This week we learn about Alzheimer's disease, how it changes the brain and may be caused by the virus which causes cold sores. We probe your grey matter to find out how memory works, what goes wrong to give us false memories, and the science behind earworms - the songs that we can't get out of our heads! Also, GM plants that can survive a drought, why future chewing gum may contain magnolia bark and how a mirror can kill phantom limb pain. Plus, in Kitchen Science, we fool our senses with some plastic, some paper and a carpet!
In this episode

01:59 - Wilt-not want-not
Wilt-not want-not
Strains of drought-resistant GM plants to preserve crop yields and combat the effects of climate change have been announced by US scientists...
The experimental tobacco plants created by UC Davis researcher Eduardo Blumwald and his colleagues grew normally under ideal conditions, could still grow well when given only a fraction of their normal requirements and were even able to tolerate 15 days without water altogether. Unmodified "control" tobacco exposed to the same conditions, however, all died.
The team created the plants by blocking a process known as "leaf senescence" in which plants artifically age and drop their leaves in order to reduce their leaf area and hence their water requirements.
Whilst this can help to preserve the growing cycle of the plant it reduces the yield of an annual crop. So to prevent this from occurring the researchers used genetic techniques to switch on a gene called IPT - isopentenyltransferase - whenever and wherever the plant tissues became stressed by a lack of water.
IPT boosts the production of a growth-related gene called cytokinin (CK), which helps to protect leaves against the effects of water shortage.
Encouragingly, the transgenic crops continued to grow well under conditions of severe water restriction. Grown side by side with unmodified control plants and given only a third (0.3 litres) of their normal water requirement for 4 months to simulate a prolonged dry spell, the modified plants dropped their yield by only 8-14% compared with a 60% loss of yield for the unmodified plants.
The team hope that their results could be used to produce low-water tolerant crops that could be used to make arid-land more productive, or enable farmers to save irrigation water whilst maintaining higher crop yields.
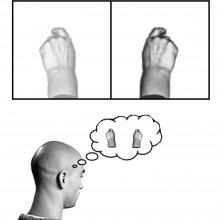
Doctors reflect on mirrors as a therapy for pain
Doctors in America have shown that a mirror is an effective therapy for the "phantom" pain experienced by 90% of patients undergoing limb amputation.
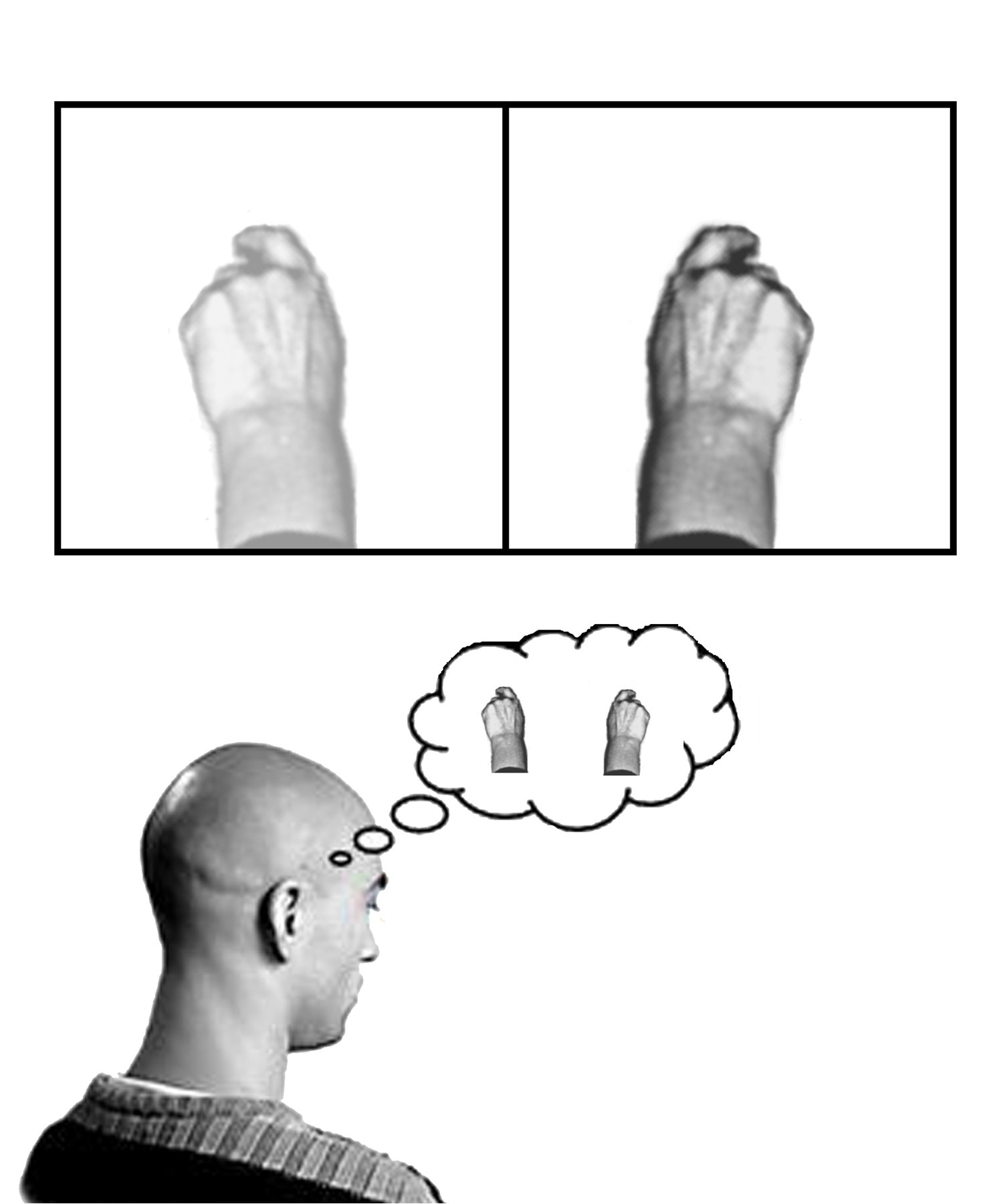 Writing in the New England Journal of Medicine, Bethesda-based researcher Jack Tsao and his colleagues describe how they recruited 22 lower limb amputees. The volunteers were randomly divided into three groups; in one group, the "mirror group", the reflection of the subject's intact limb was used to create the illusion that the missing body part was still present. The patients were told to try to make movements with their absent limb by watching the reflection of their intact leg making the same movement. In the second "control" group the mirror was covered with an opaque sheet, whilst the third group of patients were instructed just to imagine making movements with their amputated leg.
Writing in the New England Journal of Medicine, Bethesda-based researcher Jack Tsao and his colleagues describe how they recruited 22 lower limb amputees. The volunteers were randomly divided into three groups; in one group, the "mirror group", the reflection of the subject's intact limb was used to create the illusion that the missing body part was still present. The patients were told to try to make movements with their absent limb by watching the reflection of their intact leg making the same movement. In the second "control" group the mirror was covered with an opaque sheet, whilst the third group of patients were instructed just to imagine making movements with their amputated leg.
