Coronavirus Explained: How COVID-19 Works
We take a detailed look at the coronavirus pandemic that’s sweeping the globe. How does it affect the lungs? What can doctors do about it? And meet some of the teams working on solutions, from new rapid tests for the virus to vaccines to stop it. Plus, in other news, evidence that solar storms can cause whales to beach themselves - and meet the ancient bird they call Wonderchicken...
In this episode
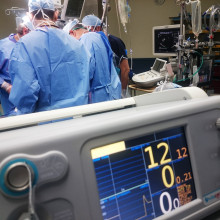
01:01 - Intensive care beds: UK close to capacity
Intensive care beds: UK close to capacity
Ari Ercole, Addenbrookes Hospital
In a UK press conference, alongside prime minister Boris Johnson and Deputy Chief Medical Officer Jenny Harries, the Secretary of State for Housing, Communities, and Local Government, Robert Jenrick, had the following message...
Robert Jenrick - Well, thank you, Prime Minister and good afternoon. As a nation we're confronted with the need to make big changes, and enormous sacrifices to our daily lives, and this is especially true today, on Mother's Day when many of us would want nothing more than to be at home with our loved ones in person. And so today we have to go further, and shield the most clinically vulnerable people to help save their lives. Following the chief medical officer's guidance, the NHS has identified up to one and a half million people in England, who face the highest risk of being hospitalised by the virus. The NHS will be contacting these people in the coming days, urging them to stay at home for a period of at least 12 weeks.
Ari Ercole, a consultant in intensive care at Addenbrookes hospital, recently published a report that predicted the UK's capacity in intensive care as the coronavirus spreads. He explained the secretary's comments to Chris Smith...
Ari - I think it's very important to realise that the coronavirus in most people, causes quite a mild disease, and it's still important because these people are infectious, hence the plans for social distancing, but most people are expected to get better from this disease without any ill effects. However, some people do go on to develop a viral pneumonia, that's an inflammation of the lungs, and when it's really severe that can prevent the patients from getting oxygen from the outside world, into their bloodstream. And in really serious cases that might mean that they need to go to the intensive care unit to be mechanically ventilated on a life support machine. And unfortunately, a lot of these people end up not surviving at the end of this process. Now as it turns out from the data that we're getting from China and from Italy, the virus seems to be effecting, particularly the older patients, and patients with comorbidities. These are the patients that disproportionately are having the severe disease and ending up on intensive care and not surviving.
Chris - What is it you've been modeling?
Ari - So one of the things that's important to realise about intensive care, is that it's not easy just to create intensive care beds. Our intensive care units, they're very specialist areas, and in the UK they run at typically 80%, often 90 or a hundred percent bed occupancy. So there isn't a lot of room to admit new patients, more patients, such as patients with coronavirus. So if we're going to deal with this pandemic, we're going to have to think about creating new intensive care beds. And unfortunately that's not something that's easy to do. It can be done, but it takes time. So for example, if you want to take ventilators from operating theatres, you need to move them, you need to train the staff, you need to make sure all the consumables are available. It's not an instant thing at all. So really, what we need, is an early warning of exactly when it is that the pandemic is likely to take hold in intensive care, and that's what we tried to do with some of the early data.
Chris - What exactly are you doing with that data and what does it reveal?
Ari - So we've taken cases as they appear, actually, in real time every day, and try to model what that means for the numbers of patients going into intensive care. And thinking about how long they will stay there, we can get an idea of how many patients at any one time are likely to be in intensive care.
Chris - Because it's not as simple as just saying: Oh, we're going to expect this number of patients on Tuesday, therefore we'll have that number of beds ready, because they don't just leave on Tuesday. They come in and they stay awhile.
Ari - Exactly. And some of them say a distribution of time. So often about seven days, but maybe up to 14 days, maybe less. It depends on the patient.
Chris - Does that mean then that those first, I don't want to call them lucky people, but will get potentially a bed, but then anyone who comes afterwards may not get one because you've got these people, I don't want to use the phrase bed blocking either, but you've got people who are occupying those high intensity beds, and they're not going anywhere.
Ari - No, exactly and that's the one situation we don't want to end up in, where we run out of ventilators, so it's absolutely, crucially important that we have enough capacity to deal with the surge in cases when it arrives.
Chris - And how much capacity do we have, and what do we anticipate the reality's going to be in terms of numbers of cases.
Ari - At the moment in the UK we have something like 4,000 intensive care beds. We're on the lower end of what's available in countries in Europe. Now, if I say that most of these, about 80% of these are occupied at any one time, at least, then maybe we can create about another 20% capacity. But once we're hitting about 20% of the number of beds, of patients with coronavirus, we're going to be in trouble with the number of beds that we normally have.
Chris - Yes. Because if 80% of 4,000, that means you've got 20% capacity leftover. That means you've got, you know, hundreds, as in about 800 beds in the entire country then, and we're anticipating how many cases?
Ari - Well it's difficult to know, but we are certainly going to have to multiply that total number of intensive care beds that we have available at by several times.
Chris - Therefore it doesn't seem that unlikely that we're going to exceed easily, the capacity that we can deliver.
Ari - Absolutely. And in fact our models suggest that we will probably reach that pinch point of 20% within a week or two. So really, really early, and after that things are likely to grow exponentially for a period of time. So actually things are going to get really bad, quite quickly if the assumptions behind our model are right.
Chris - And let's assume you are right. What preparations have you got in place to try to mitigate some of that impact?
