Reporting from New Zealand on how a bank of frozen human brains is acting as a reference library, how a Hindu resolves religious and scientific beliefs and scientists creating human brain circuits in a dish in order to piece together the jigsaw of Huntington's Disease.
In this episode

00:00 - Living with Huntington's Disease
Living with Huntington's Disease
with Richard Price
Huntington's disease or HD affects around 1 in every 30,000 people worldwide. It's a hereditary condition, so can be passed from mother or father, down generations. To find out more about this disease, I firstly met Richard Price, whose Heather started to exhibit symptoms 8 years ago.
Richard - She started off with not being able to handle stress, even the smallest of the issues can make her quite upset. Also, in terms of depression, she suffered from that a little as well. My wife Heather is now in residential care. She has what has turned out to be a very aggressive form of Huntington's that has affected not only her cognitive side and mobility, but also her mental state. So, from that perspective, it has changed quite a lot. She went into residential care about 2 years ago. But just in the last 6 months, she's been declining in terms of her mental state. It was really just trying to get treatments. So, we're trialling new treatments to try and make her just more comfortable and less upset, and less unsettled than she currently is. Where she currently resides there as - between 4 and 6 people with Huntington's and they all are so different. You've got one person that you just wouldn't realise. In fact, the GP probably won't realise that they have HD. You've got other people that have the movement issues and you've got people with the emotional and the cognitive issues. Unfortunately, Heather has had all three. Yeah, it's been real tough. Of course, Heather, having watched her mother go through what she's going through, it's been really quite tough on her.
She's 43 now. She was tested when she was 18. At that stage, they'd only  just discovered how to actually discover the gene and test for it. Heather is a very positive and proactive person, so she wanted to know whether she was going to have the symptoms later on in life. So, it was quite tough and she got through it. In fact, that helped her knowing rather than not knowing.
just discovered how to actually discover the gene and test for it. Heather is a very positive and proactive person, so she wanted to know whether she was going to have the symptoms later on in life. So, it was quite tough and she got through it. In fact, that helped her knowing rather than not knowing.
Hannah - Did she ever mention that as a result of having this test and knowing that she was going to develop Huntington's down the line, do you think she led her life a little bit differently because of that?
Richard - Differently. In fact, that was her purpose, everything from deciding to get a diploma rather than a degree, rather than going to a university and really just getting into the workforce and really just building up a nest egg for when the symptoms really started to appear. She was able to manage that, understand that and then make some decisions around it. So, she always had planned on travelling and for a Canadian from the East Coast, that's not as common as we have in New Zealand. She sold the house and went travelling when I met up with her in London.
Hannah - Do you have children with Heather?
Richard - No, that was another sort of decision that she made quite early on because it seems her family may be more prone to passing it down the line. Her brother has it as well. He does have a son. So, yeah, I mean, Heather had a lot of time to sort of process and accept that. We're both at the same mind, so we had dogs instead of children.
Hannah - Thanks to Richard Price who's wife Heather has Huntington's disease.

13:26 - What do human brains tell us?
What do human brains tell us?
with Dr Maurice Curtis, Auckland University
Now, over to Dr. Maurice Curtis, Deputy Director of this brain bank on some of the results from the samples to date.
Maurice - So, one of the things I've been interested in are the stem cells in the  brain. These are cells that have the capacity to divide and become any other cell type in the whole body actually. but in this case in the brain, they would normally go on to become either glial cells which are the supporting cells of the nervous system or neurons which are kind of the active unit of the brain. These stem cells we'd would always thought were very important during the development of the brain. In fact, it's those stem cells that produce about 160 billion neurons in the course of about 4 or 5 weeks when we are developing. But once your born, the thought has always been that you don't have any more stem cells in the brain.
brain. These are cells that have the capacity to divide and become any other cell type in the whole body actually. but in this case in the brain, they would normally go on to become either glial cells which are the supporting cells of the nervous system or neurons which are kind of the active unit of the brain. These stem cells we'd would always thought were very important during the development of the brain. In fact, it's those stem cells that produce about 160 billion neurons in the course of about 4 or 5 weeks when we are developing. But once your born, the thought has always been that you don't have any more stem cells in the brain.