The results were shocking - after four weeks of treatment 100% of the patients in the mirror group reported that their pain had improved, although patients in the other two groups faired less well. Amongst the covered-mirror volunteers 50% felt that their pain had worsened (although one patient reported improvement), and the visualisation group fared worst of all - 67% said their pain had intensified. Next the researchers switched the patients from the visualisation and covered-mirror groups to mirror therapy, and their pain improved dramatically, becoming similar to that reported by the first group of mirror patients. The researchers aren't certain how the technique works but suspect that a population of appropriately-termed "mirror" neurones in the brain may be responsible. These nerve cells fire when a person makes a movement or watches another individual performing the same movement, so it may be that the reflected image fools these cells into responding as though the amputated limb were still present, altering the pain perception.

Minty fresh magnolia
Researchers have found that the key to fresh breath might lie in an extract of magnolia bark.
 Michael Greenberg and his colleagues found that, in the test tube, two key chemicals in the bark, magnolol and honokiol, could kill more than 99.9% of the mouth bacteria that cause bad breath in just 5 minutes. To find out whether the extracts could also work in the mouth the researchers collected saliva samples from 9 volunteers 1 hour after lunch and then at 30 and 60 minutes after eating a mint laced with the chemicals or at 40 minutes after chewing a piece of chewing gum containing the same chemicals. In separate trials the subjects also chewed control gum and mints that did not contain any magnolia extracts. The saliva was then incubated on bacterial growth media and the numbers of bacterial colonies that grew were counted.
Michael Greenberg and his colleagues found that, in the test tube, two key chemicals in the bark, magnolol and honokiol, could kill more than 99.9% of the mouth bacteria that cause bad breath in just 5 minutes. To find out whether the extracts could also work in the mouth the researchers collected saliva samples from 9 volunteers 1 hour after lunch and then at 30 and 60 minutes after eating a mint laced with the chemicals or at 40 minutes after chewing a piece of chewing gum containing the same chemicals. In separate trials the subjects also chewed control gum and mints that did not contain any magnolia extracts. The saliva was then incubated on bacterial growth media and the numbers of bacterial colonies that grew were counted.
The results were impressive. The mints reduced salivary bacteria by 62% at 30 minutes and 33.8% at 60 minutes, whilst the chewing gum cut bacteria by 43% at 40 minutes. By comparison, the placebo mint cut bacterial levels by 3.5% at 30 minutes and increased bacteria by 50% at 60 minutes. The placebo chewing gum cut bacteria by 18%. The researchers point out that this could represent an effective way to cut oral bacteria without the risks of side effects and "rebound halotosis" (subsequently worse oral malodour!) associated with other breath-freshening strategies. For instance, triclosan has been found to react with chlorine in drinking water to form toxic substances, chlorhexidine-based solutions have been found to stain teeth, whilst alcohol-based rememdies can dry the mouth and make the problem worse. The team behind the results are based at Wrigleys, so it shouldn't be too long before magnolia gum hits the shelves; but whether it will stick's another matter.