Ari - So I think the good news is that an awful lot of NHS staff have been working really, really hard, actually for some time now to try and come up with ways and strategies of creating more capacity. But I think the really crucial thing is that we keep the efforts up, and because actually, if our model is correct, the peak might really be very close to hand.
Chris - Do you also assume then that people who are working in ITU continue to work in ITU? Have you taken into account the fact that doctors like you, are probably amongst the most exposed clinicians here, and may well therefore be lost to the service?
Ari - Absolutely. In fact that was the experience in Italy, that's been particularly hard hit. One of the things we're trying to do is find more staff, because of course one of the problems is it's not a matter of just creating a bed with a ventilator, you need the staff to actually look after the people. And of course you do have to factor in that some people are going to get ill.
Chris - Have you got them?
Ari - Certainly a huge amount of work has been done on that, and these beds are becoming available, but it's urgent now.

07:41 - Coronavirus mythbusting: ibuprofen, pregnancy & pets
Coronavirus mythbusting: ibuprofen, pregnancy & pets
Chris Smith
Phil Sansom put a few common questions about the coronavirus to virologist Chris Smith...
Phil - First off, is it actually true that you're at higher risk if you take ibuprofen?
Chris - This story emerged, we think because someone from the French ministry of health made a statement saying you shouldn't take ibuprofen if you've got this disorder, and the problem is once you've made a statement medically, it's very, very hard to row back from that, and now people are being very cautionary about it, but there is no evidence at all that people who use ibuprofen in the context of this and other viruses are at any greater risk, specifically with this one, and therefore if you're already on ibuprofen, I certainly wouldn't change what you're taking. If you're about to start taking some anti-inflammatory drugs, for instance, you have a high temperature and you want to lower it, Paracetamol is an excellent drug that is actually a bit kinder to your stomach and has fewer side effects overall than ibuprofen. So that would be a good starter drug, but I certainly wouldn't - if you only had ibuprofen and you were feeling pretty rotten - eschew using ibuprofen just because you've heard these headlines. If you have no other contraindications to using it, you're not been told by anyone not to use it in the past, you're probably going to be fine.
Phil - Okay. No evidence for risk of ibuprofen. What about if you're pregnant? Are you at higher risk? Is your baby at higher risk?
Chris - Okay. The good news here, and it's nice to have some good news around the coronavirus outbreak, is that there is again no evidence that women who are pregnant are at higher risk during their pregnancy compared with someone of the same age and other risk profile from them who's not pregnant. The only exception to this is that we know that when someone's pregnant in the first part of their pregnancy, so that's the first trimester, the first about 12 weeks, there is, for any kind of infection or any kind of problem that you might get, that causes this associated with a high temperature, there is a slightly higher risk of a bad outcome to your pregnancy. It's a small risk or the same, but therefore if you can avoid catching this, because being pregnant is a risk factor for that happening, that would be a good idea. But when the chief medical officer said that we're going to regard pregnant women as in a high risk category, it did alarm a lot of people. But that's just because we're being very cautious. It's not because there's evidence that there's any risk of harm. And the other good piece of news is that there's no chance that this virus can jump across the placenta, which is the connection between the mum's bloodstream and the baby's bloodstream. It doesn't cross that barrier. Therefore it doesn't infect the baby when it's inside the mum and there's no risk of it doing developmental damage to the baby.
Phil - And finally, what about our beloved cats and dogs? Can they catch the virus?
Chris - This gets asked a lot. There was one paper that came out from Hong Kong, where a person who had this infection, that somehow their dog ended up being tested. It was a Pomeranian dog. It got tested and low levels of virus were recovered from the dog. Now this virus does infect animals. It came to us after all from bats, and probably via a pangolin as well, another mammal, so it can infect other animals. Therefore, there's no reason why it couldn't infect a dog or a cat, but we don't actually believe that the risk is high. We don't think the dog was shedding appreciably large amounts of virus and therefore you're probably absolutely fine, and your pets are not going to affect you, and you're probably not going to put them in jeopardy either.

12:12 - Whales and solar storms: a surprising link
Whales and solar storms: a surprising link
Jesse Granger, Duke University
Every year, hundreds of whales get stranded on beaches - many of them still alive, healthy, and with seemingly no reason to be there. But there’s a bizarre correlation between these strandings and the activity of the sun. And now, biologists from Duke University think they might have uncovered the specific connection, and it's to radio noise that comes from solar storms. They’re suggesting that whales might be using the Earth’s magnetic field to navigate, and their magnetic sense gets thrown off by this radio noise. Phil Sansom heard more from lead author Jesse Granger…
Jesse - We have discovered that there seems to be this really strange correlation, between grey whale strandings and things that are happening on the Sun. It seems as though there is a pattern between how active the Sun is, how much it's spewing out radiation, and how often these grey whales seem to be stranding.
Phil - I have to say, it sounds kind of like a 2012 style movie plot, that something going on with the Sun is making whales wash up on beaches. I mean what's the connection there?
Jesse - I know it's a bit crazy. I'm still a bit shook, and I'm still not sure I believe it, but what we really think is, so there are many animals on the planet that have the ability to sense the Earth's magnetic field, and they use that as essentially their own internal GPS system, while they're making these really long distance migrations. Perhaps these whales are magneto-receptive. They're also using the Earth's magnetic field when they're making this navigational trek. And the Sun might actually be disrupting the information that they're getting. And that's why we're seeing this pattern.
Phil - Is that something that's dangerous for whales?
