Behind Blood donation
For World Blood Day we've been delving into the history of blood letting, getting stuck into blood donation and exploring exciting new possibilities for making blood that's safe for everyone. Plus, a new test to reveal every virus infection you've ever had, the LHC fires up again after a two year shut down, and a new weapon in the fight against Ebola...
In this episode

00:58 - Firing up the Large Hadron Collider
Firing up the Large Hadron Collider
with Mike Lamont, CERN’s Head of Operations
The world's biggest particle accelerator - the Large Hadron Collider (LHC) - has  been successfully restarted this week after a two year maintenance shut down. Now it's back to smashing together protons, the positive particles that sit at the centres of atoms, to help scientists glimpse what the Universe is made of. Graihagh Jackson went to CERN to meet the LHC's Head of Operations, Mike Lamont, to find out more about the next run of tests...
been successfully restarted this week after a two year maintenance shut down. Now it's back to smashing together protons, the positive particles that sit at the centres of atoms, to help scientists glimpse what the Universe is made of. Graihagh Jackson went to CERN to meet the LHC's Head of Operations, Mike Lamont, to find out more about the next run of tests...
Mike - The LHC is 27 kilometres in circumference and it's divided into 8 sectors. The first stage is to actually cool the magnets down. So, unless the magnets in the LHC are superconducting, they're cooled to 1.9 Kelvin.
Graihagh - Pretty cold.
Mike - Chilly! This is colder than outer space. Once the whole sector is cold then we can start putting current into the magnets and making sure that the magnets behave properly.
Graihagh - And then what's involved after that?
Mike - Our main magnets are the dipoles. These are the big guys which are bending and focusing the beams. These all have to be tested. The whole process for the whole machine lasted about 6 months to check out all the magnetic circuits. So, this is a huge, hundreds of thousands of tests. So, once that's done over the full 27 kilometres then we're in a situation where we think we start taking beam.
Graihagh - When you say 'take beam', what do you mean?
Mike - The protons come in bunches. So, we group the protons together. A bunch is about 30 centimetres long and typically about a millimetre in transverse dimensions. So, you think about a long thin worm. We're going to put 100 billion protons into each bunch and then spread out a lot of bunches around most of the LHC's circumference and that's what we call the beam.
Graihagh - And you're accelerating these round and then I suppose, you choose exactly where they collide. How many protons are actually colliding every single rotation?
Mike - So, the total number of protons in the beam is astronomical. We're talking like 2 x 1014. The number of collisions we generate a second is in the order 600 million which is actually quite a small proportion of the total number of protons circulating.
Graihagh - It sounds like a pretty good number to me. How can you keep track of all of them?
Mike - We got some rather cute beam instrumentation which measure the number of protons we have in the beam and where they're all going. We have to be very, very careful about not losing these guys because they have very high energy and they can damage the magnet. So, we have to be very careful about beam wrangling if you like and keeping control of all these protons.
Graihagh - Tough job.
Mike - Somebody has got to do it.
Graihagh - So, now that we're ready to go, we're going to be seeing the first few experiments in the next coming days, what can we expect for scientists to be looking out for in the next run?
Mike - So, the key thing about this run, run 2, we're starting now is, we can now take the protons to a higher energy. So rather than 40, at the end run 2, we're not going to 6.5 TeV. TeV is what we call a terror electron volt. On a terrestrial scale, this is about the same as a house fly, flying at a couple of miles an hour.
Graihagh - A house flying!
Mike - A house fly.
Graihagh - Oh a house fly! I was trying to imagine.
Mike - We've got strange analogies, but not a flying house, a house fly.
Graihagh - So, a house fly flying at 2 miles an hour is the same as 1 TeV.
Mike - The exact numbers escaped me, but at that order. So, on a terrestrial scale, this is not a huge amount of energy but what we're doing is we're giving that energy to a minusculy tiny particle the proton or a particle physics scale is really is a lot of energy. This is opening up new territory for the physicists. One of the big hopes is for signs of something called 'supersymmetry' which will open up a completely new world of high energy physics if it's there. the interesting thing here is we're probing the way the universe is structured. If the universe has chosen not to use supersymmetry as a solution to its problems then it's not there. and that is a fact that we will have to face and you don't have to develop other theories to explain things like dark matter.

05:17 - The Higgs Boson Song
The Higgs Boson Song
with Domenico Vicinanza, Anglia Ruskin University
What could be a more fitting tribute to the 2012 Nobel prize-winning discovery of  the Higgs particle than a musical composition created by the collider itself? Domenico Vicinanza heads the Electronics and Sound Engineering Research Group at Anglia Ruskin University. He's used a process called data sonification to turn the measurements from the experiments that uncovered the Higgs Boson into a piece of music. He explained to Chris Smith how he did it...
the Higgs particle than a musical composition created by the collider itself? Domenico Vicinanza heads the Electronics and Sound Engineering Research Group at Anglia Ruskin University. He's used a process called data sonification to turn the measurements from the experiments that uncovered the Higgs Boson into a piece of music. He explained to Chris Smith how he did it...
Domenico - What we're listening to is the result of a process called data sonification and data sonification is all about making measurements into something audible. So if you like, it's like using notes and melodies represent data instead of using conventional points and lines.
Chris - Which data did you use?
Domenico - So, in this case, we used energy measurements that were taken by physicists in 2012. So, what we are listening to is the distribution of the energy going from really low to high energies when the Higgs was actually discovered.
Chris - I see. So, when you see a collision happen, those recordings that were made in the detectors at CERN, they've given you that data and you've done something to it to turn it into a tune.
Domenico - Exactly. What we did to the measurements was mapping them or basically associating to each single measurements in each single number a music note using an algorithm. So, a set of rules that are actually linking the data to the music notes and giving a melody.
Chris - There's only a small number of notes but the energy levels must have been a continuous variable. It must have been over a huge range. So, how do you turn something with many, many possible energies into a discreet number of musical notes?
Domenico - What we did was actually using a mapping process that was compressing the range of the energy variation to a certain number of octaves in music terms. So we had an orchestra, we had instruments really able to play really low notes like double bases, to instruments able to play really high pitch notes like flutes and piccolos. So, we decided beforehand what was our range or energy range in sonic terms in some way and we did the mapping.
