We visit the annual British Society for Gene and Cell Therapy conference to explore the latest in this exciting area of medicine...
In this episode

01:02 - Other habitable planets?
Other habitable planets?
Dan - Well, the story I've got this week is about exoplanets - planets around other stars. There's an announcement this week that the Kepler satellite has discovered the best candidate so far for a habitable planet around a distant sun-like star. So, it could have oceans, it could have land, it could be habitable by some sort of creature, but we don't know that much about it. Only that it's the right size, the right distance from its sun, and you know, it looks a little bit like Earth.
Ben - So, what are we looking for when we're looking for habitable planets rather than just any old lump of rock or gas? What are the indicators?
Dan - Well, all they can tell with this particular method that Kepler uses, because planets are so small and so dim compared to the star they're orbiting around, you can't see them directly. It's very, very hard to see them directly, so you have to detect them by other methods.
Kepler uses the method of transits. So, it essentially looks at a star,  measures how bright it is and keeps watching it. And if ocasionally, it gets a very, very tiny bit dimmer, that means that a planet has passed in front of it. So, the only information you get are about its orbit - so, how long it takes to orbit the star and the size of the planet so you can tell its radius. So, the stellar system it has discovered in this case has 5 planets that they've detected so far, ranging from half the size of Earth to twice the size of Earth. But the most distant one is the one that looks the best candidate and they judge that by its distance from the star and essentially how much energy it's getting from the star.
measures how bright it is and keeps watching it. And if ocasionally, it gets a very, very tiny bit dimmer, that means that a planet has passed in front of it. So, the only information you get are about its orbit - so, how long it takes to orbit the star and the size of the planet so you can tell its radius. So, the stellar system it has discovered in this case has 5 planets that they've detected so far, ranging from half the size of Earth to twice the size of Earth. But the most distant one is the one that looks the best candidate and they judge that by its distance from the star and essentially how much energy it's getting from the star.
If it's too far away, any water and other gases on it would freeze out. If it's too close, it would be too hot and they would boil off. So, you're looking for one that's in the middle of - between those two extremes, so youre going to get the most temperate atmosphere. But sadly, we can't know if it has an atmosphere. We don't know what it's made of. We don't even know for sure that it's got a rocky surface. It could be made of gas. But it's 40% bigger than earth, so the likelihood is that it could be a solid planet.
Ben - And Kepler has been out there for awhile now and it's found hundreds of them. It seems to turn up a few hundred more every month in fact. How do we now start asking the questions you were talking about? Does it have an atmosphere? Is it rocky? Surely, Kepler can' do that because of the way it's looking for planets.
Dan - That's true. It's not there to characterise the planets. It's there to see how many there are and how they're distributed. So, to find out more about individual planets, we have to have another method, and the ideal method is direct observation. But that's extremely hard because it's like looking into the beam of a search-light in trying to identify a firefly flying around nearby. And it can be done.
The Hubble Space Telescope and some ground base scopes have identified a few planets. But they tend to be special cases like very bright planets around very dim stars and in very wide orbits. So, they're a long way away. But you need special telescopes or special satellites to get any further. Later this year, there are a couple of new instruments that are going to be attached to some of the world's biggest ground base telescopes and they'll be able to directly image some bigger planets, but not ones that are earth-sized. To get earth-sized planets, you need a specially purpose-built telescope in space and at the moment, they're just too expensive.
05:08 - Insects surviving extreme conditions
Insects surviving extreme conditions
Ben - Now, you've been looking at a new way to make insects survive some very extreme conditions.
Phillip - Yes, this is a polymer nano-suit that will protect insect or insect larvae from the high vacuum and electron beams inside a scanning electron microscope.
Ben - So, we call it a polymer nano-suit. It does involve actually putting a  suit on the insect before we put it in the machine.
suit on the insect before we put it in the machine.
Phillip - Well yes, but that's not how it was discovered. The original discovery was made because a particular kind of larvae - Drosophila which are the fruitflies that we're very familiar with from a lot of biological studies - actually naturally produce a material on their surface that when it's bombarded with electron beam, crosslinks to make a natural polymer nano-suit.
And thats what Takahiko Hariyama at Hamamatsu University found when they put these Drosophila larvae into their SEM, they expected them to die and dehydrate, all their water to evaporate. But actually, they found that the larvae were wiggling around and moving for over an hour and if you want to see it, you can look at the video on the Chemistry World website. We've got some videos of the Drosophila larvae wiggling around in the microscope.
Ben - So, why do the larvae do this? Do we have any idea why they would protect themselves from conditions that they're simply never going to encounter on Earth?