16:01 - Herpes at the root of Alzheimer's?
Herpes at the root of Alzheimer's?
with Professor Ruth Itzhaki, Manchester University
Sadly, dementia's a disease which is found in increasing numbers of people these days. It shows itself in lots of different forms from what's called mild cognitive impairment, which affects memory and language, to more ruthless things such as full-blown Alzheimer's disease which can affect daily lifestyle very severely. Scientists have been looking into Alzheimer's disease for decades and trying to figure out just how it happens. There's one group based at the University of Manchester that have uncovered one aspect of it that could lead to its prevention. Meera Senthilingam has been finding out how...
Meera - Alzheimer's is a form of senile dementia and it's very common. In fact, one person in five over the age of 80 develops the condition which causes memory loss, sleep disturbance and personality changes. Patients with the disease show accumulations in their brain with an abnormal protein called beta-amyloid and this is thought to be toxic to the nerve cells: triggering the disease.
Scientists still don't understand exactly what causes the build up of this pathological protein in the first place. In recent years they've shown that the disease does have a genetic basis but they also suspect there might be another player involved and that's the herpes simplex virus or HSV. Surprising as it sounds 80% of us are infected with this virus which usually causes cold sores. What's unusual about HSV is that once you're infected the virus remains in your body for life. It hides inside nerve cells as a tiny piece of DNA which can periodically reawaken to control the production of new virus particles that then leave the nerve to produce infectious cold sores. Occasionally the virus can also invade the brain, causing a condition known as encephalitis. Professor Ruth Itzhaki from Manchester University thinks this might provide us with the clue to how Herpes Simplex is linked to Alzheimer's.
Ruth - The main reason was because in the very serious, rare luckily, illness called herpes simplex encephalitis the virus destroys the same regions as those that are mainly affected in Alzheimer's disease. Another point is that once people get infected it stays in the body throughout life so it's in a position, possibly, to do harm in old age.
Meera - When it comes to herpes simplex virus, how does it get into our body? How does it infect our body and how does it work?
Ruth - The main route it takes is transmitted in saliva and probably kissing and so on. Infants are kissed often and it probably then enters the body and travels in and eventually ends up in what's called the peripheral nervous system. This is the part of the nervous system other than the brain and the spinal cord. It stays there for life.
Meera - Once it's in the body what then causes it to become active?
Ruth - It's thought that it reactivates under conditions of stress or when the immune system is suppressed. A number of causes make it reactivate but I should say that when it reactivates it doesn't necessarily cause any harm in the people at all.
Meera - When research started being done into this connection what was found to connect them?
Ruth - The first bit of evidence was when we looked for the virus to find if it was present in brain, viral DNA. We found that it certainly is present in a high proportion of elderly people. That led us to continue with the work. Having found the virus was present in the brain we used other methods which suggested it had been possibly active in the brain and not active just once but maybe recurrently. We think it might cause a very mild type of disease like encephalitis. After that we discovered that it looks as if there's an association between the virus in the brain and a bit of the genetic factor, and it's the two together that we think cause the disease in about 60% of Alzheimer patients.
Meera - What's the genetic factor that you thought to link them?
Ruth - It's the type 4 form, so called 'allele,' of a gene called Apolipoprotein E which codes for a protein which is involved with carrying lipids, fats, in blood - in the brain.
Meera - How is this gene thought to work in order to aid herpes and the formation of Alzheimer's?
Ruth - We think it affects a degree of damage. It may be that there's an early entry of the virus into the brain but we think the main affect is that it affects the extent of damage there.
Meera - So you found this connection now, what next?
Ruth - We've recently been finding rather - I think a major finding - that looks as if the virus does actually cause the formation, or increased formation of an abnormal protein called beta-amyloid which is the main component of one of the abnormal features of an Alzheimer's diseased brain. We found the virus infection increases that in cells in culture in a mouse brain. It also, we found, even more strikingly in the sections of human brain post-mortem that it's located within these structures. We think this strongly implicates this in the formation.
Meera - In the grand scale of things is this going to lead to some kind of treatment? I've heard things about a possible vaccine. Is that likely?
Ruth - It is possible in the future but at the moment there's no vaccine for this particular virus. It's something that would have to be developed and would involve a very lengthy clinical trial. People would have to wait for many decades to see whether people do or do not develop the disease when they've been vaccinated. What is much more imminent and practical at the moment would be antiviral treatments which is available fairly cheap and could be used with rather minimal side-effects. It would be good because that the moment there's no real effective treatment against Alzheimer's.
Meera - So Ruth's team have found further evidence connecting herpes simplex virus to the onset of Alzheimer's disease but as she mentioned, there are still many other connections to be found. Teams of scientists across the globe are working in this field, hoping to find a treatment or preventative measure as such a large percentage of our population are affected by this form of dementia.