Chris - You've got a real kind of orchestrated piece here though. It's not just individual discreet notes. So, how did you then add the extra layers of orchestration? Did you apply one rule for one set of instrumentation and another set of rule for another, and then get something that sounds good?
Domenico - That was indeed a possibility. So, what I prefer to do was taking the energy measurements and create one single long melody, really long one. And then I was listening to it and I was extracting pieces of this long melody that was sounding particularly nice. so, it was particularly suitable for an orchestration. As a composer, what I like to do was actually using the right pieces for the right instruments. So, I actually started working, trying to imagine how these little pieces could layer on top of each other. I work on my orchestration to tell a story. And the story I wanted to tell was how the discovery happened. So, working from low energy, low frequencies, double bases and Cellos at the beginning and having it building up with woodwinds and with horns, sustaining the melody and finally the big discovery.
Chris - Could you use the same technique to do other data? Presumably, you could.
Domenico - Indeed. So, data sonification is a really, really general technique. We can actually use it to represent whatever we like. For example, I was recently involved in a research actually using data sonification to help doctors to discriminate between healthy and potentially dangerous cells in cancer so actually using sound to discriminate between healthy and unhealthy situation.
Chris - Where previously, they would look down a microscope and try to discriminate visually, you would have a computer reader slide and translate what it's "seeing" into sounds and then the doctors using their ears to discriminate rather than exclusively their eyes.
Domenico - Exactly. The reason why we are doing that is because we believe that ears can be much better than eyes in discriminating anomalies and discovering patterns. So, in some sense, the hearing sense is a neglected one. Wwe are so much relying today on looking at graphs and looking at visual representation of information that we forgot that we can actually use other senses. Hearing is one of the best ones. We have one of the most complex way of detecting patterns embedded in our ears and we're not using it.
Chris - I suppose this is the audio equivalent of creating a graph. If I've got a complex series of numbers and I want to represent them in the way that makes them easier to interpret and to show what the trend is, I draw a graph. You're doing the same thing with music for big data sets.
Domenico - Exactly. What we are hoping to do is actually, using the natural capability of our ears in detecting trends and patterns and anomalies. One example I really like is when we think about a graph and we think about lots of points in a graph, sometimes it's really, really difficult to identify one misplaced point in a graph. If we think about a melody which has a lot of notes and really complex is quite easy actually to spot a wrong misplaced note in a melody. That's all because we are so good in detecting anomalies in patterns using our ears.
Hear the Higgs Boson sound-track composed by Domenico using data from the LHC
11:59 - Test for every virus that infected you
Test for every virus that infected you
with Stephen Elledge, The Harvard Medical School
US researchers have developed a new test which detects every virus infection you have ever contracted, using just a drop of blood! Humans can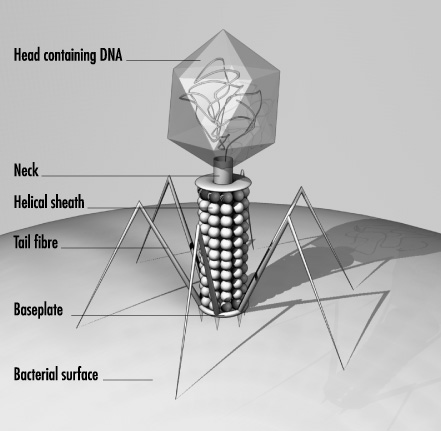 succumb to tens or even hundreds of viral infections over a lifetime. And although the majority are cleared by the immune system, certain combinations of infections earlier in life might alter your chances of developing other diseases later, like asthma, diabetes or cancer. So the ability to screen for every virus infection you've ever had could make a massive impact on our ability to diagnose, treat and predict disease. Chris Smith spoke to Stephen Elledge...
succumb to tens or even hundreds of viral infections over a lifetime. And although the majority are cleared by the immune system, certain combinations of infections earlier in life might alter your chances of developing other diseases later, like asthma, diabetes or cancer. So the ability to screen for every virus infection you've ever had could make a massive impact on our ability to diagnose, treat and predict disease. Chris Smith spoke to Stephen Elledge...
Stephen - People are infected with viruses all the time. Your immune system is what keeps you healthy and keeps the virus from killing you. Every time you get infected with the virus, it leaves an indelible mark on your immune system, a memory. We were interested in trying to measure this memory. The way that we were doing it is that your body makes antibodies to viruses. We wanted to take antibodies out of people's blood and develop a method that will allow us to determine which viruses those antibodies recognise. That will tell us what viruses you've been infected with throughout your life. Not only did we want to be able to do that but we wanted to do it for all viruses at one time. So, we could look at over a thousand human viruses in one experiment and tell you which ones you've been infected with because your body continues to make antibodies to a virus even after the virus is gone.
Chris - How do you assemble such a massive repertoire of tests to pick up all of those different antibodies that say, I will have made and assembled during my 40 years so far of interacting with the microbial world?
Stephen - Recently, it's become possible to make various pieces of viral DNA that encode the proteins the virus needs to grow in people. It's these proteins that your antibodies detect. Since we were able to take the DNA from the sequences of all known viruses, we could make bits of each protein for each virus. And we could display that in a way that we could figure out which bits your antibodies recognise.
Chris - How do you tell which antibodies are reacting with which bit of which virus?
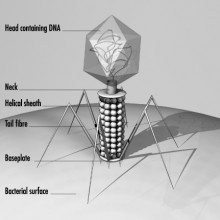
Stephen - We take advantage of something called a bacteriophage, which is a virus for bacteria. We can insert any piece of DNA we want into those viruses. So, we could, for example, insert a tiny bit of human virus DNA into the bacteriophage. The bacteriophage builds a little house that encapsulates its own DNA. The proteins on the outside of the house, we can have our little bit of viral protein fused to it. So, it decorates the house. Then, an antibody can recognise that and we have special magnetic beads that will then purify the antibodies away and if they happen to have touched a particular house, it will bring with it its own DNA and then we can just sequence the DNA. That all sounds very complicated but in fact, it's really simple.
