybe how much our vagus nerve is stimulated and in what way may affect how we feel and our mood.
Katie - It’s so interesting you said that because I actually quizzed the Naked Scientists office about occasions where they may have been “listening to their gut” or gone with a “gut feeling”. I mean in an emotional or psychological sense. But actually one person said they really associate the phrase gut feelings with anxiety. So how can this gut-brain connection have any impact on our mood as you say? What's going on?
Katerina - A lot of the studies at the moment are in animals because it's at early stages, but if you use a probiotic - so this is a type of live bacteria, in this case lactobacillus - in animals it was actually found to reduce anxiety and the depressive like behaviours that the animals showed. But this was only the case when the vagus nerve wasn't damaged. We know that this probiotic actually seems to increase the firing rate of the vagus nerve.
There's a big link between anxiety and stress and how we feel in our gut. Most notably for example irritable bowel syndrome where people often suffer from gut conditions and kind of psychological symptoms at the same time. A study found that in two thirds of cases, people suffered from gut conditions before the onset of things like stress and anxiety, and in the other one third of cases they suffered from stress and anxiety prior to the onset of gut conditions. So this really underpins the fact that this is a 2-way communication between our gut and our brain.
Katie - Does that hint in any way as to the cause of someone's anxiety? Are we saying that what's going on in your gut may cause you to feel anxious in your brain?
Katerina - It's a bit tricky really because there's so many factors that might affect how we feel and our mood and our anxiety. And research in this whole field of the microbiome at the moment is starting to suggest that the types of bacteria in our gut may influence how we feel, but we don't know at the moment how strong this is. So do they have a really big impact on our brain? Or is it really just like one tiny piece of the puzzle?
But if you're stressed or you're worried about something, you often feel it in your gut. And if you’re stressed, particularly over long periods of time. There's some studies that suggest that stress can deplete the abundance of beneficial gut bacteria and actually it can affect our whole kind of gut environment and how a gut works in terms of things also like mucus secretion and are the motility of our gut.
So, yeah, it's an interesting question trying to understand how much our gut affects our brain. And there was one interesting study that found that people with a lower abundance of a certain type of bacteria, that we know is a prolific producer of the neurotransmitter GABA, actually also tended to show stronger kind of brain signatures of depression when their brains were scanned. And so this is just one study that we need to look more into, but it does suggest that maybe the types of chemicals and neurotransmitters produced by bacteria in our gut might be one factor influencing how we feel.
Katie - One of the functions that the gut has is to digest our food. So how does what we eat relate to this connection between the gut, and the microbes, and the brain?
Katerina - There's a lot of interest at the moment trying to understand whether what we eat has a big effect on the types of bacteria that live in our gut. So we know that, for example, people that eat more fruit and vegetables, they have a high abundance of gut bacteria that like to digest fibre. There have been some initial studies, for example, there was one looking at a particular type of fibre known as prebiotic fibre. And this is actually known to promote the growth of bacteria we tend to associate with good health. So bifidobacterium and lactobacillus that also have anti-inflammatory properties. And they actually found that after a few weeks, people that had been consuming this prebiotic fibre tended to have lower levels of cortisol, so their bodies’ stress response had reduced. So it does suggest that maybe changing the types of bacteria in our gut may influence our physiology and how we feel. And this prebiotic fibre is found in foods like banana, chicory, onion, garlic, pulses and grains, but really in terms of understanding how specific elements of our diet affect our gut, it's still in its infancy.
Katie - If there are bacteria that thrive on food that we may consider to be more healthy, like high in fibre for instance, I imagine there are gut bacteria that thrive on things you may consider to be less healthy. Does this have any relation to our (well, my) desire to consume foods which are high in fat and sugar?
Katerina - Yes. So when gut bacteria break down particular types of food, they can release metabolites that then potentially can travel to the brain and affect our feelings of appetite. But we're not sure at the moment, we can't say that, our gut bacteria make us crave a certain type of food because they want it. That's probably unlikely because it's very costly for bacteria to produce a signaling chemical and it would probably be out competed because our gut microbiomes are so diverse. But our gut bacteria are really important for affecting things like how hungry or full we feel. But yeah it's still kind of in its infancy at the moment.
23:59 - Microbes and neurological health
Microbes and neurological health
Simon Carding, UEA, Quadrum Institute
Could there be a link between the health of your gut microbiome and your neurological health? Phil Sansom spoke to Simon Carding from University of East Anglia and the Quadrum Institute...
Simon - It's quite clear from studies looking at dementia patients, in particular Parkinson's Disease, that G.I. symptoms, that's gut disorders, seem to precede the onset of the classical Parkinson's symptoms. Several research groups have shown using animal models of Parkinson's disease, that microbes might be playing a causative role in Parkinson's disease, and again, it’s through the production of things that interfere with the communication, or they actually make the misfolded proteins that cause some of the defects in the brains of dementia patients, they can actually make them themselves, to exacerbate the disease process.