Phillip - Well, it's not necessarily likely to be designed for that purpose or evolved for that purpose. It's just a protective kind of sticky layer that protects them as they develop as larvae. It only becomes a nano-suit actually when it's bombarded with the electron beam. So, if you put them into a high vacuum without the electron beam, they do dehydrate, shrivel up and die. But when you have the electron beam there, the energy and the electrons in the beam can make whatever is in the molecules in the extracellular substance crosslink conforms kind of polymer.
The interesting thing is that the group found that if you take a similar molecule called Tween which is a surfactant that's used quite extensively in biology. It acts in a very simple way if you dip larvae that don't naturally have this extracellular substance on them into a solution of Tween and put them into the microscope and apply the electron beam, it crosslinks and makes a sort of manmade polymer nano-suit. So you can then look at all sorts of different kinds of larvae and spiders, and crustacean larvae as well. So, they've extended it to look at all sorts of things in much more realistic conditions because of obviously, they're not dessicated and dried out so you can see what these things are actually like and how they move.
Dan - How big a creature could you image in this way?
Phillip - Well, at the moment, what their team has done is mostly sort of larvae of spiders or insects, or whatever. So, these are quite smart. I mean, if you think of a fruit fly, that's a prety tiny thing so the larva is probably even smaller. So I mean, these are still quite small things and if we had bigger things, you'd probably look at them in a different kind of microscope. You wouldn't necessarily need an electron microscope. So, this I think, it's going to be for relatively small things. But I guess in theory, there's not a huge limit to how big a thing you could put in as long as it's covered and fits in the actual equipment.

08:34 - Strange properties observed
Strange properties observed
Ben - Now Peter, we're going to jump back into the world of Physics for you and this one is about a nano particle. In this case, the wonderful buckyball fullerene and its interactions with nanotubes. What have we got?
Peter - Okay, well if you start at the middle so to speak, something everyone'll be familiar with, a water molecule. This paper is by two theoretical physicists, using computer simulations. So, everything I talk about is done on the computer and not in the lab.
But basically, if you imagine taking a water molecule, placing it inside a  fullerene which is like a mini football 60 carbon atoms forming roughly a sphere. And you can do that in the lab, and that has been done in the lab and lots of other things have been put in in fullerenes as well. And then they put the fullerene containing the water molecule which they call an endohedral fullerene. They put that in a carbon nanotube which as its name implies is, a very small tube made of carbon atoms rolled up a bit like a drinking straw. And then they model what happens if you apply an electric field along the direction of the nanotube and they basically find that the fullerene containing the water molecule moves.
fullerene which is like a mini football 60 carbon atoms forming roughly a sphere. And you can do that in the lab, and that has been done in the lab and lots of other things have been put in in fullerenes as well. And then they put the fullerene containing the water molecule which they call an endohedral fullerene. They put that in a carbon nanotube which as its name implies is, a very small tube made of carbon atoms rolled up a bit like a drinking straw. And then they model what happens if you apply an electric field along the direction of the nanotube and they basically find that the fullerene containing the water molecule moves.
That's a bit mysterious because it's neutral. Water is neutral and the fullerene is neutral so you wouldn't expect it to move if an electric field was applied. Although again, it's not surprising because water is what's known as a polar molecule and that they charge separates and so the oxygen becomes negative - slightly negative and the hydrogen atoms becomes slightly positive. So then it's overall neutral, but it's got a charge distribution so you might expect it to do something in an electric field.
Well, what they found that was really strange was that in their simulations, as they increase the strength of this field, first of all, the fullerenes containing water molecules moved in one direction and then when the field increased above a certain value it started moving in the other direction.
Ben - So, that's just really increasing the actual strength. That's not changing their polarity. We're not using AC alternating current.
Peter - No.
Ben - Literally just a more powerful or stronger electric field.
Peter - That's right, yeah. So basically, what they say is that a water molecule is moving all the time. It's rotating, it's vibrating and they basically argue that the energy that's sort of tied up in these forms of motion becomes converted into motion in a straight line because basically, in the nanotube, it can either go forwards or backwards. There's nowhere else for it to go.
That's their working hypothesis, but they really need to be sort of confirmed in a lab to be useful for anything and that might be fairly tricky because as I say, water molecules and lots of other atoms have been put in. Fullerenes have been put inside nanotubes to make what's known as nano peapods.
But the electric fields you're talking about in these experiments are very high. The voltage at which it changes from moving in one direction against the field to moving with the field. You know, it's something like half a billion volts per meter. All sorts of other things might happen if you applied a voltage like that to a system like this. It's an example, in a way, a very sort of pure research and just thinking what would happen if I take this very well understood system. Nanotubes has made thousands of papers on fullerenes, theres has been thousands of paper on water, countless papers on it. So, it's interesting that there are still new things we can explore in such well-known systems.