Jesse - It is. It can potentially be deadly for many of them. A lot of whales that strand, actually strand dead, but we actually didn't look at any of those strandings. We only looked at these standings where the whales were alive, and there didn't seem to be a really obvious reason for them to be stranding. And we said, well, perhaps they're making a navigational mistake, and that's how they ended up washing onto the beach.
Phil - In that case, what's going on with the Sun that could disrupt the Earth's magnetic field?
Jesse - So we kind of came up with two hypotheses for what could be happening. Option one, the Sun could be pushing around the Earth's magnetic field. If you've ever had your GPS, like, jump over a couple of streets and it tells you you're not where you are, maybe that's what's happening.
Phil - It's like they're reading the magnetic field like a map, but all the contour lines have been pushed weirdly to the left or something.
Jesse - Yeah, exactly.
Phil - Okay. That's theory one. What's theory two?
Jesse - So theory two, the Sun does create a lot of radio frequency noise. Radio frequency noise can prevent an animal from sensing magnetic signals. There's radio frequency noise coming off the Sun during these solar storms, so perhaps it's actually turning off the whale's sensor altogether. So the whales using this GPS to navigate and all of a sudden it just turns off.
Phil - And what did you do to distinguish between whether it's solar storms disrupting the Earth's magnetic field, or it's the radio frequency noise that's messing with the whale's ability to read the magnetic field.
Jesse - So we can actually distinguish between those two things using some variables we measure here on the Earth. One of them is going to be looking at how much the Earth's field is wiggling around, and we measure that using a variable called the Ap-index.
Phil - What's Ap stand for?
Jesse - I don't know.
Phil - Okay, it's wiggling.
Jesse - It's wiggling. It's wiggling around, we look to see, do the whales seem to be stranding when the Ap-index is really high? So the Earth's field is wiggling around a whole lot, and the answer was no. I sat and got very frustrated and I was like, what the heck? What's going on? I'm so angry. Why didn't this work? I went back to the drawing board and we started to ask, okay, so what is the second option? That's where we came across this radio frequency noise, or RF noise for short. And our actual strandings were all happening so much more frequently when the RF noise was really, really high. However, you have to be really, really careful with stats like this. It's so easy to look at a correlation and try and say, well, obviously this must be affecting a magnetic sensor. But with correlation studies like this, all you can say is we see a pattern. Maybe this is an explanation.
Phil - If this is the case, what might this mean for whales?
Jesse - So one of the things about this study that I think has a lot of really great potential, is regardless of what the mechanism is behind this correlation, we see it. Whales strand alive more often when the Sun is really active, and whether or not this is actually an effect on a magnetic sense, we can predict when the Sun is going to be really active fairly well. Potentially, this could be used as another way of predicting when we need to be more active about looking for live strandings happening. So perhaps we can save one more live whale from dying on the beach.

17:47 - Microorganisms discovered under seabed
Microorganisms discovered under seabed
Ginny Edgcomb, Woods Hole Oceanographic Institution
Scientists have discovered life in the deepest parts of the rock floor under the oceans - tiny microorganisms that live in the 'lower oceanic crust'. Melanie Jans-Singh reports...
Melanie - Over the last decades, researchers have looked for signs of life underground, in gold mines and in the seafloor. They’ve focused mostly on life in the first layer of the seafloor, which consists of sediments, and that’s mud mixed with dead fish and other microorganisms containing carbon. Below the mud is the rocky ocean crust. And the lower crust has not been explored much because it's typically 4-8 km deep. But there are parts of the world where this lower crust is exposed, like in Atlantis Bank in the middle of the Indian ocean where this expedition took place.
Ginny - We really didn't know what to expect because it seems like such an inhospitable environment.
Melanie - That's Ginny Edgcomb, from the Woods Hole Oceanographic Institution.
Ginny - But there had been a study previously, that had found signatures of life in gabbro samples from another location. And so we were optimistic that we might find something and we thought if we did, we'd probably find signs of life around cracks and fissures in the rock where fluids might be able to deliver carbon and energy sources to microbes living down there.
Melanie - How did you manage to get samples from under the sea floor like that?
Ginny - This kind of work is made possible through ocean drilling and requires a special drill ship that can hold a position over a spot that you want to drill into the sea floor on. And, and we spent two months, drilling down through the lower crust at this one location and every 10 meters of advancement a sample of the rock would come up to the drill ship and people would be able to quickly process it, and we could take samples for microbiology.
Melanie - How did you make sure that nothing was being contaminated by the environment around you?
Ginny - Since drilling requires us to pump fluid down to the drill bit to keep it cool while it's drilling, we had to be really careful that we removed all traces of that fluid before we collected samples for analysis. We did this in a couple of different ways. We ran a chemical along with the seawater and mud that the ship pumps down to the drill bit. We put a chemical in there that we would be able to detect in the laboratory, and we made sure that we couldn't detect any more traces of that chemical before we collected samples for analysis.
Melanie - When analysing in the lab they also checked that they were not contaminating through the lab equipment or the handling process, and took many steps to control everything, sometimes throwing away possibly good data. It was worth it though! They found that microorganisms deep under the seafloor were alive because they had genes to do things like dividing, which must mean they have enough food to live on. I asked Ginny how they could survive there?