Chris - I get it. So, because these individual little bacteriophages - these viruses that prey on bacteria - because you're decorating each of those to have a specific marker corresponding to an antibody which I have made when I responded to a certain virus in the past, any time those antibodies bind to one of those bacteriophages, and because the genetic message in the bacteriophage is unique to that particular one, you can easily pull it out and say, "we know which antibody it was that bound onto you, and we can therefore work out which antibody Chris has got in his bloodstream."
Stephen - That's exactly correct and you said it much better than even I can!
Chris - I was lucky, wasn't I? So, what are the implications of this then Steven? It's all very well to say, well, you can make these incredible deductions about what has happened to me as I've gone through life and interacted with what must amount to thousands of virus infections. But why is this useful?
Stephen - This is useful because you can now look at all viruses at one time instead of one at a time which is what people do now. They have to guess you might have been infected with a virus and say, "Okay, check for that one." A lot of viruses - HIV for example or hepatitis C can go unnoticed for a long time, unless someone suspects you've been infected with one of those, they won't even look for it. You can imagine that if there's a simple test that eventually makes it into the clinic that looks at all viruses at once, it could be part of a normal yearly visit to the doctor. We only need a drop of blood - a pin prick will do it - then you could have all of your viruses examined at that time and if you happen to have something that's not good, you can get treatment for it. There are millions of people right now who are chronically infected with hepatitis C and do not even know it.
Chris - But it doesn't tell me anything about when in my life, what age I was when I caught whatever infection because I suppose if one wants to ask, "When did you have infection X" because we're interested in how time relates to different infections occurring at different ages because the impact on your health could be different at different ages, couldn't it? It doesn't really give us any insight into that, does it?
Stephen - No. It could be 2 weeks ago. It could be 2 years ago. It could be 10 years ago. But whenever you find it, you can treat it.
Chris - Stephen Elledge. He published that work this week in the journal Science.

17:50 - How sitting harms your health
How sitting harms your health
with John Buckley, Chester University
Are you sitting comfortably? If so, you might want to stand up, because  according to many recent headlines, the sedentary lifestyle is harming your health. Some businesses are even installing "standing desks" and scheduling "walking meetings" to combat the risk. But what are the facts? Georgia Mills spoke to John Buckley from Chester University, who has been looking at the evidence...
according to many recent headlines, the sedentary lifestyle is harming your health. Some businesses are even installing "standing desks" and scheduling "walking meetings" to combat the risk. But what are the facts? Georgia Mills spoke to John Buckley from Chester University, who has been looking at the evidence...
John - Well most people spend 70 per cent of their waking hours actually sitting down. So, a group of us from around the world have collected up information along with some of the larger observational studies that they've taken on people who have had standing jobs. So for example in Canada, a Canadian fitness survey looked at people's different occupations and followed them for a number of years - 13 years, in fact - and looked at those occupations where people are predominantly sitting and people predominantly standing and showing a clear link that as people stood more in their day, they had fewer instances of early death or heart disease, diabetes and some cancers.
Georgia - Why is sitting down so bad for you?
John - Well, you're not using your muscles at all really. As soon you engage your muscles, then your body obviously has a small physiological challenge to maintain that posture. So, as soon as you're doing a little bit of work, everything is elevated. The whole system is like breathing, just like the heart, metabolism is raised. And all those factors are just working the system a little bit all the time, making sure your blood sugars are operating at the right level and taking up little bits of fat, a little bit of cholesterol, in very small amounts if you extend it over a long period of time. We're thinking that, that is probably why these things are related to better health outcomes because the body is designed to be active and moving.
Georgia - I am one of these people who spends a huge amount of time sitting down at my computer. What should I be doing?
John - The ultimate option is you get a sit / stand desk so that you could raise your whole desk up and you could stand and work at it for a number of hours, 3 to 4 hours in the day but you don't have to do it all at once. If you haven't made that investment, then to make sure that throughout the day, you are actually getting up on your feet for at least 5 minutes to 10 minutes at a time and that could be like what we're doing now. We're having a discussion on the telephone and you're recording this, so you're not having to write anything down. So, there isn't any reason why we can't be having this meeting standing up.
Georgia - So, should I stand up?
John - Yes.
Georgia - Okay, I'm going to raise the microphone up and I'm going to stand up and now, I'm less likely to get cardiovascular problems.
John - Well, if you did this for the next 20 minutes, 3 or 4 times in the day because I'm sure you have opportunities during the day where you've got these blocks of 20 minutes when you can actually do this.
Georgia - How much time in total and how often should we be trying to stand up?
John - Well, that's the million-dollar question with all of this, but looking at the current evidence, it looks like people need to do 2 or more hours per day if you're an office worker. And the benefits really show a lot of difference when people are doing 4 or more hours per day.
Georgia - That's a huge amount of time. I'm sure many people will be thinking, "This just simply isn't feasible for me."
John - It depends how you achieve it. We're going to have this discussion for 20 minutes. How many of these discussions do you have in a day?
Georgia - I'm on the phone quite a lot.
John - Okay, so why can't you spend most of the time - you could walk around even by having discussion on the phone.
Georgia - Is just standing up enough or do you have to move around as well?
John - The data that we have from people who were just doing sort of standing up interventions, it looks like they're having to do sort of more than 5 minutes at a time.
Georgia - Earlier, you mentioned standing desks. Is there any evidence that these are really good for you and can improve your healthy?
John - Yes. We're seeing amazing changes to people's energy expenditure, to their changes in blood glucose, and even starting to see changes in people's productivity and their alertness as well.