Why are my radio controlled clocks not syncronised?
We're actually not sure about this one!
Most radio-controlled clocks update themselves once a day, but cann't do so if they can't receive a strong enough radio signal. It's possible that one of the clocks has a weaker antenna, and so isn't receiving a signal, and has fallen out of time.
Please let us know if you can think of any other reason for this!

Is it harder to wipe boys bottoms?
We're not sure about this one, but we think it could just be that boys are better at making a mess!
If you've got a more helpful answer, please let us know!
Could mirrors help blind people with phantom limb pain?
That's an amazing point that you've made. I think it's one which, unfortunately, hasn't been considered in the present research. You're absolutely right, diabetes is the leading cause of sight loss in countries like this one and unfortunately because the trial they did involved people being able to see it would mean that people that have blindness from diabetes and had had an amputation would have a problem with doing this. It would be difficult. We therefore have to think, 'is there another way to do what they did?' It might be that there are ways of using various nerve stimulation to fool the brain into getting signals from the missing body part and that's definitely possible because a lot of the nerves that supplied the missing body part, the stumps of those nerves, may still be there. It might be possible to do that instead.
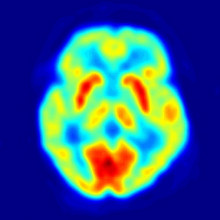
24:27 - Alzheimer's and the Brain
Alzheimer's and the Brain
with Dr Peter Nestor, Cambridge University
We're very fortunate to be joined by Dr Peter Nestor. He is from Cambridge University and he works on mild cognitive impairment and also specializes in Alzheimer's: investigating what brain processes occur to give someone the disease in the first place and how we can actually try and prevent it. Hello Peter!
Peter - Hi.
Chris - So if I was to do a brain scan on someone who had Alzheimer's disease, what would I see?
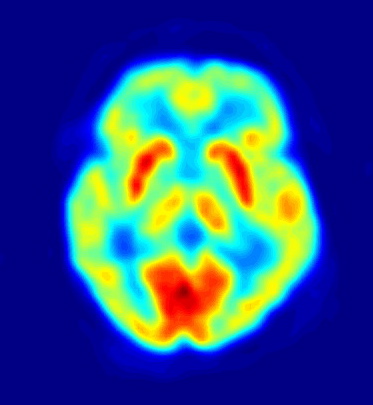 Peter - Well, it depends on the kind of brain scan. If you do a structural brain scan such as a CAT (CT) scan or an MRI scan, the answer can be not very much. There's shrinkage of the brain and particularly certain areas such as the hippocampi. However, our brains shrink as we get older so it's not such a great discriminator. If you do functional brain scans such as a PET scan (positron emission tomography) and look at brain metabolism then you typically see reduced brain metabolism in areas of what we call polymodal association cortex - particularly around the back of the temporal lobes and parietal lobes.
Peter - Well, it depends on the kind of brain scan. If you do a structural brain scan such as a CAT (CT) scan or an MRI scan, the answer can be not very much. There's shrinkage of the brain and particularly certain areas such as the hippocampi. However, our brains shrink as we get older so it's not such a great discriminator. If you do functional brain scans such as a PET scan (positron emission tomography) and look at brain metabolism then you typically see reduced brain metabolism in areas of what we call polymodal association cortex - particularly around the back of the temporal lobes and parietal lobes.
Chris - What do those bits of the brain do?
Peter - Lots of different things. Interestingly, given that the key deficit is memory impairment or amnesia with Alzheimer's those particular areas that we see easily on the brain scan are not so important for memory. Other areas that are important for memory such as the hippocampus and an area we've been doing a lot of work on called a posterior cingulate cortex are important for memory. Of those the posterior cingulate seems to become dysfunctional first of all, at the start of the illness.
Chris - There are lots of different diseases though, that constitute senile dementia, aren't there? We tend to use an umbrella terms and say, 'this person's got dementia,' or lots of people say, 'this person's got Alzheimer's,' but can you see differences between these different diseases on your scans?
Peter - Yes, you can. You're absolutely right. Dementia is just a generic term for losing mental abilities and obviously that can be due to all sorts of pathological processes of which Alzheimer's is the most common. But other common dementias include what's called 'Dementia with Lewy Bodies' or Fronto-Temporal Dementia. They tend to have different signatures in terms of the location, the topography if you like, of the damage in the brain.
Chris - Presumably as we get better at spotting these disease early and come up with treatments it will become very important to be able to discriminate between them because you can put someone on a certain drug and therefore, if you know what the disease is in the first place, you can get the drug right and slow the disease down.
Peter - Yeah, that's absolutely right and it's a very important point. It's a very important point because of trial research because obviously one doesn't want to include people with the wrong kind of pathology if your therapeutic agent that you're experimenting with is thought to work on a particular pathological pathway. Having people with the wrong kind of dementia syndrome in the trial is a big problem. That's a major incentive to work at the moment.