Philip - If you're starting to talk about drug delivery, is the idea to then start putting bigger, more complex molecules inside the fullerene with slighlty more complicated charge distributions and see how they behave when you start to apply the field. Is that where that might come in?
Peter - I think you could try and do it with sort of larger and more complicated molecules, but I think that really, really is far off. I think it's more a fundamental problem. Where they're just trying to get the terms with the basic physics and chemistry that are going on in these systems.
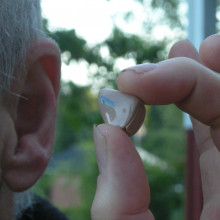
12:38 - Why Does Hearing Dampen After Loud Music
Why Does Hearing Dampen After Loud Music
with Professor Gary Housley, University of New South Wales
This week, researchers in Sydney and in California have identified a chemical factor dampens down hearing, causing the temporary hearing loss that we experience after exposure to loud sounds such as a rock concert. And this can even protect us from the permanent hearing loss that's caused by very long term noise exposure. To find out more, Chris Smith spoke to Gary Housley from the University of New South Wales in Sydney.
Gary - So, what we've discovered is that this receptor which is called a receptor for ATP is activated when sound levels come up in our environment. So, as noise develops, then we found that the hearing organ, the cochlea releases a particular chemical which binds to this receptor and then the receptor triggers a process which is quite remarkable which reflects adaptation or adjusment of hearing sensitivity. This research has identified this one receptor, one molecule as the start of a process that over a period of 20 minutes or more with an increase in background noise turns down the sensitivity of our hearing.
Chris - You said that it kicks in after about 20 minutes. So, how long does the effect last for, once you've got the diminuendo in or reduction in hearing sensitivity? How long do you remain partially deaf for?
Gary - Perhaps, I can put this in the context, the experiment itself. So, having identified a receptor, we wanted to find out what it was doing with regard to the influence of noise on hearing and a drug company in the United States had developed a mouse model where those mice no longer express that receptor.
We were provided with some of those mice and we exposed the mice to 20 minutes an hour or 2 hours of quite loud sound - 85 decibels of noise which is louder than a lawn mower. We were expecting to see a major hearing loss because that's what happens with mice or people when they're exposed to these loud sounds. So, the eureka moment for us was then after all this time in the sound chamber, we tested them out - the hearing of the mice - and there was no change in the hearing sensitivity. It was beautifully acute. So, noise had had no impact on the sensitivity of the mouse.
So, what we then did is of course compared this with a normal mouse where that receptor was present and functioning, and that's when we plotted the time constant for the development of the loss of hearing. And the time constant is roughly a measure of the time it takes to get half that makes more effect, and thats about 20 minutes. So, the next question was, once this hearing desensitisation or adaptation has occured, how long after noises turned off does it take for the hearing to return? We found by testing the hearing various times after we'd turn the noise off that the time constant is about 12 hours for recovery and what that means in practical terms is that after half an hour of loud noise, a normal mouse would take more than 24 hours to regain its baseline level of hearing.
Chris - It takes 20 minutes for that protective effect to have at least half of its effect.
Gary - Yes.
Chris - Sounds can do damage much more accutely than that though. If  you go and listen to The Who - the loudest band in history - they're going to start playing chords that are 110 decibels from the minute their hands at the guitar strings. So, I'm surprised the system isn't faster.
you go and listen to The Who - the loudest band in history - they're going to start playing chords that are 110 decibels from the minute their hands at the guitar strings. So, I'm surprised the system isn't faster.
Gary - Well, perhaps the good news is that ther are faster response systems for dealing with loud transients and that's part of your feedback control to the hearing organ from the brain. And so, that's called an efferent system and that neural pathway can adjust the hearing sensitivity in a matter of milliseconds per seconds. So, it's a very fast dynamic process that actually enables us to pay attention to particular sounds against a noisy background. But that also adapts very quickly, so it's a dynamic response.
When it comes to recreational noise exposure or perhaps music exposure in the case of The Who, those very intense sounds are worrisome. It's something that as you pointed out, it's not within normal physiological parameters for our hearing organ and there's a high likelihood that will cause damage. I suppose the issues that our research raises is that with this natural ability to adapt to loud sounds, it's likely that some people will have this in a more effective mechanism than others. And so, if people have less dynamic control of their hearing sensitivities through this ATP receptor pathway we've identified then they may well be at risk of hearing loss because we found that with our mice that didn't have this receptor, if we raise the ante as it were and expose them to very loud sounds in excess of 95 or 100 db which is aproaching those sorts of levels you talked about then after some time of exposure, they had far risk permanent hearing loss than the normal mouse that has the fully developed adaptation reflex.