Ginny - Organisms that live so far under the sea floor have to survive by being able to store carbon. When they see it, they can store it. We think in the form of a molecule that is kind of like storing fat would be for humans. But it's not fat. They can store it and keep it for a rainy day. They can also recycle different forms of carbon internally, which is something not all organisms do or have to do because they live in environments where they have plenty of carbon to access. So in the deep seafloor, and below the seafloor, many organisms are probably in a state of suspended animation. You know, they're just eking out a living.
Melanie - Even if the cells down there are just surviving, they're still consuming carbon. So now we know to take these organisms into account when calculating the world's carbon budgets.
Ginny - We are expanding our idea of what the habitable portion of Earth's biosphere is. So it's not just what you see above land and in the oceans, and it's not just the muddy ocean sediments, it's not just the basalts of the upper ocean crust, but it now includes at least some portion of the lower ocean crust.

22:37 - Wonderchicken: meet the oldest ever fossil bird
Wonderchicken: meet the oldest ever fossil bird
Daniel Field, University of Cambridge
When scientists at the University of Cambridge scanned a nondescript piece of rock dating from the end of the dinosaur era, they got the shock of their lives. Inside was a near-complete skull of a bird similar to modern day ducks and chickens. In fact, they’ve dubbed it “Wonderchicken”. Phil Sansom spoke to its discoverer Daniel Field about its significance...
Daniel - Well, it looks like a very strange bird skull, because it shows some features shared by living chickens and also living ducks. So in some ways the skull is a mash up of what you might think of as a chicken-like bird skull and a duck-like bird skull. If you hold it in your hand, it's tiny about the size of a large quail or a small partridge.
Phil - And how did you actually find it?
Daniel - The bones themselves were actually dug out in Belgium back in the year 2000, but the specimen doesn't look like much. It's basically just a few broken rocks with some nondescript, poorly preserved limb bones poking out. So the specimen wasn't studied until 2018. I CT scanned it with my PhD student, Juan Benito at Cambridge, which allowed us to peer inside the rock. And when we did, we were absolutely shocked to see that inside the rock. Totally invisible from the surface is this beautifully preserved bird skull from about 66.7 million years ago.
Phil - What were birds, and the rest of the world like, back so long ago?
Daniel - We're talking about rocks that date to the very end of the age of dinosaurs, when Tyrannosaurus Rex and Triceratops, some of the most iconic dinosaurs of all time, were still roaming the Earth. But what's fascinating and what we really didn't know that much about before, was the extent to which what we think of as modern birds were around at that point. And finding this fossil, which is the oldest, well-documented modern bird fossil ever discovered, tells us that there were at least a handful of major living lineages of birds around on the planet before that asteroid struck.
Phil - Now when you say modern bird, what do you mean? Because I heard dinosaurs come from birds.
Daniel - Well we have birds are of course..
Phil - The other way around. Birds come from dinosaurs, you know?
Daniel - That's right. Yup. But that's a very long, protracted process that we're talking about. So, you know, roughly 150 million years ago, we have Archaeopteryx, which a lot of people like to talk about is the first bird. It's a very bird-like dinosaur in that it's got feathered wings, but it also has tiny teeth in its mouth. And we know that bird-like animals that retained teeth persisted all the way to the age of dinosaurs, until the asteroid struck the earth and wiped them out. So when I talk about modern birds, I'm talking about the most recent common ancestor of all living birds and then all of that ancestor’s descendants. And we think this new fossil provides us with our best insights so far into what these early modern birds were like, coexisting with the very latest stages of non-avian dinosaur history.
Phil - Now you mentioned teeth. Is that crucial here?
Daniel - Well the Wonderchicken, being a modern bird, does not have teeth. So modern birds, as I've defined them, would have shared a bunch of features ancestrally that we associate with birds today. So that includes, of course, a toothless beak, feathered body and ancestral ability to fly, high metabolic rates, those sorts of things. But the beak of the Wonderchicken itself is interesting, because it doesn't seem to show any particular specialisation for a particularly specialised diet. So it sort of looks like the beak of a living chicken. And we know that most chicken-like birds are fairly generalist in terms of what they eat. And we're wondering if the shape of the beak in the Wonderchicken might suggest some features that might've helped the ancestors of modern birds survive in the aftermath of the extinction event.

27:49 - Modelling: the UK's coronavirus strategy explained
Modelling: the UK's coronavirus strategy explained
Freya Jephcott, University of Cambridge
There's a foundation of science underpinning the UK - and other nation’s - strategies to control the outbreak. The governments of these countries are relying heavily on mathematical models, including work by a team from Imperial College London. Freya Jephcott at the University of Cambridge independently studies how diseases spread, and Chris Smith asked her what those models are saying...
Freya - Right now we're moving towards something called suppression. So that model that Imperial made to feel out all these different possible scenarios came up with two key scenarios for us. One was when we do something called mitigation, which is where we try and slow the spread of the outbreak; that's where all that discussion of flattening the curve has come from. And then the other scenario, scenario B, is the suppression strategy; where we essentially try and just block transmission altogether through some more extreme social distancing interventions. This comes down to three key elements: home isolation for people with any signs of respiratory illness and isolation of all their household members, and that's for two weeks; and the other elements that have come in here is social distancing of the whole population. Now what that actually means was this idea that all of our contacts outside of work and school and the household would reduce by three quarters. Going to the pub, seeing friends, going to coffee shops; all of these interactions would dramatically reduce. Also workplace rate, so the amount that adults are mixing at work; that this would reduce by at least a quarter. They did allow that our household contacts, if we do this, were going to increase by a quarter. So there's a bit of an offset there. And the final element was either partial or full closures of schools and universities, and this seems to be the thing that's coming to the fore right now: this idea that we're going to close school to some children. Now one of the big concerns earlier on when this was discussed is that something like a third of our nurses, or healthcare workers in general, actually have school-age children; and that we're doing all these things to try and reduce the strain on our health system in the coming months, and that perhaps we might actually be making staff shortages worse if we do this. So it looks like the government has come to a strategy where people who have children, people who work in what are considered essential services - so healthcare, groceries, police, firefighters - their children will still attend school.