Hannah - So, the number of cells in your brain that you are born with, people used to think that that was it for life. So, if you have any trauma or if you do any damage to your brain then you can't replace those cells. That was the traditional hypothesis.
Maurice - That's right. That's what I was taught when I first started at the university. Only a few years later and I can still remember where I was standing when I read the paper in 1998 which indicated a paper that showed unequivocally that the brain produces new brain cells. That was staggering to me and I thought I have to know more about this. And so, we were actually interested in the Huntington's disease brain for the reason that the area that the stem cells reside is exactly next door right - they're neighbours - right next door to the area that actually degenerates in Huntington's disease. So, you've got this interesting situation where in Huntington's disease, the regenerative area and the degenerative area are neighbours. They're right next to each other. So, the areas that we're referring to when we say the stem cell area is an area called the subventricular zone that sits right next to the lateral ventricle in the brain that's the fluid-filled space in the middle of the brain. Just next to the subventricular zone is the caudate nucleus. The caudate nucleus is the area that degenerates in Huntington's disease and it normally is involved with mood and movement and hints people with Huntington's disease of problems with movement and also, they can have mood disturbances. And so, we were interested to see whether or not the area that is responsible for regenerating the brain at least during development was upregulated or whether more stem cells were born in that area, in response to the area next door, the caudate nucleus degenerating. And so, we used some special stains and what we found was that the more degeneration that was occurring in the caudate nucleus, the more regenerating cells or the more stem cells we found in the area next door the subventricular zone.
 Hannah - So, it's kind of almost the opposite of what you might expect.
Hannah - So, it's kind of almost the opposite of what you might expect.
Maurice - Yeah, that right. So, you might naturally think it might go the other way, but if you think about how skin repairs itself, when you cut yourself, you'd think, well, that's going to kill off the cells. But actually, what it does is it gets the stem cells engaged and they come along and they appear and within a few weeks, you're left with just a small scar, but not an open wound anymore. Of course, the brain isn't nearly as able to cope with insults, but the process is similar just on a smaller scale.
Hannah - So, what's going wrong with the patients with Huntington's disease then? So, they're having more degeneration in this particular area of the brain, but they're trying to compensate with this regeneration. But why isn't it happening properly so that those regenerating cells are properly getting down into that region, making the circuits and replacing those lost cells?
Maurice - Yeah, so there's a couple of problems there I suppose that the brain has to overcome. Unlike skin which are relatively simple cells, the neurons are highly specialised, very, very specialised and they've actually done their job successfully for 40, 50, 60 years. Were then asking stem cells to come along and just replace these cells that have done their job well for a long time and asking these stem cells to find the right place to connect up with is actually quite a big ask. It's a case of too little too late. So, we don't really get the true regeneration that would be nice to be seen there.
Hannah - So, is there some genetic reason for why these new regenerating cells aren't recircuiting or getting into the circuit properly as well? Is that something to do with the genetics of Huntington's?
Maurice - We don't know that. We certainly don't have a lot of information about that. what we do know is that some of the abnormalities that occur in cells with Huntington's disease actually affects stem cells less. So for instance, the Huntington protein which abnormally accumulate in Huntington's disease, that normally is a real problem for neurons. It accumulates because the neurons are very old and they don't have such good ways of being able to get rid of those abnormal proteins, the Huntington. Stem cells, they actually don't accumulate the Huntington. Cells that are dividing don't seem to accumulate these abnormal proteins that occur later in life with diseases like Alzheimer's, Parkinson's and Huntington's. So, the stem cells seem to have a window of being immune to these problems and part of it is just the fact that they're regenerating.
Hannah - So this finding, will it lead to maybe a treatment where you can start using these stem cells which wont accumulate these misfolded or improper proteins and somehow make sure that they do make the proper connections and kind of get themselves in place in the circuit properly in order to help cure or treat Huntington's and other disorders as well like Alzheimer's?