Chris - So, before I go to my next rock concert, should I be popping a pill of something or is this the ultimate aspiration? We can give people pharmacological ear defenders then.
Gary - So, the neat thing about these sorts of elements is perhaps the potential for prophylactic treatment. One of the challenges from noise-enduced hearing loss has been that the safe levels of sound exposure are defined but people get caught out or they make a voluntary decision that they're going to ignore those kinds of prudent guidelines.
So, if indeed there is that therapeutic window either to provide a pill, switching on a pathway which can deal with the noise stresses or indeed perhaps other chemical stresses then that may provide some protection or conversely once the hearing damage is established. What the field suggests now is that those pathways that lead to irreversible damage principally to the hair cells and the auditory neurons are activated over a period of hours or potentially days after the initial insult. These are the challenges I think for the hearing science to identify which pathways within particular cells in the hearing organ are key to preserving hearing function.
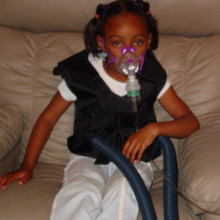
20:32 - Cystic Fibrosis and Gene Therapy
Cystic Fibrosis and Gene Therapy
with Stephen Hart, University College London
Chris - This week, we're at the British Society for Gene and Cell Therapy's Conference at Royal Holloway University in Surrey. Earlier today, I spoke to the society's president to find out a bit more about the purpose for today's event.
Adrian - I'm Professor Adrian Thrasher. I'm a Consultant Immunologist at Great Ormond Street Hospital and I'm currently the President of the British Society for Cell and Gene Therapy. This is a meeting that the society holds every year throughout the country. What we try and do is bring together a group of scientists to discuss the latest advances in gene therapy. And actually, one of the innovations we've had this year is to try and bring the stem cell community together because we feel that there are considerable synergies between the two parties if you like.
Chris - I did my PhD in gene therapy and most of the things that we were writing about were things that were very speculative and in the future. The thing that's really striking me from being here is scientists are now saying at this meeting, we are doing those sorts of things we dreamed about 10 years ago. It's really coming to fruition.
Adrian - It is no question. I mean, there are a number of different  diseases, both rare diseases and more common diseases including cancer that are responding well to the new genetic therapies. So, the question has changed from, can we do this in a few diseases to what other diseases are targetable by gene therapy or cell therapy?
diseases, both rare diseases and more common diseases including cancer that are responding well to the new genetic therapies. So, the question has changed from, can we do this in a few diseases to what other diseases are targetable by gene therapy or cell therapy?
Chris - What are the really big announcements or the really big developments that are being championed here at the conference?
Adrian - It's difficult to pin down single advances because there are actually large numbers of what we would think of as big advances. So the new diseases that are responding to treatments, rare hematologic diseases, rare metabolic diseases where patients are having sustained lifelong benefits. In the cancer field, we're seeing patients with leukemia responding incredibly well to redirect a T-cell therapy for example. So, there are lots of huge advances.
Chris - Well, let's hear about some of those advances. Kate Lamble has been speaking with Steve Hart who's from UCL and works on cystic fibrosis.
Steve - Cystic fibrosis is caused by a genetic mutation in a gene called the cystic fibrosis transmembrane conductance regulator, CFTR for short and it affects a number of organs - the lung, liver, gut, pancreas, and the major health problem in cystic fibrosis is the lung. So, patients that have very thick mucous lining the airways and that leads to bacterial infection. Bacterial infection leads to inflammatory response and that exacerbates the damage to a lung. So, the long term prospects are one of a slow loss of lung function.
Gene therapy, which I started working on - now, this is my 20th anniversary of trying to develop gene therapy for CF. So far, unless we hear something new and exciting at this conference, there hasn't yet been a report of anything therapeutic.
Kate - So, in gene therapy, you're hoping to replace this mutated gene in people's cells. What's the best way of getting that gene into those cells?
Steve - The challenges are to get the gene to the correct area first of all. The lung has an enormous surface area equivalent to at least Wimbledon tennis court and so, whereabouts in that huge area have you got to deliver your genes is obviously a big challenge. We've taken that that site of delivery should be the site where CFTR is normally expressed within the lung. And that happens to be in the trachea, the bronchii, and the bronchioles which are together known as the conducting airways.
So, delivery to the conducting airways is the challenge. Once you get there however, the next barrier is the mucous. So, how to get through the mucous. So, even then if you get through the mucous, the barrier below that, you have cilia which are these small hair-like projections which are highly motile and moving very rapidly, all in one direction to sweep out particles from the lung. And only last year, it's emerged now that there's another protein mesh between these cilia which excludes particles, any larger than about 20 nanometers. So essentially, it's able to exclude even viruses. But we take hope from biology where we know that people do get respiratory infections.