Chris - The overriding aim is to reduce contact between people because that is how the disease spreads. So if you reduce the contact between the people, you reduce the opportunities for transmission, and therefore we must by default slow down the spread, the rate at which it's transmitting through the population.
Freya - Absolutely. That's it. So everything we're doing now is to try and reduce the number of opportunities for new people to get infected with the virus, even if they're not confirmed cases. And so we're doing that by trying to reduce social contacts generally. Though we've gone from trying to just slow it, to actually now the strategy is to try and sort of stamp it out almost entirely for now.
Chris - Do you think that is likely to be achieved?
Freya - The reason we think it might be possible: in China - and they do have a lot more infrastructure and was a lot more compulsory than anything you'd bring in here - it does seem to have significantly reduced transmission, to the point where maybe there's very, very little community transmission going on now. South Korea similarly, they took a slightly different approach there, but again with this extreme social distancing. And they're seeing a bit of an uptick in cases, but otherwise they did bring down the community transmission dramatically. The catch here is that with this strategy, if we began to loosen these quite extreme measures, there is a good chance that we could see a big uptick in cases again.
Chris - If everyone did this all at the same time for a period of time, would it just disappear? Is it just the fact that at the moment, if any one country loosens its grip, it will just get this thing coming back; and we can be really diligent here in the UK, but if say a third world country which doesn't have the ability to implement these sorts of strategies acts as a sort of nidus or a hotbed for this, it'll just seed it back into everywhere that's very successfully stamped it out?
Freya - Absolutely. We are all in this together and we're only as strong as our weakest part. We need basic infrastructure so these kinds of interventions are possible globally, because like I said we can stamp it out in countries with the infrastructure, but as soon as we loosen it, we will get imported cases and we will get transmission starting again.
Chris - And just finally Freya, where do you think - and I realise I'm putting you horribly on the spot - but where do you think this is going to end, and how?
Freya - If we did absolutely nothing, it sounds like we would have hit peak cases and peak deaths within the next three months. So that would be quite a short ending but quite a bad ending. So I think that actually we're looking at this unfolding over months and years. The interventions that Imperial College suggested: in their models they lasted for about five months. If you hear the discussions of vaccines, that's still maybe a year, 18 months at best, away. It is worth keeping in mind that we're in this for the long haul and we need to think about interventions and policies for the distant future.
32:55 - Coronavirus: what it does to your lungs
Coronavirus: what it does to your lungs
Sanjay Mukhopadhyay, Cleveland Clinics
What actually happens to people infected with the coronavirus? The vast majority develop two main symptoms: a dry cough and a fever. Most also report fatigue and muscle aches and pains, and data released in just the last few days suggests that a lot of patients also develop gastrointestinal symptoms, including diarrhoea. The biggest impact though does appear to be on the respiratory system. So what is the virus doing to produce these effects? Phil Sansom asked lung pathologist Sanjay Mukhopadhyay to explain…
Sanjay - In the most asymptomatic - so people who don't have any symptoms - the best hypothesis would be that these viral particles just sort of stay there and evoke minimal reaction from the tissue. As you get to more and more symptoms, it would be plausible that the tissue reaction actually involves inflammation; that means the immune cells come in to destroy the virus, and that the interplay between the virus and the immune cells causes further destruction. And then the most severe people it seems are developing a very severe form of lung damage, that we call as pathologists diffuse alveolar damage...
Phil - Diffuse alveolar damage?
Sanjay - That's correct. And diffuse alveolar damage is essentially what happens if you get any kind of very severe injury to the lung, regardless of the stimulus. Conceptually, diffuse alveolar damage as seen by a pathologist is sort of the equivalent of seeing a building strewn all over the ground in a damaged way. You see the end result of what happened; you'd don't necessarily see what caused it.
Phil - What does it look like then?
Sanjay - What happens is: the alveoli - which is the air sacs, right, the very last portion of your lung where the gas exchange goes on - they're like little balloons. Every time you inhale, those balloons get bigger, and when you exhale, those balloons get smaller. Oxygen is supposed to traverse the wall of those balloons and then go inside the blood vessels that are in the substance of the balloon. The thickness of the balloon therefore has to be extremely thin so that gas exchange can occur. When the damage occurs you get a lining of sort of debris that lines the inner side of those alveoli or air sacs. It looks pink under the microscope. And as time goes on, the walls of the alveoli tend to get really, really thick. And you can imagine if the thin alveoli are necessary for breathing, that thick alveoli would be very bad for breathing.
Phil - Do you have to go into someone's lungs and take a look at the tissue? Is there an easier way to tell that they've got this kind of damage?
Sanjay - Almost nobody, or very few people, actually come to the stage where doctors actually need to send a piece of tissue off to a pathologist to look at under a microscope. And so most of the patients who are sick and come to the hospital get a chest X-ray or a CT scan, and on those, normal lungs look black because they're filled with air. Now when you get an infection, you start to get what are known as opacities in the lungs. And that means that the lung, instead of being black, starts to look white.