Maurice - That's certainly always been the desire as to be able to get new cells and a cell replacement therapy essentially. What I guess we've learned from other cell replacement therapy approaches is that getting one group of cells that you put into the brain to connect up with the right target cells is actually quite tricky. It certainly has been done a lot in the past and the hope is that using endogenous stem cells, the brain can direct it themselves and we just help the brain out. So, that's certainly one of the goals. We want to know more about how is it that you actually get the brain cells to do what they would naturally do and connect up in the right places. But part of it is actually understanding what it is that drives a stem cell to make a projection to actually look for a place to connect up with elsewhere. And so, we're studying those features currently.
Hannah - Maurice Curtis on how a bank full of frozen human brains can tell us about Huntington's disease. If you would also like to donate your body and brain to research, further information and links are on our website. That's nakedscientists.com/neuroscience and have a look for the show called Naked in a brain bank.
20:38 - Creating human brain circuits
Creating human brain circuits
with Professor Mike Dragonow, Auckland University
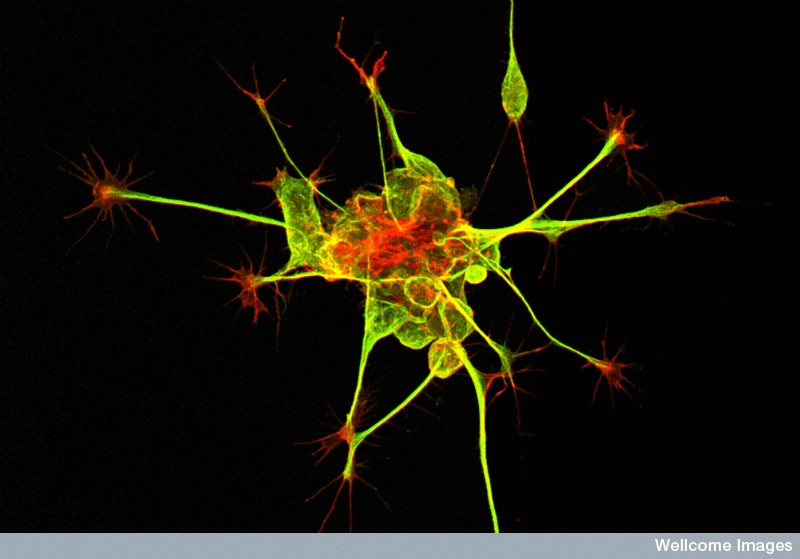
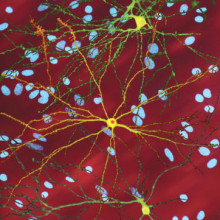
Professor Mike Dragonow, also based at Auckland University is able to culture these stem cells from the brain bank. As well as this, he gets brain tissue donated from epilepsy patients who've elected to have surgery to cut-out brain tissue to help control their seizures. He harvests these tissue and grows these cells in a Petri dish, forming a brain network. I started by asking him, how similar these cells in a dish are to a conscious, real living brain. Can you really compare the two?
Mike - Well, it's always a challenge actually because once you grow them in a dish, 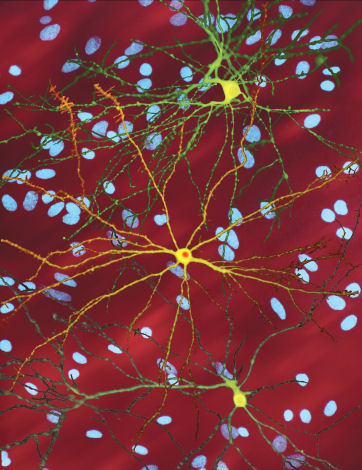 you already have a very much artificial environment. But what we can do is we can use markers for the different cell types that we know are present in the brain and see where those markers exist in the cells in the dishes, and they do. And so, what we're trying to do really is understand how does human brain cells function their basic biology because we can test that. so, we're looking at understanding how human brain cells that are involved in a number of neurological disorders, how they behave, their biochemistry. And also, we're testing compounds directly on those human brain cells. Now, one of the big problems in the neurosciences really is that compounds developed in model systems haven't actually translated to humans. So, you have medications that work wonderfully in transgenic models of Alzheimer's disease in mice for example that kill the mice with those of Alzheimer's and yet, so far at least, none of those compounds have worked effectively in humans with Alzheimer's. And the approach we're taking I suppose is to try and take a more direct approach if we can actually understand first the biology of the cells and secondly, use those cells to test drugs. The drugs that work on the human brain cells in the dish may - we don't know if they will, but they may be effective in real humans that are living. So, what we've been doing really is learning how to grow the cells, defining the different types of cells and some cells grow better than others - is that the dividing cell population that we do freeze down because they bulk up, it turns out that these dividing cells - we're not 100% sure. We're about 95% sure now through a number of different genetic techniques in fact sorting...