Chris - We've mentioned some of the symptoms and signs of Alzheimer's disease so far but what are the cardinal features of people who are going to get the disease tend to show?
Peter - Well, the hallmark is memory impairment, forgetfulness, which brings up this term you mentioned earlier, 'cognitive impairment.' This is this isolated memory impairment. There's a sort of a programme which can last for many years where someone has memory problems without having impairments in other mental abilities such as language or spatial abilities and so forth. Ultimately those other things do catch up with the patient. As the disease progresses one gets impairments in all mental abilities but for a long time it's just focussed on memory.
Chris - So, as we become better at working out what these things are and who's got what disease what are we going to do about trying to treat people? Are we at any stage where we can intervene in these disorders?
Peter - Well, there's nothing that's available yet as a treatment that's been proven to work but there are a number of trials underway. I think you mentioned before in the previous article about vaccines and one strategy that has been tried is to give a vaccine against those amyloid deposits, the cause pathology in the brain. The jury's still out on that. The first trial was stopped because one or two people had some quite severe side-effects from it. It's not really clear yet whether it may actually be helpful. That's one but there are lots of others that are trying to modify the sort of molecular pathology, if you like.
Chris - Do some of the drugs try to correct the chemical imbalance that you get in the brain? As far as we know people who develop Alzheimer's disease lose signalling from a chemical called acetylcholine and any of these drugs that you get given seem to boost that drug in the brain and can make people improve for a while.
Peter - Yes it's an interesting story, acetylcholine. That is the only drug that we have that as treatment for Alzheimer's at the moment but it's not a disease-modifying treatment, it's replacing the cholinergic activity. Interestingly, though it's been rather disappointing as a symptomatic treatment. Most people do find that it helps a little bit but it doesn't dramatically restore memory or anything like that. Interestingly, the work that was done that showed there was a cholinergic deficit in Alzheimer's disease over 25 years ago was done on end-stage disease (post-mortem brains of people who'd died at the ends of the illness). That showed the deficit. Recent evidence suggests that it's probably not a major feature of the very early clinical course of the illness.
Chris - So by putting people on drug that effect that, we might be barking up the wrong tree?
Peter - Well, it's a symptomatic treatment so it could be if someone has the deficit. Given that it's a symptomatic treatment and you're trying to improve someone's symptoms you can always give it a go. If it doesn't work you can stop it again. Interestingly though, another condition related to Parkinson's disease called Dementia with Lewy Body turns out to have a much more profound cholinergic effect early on in the illness. That condition seems to respond much more dramatically to cholinesterase that does Alzheimer's disease.
Chris - It sort of flies in the face of the fact that haven't the government been quite difficult to persuade that these drugs are good for people who have this condition? I know that people who care for people who have these conditions find these drugs very helpful.
Peter - Yeah. In the case of Lewy Body disease it's disappointing they haven't looked at that one because I think there is enough evidence now to say that's very useful. Certainly I know from my own practice of seeing patients that it can very significantly help. I guess with regard to the bigger issue of Alzheimer's disease one of the other problems we have is how does one measure accurately that there's been an improvement? I think one of the problems in the trials that the government have used for evidence is that they've used fairly old and antiquated methods of measuring cognition. It is sometimes those measures are somewhat at odds with what the actual families report. They do see some improvement but that said it has to be acknowledged that the improvements are not dramatic. It's a little bit of an improvement.
Chris - Just to finish off, what do you think the long-term effects are going to be here? We've got an ageing population, at the moment 1 person in 5, roughly gets Alzheimer's disease but there's going to be a hell of a lot more people over the age of 80 who are therefore in that risk group before too long. What's going to happen?
Peter - Well, yeah. It's a huge problem and a huge financial problem to say nothing of the huge distress it causes the families and patients. Yes, as the population ages the prevalence is going to go up and up. Already it's estimated in the United States that Alzheimer's disease costs more than all of cancer combined. If you factor in all the indirect costs such as needing to look after people, people needing to stop working to stay at home and care for someone and that kind of thing. Yes, that's an enormous potential problem for the future.
Can peripheral nerves regenerate?
This was asked along with Or's question:
The nervous system is divided into two camps. There is the central nervous system which is your brain and your spinal cord. Then there is the peripheral nervous system which is everything else. The central nervous system (the brain and spinal cord) if you injure that as far as we know, it's permanent. The nerve cells may die, they may not die but they certainly don't reconnect where they should connect. That stops signals getting through which is why you get problems of paralysis of loss of sensation depending on where the damage is. That's why a stroke is so disabling. In the skin the nerve cells there seem to be able to survive. They also seem to be able to re-grow their targets so they go back to where they should have gone in the first place. They reconnect to, if it was a muscle they were supposed to be supplying, they'll reconnect with the muscle. If it was a patch of skin they can branch out and re-supply the skin so you do get sensation back. Nerves grow quite slowly, probably a couple of millimetres a day. So if you've got a big injury the length of your arm it can take a few weeks before the nerves can get back to your arm. The sensation may not be absolutely perfect because some nerve cells might die but you should get coverage of the skin back afterwards.