22:01 - Breaking Ebola transmission chains
Breaking Ebola transmission chains
with Ian Goodfellow, University of Cambridge
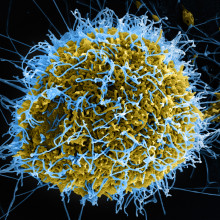
Although media coverage has decreased, the Ebola crisis that dominated the news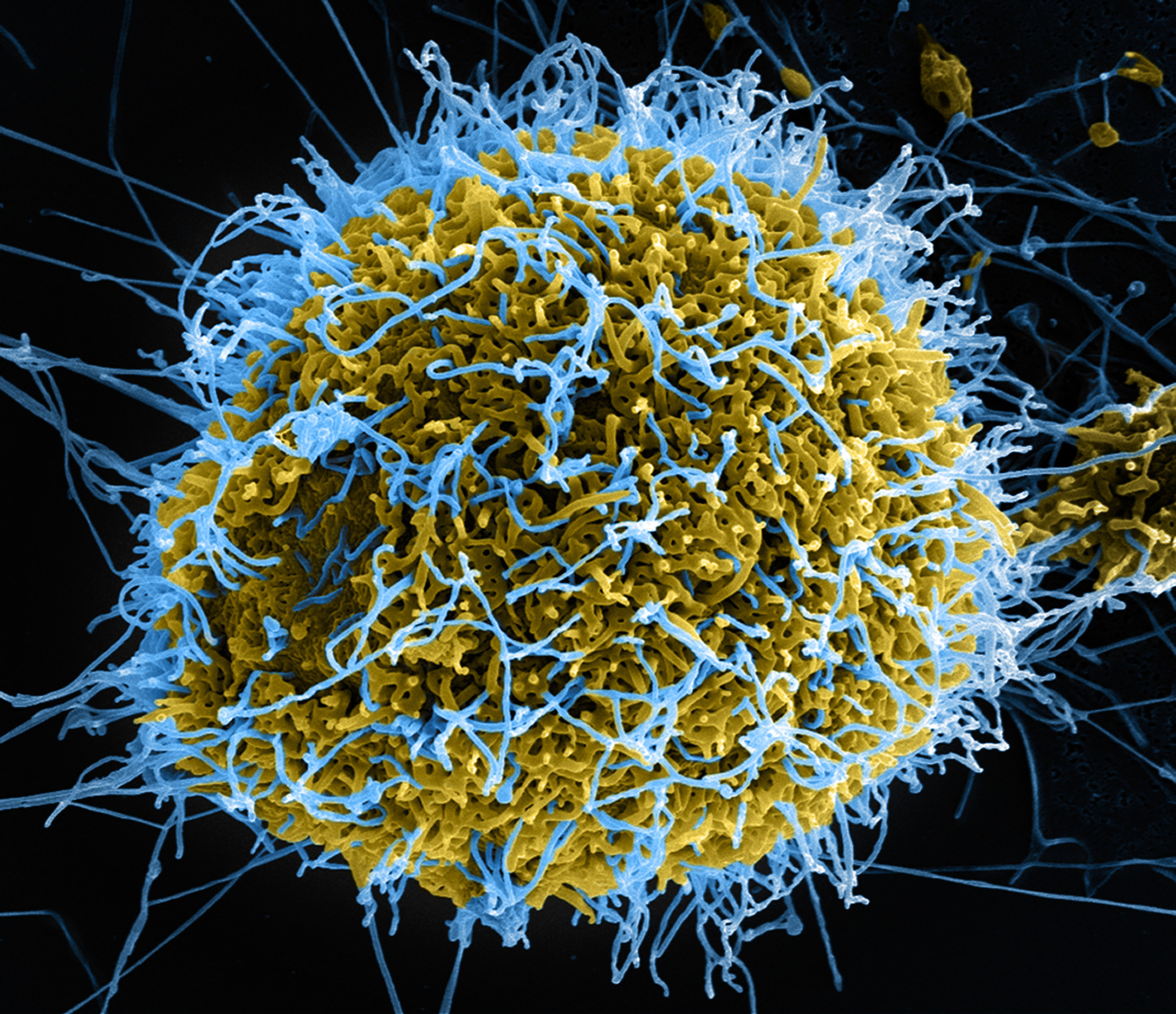 across much of last year hasn't actually ended and there are still cases being declared. Now scientists have a new weapon to break the so called transmission chain of ebola and that's a DNA sequencer. Cambridge virologist Ian Goodfellow has been in Sierra Leone where he's installed this machine - in a tent - and it's reading the genetic information of viruses recovered from victims, enabling scientists - and the government locally - to act more effectively. The first publicly-available data came off the machine this week. Previously, getting samples to analyse like this, was nearly impossible, as he explained to Chris Smith...
across much of last year hasn't actually ended and there are still cases being declared. Now scientists have a new weapon to break the so called transmission chain of ebola and that's a DNA sequencer. Cambridge virologist Ian Goodfellow has been in Sierra Leone where he's installed this machine - in a tent - and it's reading the genetic information of viruses recovered from victims, enabling scientists - and the government locally - to act more effectively. The first publicly-available data came off the machine this week. Previously, getting samples to analyse like this, was nearly impossible, as he explained to Chris Smith...
Ian - You have to get this material out of the country and you have two options. One is you take the actual infectious material out which has real challenges because the commercial flights won't carry it. Or you take the genetic material out and that has its other challenges because you need to be confident that you're inactivating the material. So, just the practicalities of getting the samples that have come out of the patients and physically getting them out of the country, getting permissions means that the whole process is slowed down.
Chris - So, how did you seek to address this?
Ian - The aim is really to try and put a machine that would allow us to determine the genetic sequence of these viruses in a treatment centre in Makeni. This is in Bombali District in Sierra Leone, in what really can only be described as a rather unconventional environment.
Chris - Just describe first of all, what do these machines that read genetic information look like?
Ian - It's probably the size of a reasonable-sized television, like a big box effectively. It just looks like a box with a whole bunch of tubes coming out of it. The machine we chose, we selected for a very specific reason and that was because we felt we could operate it in that environment. We needed something that's going to be able to cope with the temperature, cope with the humidity, cope with the dust, the insects that are crawling around the inside of the tent.
Chris - And the data is now coming off of the machine is it? You're getting sequences now from this machine.
Ian - We are getting sequences. One of the big problems we faced is getting the data out. Here in the UK, I have a superfast broadband which means I can send large files across from here anywhere in the world very, very quickly. In Sierra Leone, we're trying to move somewhere in the region of 5 gigabytes of data per run of the machine. We're doing this on a Wi-Fi dongle, so this is slower than the internet connection you will get from a mobile phone.
Chris - But critically, this means that now, you're literally testing the genetic sequence of Ebola that is infecting people and you can therefore marry up what the outcome was for that person where they'd come from in a country who they'd had contact with and perhaps whether or not those viruses spread. I presume you can begin to learn something about how the viruses behave based on their genetic information and how fast they're changing and so on.