Phil - So white long on the scan equals probably this kind of damage?
Sanjay - Yes, that's correct. And the more the white, the worse it is.
Phil - So you have these two things then that you talked about: the war between the virus and the immune system, and then also this diffuse alveolar damage. How do those things connect to the symptoms that the coronavirus causes?
Sanjay - I'm not sure there's a complete one-to-one correspondence between the symptoms and what's going on, but it is plausible at least that as the virus goes down from the back of the throat down into the windpipe, that damage - or the back and forth damage - actually causes irritation to those cells, and that to some extent accounts for the cough that's going on. It is also possible that the damage in the air sacs and all that debris that that's producing is also producing some degree of cough. So both the action in the airways as well as the action in the air sacs all could be leading to the cough that's going on in these patients.
Phil - And how does what you're seeing in these people's lungs compare to something like the flu?
Sanjay - Overall the immune response and the kind of damage that's occurring in the lungs is likely to be very similar to the flu, and to other similar viruses that we've seen in the past. Now I will add a caveat that we are in very early days, but from the very early reports it seems like it is almost identical to what we have known with other viruses.
Phil - But they have different symptoms?
Sanjay - In terms of just the standard symptoms of cough, shortness of breath, and fever, those are not very significantly different between SARS coronavirus and other severe viruses.
Phil - The people who have this diffuse alveolar damage - I assume the worst-off are those people that we see needing ventilators because they have trouble getting enough oxygen - is that damage to their lungs permanent?
Sanjay - Depends. In general, people with diffuse alveolar damage develop a syndrome that's called acute respiratory distress syndrome. In about half of these patients the outcome is fatal. So it's a very severe and irreversible form of disease in about half or 50% of patients. In the other half of patients, there's sort of a mixed outcome. Some of those patients can recover completely, but there are others who go on to develop scarring in the lungs or what we call fibrosis. That can cause problems in terms of breathing and cough in the long term.
Phil - And for the people who don't have this diffuse alveolar damage, who only have a very mild case of the infection, will they come out with any sort of issues with their lungs?
Sanjay - They shouldn't! We have been focusing on the very, very severe end of this spectrum, right? But we must remember that the majority of patients actually don't get to that point. The vast majority of patients either have no symptoms, or they have symptoms that are relatively mild - so cough and shortness of breath - but nowhere near developing the acute respiratory distress syndrome. It seems like many of those patients recover completely and then can go back home.
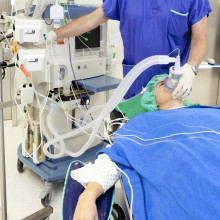
39:08 - Treating coronavirus: what's intensive care?
Treating coronavirus: what's intensive care?
Charlotte Summers, Addenbrooke's Hospital
A small number of coronavirus patients get more severe symptoms. So when doctors have to treat those symptoms, what do they actually do? Chris Smith asked Charlotte Summers, an intensive care doctor at Addenbrooke’s Hospital in Cambridge...
Charlotte - The main reason that they present to us is because they are not able to get enough oxygen in, because their lungs are not functioning efficiently.
Chris - Why?
Charlotte - The gap between the oxygen coming into the airway sacs and your blood has got a bit bigger, and so the diffusion of the gas from the alveolus into the bloodstream is compromised. So actually you're not getting enough oxygen from the air across into your blood and off to the remote tissues for your organ functions.
Chris - And if I just breathe a bit more often, is that not sufficient to compensate for the fact that my lungs aren't pushing as much oxygen as quickly into the blood? I just breathe a bit more, that should compensate, shouldn't it?
Charlotte - It's about supply and demand. When the gap between your lung tissue and your blood has got bigger, the speed at which you breathe does not necessarily compensate enough for the profound lack of oxygen that you get.
Chris - When someone shows signs that they're not getting enough oxygen into the blood - and I presume you can measure that - what's the first thing you do?
Charlotte - The first thing's really simple: we give them supplemental oxygen. So we do that via facemasks, or via some tubing that goes into the nose, to give you an increased amount of inspired oxygen.
Chris - And how does that help? Because if you've got that gap between where the oxygen is and where the blood is that needs the oxygen, how does having more oxygen there to start with compensate?
Charlotte - Well like any other substance pretty much in biology, things move from an area of high concentration to an area of low concentration. If I can increase the size of that concentration gradient, then actually I'm probably increasing the efficiency of the oxygen transfer from the alveolus into the blood.
Chris - And in what fraction of patients will that be enough?
Charlotte - So in the setting of coronavirus, it looks like about 1020% of people out of all of the people who get the virus probably need to come to hospital, and most of the people who are coming into hospital are coming in because they're unwell enough to need some support for their breathing.
Chris - When would they become a candidate for you then?
Charlotte - So if giving you supplemental oxygen wasn't enough, then you get to meet people like me.
Chris - So if a person gets taken to intensive care, what sorts of things do you do to keep people alive?
Charlotte - We can use tight-fitting facemasks that blow air into your lungs to try and open up congested bits of your lung. If that's not working, then actually we end up saying, "fine, we need to put you to sleep using drugs - so very much like a general anaesthetic that you would have for a surgery - and pop a tube down into your trachea that securely sits in your airway, so that we can use a mechanical ventilator to blow air into your lung and try and take over the work of your breathing completely.
Chris - Why is is blowing air in in that way any different than a person breathing for themselves? What can you achieve by that, that I can't achieve by just taking a deeper breath?