you already have a very much artificial environment. But what we can do is we can use markers for the different cell types that we know are present in the brain and see where those markers exist in the cells in the dishes, and they do. And so, what we're trying to do really is understand how does human brain cells function their basic biology because we can test that. so, we're looking at understanding how human brain cells that are involved in a number of neurological disorders, how they behave, their biochemistry. And also, we're testing compounds directly on those human brain cells. Now, one of the big problems in the neurosciences really is that compounds developed in model systems haven't actually translated to humans. So, you have medications that work wonderfully in transgenic models of Alzheimer's disease in mice for example that kill the mice with those of Alzheimer's and yet, so far at least, none of those compounds have worked effectively in humans with Alzheimer's. And the approach we're taking I suppose is to try and take a more direct approach if we can actually understand first the biology of the cells and secondly, use those cells to test drugs. The drugs that work on the human brain cells in the dish may - we don't know if they will, but they may be effective in real humans that are living. So, what we've been doing really is learning how to grow the cells, defining the different types of cells and some cells grow better than others - is that the dividing cell population that we do freeze down because they bulk up, it turns out that these dividing cells - we're not 100% sure. We're about 95% sure now through a number of different genetic techniques in fact sorting...
Hannah - Sorry, fac sorting. Is that fax as in like faxing something, f transfer of information there?
Mike - It's a sort of flow cytometry. It allows you to actually sort cells on the basis of certain markers on this surface. We use that to try and identify what sort of cells you have. Using these approaches, we think that pretty sure these cells that we're growing in bulk here are called brain pericytes. Now the pericyte actually is a very old cell, but very, very understudied, and under understood cell really because what it does, it actually lines blood vessels. In the brain actually, there's actually a large number of pericytes and one of their functions in the brain to line blood vessels is to maintain the blood-brain barrier. Now, this barrier is very important because molecules in the body and the blood, there are certain molecules you don't want to get into the brain. And so, the brain has this privilege, this blood-brain barrier, the pericytes maintain the barrier and we now know through work by a number of research around the world that the blood-brain barrier breaks down in a number of neurological disorders especially in Alzheimer's.
Hannah - So, these pericytes in this blood-brain barrier really stops any toxins entering the brain that might cause damage to the brain and therefore, cause any behavioural problems like seen in Alzheimer's or Huntington's for example.
Mike - That's right, yes and so, people think that once that barrier breaks down, toxins can get into the brain. They can actually add directly to the nerve cell degeneration but they can also activate immune cells in the brain to cause inflammation. We need to study more human versions of these inflammatory cells in the brain, the microglia and the astrocytes directly.
Hannah - Which is why it's so important to get these samples from the human brain bank tissue and also from the surgery.
Mike - It's amazing really and our work really is driven by the amazing generosity of the patients who are undergoing surgery and also the donations that people with fatal brain disorders give to the brain bank. It's incredible and their families. They really drive our work and they also motivate you as a scientist. When you're studying human brain cells, you're much more motivated to try and understand and provide some useful answers. and so, that's our approach really, by studying human brain cells by testing drugs directly on them. Our hope is to identify molecules that will work in humans to help reduce and stop the progression of some of these terrible disorders.