Ian - The only way to be able to break transmission chains is if you know how that transmission chain is operating and there's clear evidence from the sequences we've released already that there's numerous viruses coming in from numerous examples of infected individuals getting viruses from Guinea. So, we're finding viruses in Sierra Leone that actually come from Guinea. That's despite the border being closed. Officially, that border is closed and there should be no movement of individuals across the border. But they're very porous borders and they're difficult to police. So, this gives you an indication that there is multiple incursions of Guinean viruses into Sierra Leone. This is something we need to be aware of and there are things that could be done on the ground with that information.
Chris - So, by reading the genetic information, you're actually learning quite a bit about what's happening politically or geographically in a country as well, aren't you?
Ian - We can, yeah absolutely. You can see our data would indicate that there's at least 12 independent transmission chains which are operating. Now, actually the government has done a fantastic job and many of those transmission chains we think are stopped. But if we see new cases appearing and anywhere in the country, we have a system set up now where the laboratory will phone the sequencing facility and we will go and collect that sample within 24 hours and sequence it. So, our plan is to make the sequences publicly available as fast as possible. We feel that it's important that this information is freely distributed to anyone who wants to see it or anyone who can analyse it because only by really opening up that data can you draw on the wealth of knowledge of people who are not able to actually go in country to do that sort of analysis. We can provide them with that data and they can use their expertise to analyse it. That analysis is then fed back to the public health people on the ground.
Chris - Is this the first time to your knowledge that somebody has put a sequencer that reads genetic data into a tent in an African country, not just for Ebola but for anything really and really broken this bottleneck like this?
Ian - I would hesitate to say that we're the first to do this. I'm not aware myself of anybody else with a sequencer that is on the ground. One thing we've learned from this outbreak, it's taken us 5 months to get to this point and that's too slow. We need the ability to have this equipment ready to be deployed into an outbreak situation. It needs to be there as soon as these sorts of outbreaks occur. It needs to be on the ground. We need to have people ready and trained to be able to get the data analysed and made available to the public health authorities.
28:15 - The history of blood letting
The history of blood letting
with Richard Barnett, Science Historian
Before blood transfusion got going, and the important role of the blood system was appreciated, doctors were more fond of taking the stuff out of people - and they had some pretty ingenious implements for doing so. Heather Douglas went to the Wellcome Collection in London to take a look at some, alongside science and medicine historian, Richard Barnett...
was appreciated, doctors were more fond of taking the stuff out of people - and they had some pretty ingenious implements for doing so. Heather Douglas went to the Wellcome Collection in London to take a look at some, alongside science and medicine historian, Richard Barnett...
Richard - We're here in front of three objects which point towards the most widely used medical therapies in history, which is bleeding. This is a medicine which is based on the idea of balance and the balance of four humours.
Heather - The idea of humours dates right back to the ancient Greeks. The theory goes that the body has these four disgusting-sounding liquids: black bile, yellow bile, phlegm, and, of course, blood. To keep healthy, they had to in balance...
Richard - Within this system, blood has a particular function. Blood is the nutritive humour. The idea is that blood is made in the liver and then sent out around the body and it carries food essentially and disease in this model is imbalance. You can have too much of a humour or too little of a humour. If you have too much of a humour, the doctor's job is to get rid of it and this is where bloodletting comes in.
Heather - Bloodletting wasn't the only way to balance the body, but it was an easy and popular treatment because everybody bleeds. It was so popular, that implements called scarificators were specially designed to get blood flowing. We took a look at some particularly gory ones.
Heather - There's one that's a metal box with blades sticking out.
Richard - Yeah, it's basically spring loaded - it's a bit like a pistol. You'd sort pull back a hammer, press it against the skin and press a trigger and steel blades would come shooting out of the skin.
Heather - That sounds horrible.
Richard - The other one is a razor crossed with a lawnmower and you sort of begin, run it along the skin and it would open up the skin and allow you to bleed.
Heather - It all sounds quite horrible to me. What diseases would they prescribe bloodletting for?
Richard - Pretty much anything. You would prescribe it for diseases where there was an excess of blood. If you have too much blood in your body, you get overheated, feverish, you get over excited. So, letting out blood was a way to sort of calm somebody down. Of course, if you lose 3 or 4 pints of blood, physiologically, you get calmer, to the point of unconsciousness.
Heather - How did we come away from this idea of blood coming from the liver and begin understanding blood?
Richard - It's not until the end of the 18th century that ideas about therapeutic bloodletting really start to change and that's with the revolution of medicine called Paris medicine. Doctors start thinking more surgical, they start thinking about fine little structure and the detailed anatomy of the human body. They start also to collect data on patients. One of the things that becomes very clear from this data is that therapeutic bloodletting has no effect whatsoever. This is where you start to get the idea of transfusion.
Heather - If you needed blood that stick needle in my arm with a tube and stick the needle in your arm and hope it flowed the right way?
Richard - Well, exactly. You have to be able to connect the pipes the right way around. But yes absolutely, a very simple and a very effective way especially on battlefields.
Heather - But they didn't start directly with human-to-human transfusions, did they?
Richard - Well, there was a long history of experimental transfusion looking back to the old classical idea of your humours determining your character. So, the idea was if you took blood out of a kind of angry vicious dog and put it into a sheep and vice versa, you might get an angry vicious sheep and a rather calmer, sheep-like dog.
Heather - Did they apply that to people as well?
Richard - There were some experiments with transfusing blood into criminals to try and sort of calm criminals. But the problem that all of these early transfusions faced was that very, very rarely, they'd work. There was really no sense of why this was happening until Karl Landsteiner who elucidates the blood groups.
Heather - So, he was the one who discovered blood types.
Richard - Yes. His work is part of a movement to try and understand the immune system and then the other functions of blood as well.
Heather - Once blood groups were discovered, it was recommended that people were tested before transfusion, which still happens today. But to start with, there was a problem of actually storing blood.
Richard - This becomes a real problem a few years after Landsteiner's work with the outbreak of the First World War. Suddenly, blood loss becomes a problem of selecting all of the blood European armies. It's discovered during the First World War, I think quite by chance, that mixing some sodium citrate into the blood stops it from clotting. So, you can start to store blood, you could start to build up blood banks. In 1939, at the outbreak of the Second World War here in Britain, you get blood banks set up in London and the blood transfusion service proves its worth during the blitz.