Kate - It seems quite odd to take hope from people getting respiratory infections. How can you replicate those infections in order to transmit the gene into the cells?
Steve - So, viruses, you can think of them as biological nano particles - very well adapted, very efficient at getting genes into cells, the sole purpose of making more virus. So, if we can develop synthetic nano particles that look like viruses and have some of the functions that enable viruses to get into cells then maybe we can develop a more efficient system.
Kate - It's one thing getting a gene into a cell and you've talked about how difficult and how many barriers there are to that in the lungs, but it's another thing to make sure that that gene, once it's in the cell is used and expressed. How do you make sure that that happens?
Steve - Genes usually come in a piece of circular DNA called a plasmid and these plasmids can be switched off very rapidly. To grow a plasmid, it needs to be amplified by growth in a bacterial culture. So, as the bacteria grow, so the plasmid replicates inside cell. So, you need switches and regulatory elements to control making more copies of the plasmid DNA and a selective force needs to be applied as well so that the bacteria need to keep that plasmid in a high copy number. And that selection is usually an antibiotic, so there is an antibiotic resistance gene on the plasmid. So, that's only needed for growth in the bacteria. So, once you come to put your DNA construct into humans or mammalian cells, you don't need all that bacterial stuff. It's now junk. And actually, it can be quite damaging to the treatments. There are certain sequences of DNA that are recognised as foreign by a mammalian cell and it will cause quite a strong inflammatory and immune respons.
So, we've been developing mini circle technology for delivery to the lung. We're not aware of any other group that's done this yet, but I'm going to be presenting some of the data of this conference. The idea of mini circles was to use simple recombinant DNA technology so you can still grow up the plasmid in bacteria to get large amounts of it. But then you can give them a further treatment so that they essentially loop out the region containing your gene and your mammalian switches that you want to keep. So, you end up with a mini circle that is much smaller because it doesn't now have all this bacterial junk.It's much less inflammatory and per weight of DNA, the benefit is that you've got more copies of the gene of interest. In our In Vivo studies, we've found that for the same weight of DNA, compared to a plasmid on mini circle will give nearly 10-fold higher level of gene expression. And at the moment, for CF, expression is the name of the game.
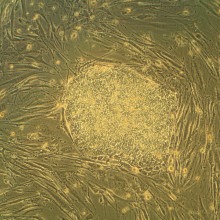
28:58 - The Future of Cell Therapy
The Future of Cell Therapy
Chris - Now we've just heard about how gene therapy can help to correct health issues caused by genetic mutations, but another approach looks at using whole cells instead. And now, I'm joined by three pioneers in this field. Dr. Robin Ali is a molecular biologist at the Institute of Ophthalmology at University College London. He's looking at ways to repair the damaged and diseased retina. Dr. Ludwig Vallier is a Stem Cell Biologist at Cambridge University and at the Sanger Institute, Professor Giulio Cossu is a Stem Cell Biologist also at University College London and he has an interest in muscular dystrophies. If each of you could first give us a quick overview in just one line on what you're work is. We'll start with you, Robin...
Robin - Well, the aim of my work is to develop a new treatment for blindness that is caused by the loss of photo receptor cells which are the light sensitive cells and the retina. And we aim to be able to replace these cells in order to restore vision.
Chris - Giulio, you're trying to do for muscles what Robin is trying to do for the eye.
Giulio - Pretty much. With that difference that for the eye, you need very few cells whereas if you want to treat a disease like a muscular dystrophy that affects 40% of that mass of our body, you're going to need a lot of cell, and that is right now, our major problem.
Chris - And Ludwig, one way to tackle both problems might be to make cells that are the individual's own cells, rather than going and getting cells from someone else that will be incompatible genetically with the individual. Wouldn't it be nice if we can make cells that are from the individuals themselves?
Ludwig - So, I guess now we have a technology to reprogram the identity of other cells into or stem cells which are capable to grow indefinitely and differentiate into a diversity of other cell types including cells for the eyes, muscle cells. And so, that - I mean, that we can generate even quantity of those cells which will be extremely useful for the cell therapy that Robin and Giulio have just described.
Chris - So Robin, when you do your work, can you just talk us through the story so far, what you've achieved, and how you've done it?
Ludwig - So, some years ago, we wanted to tell whether it might be at all possible to transplant a photoreceptor cell.
Chris - The rods and cones.
Ludwig - Rods and cone cells. They're one of the most specialised cells in the body and they make very specific connections. We hypothesise that it may be possible to transplant these cells and have the appropriate connections. We carried out to see those experiments in which we looked on what stage of development is necessary for successful transplantation. We determined that it was a very specific stage which was between a fully mature cell and one, not quite fully mature. And provided we transplant photoreceptor cells at this stage, they're able to integrate into the retina and make appropriate connections.