Hannah - So, a whole host of brain disorders show an altered immune system where the brain is effectively being attacked by its body's own defence system. Cases of Schizophrenia, Alzheimer's, and Huntington's all involve the brain being almost on fire with inflammation. And Mike is now working on trying to come up with molecules that will dampen down this heightened inflamed response and repair the brain and hope that this will lead to new treatments for patients.

25:44 - Mysteries of the Mind
Mysteries of the Mind
with Professor Richard Faull, Auckland University
How researching Huntington's Disease is also helping us to grasp the incredible scale of complexity of the human brain.
Next, I speak with Professor Richard Faull who set up this Brain Research Centre at Auckland University to find out how researching Huntington's disease is also helping us to grasp the incredible scale of complexity of the human brain.
Richard - So, Huntington's disease was certainly thought to be a simple disease because it was caused by one gene and why there has been so much attention on this gene scientifically and on this disease, was a simple idea. If we could solve this disease by working out what this one gene defect caused, then we could solve diseases like Alzheimer's, Parkinson's, and motor neuron disease which are multiple gene diseases. Well, it just so happens that we now know that this single-gene disease, Huntington's disease is a very complicated disease because it actually causes dysregulation and upset of at least a quarter of all the genes.
We have 45,000 genes in each cell and depending on what part of the brain it is, will upset different combinations of these other genes you see. That's why you get all the different symptoms. And so, genetics is a very complex science now. We thought it was a simple science when I was at school and that this gene would do just one thing. It doesn't. The gene makes a protein, that protein interacts with other genes, and causes them to change their function or change their pattern of protein production. So, there is a sort of an effect which spreads like wild fire in variable ways. And the variation is affected by the environment. And so, we know that people in different environments, even with the same gene will result in different patterns of brain degeneration symptoms. And Huntington's disease has taught us the fundamental principles that the human brain is more complex than what we ever, ever imagined.
We can't explain a human thought. We can't explain why the sudden burst of genius, and we're beginning to unravel it. But it's almost as if we climb to the top of Mt. Everest, thinking we're going to solve this disease and then we see all the Himalayas before us which are even higher. And that's the challenge of doing brain research. it's going to be several lifetimes of work to unravel a human brain. And this disease has actually led us along that path.
Hannah - Thanks to Richard Faull

28:21 - Some Neuroscientist's Jokes!
Some Neuroscientist's Jokes!
with Alisa McGregor, Maurice Curtis, Mike Dragunow, Auckland University
we close the Naked Down Under show series with some of the Auckland scientists' favourite jokes...
Mike - Well, it's someone bringing back a parrot to a pet shop in one of the old  monkey python movies and the owner of the pet shop is trying to convince the person bringing it back that it actually is alive and isn't dead at all. They just to and fro, it's a fantastic skit.
monkey python movies and the owner of the pet shop is trying to convince the person bringing it back that it actually is alive and isn't dead at all. They just to and fro, it's a fantastic skit.
Lynette - I can only remember one. It's pretty terrible.
Hannah - Yeah, that's fine.
Lynette - It's my daughter's joke. What's green and goes up?
Hannah - I don't know. What's green and goes up?
Lynette - A cucumber in the elevator.
Maurice - My favourite joke is a kid joke and it's one that my wife just hates when I tell. It's, will you find a legless tortoise? And the answer of course is, when you lift it. That's pretty bad, isn't it?
Alisa - Scientists don't really do humour. We're not a normal cross-section of the population.
Hannah - And that's all we have time for. Thanks to all those in the New Zealand Naked Scientists series. That's Richard Faull, Richard Price, Lynette Tippett, Russell Schnell, Jenny Morton, and Alyssa McGregor, Malvinder Singh-Bains, Maurice Curtis and Mike Dragonow.
You can find the full transcript for this episode and others in the series at nakedscientists.com/neuroscience. If you have any questions or comments then do get in touch at Hannah@thenakedscientists.com and you can find the Naked Scientists on Facebook and Twitter. See you next month to continue the journey to open our minds.
- Previous Winter Olympics
- Next David Willetts AAAS Audio Blog










Comments
Add a comment