Heather - That was the real start of donation and people at home would go along then give their blood.
Richard - Yes. This is where scientific developments starts to mesh with cultural ideas. Here in Britain, ever since the '30s and the '40s, we've had this idea that blood transfusions are kind of civic duty. It's something you can do for society with the idea that if and when you need it, somebody else will be there to do it for you.

33:48 - Donating blood
Donating blood
with Jacob Grinfeld, Cambridge Stem Cell Institute
Around one in four of us will need a blood transfusion at some point in our lives, yet  only 4% of us regularly donate. But why is there this demand for blood in the first place, and how does the donation process work? Georgia Mills accompanied blood specialist - or haematologist - Jacob Grinfeld to the Cambridge Blood Donation Centre to explore blood groups and try her first donation...
only 4% of us regularly donate. But why is there this demand for blood in the first place, and how does the donation process work? Georgia Mills accompanied blood specialist - or haematologist - Jacob Grinfeld to the Cambridge Blood Donation Centre to explore blood groups and try her first donation...
Georgia - Right now, blood is coursing through your veins and arteries. It's transferring oxygen to your tissues and organs, and helping you to fight off infections. Your body is constantly replenishing your blood but due to illness and accidents, around 25 per cent of us will need to top up at some point in our lives. For this, we need someone else to donate theirs. To find out more about blood donation and to try and perform my social duty, I took a visit to Cambridge Donor Centre. There, I met haematologist Jacob Grinfeld who told me a little bit more about what it was that people were giving away.
Jacob - Broadly speaking, blood has 4 main constituents. There's 3 different sorts of cells and then there's the plasma which is the fluid that they swim in. Red blood cells give blood its red colour and they contain haemoglobin which carries oxygen throughout the body. There's various sorts of white blood cells but effectively, their job is to fight infection. Platelets are tiny cells that are involved in clotting the blood. The plasma transports lots and lots of different proteins, sugars, nutrients, and also carbon dioxide.
Georgia - Something you hear people say a lot about blood is they've got a specific blood type. What does this mean?
Jacob - What people are generally referring to are the ABO blood groups which refer to proteins on the surface of the red blood cells. There's 2 main proteins there, there's A proteins and B proteins. So, you can either have all A's, all B's, a combination of the two which gives you AB or you can have neither which means you have O blood.
Georgia - So, why does your blood type affect who you can and can't give your blood to?
Jacob - Everyone develops antibodies to the A and B groups. If you don't have either of them then you have antibodies to both A and B. If you lack A or B then you have antibodies to that specific group. This is important because if you give blood to someone who has antibodies against that blood, they immediately have a very dramatic reaction to that.
Georgia - These proteins on the blood cells act as sign posts. If the blood has a sign post that isn't recognised, things called antibodies go on the offensive, much the same way they would if a virus had invaded the bloodstream.
Jacob - So, what this means is group O blood is the best to give because it doesn't have any A or B proteins on the surface. You can give it to anybody which is why it's very important for hospitals to have a stock of O negative blood. So, in emergency situations, when you don't know what blood group a patient is, you're pretty much guaranteed that you can give them O negative blood.
Georgia - At the start of each donation, you fill out a health check and then get the iron levels in your blood checked via a simple finger prick test. If there's enough iron in your blood, it sinks to the bottom of a small test tube.
Donation assistant - This is where it would start sinking.
Georgia - We want it to sink.
Donation assistant - We do.
Georgia - Oh no, it's not sinking.
Donation assistant - And it hasn't unfortunately. So, it's just floated back up to the top.
Georgia - As you heard, I failed that test but my producer Heather passed with flying colours so I joined her in the donation hall.
Heather - Ready. It's going in. It's going to go in now. It's just like a little pinch.
Georgia - So, I can see they've got this little blood bag. Is this is your blood?
Heather - I hope so.
Georgia - It looks like there's already a liquid in the bag. What is this?
Jacob - That's citrate which is an anticoagulant.
Georgia - Why is this important?
Jacob - So that you could get the blood back out of the bag and it's not all clumped and in a lump.
Georgia - So, how are you feeling Heather?
Heather - Yeah, fine. This chair is really comfortable.
Georgia - Each donation takes under 15 minutes with some people being done in 4, but whatever the time, when you're done, there is a reward.
Heather, I see you're having your celebratory biscuit. How are you doing?
Heather - I'm really good. This biscuit is really nice.
Georgia - I wasn't allowed to give so I don't think I'm allowed one of these biscuits.
Heather - I asked and they said it's fine.
Georgia - Brilliant! I'm cheating the system.
While we ate our biscuits, some of them not quite earned, we met first time donor Anna.
How did it go?
Anna - Yeah. It was fine. I was really worried about the actual giving blood there but then that bit was easy. All the nurses were really, really friendly.
Georgia - Would you do it again?
Anna - Yeah. I feel really proud of myself. I've achieved something today.
Georgia - Heather and Anna were just two of the donors there last week. But I wanted to know what their blood will be used for.
Jacob - When we take the blood we actually break it down into its components. So, we can get from it red cells, platelets and proteins from the plasma. We use red cells for patients who have lost blood or can't make enough blood themselves. Similarly, we can give platelets for patients who have low platelet counts and therefore, have problems with blood clotting. Also, we use plasma which contains a lot of clotting proteins as well to correct problems with clotting.
Georgia - Can blood be used if someone has say, an accident on the road?
Jacob - Yes. So, that's obviously a source where blood will be in demand, people that have lost a lot of blood from accidents. As I mentioned before, that's where it's important to have a stock of O negative blood.
Georgia - But it's not just the rare O negative blood types that doctors are on the hunt for.
Jacob - In particular in Addenbrooke's, we have a lot of cancer patients and also do a lot of complex surgery including multi-organ transplants. So, there's a high demand for a range of different blood products. Currently, only 4 per cent of the eligible donor population in the UK are actually giving blood. So, we're always on the lookout for more new donors.
Georgia - Hopefully, that will be next time. I will donate in the future I've been given a little pamphlet and I'm going to eat spinach and kale and in 3 months' time, I'm going to give it another go.
