In this NewsFlash, we find out what a rare, self-healing skin tumour can tell us about more common cancers, explore the capacity for self repair in the mammalian heart, and discover the new laser based tool for diagnosing melanoma. Plus, how the bones of people who died up to a hundred years ago are being used in the development of new treatments for chronic back pain...
In this episode
00:30 - Self-healing skin tumour could shed light on more common cancers
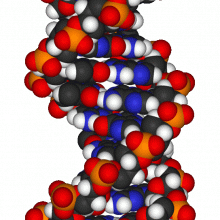
Self-healing skin tumour could shed light on more common cancers
"Self-healing" is not a word that people usually associate with cancer. But researchers studying a very unusual and rare form of skin cancer that can clear up by itself have learned some lessons that could potentially lead to new treatments for the disease in the future.
It's a rare hereditary cancer called multiple self-healing squamous epithelioma, or MSSE for short - it only affects a handful of people every year in the UK, and most of them can trace their ancestry to a single family from Scotland. The disease causes large flat tumours on the skin which heal up of their own accord, leaving disfiguring scars but no other lasting effects.
Because of the inheritance pattern of the disease, scientists know that it must be caused by a fault in a single gene, but the identity of this gene has been a mystery for more  than 40 years. But now an international team of researchers led by Cancer Research UK's Dr David Goudie in Dundee have found the culprit. The team have published their findings in the journal Nature Genetics this week, and their discovery could shed light on more common types of cancer as well.
than 40 years. But now an international team of researchers led by Cancer Research UK's Dr David Goudie in Dundee have found the culprit. The team have published their findings in the journal Nature Genetics this week, and their discovery could shed light on more common types of cancer as well.
The researchers looked at DNA samples from around 60 people with MSSE, and compared them with DNA from more than a hundred of their relative who were unaffected. They focused in particular on a region of DNA that had previously been shown to harbour the likely gene, narrowing down their search until they found the gene TGFBR1.
This gene encodes a receptor protein, which receive signals from a protein called TGF beta. These signals tell cells to divide, or to stop dividing, and the researchers were able to prove that carrying a faulty version of TGFBR1 caused people to develop MSSE tumours. Intriguingly, faults in TGF beta signalling have been found in many types of cancer.
TGF beta signalling is very interesting to cancer researchers, because it can be both a 'goodie' and a 'baddie' in the disease. In the early stages of more normal cancers, it tells cells to stop dividing, acting as a brake on tumour growth. But after a while, it switches sides, and TGF beta signals tell cells to divide and grow faster, fuelling the growth of cancer.
But in the case of MSSE, the opposite seems to happen. Cells start off growing out of control, forming the characteristic skin tumour, but then they stop growing and go into reverse.
TGFBR1 is just one of a family of receptors that are involved in receiving TGF beta signals. The researchers think that the pattern of signals must be changing as the tumours grow and then heal, allowing the 'good' side to come forward.
Although MSSE is a very rare and unusual cancer, this discovery could shed light on other, more common, types of cancer, because we know that TGF beta signalling is involved in many types of cancer. If researchers could figure out exactly how the changes in TGF beta signalling make MSSE tumours heal up, then maybe it could pave the way for future treatments for more common types of cancer. So this is a nice example of how research into a very unusual disease could have a much wider relevance.
Goudie, D. et al (2011). Multiple self-healing squamous epithelioma is caused by a disease-specific spectrum of mutations in TGFBR1 Nature Genetics DOI:
10.1038/ng.780
03:46 - Getting to the heart of cardiac repair
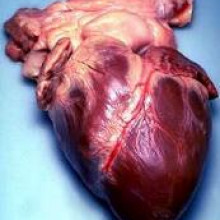
Getting to the heart of cardiac repair
A surprising discovery suggests cardiac self-repair may be possible. Prevailing wisdom suggests that mammalian hearts like our own lack the capacity to self-repair if they are injured. This is in stark contrast to other 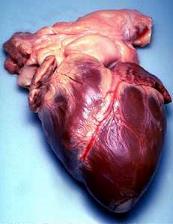 animals, including fish, that can regenerate up to a quarter of their heart muscle if it is injured or removed. But now scientists have discovered that the newborn mammalian heart also initially has the ability to do the same, but only for a short while.
animals, including fish, that can regenerate up to a quarter of their heart muscle if it is injured or removed. But now scientists have discovered that the newborn mammalian heart also initially has the ability to do the same, but only for a short while.