Charlotte - What it's aiming to do is to stop inflamed and congested bits of your lung collapsing at the end of you breathing out, by providing some pressure; but also providing support for your muscles breathing in and out, and the extra work of breathing that you have to do when you're profoundly lacking in oxygen.
Chris - How long are they probably going to need that ventilation, and what is that doing? Is it giving time for the lungs to recover themselves and just keep the person alive while that happens, or is there something else going on?
Charlotte - It's a supportive therapy, it is not a cure. It is just buying time for your body and whatever therapies can be instituted to do their work. In coronavirus there are no validated therapies and things that have been shown to be of clinical benefit, so all we have is supportive therapy and the hope that your body can heal itself over time with us looking after it as best we can. The length of time that people are needing mechanical ventilation is actually days to weeks currently based on some of the data that's coming out of Europe, so it's not something that happens for a very few hours. And every day you are on a ventilator the consequences of being ventilated climb, and your muscles get a little bit weaker, and the road back to being the person that you were when you came into hospital is just that little bit longer.
Chris - Charlotte Summers there from Addenbrooke's Hospital. We've also had an email to chris@thenakedscientists.com from John Blanning who says, "can you tell us how many people who go into the Intensive Care Unit on a ventilator actually survive with coronavirus?" I put this question to Ari Ercole, consultant ITU physician, who said actually, the numbers are not that encouraging. A significant proportion of people are not going to make it despite the best efforts of ITU. So that is a very sobering message.
44:20 - Antigens: mass-producing coronavirus parts
Antigens: mass-producing coronavirus parts
Andy Lane, The Native Antigen Company
Alongside the medical efforts being made, scientists are also hard at work trying to understand the virus and come up with better ways to detect it and make vaccines. To do that, they need key parts of the virus to study, and in particular components of the coat of the coronavirus - the spikes that make it look like a crown, or corona, and so give it its name. And this is where the Oxford-based Native Antigen Company are making big steps forward and providing researchers with these critical components. Adam Murphy spoke to their commercial director, Andy Lane...
Andy - There's a protein on the surface of the virus that is called the spike protein, which the virus uses for a number of things, but especially to gain entry into human cells. We make two proteins from that, one called S1, one called S2, and what people think happens is that the surface protein on the virus, the spike protein, binds to a particular receptor that some cells have on the surface. And once it's bound to that, it becomes internalised into the cell. And that's where it can replicate and obviously grow in numbers.
Adam - How do you go about making protein parts of a virus?
Andy - We rely very much on having the genetic sequence of the virus available. That was published by the Chinese really quite early in the outbreak. Once the genetic sequence is available, we can synthesise the individual genes from the virus and to put it very simply, we insert them into a human cell system that we have that makes proteins pretty much on demand.
Adam - Who are you sending them to and what are they going to do with them?
Andy - So we send them to probably three different types of people. One key type for us at the moment are companies around the world who are trying to make diagnostic tests. The aim is to detect the body's immune response to the virus, which is generally considered to be an antibody response. And if you make an antibody response to the virus, those antibodies will bind the proteins we make and can be used in tests that these diagnostic companies make. An antibody test has a great advantage that it can detect an immune response from many months after an infection and an antibody test will potentially be able to find out how many asymptomatic people there are in the population. The vaccine development companies is another group of customers. When they test their vaccines, initially usually in animal models and then later on in humans, they will be looking to make sure that those vaccines produce an immune response against the virus and they can use the proteins that we make to confirm that. And then the third group of people are the academic researchers who are really investigating everything they can find out about the virus at the moment. But we're finding it important in ourselves to realise that this isn't just a simple business opportunity, that we're here right now to help the worldwide response to this, developing the right proteins and making sure that we support as many efforts as we can both in the UK and around the world.
47:33 - Testing: building a rapid coronavirus test
Testing: building a rapid coronavirus test
Annelyse Duvoix, Mologic
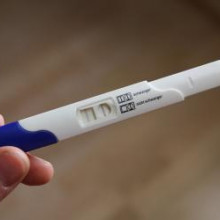
Some of the coronavirus antigens are going to companies working on better tests for the coronavirus. At the moment we’re testing for it by looking for the genetic code of the virus, and that’s a relatively slow process. But Bedfordshire-based Mologic have just received a million pound grant from the UK government to develop a rapid test that should work within minutes. They’re a company that formed out of the team that invented the modern pregnancy test. And when Phil Sansom spoke to their scientist Annelyse Duvoix, she explained that the finished coronavirus test should be very similar...
Annelyse - It's basically going to look like a pregnancy test, except we do not use urine as our sample.
Phil - So a little bit of plastic that you can just spit on or something. And then it could tell you whether you might have the coronavirus?
Annelyse - Yeah, something like that. So we might use blood samples from your finger like you would do if you had diabetes.
Phil - Like a pregnancy test, it should be able to detect the presence of the coronavirus by showing up a visible line on the test. They're going to do this by using antibodies, parts of people's immune systems that recognise invaders, and these ones are going to recognise the outer coating of the coronavirus. Usually this kind of test actually involves a pair of antibodies.
Annelyse - So we usually need two. We've procured some antibodies, commercial antibodies. We are very early on and we're just going to start testing those.
Phil - One antibody is stuck onto the test in a line at the far end. The second antibody is linked to a coloured material. They use tiny, tiny particles of gold.
Annelyse - We usually use gold cause it's large and it's red.