Chris - I thought you're going to say "some iron supplements".
Georgia - I think there's a lot of iron in spinach, I was told.
Chris - But is it available because that's the point, isn't it? Lots of foods have got lots of iron in them but it's not in the form that you can readily absorb.
Georgia - I see. Apparently, as well, cups of tea inhibit your ability to absorb iron which I think might have been my problem. I overdose on tea daily.
Chris - Orange juice puts iron into a form which is efficiently absorbed. So, drinking a glass of orange juice with your spinach or whatever your source of iron is, your black pudding whatever you're going to eat. This increases the uptake in the gut. That's the best way to do it, actually. So, up your vitamin C intake because it keeps it in the form - in the un-oxidised state - that means it can be better absorbed.

40:32 - Making all blood universal
Making all blood universal
with David Kwan, University of British Columbia
In an emergency situation, when a blood transfusion can mean the difference between  life and death, there might not be enough time to test a patient's blood type. Under circumstances like these, the universal donor blood type (group 0 negative) that can safely be given to everyone is what's needed. But it's in short supply: only about 7% of the population have this blood type. Scientists at the University of British Columbia are tackling the problem by developing a way to turn blood of any type into the equivalent of group O negative, by stripping off the blood group markers, or antigens, from the outsides of the blood cells, as David Kwan explained to Chris Smith...
life and death, there might not be enough time to test a patient's blood type. Under circumstances like these, the universal donor blood type (group 0 negative) that can safely be given to everyone is what's needed. But it's in short supply: only about 7% of the population have this blood type. Scientists at the University of British Columbia are tackling the problem by developing a way to turn blood of any type into the equivalent of group O negative, by stripping off the blood group markers, or antigens, from the outsides of the blood cells, as David Kwan explained to Chris Smith...
David - The cells in your body, including blood cells, all display certain markers on their surfaces. These could be proteins or carbohydrates - anything that kind of identifies the cell to other cells in the body. The immune system is able to recognise molecules on the surfaces of the body's own cells, but if you introduced other molecules then the immune system will potentially attack these. This is the problem with transfusing blood of different types.
Chris - Your strategy is to say, "Well, if we can remove those markers from the surfaces of the cells we want to transfuse then the immune system would not have anything to recognise and therefore, it shouldn't react.
David - Precisely.
Chris - So, how on Earth can you remove those markers from the surfaces of cells?
David - We want to use enzymes which are like molecular scissors to cut off the antigen molecules from the surface of blood cells. Now, this idea has been around for some years, but the problem has been that the enzymes available have not been very efficient. So, what we wanted to do was to engineer these enzymes to better do the job.
Chris - Do these enzymes exist in the body naturally to strip off these antigens?
David - The enzyme that we have been working on comes from a pathogen. It comes from Streptococcus pneumoniae which is the causative agent of pneumonia. These enzymes chop off blood group antigens which are made up of sugar building blocks and this allows the organism to take up these and use them for its own food source.
Chris - What you're basically doing is stealing a pathogen's digestive system and you're going to use it to digest the antigens off of cells to make them more compatible for transfusion.
David - Exactly.
Chris - Why is the enzyme not good enough? Why can't you just use it as it is?
David - These molecules can be linked on to the cell surface in a number of different ways. It's very good at cleaving off the most predominant linkage by which these molecules, these markers, are presented on the cell surface, and that job is good enough for Streptococcus pneumoniae. But the immune system is very sensitive to these markers, and so, we need almost complete removal of them.
Chris - How can you improve on what nature has given you in the form of the enzyme from Streptococcus then?
David - To improve on nature, we take lessons from nature. We actually do a process called directed evolution to engineer this enzyme. We take the gene for the enzyme and we put it into another system that allows us to produce large quantities of this enzyme. Once we have the gene, we can mutate it and this gives us a population of different mutants. We select the improved mutants, take the genes of those and continue the process of mutation and selection to get the best mutants.
Chris - So, in a nutshell, you are introducing genetic spelling mistakes into the gene that encodes this enzyme and then you do trial and error, do any of those spelling mistakes actually make the enzyme much better at stripping off these antigens, and if some of them do, you take the best performing gene and then just keep repeating that process until you've got one that's really good.
David - That's right.
Chris - Does it work?
David - It does. We've been able to improve the efficiency of this enzyme 170 fold compared to the parent ancestral enzyme for cleaving a specific linkage that the parent enzyme had difficult cutting.
Chris - I'm sensing there might be a but coming here - does that mean that it does one of these antigens quite well, but there are others that you can't yet chop off with this enzyme quite so well?
David - You're right. Our enzyme is good at cleaving some of the linkages by which these antigens are linked to cell surfaces but not all of them and we're trying to improve that.
Chris - Does that mean then that you can do certain blood groups but not others or are you literally just at the stage where you can remove some of the antigen but not the whole lot? So it's not really ready even for one blood group quite yet?
David - The enzyme can completely remove the B antigen from B blood type individuals, but for the A antigen, it's not quite there yet. The problem is that there are many different ways by which the A antigen can be linked to cell surfaces and we can only cleave some of these linkages.
Chris - Have you actually demonstrated though that this blood, were it to be transfused having been stripped of its antigens using your strategy would be safe and wouldn't trigger a reaction if I for instance put group B blood treated in this way into a group A person?
David - Well, we haven't done the transfusion yet, but the typical clinical test for antigenicity of blood type B shows that these cells have the antigens completely removed from them.
Chris - How do you actually practically do this? Do you have a pot with some of this enzyme in and you just tip into the cells and let it work its magic, and then wash it off? Is that how it works?
David - Essentially, that's the case. We want to take the donated blood, add a few drops of the enzyme to it, let it sit for a few hours and then wash the enzyme away.
Chris - Do the cells tolerate this? Are they harmed in any way?
David - All these tests that we have done don't show any indication that the cells are harmed in any way by this.
Chris - That's very reassuring. How long do you think it will be based on the present trajectory before you've got something that you could consider for a clinical trial here?
David - Well, I can only give you an estimate but I'd say something like 10 to 15 years perhaps...
46:50 - Can we grow blood in a laboratory dish?