Writing in Science, University of Texas Southwestern Medical Center scientist Enzo Porrello and his colleagues removed about 15% of the muscle from the apices of the left ventricles of 1 day old mice. After forming a blood clot to seal the wound at the site of the injury, the mouse hearts re-grew completely within 21 days, without the development of scar tissue and with the formation of new muscle tissue and blood vessels; functional tests carried out at two months also confirmed that the recovered hearts were beating completely normally.
The recovery was achieved, the scientists found, through the proliferation of surviving muscle cells elsewhere in the heart; newly-produced heart cells migrated to the site of the injury where they then wired themselves into the regenerating tissue to replace the lost muscle. However, when the same procedure was attempted on slightly older, 7 day-old mouse pups, there was no such regenerative effort, the injured hearts developed significant scar tissue and failed to repair themselves. This intriguing result shows that the mammalian heart is capable of self-repair similar to the hearts of simpler species like zebrafish but, for some reason, this capacity is lost soon after birth.
Encouragingly, however, it also suggests that if scientists can uncover the reason underlying this switch from a pro- to a non-repair state, using a model system like this, then it might be possible to trigger the same restoratative pathway in adult human victims of cardiac diseases.
06:22 - Video - Learning from Old Bones
Video - Learning from Old Bones
| ||
For a full transcript of the interview click here.
12:16 - Laser technique offers optical biopsy
Laser technique offers optical biopsy
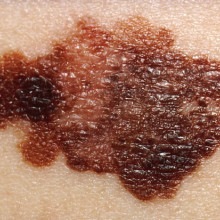
Scientists have developed a new tool that could significantly improve the sensitivity of melanoma screening techniques.
Currently, the majority of melanoma diagnoses are made clinically by eye, 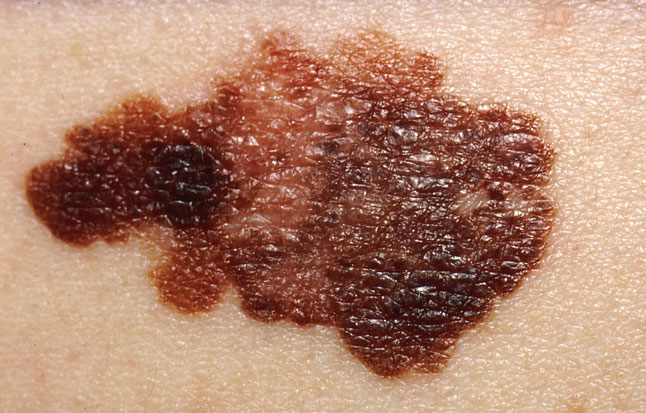 but even visualisation by a skilled dermatologist can miss up to 15% of lesions. Moreover, studies have also found that pathologists can fail to agree on a diagnosis in 14% of biopsy samples. As a result, doctors tend to act cautiously and "when in doubt, cut it out", leading to a high false-positive rate and over-treatment of benign lesions.
but even visualisation by a skilled dermatologist can miss up to 15% of lesions. Moreover, studies have also found that pathologists can fail to agree on a diagnosis in 14% of biopsy samples. As a result, doctors tend to act cautiously and "when in doubt, cut it out", leading to a high false-positive rate and over-treatment of benign lesions.
Now clinicians could soon have a new weapon with which to combat the problem. Writing in Science Translational Medicine, Duke University researcher Thomas Matthews and his colleagues have found that a laser technique called "pump-probing" can be used to detect the quantities of different forms of melanin in a skin sample. Using 42 biopsy specimens, which included a mixture of benign and melanoma lesions, the team exposed the tissue to two brief bursts of laser light of two slightly different wavelengths (colours).
The first burst of light (the pump) sensitises one form of melanin - called eumelanin, which is darker and increases in concentration proportionally in malignant cells - to the second short laser blast (the probe) delivered shortly afterwards. This enabled the team to quantitate the relative concentrations of eumelanin and its lighter phaeomelanin relative in their samples. Comparing the levels of each enabled the researchers to correctly identify all of the genuinely-malignant specimens amongst the samples studied, although the team acknowledge that they have not tested their system against the subset of non-pigmented melanomas that don't make melanin.
However, for the majority of malignant melanomas, which are pigmented, the team point out that, apart from having the potential to dramatically improve current clinical protocols, at the laser powers they have been using, the system could readily be adapted to do diagnoses in-situ on a patient without needing to take a biopsy first.










Comments
Add a comment