Phil - And that's at the opposite end of the test. When you add the saliva or blood to the test, it dissolves and takes up the antibody with the gold into a suspension. If the blood or the saliva had virus in it, the antibody is going to stick to the virus. Then all this liquid soaks up through the test carrying the virus and the antibody with it. When it reaches the opposite end of the test, the second set of antibodies, the ones glued into a line there, they grab any of the virus that's in there and because the antibody with the colour was already stuck to those virus particles, that gold comes out and is visible there as a line. How long does the test take between a sample of blood or whatever and actually revealing whether or not there's the coronavirus present?
Annelyse - Usually we go for 10 minutes.
Phil - How long does that compare to the test people are using at the moment?
Annelyse - Some of the tests you need to send a sample to the lab, you will get an answer within the day, I would say, but nowhere near 10 minutes.
Phil - So this is a fraction of the time and presumably a fraction of the cost once it's actually made, right?
Annelyse - Yes.
Phil - Okay, million dollar question: how long do you think it's going to take?
Annelyse - We don't know. It could work very easily and simply. However, we could also find that the antibodies that we've got don't like to work together, or that we detect more than the COVID-19 virus and we need to go back and find the antibodies that don't recognise other viruses; but if everything works and we are lucky we could have a first prototype, early prototype, within two weeks to a month.
Phil - Murphy's law, things very often go wrong...
Annelyse - Of course.
Phil - ...it may take a few more months, yes?
Annelyse - Yeah.
50:55 - Vaccinating: making a nasal vaccine for coronavirus
Vaccinating: making a nasal vaccine for coronavirus
Steve Powell, eTheRNA
How is the world going to stop this pandemic? And not just stop it, but stop it coming back? It looks like a vaccine is the best option, and there are already thankfully teams all over the world racing to develop vaccine candidates. But one possibility is that the virus could change or mutate in some way, the company eTheRNA are targeting parts of the virus that they think won’t ever change. Their approach, developed originally as a vaccine for cancer, involves administering short pieces of genetic material that code for certain parts of the virus structure. Immune cells can pick up these instructions, decode them and then mount a protective response - as CEO Steve Powell explained to Chris Smith...
Steven - The traditional vaccine approach is based on generating antibody responses to the virus. The problem is that when this virus comes back, just as we see with waves of influenza, then the chances are it will come back in a different format. Rather than focus the vaccine on a specific protein that is sitting on the surface of the virus, what we want to find are parts of that virus coat that however much the virus mutates will always be present. And then rather than just create a short lived antibody response, which is a typical response of the body to any invader, what we want to do is to create a longer lasting response which would provide long term protection for healthcare workers when an epidemic breaks out.
Chris - How easy is it to find parts of the virus that don't change in that way?
Steven - Well, the advantage is that people have been able to understand the structure of the virus and been able to analyse that structure. And we have been working with a number of different partners to really take all of that data, push it through very large data processing programmes, and then identify very specific parts of protein that we can then build into our vaccine, which we will then deliver in a slightly unusual way. We're looking to deliver them up the nose using a nasal spray and therefore what we're looking to create is a very strong vaccine response in the upper respiratory tract and in the nasal passages.
Chris - Having identified these parts of the surface of the virus that you think are not ever going to change, you can then, what, make those bits of the virus artificially?
Steven - That's right, so we can take those pieces, make them artificially, we can then use our existing technology to amplify the body's response to those pieces.
Chris - So you get more bang for your immunological buck if you like.
Steven - Yeah, that's exactly right. Now we've been doing this work in both cancer disease areas and also infectious disease areas so we know we can amplify the signal. The key to this is finding the right piece.
Chris - And this all goes up the nose.
Steven - In this case, in the setting of corona, we need to be able to deliver this to a very large, healthy patient population.
Chris - And is it protein, the bit of the surface coat of the virus that you're doing this with, or is it the genetic code that codes for that protein in the virus that you're putting into the patients?
Steven - Yeah, so we use something called messenger RNA. We take the code for the protein and we build that into the messenger RNA. And when that's delivered into the body, it's read, just like a computer programme. And from that reading comes the protein that would exist in the virus coat and that then creates the immune response.
Chris - You've been doing this, as you say, for targeting cancers. How do you know though, that this will work against something very different? Because an infectious disease is quite a different entity to a cancer.
Steven - It is and we have indeed already done it for a number of other viral infections including HIV and other respiratory tract virus infections. So we know it will work.
Chris - There are a number of players entering this market because obviously the potential here is huge. They're all saying though that it's one thing to make a potential vaccine, it's another to then get it very rapidly through all of the regulatory hoops to make sure we've got something that's safe and effective and therefore good value for money.
Steven - I think the difference between what we are advocating and what is being quite widely talked about, is that the other approaches are relatively short term measures. What we're trying to do is to develop something rapidly, way more rapidly than would normally be done, but equally it's not something that we're trying to push into a clinical trial in the next few weeks. We're actually looking to do this over a longer period of time so that we can interact effectively with a number of different regulatory agencies, not just in one geography but quite widely.
Chris - How long is longer term do you think? When do you think, with a fair wind behind you, you could have something that would actually be useful in the present outbreak situation?
Steven - From our approach, this is months. This is putting something into clinical trials very early in 2021, so next year. But this approach is relevant not just for coronavirus, but for other serious viral infections, including something that we're all well acquainted with, such as influenza, and that we can use this approach with a number of different virus infections as and when they inevitably return in different mutated forms.
Related Content
- Previous Is space lettuce good for you?
- Next COVID-19: Will lock-down work?










Comments
Add a comment