Can we grow blood in a laboratory dish?
with David Kent, Cambridge Cancer Centre
We currently face a blood shortfall, so why can't we just grow some blood in a lab? Chris Smith spoke to David Kent, from the Cambridge Stem Cell Institute, who is aiming to do just that. His idea is to harness the bone marrow stem cells that normally produce blood in the body and use them to make tailor-made blood products for each individual...
David - Blood stem cells are very rare cells in the adult bone marrow and they are ultimately responsible for the production and destruction of trillions of blood cells every day. So, quite potent cells, but as I said, quite rare, so difficult to find in adults, but when you can find them and you can manipulate the way they make decisions then you can start going down and making all of the different mature cell types in a blood system. So, all the red cells and platelets that are so desperately needed in the blood donation clinics.
Chris - You make it sound very simple. What's the stumbling block?
David - The big stumbling block is that there are many, many cell intermediates that these cells have to go through before they come from a stem cell all the way down to a very mature red cell.
Chris - You mean, they start off as sort of "baby cells" then they grow up into adolescent cells, and then eventually become young adults and then mature adults - that's where we want them, at the mature adult stage - but you've got to shepherd them through all those stages first?
David - Exactly and understanding teenagers, as we all know, is very difficult. So, trying to figure out what proteins are really directing the fake choices is what our lab really focuses on. And so, we try to understand at a single cell level how individual stem cells are making the decision to make a new stem cell or maybe go off and make one of the many different types of the blood system.
Chris - Is it just the way the cells talk to each other and how they send messages amongst themselves with protein signals and so on that's important, or is the physical environment itself important because obviously, when we look at the bone marrow, it's a 3-dimensional environment. You've got cells touching each other and communicating in 3 dimensions. A culture dish is often just two...
David - Yeah, absolutely and there are many groups sort of attacking this problem from many different ways. But on the bone marrow itself, there's a specialised area called the bone marrow stem cell niche and this niche is this place where all of the bone line in cells and all of this supportive cell types that feed the stem cells are located. There's been enormous amount of work on that. But in a culture dish, you can actually start to create these 3-dimensional micro environments as well. And so, there are many groups that have actually started to try and mimic what goes on in a bone marrow micro environment.
Chris - If you do that, do you start to get these stem cells to turn into the kinds of cells that we would need to produce - I don't want to say fake blood - but artificially produced personalised blood?
David - That would be one of the ultimate goals, is to really understand how a single cell makes that entire journey to mature red cells or mature platelets. There are also groups that are trying to do this even with the knowledge that we already have. So, we don't understand everything completely, but trying to give a best push at it. There's been some serious progress made. But the amounts required in an individual transfusion are quite enormous and scaling this up has been the big problem. So, that actually requires bioengineers to be thinking about things as well as biologists to really try and understand how we make blood products for everybody from these stem cell populations.
Chris - I read somewhere that it's about a million million cells every day that your bone marrow has to replace which are continuously just being thrown away because they've got old. So, we have to come up with a culture dish capable of the same incredible turnover that your bone marrow does.
David - Right. So, what we'd tried to do I guess in an ideal world is put in the sort of teenager cells so we wouldn't have to put in that enormous number of cells. We'd put in cells that could create that enormous number of cells over the lifetime of an individual. So, similar to how stem cell transplants work, when somebody has a full bone marrow transplant, the stem cells go in and setup shop as if they were indeed the local resident cells. And so, if you could get some sort of intermediate there, I think that would be quite a good way to go.
Chris - I suppose one problem is that when people come to hospital and they're acutely, urgently in need of blood transfusion, there wouldn't be time to do this. This is something longer term. So, you would presumably need to take from me a sample of my bone marrow in order to start your process and you're going to have to scale that up but in the meantime, I'm still going to need blood from somewhere.
David - Right and so, I guess the middle ground solution in that case would be to make unlimited supplies of A blood cells, AB blood cells, O blood cells, etc. and so, you can take individual donors, scale those processes up, make the mature cell types, store them all down so you have banks of blood cells that are made in this way, but not individually transfused back into the same person. So, you wouldn't have the need to wait that period of time outside the body.
Chris - Are we far away? How long do you think before we see on the shelves, blood that's tailor-made to an individual?
David - Well, I would say, in my own career, the rapidity with which sciences progress has been incredible especially in the stem cell field. And so, I think anything is possible but we're certainly 5 to 10 years away from seeing anything that's in a patient I think.
Why don't mothers reject their foetus?
A foetus is created from a mixture of its mother's and father's genes so the baby is genetically unique. So, what is it that protects babies from their mum's immune system. Ziyad Yehia asked Dr. Lucy Fairclough, an immunologist at the University of Nottingham, just how this works.
Lucy - The immune system normally functions to remove anything foreign from the body such as an infection. In the case of pregnancy, the mother's immune system will see the baby as foreign because the baby is genetically made up from the mother and the father. However, in most cases, the mother does not reject the baby.
Ziyad - What allows mums to put up with this alien life form inside of her for so long? Well, besides a lot of patience and random food.
Lucy - Well, at the side of the placenta, there is contact between the foetal and maternal tissues. But at the placenta, there is maternal tolerance of the foetal tissue despite these genetic differences.
Ziyad - I think a lot of expectant mothers would definitely say they tolerate a lot during pregnancy. Just how do they do it, Lucy?
Lucy - There are many mechanisms that help to maintain this tolerance. This can include the secretion of special proteins that suppress the mother's immune system or an accumulation of cells that regulate and keep the immune system in check. There can also be lack of other proteins that normally activate the immune system. All of these causes a local suppression of immunity during pregnancy that enables the foetus to survive even though it was genetically different than mother.
Ziyad - Sounds like mums got it covered, but nobody is perfect, right?
Lucy - There are some instances when the foetus may be attacked by the mother's immune system although this is not controlled by careful screening. There are many proteins expressed on the blood cells of the body and an individual's blood type is defined by some of these proteins. In the case of pregnancy, when the father's red blood cells express a protein called rhesus D, but the mothers does not express this rhesus D protein, the mother generates a molecule called an antibody that targets the foetus's red blood cells. This is called haemolytic disease of the new born. In most cases however, the red blood cells do express rhesus D, so this is a fairly rare occurrence.










Comments
Add a comment