What happens when you break the nerve the actual cell inside is just one massive long cell. The distal bit (the bit downstream of the cut site) will degenerate. It retracts and forms this little lump bulb. This thing grows back along the original path of the nerve so it uses the original pathway of the nerve as a guide. Rather like a motorway cone. It uses the cones and lays down a new road surface, which is the nerve, and it gets back to where it was supposed to attach. The distal site it was supposed to attach to switches on various markers so it can recognise it and off it goes!
Can nerves regenerate?
The nervous system is divided into two camps. There is the central nervous system (CNS) which is your brain and your spinal cord. Then there is the peripheral nervous system (PNS), which is everything else.
In the central nervous system (the brain and spinal cord), if you injure that - as far as we know - it's permanent. The nerve cells may die; or they may not die but they certainly don't reconnect with where they should connect. That stops signals getting through which is why you get problems of paralysis or loss of sensation, depending on where the damage is. That's why a stroke is so disabling.
In the skin the nerve cells there seem to be able to survive injury. They also seem to be able to re-grow to their targets so they go back to where they connected to in the first place. So if it was a muscle they were supposed to be supplying, they'll reconnect with the muscle. If it was a patch of skin they can branch out and re-supply the skin so you do get sensation back.
But nerves grow quite slowly, probably a couple of millimetres a day. So if you've got a big injury the length of your arm it can take a few weeks before the nerves can get back to your arm. The sensation may not be absolutely perfect because some nerve cells might die but you should get coverage of the skin back afterwards.
What happens when you break or interrupt a nerve is that the actual cell inside is just one massive long cell. The distal bit (the bit downstream of the cut site) will degenerate. It retracts and forms this little lump bulb. This then grows back along the original path of the nerve so it uses the original pathway of the nerve as a guide, rather like a motorway cone. It uses the cones and lays down a new road surface, which is the nerve, and it gets back to where it was supposed to attach. The distal site it was supposed to attach to switches on various markers so it can recognise it and off it goes!

37:04 - Earworms - Songs that stick in your head
Earworms - Songs that stick in your head
with Professor Daniel Levitin, McGill University
Have you ever had a song stuck in your head and you just can't shift it? Even if you don't like it, it's just stuck in your head. This week Meera has been finding out why this happens and just how music manages to worm its way into your head.
Meera - I'm sure you've all been walking along, say to the shops or to the park, and found you're humming a song. It could be the latest track by your favourite band or a song that reminds you of someone or something. Not only is this song currently in your head but you soon realise that you've been humming it all day, possibly even all week. To find out why songs and why music stays in our memory so easily I spoke to Professor Daniel Levitin from McGill University in Montreal, who's not only an expert in the field of music perception but he's also an ex-recording engineer and record producer. To start with I had to ask, 'why do our brains remember music so easily?'
 Daniel - In the jargon of our field I would characterise it as being constituted of multiply redundant, or reinforcing cues. What I mean by that is that if you're trying to remember the words there are a lot of things that constrain them. You've got the access structure, the melody, you've got a rhyming scheme. There are only certain words that will fit at the end of a line. In terms of melody, you may not remember all the notes of a melody. But if you remember the melody starts low and goes high, it might be going be-de-de-de-ri-naaaa [ascends to higher notes after a few beats]. You've got to get from one to the other, there's only certain notes that it could be. What we've learned about memory is that there's a certain aspect of human memory that's illusory. You don't remember every detail of everything. You construct some of the details at the moment of recollection. You fill in information that isn't actually in your memory with a plausible substitute. This happens all the time in music.
Daniel - In the jargon of our field I would characterise it as being constituted of multiply redundant, or reinforcing cues. What I mean by that is that if you're trying to remember the words there are a lot of things that constrain them. You've got the access structure, the melody, you've got a rhyming scheme. There are only certain words that will fit at the end of a line. In terms of melody, you may not remember all the notes of a melody. But if you remember the melody starts low and goes high, it might be going be-de-de-de-ri-naaaa [ascends to higher notes after a few beats]. You've got to get from one to the other, there's only certain notes that it could be. What we've learned about memory is that there's a certain aspect of human memory that's illusory. You don't remember every detail of everything. You construct some of the details at the moment of recollection. You fill in information that isn't actually in your memory with a plausible substitute. This happens all the time in music.
Meera - What about those irritating songs that stay in your head no matter how hard you try to throw them out? You know the ones I mean!
Daniel - There's a word for this. They're called 'earworms,' like those little insects that burrows into your ear canal and you can't get it out. They tend to be simple melodically and rhythmically. They tend to be the kinds of songs that the popular radio stations play and overplay. So they get stuck in there and you can't get them out. Most people aren't running around with Stravinsky in there, they're running around with Who Let the Dogs Out or, what I've had stuck in my head for the last week which is, Crazy by Patsy Cline.
Meera - Crazy isn't a bad song to get stuck in your head. I get far more annoying things like the Flintstone's theme. Can you imagine how irritating that is? Playing like a broken record in your head all day long? I had to ask him if there was a cure.