Chris - How do they know where to go in the retina because you're literally taking a retina from say, let's call it a 'donor animal' which is at the right stage of development? You're taking the cells out of that retina and injecting them into an animal with a lack of those photoreceptors. How do they know? How do you know you are taking photoreceptors where they will go in the retina?
Ludwig - They are already almost fully mature photoreceptors. We discovered that injection of stem cells doesn't result in maturing into photoreceptors and connections. They are almost fully mature photoreceptors. They're then migrating within the retina and they're just recapitulating that normal development. We're transplanting them very close to the site that they finally end up. So, they're probably just following their normal processes of development.
Chris - And the mice, because you're doing this in mice at the moment aren't you, that the mice that get these cells, can they see again afterwards?
Ludwig - So, we carried out experiments last year in which we could show in mice that lack night vision. They have no functional rods, if we transplant new rods into these animals that we can restore cognitive vision. So, not only do the cells integrates into the retina, but they're making functional connections to the brain and the mice were able to see in dim light.
Chris - How does this work with a muscular dystrophy study there because Robin is saying, "Well, I'm just able to put the cells roughly where they needed to go. They don't have far to go and they're almost the sorts of cells that they need to be." Is that the same with your approach?
Ludwig - It is quite similar indeed. If you transplant stem cells, they still do not know what they will become. The chance that they will learn how to make a functional muscle cell are very small and if you transplant a mature contracting muscle fibre, most likely, it will not survive. So, also in this case, you have to transplant cells that are already committed, they have decided that they will become muscle, but they're not yet muscle. And in terms of knowing where to go, obviously, you have to inject them in the right place that don't have a map so that you can put them in the brain and they travel to the muscle.
Chris - Well, if you look at say, what a haematologist does with a bone marrow stem cell when we have a bone marrow transplant, actually, we do just inject stem cells into a vein and they do know where to go. They go back to the bone marrow and they repopulate new bone marrow and turn into new blood.
Ludwig - That's correct, but this is the exception. It's not the rule. For the very simple reason, the blood is the only tissue that is liquid and the cells circulate and by circulating, they have to learn how to find the right signal how to move and how to go home. All the other tissue do not have this evaluative pressure to find their way home so you have to put them close to the place where you want them to be.
Chris - So, in your example of muscular dystrophy, does this mean that a person who was going to have this sort of therapy would face a total body injection for want of a better word? You've got to inject everywhere or is there a way of doing for muscles what a haematologist does for bone marrow.
Ludwig - There is a weight in between. But 20 years ago, there were trials where the cells were injected directly into skeletal muscles. But because we have so many muscle and the cell don't move much from the point of injection, this would turn out to be non-practical. What we found that another kind of muscle progenitor that can be delivered through the arterial circulation can inject in the artery will come out of the arteries if there is inflammation like there is in muscular dystrophy. And so, with a single injection, you can colonise all the muscle downstream of the artery that you are injecting. This is not 100% efficient, but it's a way to bring the cells where you want to be.
Chris - What is that cell that's able to do that?
Ludwig - The cells, we call mesoangioblast and is a name like mesenchymal stem cell or embryonic stem cell. These are not real cells. Our cells we have adopted to grow in culture starting from a specific cell type. In our case, a cell called pericyte that is around the very small blood vessel.
Chris - So these cells, when you put them into the arterial circulation and they find themselves going through a muscle, is it the environment in the muscle that says to the cell, "You should now become a mature skeletal muscle cell"?
Ludwig - Yes, obviously, these cells, once you've taken them and isolated from a skeletal muscle will never be able to turn into neuron or into hepatocyte, but they have a few developmental options. They can decide to become a skeletal muscle or a smooth muscle that will form the layer around the blood vessel and will decide what to do depending on where they find physically associated. So, if they get close to a regenerating muscle fibre and will get into the fibre and will be incorporated in the newly fibre. As they remain close to the vessel wall, they most likely will become part of the vessel wall.
Chris - In (a dish in) muscular dystrophy, patients with this don't just manifest problems in their skeletal muscles. They have other muscles in the body including cardiac muscle. Will these mesoangioblasts also find their way into the heart and repopulate the heart with healthy cardiomyocytes there?
Ludwig - Not the one that we isolated from skeletal muscle. There are other strategies to treat the heart and right now, pharmacological help seem to be the easiest way to go.
Chris - So, you're doing this in dogs which have a form of muscular dystrophy similar to a human. Is therefore the capacity if it works in a dog to translate this to a human? Do you think it'll work?
Ludwig - Well, we did it. We have a trial running in my previous institution at in Milan and we are accumulating results to see whether first of all, there are damage for the patient, what is called a phase 1 trial is designed to test safety and then to see whether we get some efficacy.