Phil - Now this system, this gut-microbe-to-brain axis, how do you actually investigate and do science on it?
Simon - There are two principal ways; one is in laboratories, in culture dishes, where we can isolate cells of particular interest. So for example, cells that make up the blood-brain-barrier, or cells that line the gut. Using these culture based systems we can look at what impact particular gut microbes, or their products, have on these cells. Does it change their pattern of behaviour, does it change the factors they produce, the hormones, or the neurotransmitters. And then for more directly relevant studies we’d move into animal models. So the mouse is used as a classical model for this. But what we really need is more human based studies to look at particularly the role the gut microbes might play in cognitive failure and dementia development.
Phil - What are your main question, or questions specifically?
Simon - Well we'd really like to know; are the changes in gut microbe populations seen in dementia patients a cause of the disease process, or are they a consequence or an effect of the disease. So to do this we have to do longitudinal studies, that's looking at people over a significant period of time, trying to identify what occurs first, and what sequence of events occurs in these patients that ultimately leads to declining cognitive function, and develop dementia.
So we have one such study underway at the moment. It’s called The Motion Study, in which we're looking at individuals 60 years of age and older. We assess their cognitive function and according to the performance of those tests we categorise individuals as low, medium, or high risk for developing dementia. And we'll follow those over a period, initially for four years, but hopefully longer, where we'll perform tests on looking at their gut microbe populations that were present in the stool samples, looking for changes in there, do they occur prior to significant change their cognitive function. But we're also looking at the structure of the brain, so we do MRI scans.
And interestingly, we're also looking at the eye, because the eyes not only the window to the brain but it's one of the fastest aging organs in the body. So again we're looking for: What are the first indicative changes in the eye, the brain, the gut, that give a signature for this patient is starting to develop dementia. And of course if we can identify these key tipping points if you like, then we can identify means of which we can hopefully intervene.
Phil - And when you're looking at the microbiome of these people, do people developing or who have Parkinson's have noticeably different microbiomes, or does everyone just have a very different pattern?
Simon - Everybody's microbiome is unique, it's like your microbial fingerprint if you like, but everybody has a core population of microbes which are important, particularly for food digestion. But what's been shown in Parkinson's patients, and Alzheimer's patients as well, is they have distinctive changes in their gut microbe populations.
Phil - So when you replicate those in your petri dishes and in your mice, what changes do you notice?
Simon - Of course, it's very difficult to recapitulate in a Petri dish or tissue culture plate the complexity of the gut and the complexity of the microbial constituents. We're looking at only a representation of what's present, but some of the changes we're seeing are these changes in the gut microbe populations that is associated with an increased leakiness of the gut, called leaky gut syndrome, and a leaky gut would allow microbes and their products more easily, or more readily accessible to the bloodstream. And again this could exacerbate certain diseases, and the classical example for this is inflammatory bowel disease. So there may be a common link to some other quite serious diseases. But in this case it would have an impact on the brain for dementia patients.
Phil - Does it cause dementia?
Simon - Well certainly the animal studies are pointing a strong finger of suspicion at gut microbes being part of the cause of dementia. So these transplant studies that had been done in mice had quite striking effects, and make the disease clearly much worse than if normal microbes from a healthy individual are transferred into those mice.
So there is if you like, a smoking gun for gut microbes right now, and you know, the evidence is quite compelling, but we really need to substantiate that and to validate the studies, by looking more closely in humans, and particularly individuals prior to the onset of clinical symptoms. If they are really a major cause of disease then there's means by which we can manipulate gut microbes to alleviate or maybe even stop the symptoms developing. I mean the classic one would be probiotics for example, or prebiotics, or even faecal microbiota transplantation, the wholesale replacement of somebody's gut microbe population with one that's a more healthy one for example. So there are quite a few interesting possible interventions if we do in fact find gut microbes are a cause of this disease.
Phil - And lastly, in this show we are talking about quote unquote gut feelings.
Simon - Yes yes.
Phil - What do you think about how gut microbes can change the way that you feel?
Simon - Yes it's very interesting. So I mean emotions play a critical role in the ability to make fast and rational decisions. These emotions are generated on physiological changes to stimuli, and this could be manifest as muscle tone, heart rate, hormone activity, and the brain transforms these emotions in an individual so it can recall if that stimulus comes again, a very rapid response which would be the emotional response.
Some of these emotions could well originate from the gut, and a physician called Emeran Mayer proposed in 2016, I believe, that from birth, gut microbe activity in response to certain stimuli produces physiological changes that are relayed to the brain. So this stimuli could be food or drugs and this could result in changes that relate to pleasure and consumption, or pain and avoidance. So in that context you can imagine that in response to certain stresses, the gut instincts, that gut feeling takes over as an immediate fast response without the brain really getting too involved in it, and that's because it's learned from previous experience.
Related Content
- Previous Simulator Special 2
- Next From pilgrimage to package tour










Comments
Add a comment