Daniel - There absolutely is! You just think of another irritating song and it pushes the first one out.
Meera - Great (!) That's not really a cure though, is it? Well, if these earworms insist on staying in our heads please tell them they serve at least some kind of purpose.
Daniel - This is a key to the evolutionary origins of music. The idea is that if a song gets stuck in your head maybe it has some evolutionary reasons to do so. Some of the anthropologists I've spoken to have told me that in certain societies this is a part of courtship. A young boy will sing a song to a young girl. The idea is a song is supposed to get stuck in her head. When he's away on the hunt, she'll remember him. They can encounter each other in the reeds for example, and he can whistle the song and she'll know it's him. Then they can go off and do whatever they do.
Meera - Hmm. So to woo your next potential partner, seems you should compose and sing them the most irritating song you can come up with. An infallible plan, I'm sure!
What is glaucoma and how do you get it?
The answer to this is it's not something you can catch, fortunately. Glaucoma seems to run in families. It's caused by a raised pressure inside the eye. At the front of the eye you produce fluid and this fluid fills the front of the eye and it then gets reabsorbed further back in the eye. The fluid's continuously being replenished. Sometimes in people with glaucoma, they don't reabsorb the fluid properly and so the pressure can go up. This puts pressure on the retina, the part of the eye that converts light into nerve signals that the brain can understand. Over time this can damage the retina. In particular, it damages the part of the eye called the optic nerve.
All of the information that the retina sends to the brain, it does so along the optic nerve. There's about a million nerve fibres in the optic nerve on each side. They run through this structure called the optic disc at the back of the eyeball. You can see this in people's eyes who have raised pressure; you can see the changes that are very characteristic in this optic disc. If you reduce the pressure with drug then what this does is reduce the severity of those changes. If you catch it early and take drugs you can prevent any damage from happening. Depending upon when you catch it then there can be more or less damage to the eye.
The optic nerve is part of your central nervous system and if you damage the central nervous system then it doesn't grow back. If you lose a connection or some of the nerve fibres from your retina to your brain then you do lose acuity: the ability to see as sharply as you once did. The longer a problem goes on, the worse it can be. If you have a family history of glaucoma then it's worth going and seeing an optician just to get checked out.
43:00 - Memories, true and false...
Memories, true and false...
with Dr James Ost, Portsmouth University
We've heard about the effect of Alzheimer's on memory, but what actually is memory? How does our brain create a memory, and how can it go wrong? Dr James Ost, from Portsmouth University tells us more...
Chris - What is memory and how does it work?
James - That's a tough question! Essentially there are a number of ways you can think about memory. Some people think of it as kind of store in our head where we put facts and things to retrieve at a later date. Much like you'd put in books. Other people think of memory more as a sort of tool we use to help us get around the world. We use memories or stories to remind us how we got where we are and where we're going next. There are a number of different ways the psychologists certainly think about memory. There's not a kind of clear answer to that one, I'm afraid.
 Chris - Put simply, you take information into your brain and it's in some way converted into connections between nerve cells.
Chris - Put simply, you take information into your brain and it's in some way converted into connections between nerve cells.
James - You can think of it like that. That's certainly one way of doing it at a reductionist level.
Chris - When you get the memory back, effectively are those nerve cells recreating or replaying in you brain the sensation that the original experience would have given you? Is that how it works?
James - No. That's a popular view. That's referred to as a 'video player' analogy. In some cases, say if you're retrieving facts or things you've rehearsed an awful lot, then yes indeed it would be like the kind of nerves replaying. For more complex things like autobiographical memory: memory from episodes in your life and things like this we know that memory isn't a literal replay at all. In fact, as the previous guest was speaking about in terms of musical memory we know that memories are a kind of reconstructive process. We fill in lots of gaps as we go along.
Chris - How do you know what we're filling in? That's a really interesting point, isn't it? People think that their memory's infallible. A lot of people think their memory's infallible and we think this is what I remember so it must be true. How do you work out how much the brain's filling in the gaps for you?
James - You basically have no idea. They've no clear way of knowing. Psychologists at the moment are looking at a number of techniques to see if there are any clear markers of what one might call true markers of recall verses or what one might call false recall. Even at that psychophysiological/cellular level it's almost impossible to distinguish these things. People have looked at people remembering real things and people remembering imaginary things and eventually moved their brain wave if you like: compared the two. Any differences are very, very short-lived and disappear within a matter of seconds.
Chris - How do you define a false memory?
 James - Again, there are a number of takes on that. The term 'false memory' was coined by one of the fore fathers of psychology, an American guy called William James, way back in 1890. He was basically making the observation that a lot of us were relating memories that go wrong. We forget where we put our car keys and so forth. Real contemporary interest in that phrase, false memory, has only come about in the last 20-25 years or so in relation to cases of recovered memories in abuse or trauma in a child and things like that.