Chris - And the cells you are using, are they the patients' own or are they from somewhere else?
Ludwig - No. In this case, they come from an agely identical donor, a brother. Pretty much, like it happens for bone marrow transplantation.
Chris - So, the obviously more solution in both these cases would be Ludwig, if we could get some cells that were from the individual themselves. Practically speaking, is that possible now with the science we have? Can we derive new cells for mature tissues?
Ludwig - So we can. Yeah, definitely now, stem cells can form tissue by reprogramming them, by overexpressing protein that by actually bringing them back to a more foetal stage directly.
Chris - So, you take skin cells.
Ludwig - Skin cells, blood cells...
Chris - And put the factors into it.
Ludwig - Yes.
Chris - How do you get those factors?
Ludwig - So, the most common method right now is still, using in fact gene therapy approach using your viruses and retroviruses.
Chris - So, you put these four factors in.
Ludwig - Yes.
Chris - And what does that physically do to the skin cell to make it into a stem cell again?
Ludwig - Any cell type in the body will have a very strong mark on the DNA. And what we do is that we just erase this identity and then pose a new one with those factors and these identities are stem cell identity which give them this capacity to grow and to differentiate. That is very interesting for genetic medicine.
Chris - And one thing you can obviously do with those cells, you can turn them into other cells which means presumably, if Robin says, "Well, I want to model why some of my patients get a certain type of eye degeneration." You could take cells from their skin, turn them into the sorts of cells that become diseased in that patient group and then study the disease in the dish rather than having to go and find loads of different patients and study them all individually.
Ludwig - Yeah, that is what we are doing already now in the past 3 or 4 years. We take sample from patient with genetic disorder, or many, and then differentiate the stem cell generated from this patient into cell type that's affected by the disease and that's how we can model a disease in the dish and do studies, studies that will now be possible to do from a biopsy or primary tissue from those patients. And that new individual model to skin drug and other agent...
Chris - Are these cells safe?
Ludwig - So clearly, those cells are like any other cells gone In Vitro. They accumulate genetic modification over time when you grow them. But that's a natural process. That occur in any cells In Vivo and In Vitro. But now, what is really important to say is that, now, we have in fact the quality control that enable us to design different cells, is too much damaged, or is safe to be used In Vivo because we can't directly sequence all genome in less than a week for a cost that is not effective for therapies. So, it doesn't mean that we can't really quality control cells and we can now have some level of safety for transplantation of these cells.
Chris - So Robin, why are you fiddling around with embryonic cells? You've got Ludwig here, you could use some cells from an adult!
Robin - Our approach is to always take the low-hanging fruits and we start our studies with cell transplantation donor retinas, just on sound transplantation. We subsequently started to work with embryonic stem cells in order to see whether we can derive the appropriate cells for transplantation and that's a huge challenge because we've been able to make photoreceptors from embryonic stem cells for some time. What we've not been able to do until very recently is to obtain sufficient numbers of embryonic stem cell derived photoreceptors for transplantation. That's taken a huge amount of time and effort to do with embryonic stem cells. IPS cells have tremendous potential, but there are still further challenges remaining with IPS also. I think that maybe ultimately the most effective way of avoiding rejection to have a personalised medicine, but I think it's going to be some time before we're able to really implement that technology clinically.
Kate - Thanks to Dr. Robin Ali, Dr. Ludwig Vallier, and Professor Giulio Cossu. This is the Naked Scientists with Chris Smith and with me, Kate Lamble. If you'd like to get in touch with any questions or comments about these therapies we've been discussing today, do email us to studio@thenakedscientists.com, you can tweet @nakedscientists or find us on Facebook.
43:27 - Fighting Cancer with Virus Therapy
Fighting Cancer with Virus Therapy
with Len Seymour, University of Oxford
As well as gene and cell therapy, one other approach being discussed here at Royal Holloway this week is virus therapy where the natural ability of viruses to infect cells can be hijacked for medical use including the treatment of cancer. Kate Lamble spoke to Dr. Len Seymour from Oxford University.
Len - Viral therapy provides some aspects of therapeutics that have not been possible before with regular chemotherapies. At one level, a very important level that allows for the therapeutic agent to amplify itself at the target site. And when I say that, I mean the virus itself will replicate selectively in cancer cells and produce very high numbers. So for example, one virus infecting a cell can go on to produce 10,000 maybe 50,000 copies of the virus inside the tumour cell which will then lyse the cell and spread to infect adjacent cells and repeat the process. So, you have the possibility to amplify the therapeutic actually within the target which is something that's never been possible with chemotherapeutic agents. With those agents, the highest concentrations of the drug are always present in the bloodstream on the way to the tumour. And therefore, they're confounded by significant off target side effects. So, bone marrow toxicities, or toxicities against hair follicles in the gut. Whereas with the virus, it really can be designed to have almost no off target toxicities.