James - Again, there are a number of takes on that. The term 'false memory' was coined by one of the fore fathers of psychology, an American guy called William James, way back in 1890. He was basically making the observation that a lot of us were relating memories that go wrong. We forget where we put our car keys and so forth. Real contemporary interest in that phrase, false memory, has only come about in the last 20-25 years or so in relation to cases of recovered memories in abuse or trauma in a child and things like that.
Chris - There's an interesting study I read, James. About a year ago, scientists in America got a bunch of students and got them to fill in a questionnaire and said they were going to give them feedback on what they got from the questionnaire. Then they invented the feedback and gave the same feedback to every single student and told them when they were little some strawberry ice cream made them violently sick. They re-tested them later and a large number who had previously not reported any kind of allergy to strawberry ice cream then said that strawberry ice cream made them ill. It's almost as if the researchers had planted a false memory. How does that happen?
James - Again, that's interesting stuff. That kind of research I'm referring to is really at the forefront of research at the moment. How does it happen? Well, again what we know is that memory is a constructive process. It's not just like pressing play on your DVD and everything coming back. When we're asked to remember something we try to take information we do have to hand: bits of true memory, bits of things we've seen, bits people have told us and we weave these all into a kind of narrative if you like. When people suggest things like in the study you were referring to that as a kid you got sick eating strawberry yoghurt [ice cream - QED] it's partly woven into your autobiographical memory, your narrative. There is research that has shown that people are more likely to avoid strawberry yoghurt [ice cream] after receiving the suggestion but again, that is still in its infancy it's very interesting stuff.
Chris - Just to finish off, can you tell us, how does this impact on criminal proceedings? How do we know that someone's account in court is allowable?
James - That really is the $4m question! I think there's a lot of work over the last 5-6 years from the DNA exoneration cases and these are people, a lot of them on Death Row in America, later is turns out that DNA evidence shows they could not possibly have committed the crime. Researchers have looked back at those cases and found that in 80% of those cases with DNA exoneration the most convincing piece of evidence to the jury was the eyewitness testimony. That is someone saying, 'yeah it was definitely James, he was there. That's the feller.' These kinds of memory errors like forgetting your keys or forgetting where you parked your car, all these things really are the minor ones. They range on a full spectrum all the way up to these cases where people are being wrongfully imprisoned for things they haven't done. It is an important issue.

49:26 - Skydiving from Space?
Skydiving from Space?
We put this question to Dr Phil Rosenberg from the Open University, who worked on the Huygens probe:
"OK so our astronaut bails out of his rocket. What would happen then? Assuming he's in orbit around the Earth, actually not a lot! Both the astronaut and the rocket are in orbit around the Earth going at about 11km/s or 24,000m/h. They basically both orbit together. If the atmosphere there was a vacuum, there's no atmosphere at all then that would mean the astronaut would stay in orbit forever. It happens that there's a little bit of atmosphere up there. A tiny amount about a thousand, trillion, trillion times thinner atmosphere than there is at the surface of the Earth. That tiny amount of atmosphere will put a tiny bit of drag on the astronaut and as time went on that drag would slow the astronaut down. As he slowed down he would start to descend until eventually the atmosphere is thick enough that he could just fall to Earth.
Unfortunately, it's not great news for the astronaut because the atmosphere's so thin it would take him about a year to get slow enough that he would just fall to Earth. Because the astronaut's travelling so quickly, 24,000m/h, as he starts to slow down and go into the thicker atmosphere the friction caused by the drag will heat him up and burn him in the atmosphere. In order to avoid that essentially what you'd have to do is slow yourself down from that 24,000m/h to essentially 0. Even the shuttle can't do that at the moment. The shuttle has a special thermocoating on the underneath it to re-enter the atmosphere. As it enters the atmosphere, it's travelling at 17,000 m/h. Even the shuttle can't slow itself down enough. Having said that, the astronaut is a little bit lighter than the shuttle so a decent sized rocket engine will slow him down enough but unfortunately most astronauts aren't equipped with such devices.
Unfortunately for our stranded astronaut I think it's pretty close to impossible, or at least very difficult in our space suit that we have to survive re-entry. I think our astronaut's going to need some sort of escape pod or some sort of space vehicle to get back down form space to earth and survive the really difficult conditions that are involved in that." We also spoke to Cheryl Stearns, Pilot and record-breaking skydiver:
"You could do this if you're only going to 100-110,000 feet, that's a project that I'm working on right now. I'm not re-entering into the atmosphere. You can freefall from that altitude and you're going to get up to a speed of 900m/h but you will not feel that speed because the atmosphere is so thin. You'd only feel maybe 150m/h of actual wind resistance against your body. The outside layers of your suit would only be maybe 200 degrees temperature with the friction that you have in the thin air. So yes, that is possible to do, a parachute jump from that height, but definitely not possible to do a parachute jump or exiting out of a space craft. You'll never be able to enter back in."
- Previous Naked Science Q & A Show
- Next Science in South Africa Special











Comments
Add a comment