Kate - When you're aiming for a virus to take a gene into the cancer cells, what are you aiming for it to do? Is it to kill the cells or just to stop it replicating?
Len - One of the main problems with cancer which we're increasingly understanding particularly since we've had whole genome sequencing of cancer cells, is that they contain a huge number of mutations.So, a typical colorectal or breast cancer cell carries something like 90 or 100 mutations.
So, to try to fix a cancer cell like that is a really difficult issue. So, it's very tempting to take the alternative approach which just say, "Well, let's not try to do it. Let's simply try to kill the cancer cells." So, we use viruses and their ability to kill cells by replicating and lysing cells, and you have also the possibility to express therapeutic proteins within the virus.
Although many of our agents are simply viruses that are killing the cells as they proliferate, we can encode additional proteins at the genetic level within the virus to mediate an intracellular biological effect or even having agents secreted from the infected tumour cells to affect other cells within the tumour that are not directly infected with the virus.
Kate - These cancer cells are genetically identical almost apart from these mutations to our own cells. How do we use that virus to tell those cancer cells apart from our normal cells?
Len - Many tumour cells seem to be selectively permissive for viruses, so they do have a level of intrinsic selectivity for wildtype viruses. But then on top of that, you can use genetic modification techniques to make viruses specifically exploit the tumour.
So, at one level, you can introduce tissue specific promoters which are selectively activated within the tumour cells to drive the virus. At another level, you can take components out of the virus and make it dependent on mutations that have occured in the tumour. There are many different approaches you can take to make viruses which depend on mutations.
Kate - Do we identify virus that's in the natural world and we think, "That's doing something good. We could use that in this certain way" or do we try and adapt them and we just pick a generic virus and adapt it to how we would use it with cancer?
Len - I think that's a great question because as a scientist, it's always tempting to go and look for really interesting clever virus that can do something sophisticated to a cell and which you can exploit. But it's also very important to keep your feet on the ground in terms of trying to translate something into the clinics and it's easier to translate something into the clinic, say, if there's a body of evidence about the virus already.
In the end, one of the most important things is the virus you're working with can be produced to launch quantities, you needed enormous amounts of material to be able then to take out for a clinical trial. Many viruses are difficult to manufacture in large quantities. So, in my mind, adenoviruses probably are the simplest and the best.
Kate - We find cancers all over the body in every different organ. Is virus therapy particularly effective over all of those different types of cancer or are some cancers more difficult to reach through this method?
Len - When people present with cancer, something like 80% of them go on to die from metastatic disease, which means the disease which is spread around the body. And so, for a therapy which is going to be effective, it must be able to be given systemically.
Now, viruses come into very difficult class of agents to give intravenously because the body has learned over a millenia to recognise them as pathogens. So somehow, we have to find a way to preserve the body or engineer the viruses where they can at least achieve access to disseminated tumours.
Now, there are several different ways you can do that. One way that has been looked at which is quite promising is to put a transient coating onto the virus to protect it during the delivery phase. Another possibility is to use a serotype of virus which has not been widely seen before and for which there are relatively small numbers of neutralising antibodies in the circulation. So, there are some tricks, but in the end, if a virus can be given intravenously to access disseminated cancer, then I think it's the only way you can use it to treat metastatic disease.
Kate - You're treating people with something that the body automatically reacts against. Can you harness the body's immune reaction at all?
Len - You touched on another really interesting point which is the immune situation of the tumour. Human tumours, by the time they present clinically have had normally several years to grow and adapt. So although tumours pick up an awful lot of mutations and you would think as they pick the mutations, they would become potentially immunogenic. The immunogenic variance have been weeded it out. So, the forms that survive in the cancer are the forms which are not that much immunogenic profile. So, although there are cancer antigens, they're not normally very strong antigens.
Now, on top of that, a tumour has become rather sophisticated in finding ways to evade immune detection. It can express a variety of different pathways that will allow it to suppress the local immune system. Now, this means that there can be a situation when a virus goes into a tumour and that the immune system has a level of suppresion already and this may be another reason why on a local level, a virus finds it a reasonable place for it to be proliferative.
But of course, the virus can express components within the tumour that can modulate some of these factors that regulate the immune status of the tumour. And so, where we dream of going is to make a virus that will, to some extent reverse the immune suppresion within the tumour and allow the body's immune system to recognise the tumour and create an anti-cancer vaccine.

50:13 - Can gene therapy treat depression?
Can gene therapy treat depression?
Transcript will be on this site shortly










Comments
Add a comment