Cancers you can catch go under the Naked Scientists microscope this week. We find out how a transmissible facial tumour is devastating devil populations in Tasmania and also hear how the Human Papilloma Virus (HPV) causes cancer. Also, Meera looks into the science of cervical screening, and Ben and Dave reveal how carrots can help us to spot cancer cells. Plus, biofuel hope from the burning bush plant, the battle between Staphylococcus species, and the introduction of Synthia - the first microbe with a genuinely synthetic genome.
In this episode

01:41 - Burning bush brings biofuel hope
Burning bush brings biofuel hope
Have you ever seen a burning bush? These shrubs originated in Asia but have managed to invade North America. They're so-called because in the Autumn they have distinctive flame-red leaves. They look impressive, but are actually considered a bit of a pest, as they're an invasive species. But researchers at Michigan State University have made a discovery that could help turn the burning bush into the saviour of future biofuels, according to their paper in PNAS this week.
 The burning bush produces an unusual oil, which could be very useful for fuel and food as it has quite a low viscosity - stickiness or thickness. Many plant oils are too thick to use in diesel engines, so they have to undergo a process to convert them to biodiesel. The oil from the burning bush is runny enough to use directly in diesel engines. And it's also lower in calories than other plant oils, so it might be useful for making low-cal foods. But unfortunately, burning bush plants aren't really suitable for agricultural growing and harvesting. So the researchers, led by WHO, sequenced the genes in a common ornamental species of burning bush, to find the gene that produces the key components of the oil - molecules called acetyl glycerides.
The burning bush produces an unusual oil, which could be very useful for fuel and food as it has quite a low viscosity - stickiness or thickness. Many plant oils are too thick to use in diesel engines, so they have to undergo a process to convert them to biodiesel. The oil from the burning bush is runny enough to use directly in diesel engines. And it's also lower in calories than other plant oils, so it might be useful for making low-cal foods. But unfortunately, burning bush plants aren't really suitable for agricultural growing and harvesting. So the researchers, led by WHO, sequenced the genes in a common ornamental species of burning bush, to find the gene that produces the key components of the oil - molecules called acetyl glycerides.
The scientists took the gene and used genetic engineering to add it to a plant called Arabidopsis - a type of cress commonly used by plant researchers. The modified plants then started making acetyl glycerides, producing oil with a purity up to 80%. So it's quite promising that they'll be able to produce high-quality oil on a large scale in the future, either by genetically modifying oil-seed crops such as oil-seed rape (known as canola in the US), or in other, more technological biological biofuel production systems, such as algae. They're not there yet, but these are exciting early results that will help to fuel further research, if you pardon the pun.

03:48 - Battle of the Bugs
Battle of the Bugs
Researchers have discovered that the key to killing MRSA may lie with one of its own relatives. In a paper published in Nature this week, Jikei University School of Medicine scientist Tadayuki Iwase and his colleagues show how a common species of "good" bacteria frequently found on the skin, Staphylococcus epidermidis, produces a chemical weapon that disables its impetigo-inducing cousin, Staph aureus, includeing MRSA. 
More than one person in three is colonised with Staph aureus, which is a risk factor for developing Staphylococcal infections elsewhere around the body, but some individuals seem to be able to evade carrying the bug in this way. To find out how, the team swabbed the nasal cavities, where Staph is known to lurk, of 88 volunteers. Predictably, twenty eight (32%) were Staph aureus carriers. But more than 90% of the volunteers were also carrying a second Staph species called Staphylococcus epidermidis, one of the most common human commensal or "good" bacteria and it seems that this friendly bug holds the key to kicking out Staph aureus in some people.
The reason, the team found, is that some strains of Staph epidermidis secrete a factor called Esp, an enzyme known as a serine protease, which behaves like the microbiological equivalent of a mace spray, dispersing crowds of Staph aureus and rendering them vulnerable to a bug-killing chemical secreted onto the skin by the immune system called hBD2 - human beta-defensin 2.
So why would Staph epidermidis want to kick out its own cousin? Pure selfishness is the answer. By taking up space and resources, Staph aureus is competing with its more human-friendly relative, which responds by poisoning it! It's tempting to speculate that it might be possible to exploit this newly-uncovered example of bacterial biological warfare as a novel way to deal with Staph aureus infections elsewhere in the body.
07:14 - Switching on egg production
Switching on egg production
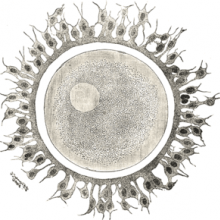
Unlike men, who are constantly producing new sperm cells, women have to work with a fixed number of egg cells from birth. Us girls are born with around 800,000 immature, dormant egg cells, known as follicles, and a couple of thousand of these are activated by hormones during each menstrual cycle, counting down our biological clock until the menopause. So there's a certain amount of time pressure on becoming a mum - at least in the biological sense. But now an international team of scientists, writing in the journal PNAS this week, have found a way to reactivate these dormant egg cells. And it could have big benefits for infertile women, or those who have had their ovary tissue frozen before treatment for diseases such as cancer.
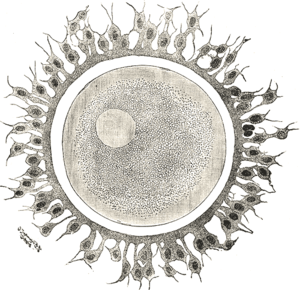 This is work from Jing Li at Stanford University in the US, and researchers in China, Japan and America, and it all hinges on a gene called PTEN. Using mice, Li and her team found that shutting off PTEN using a special chemical could activate the dormant egg follicles in the ovaries of newborn mice - and when they transplanted these follicles into adult female mice whose ovaries had been removed, they could produce mature eggs and even baby mice.
This is work from Jing Li at Stanford University in the US, and researchers in China, Japan and America, and it all hinges on a gene called PTEN. Using mice, Li and her team found that shutting off PTEN using a special chemical could activate the dormant egg follicles in the ovaries of newborn mice - and when they transplanted these follicles into adult female mice whose ovaries had been removed, they could produce mature eggs and even baby mice.
It turns out that PTEN helps to switch off another gene called PI3K - this is makes a molecule that sends signals inside cells. Normally, PI3K works on a protein called Foxo3, changing its location inside follicle cells and triggering the follicle to mature. So blocking PTEN with the chemical means that it can't switch off PI3K, so PI3K can act on Foxo3, triggering the egg maturation process.
As PTEN is also involved in protecting our cells from cancer, there is a concern that blocking it might cause cells in the follices to develop into tumours, but luckily the researchers didn't find any tumours developing. Instead, the activated follicles developed into mature eggs, which could produce healthy baby mouse pups. And these pups grew into adults and had healthy babies of their own, suggesting there aren't any fundamental inherited problems with the cells or the DNA within them.
Obviously, it's more challenging to do these experiments in humans, but the researchers managed to do some tests on ovary tissue that had been taken from women having operations for ovarian cancer. Treating them with the PTEN-blocking chemical caused follicles to mature and produce egg cells, but unfortunately it seems that there might be some problems with them. So it's not certain that it will work in women, and a lot more research will need to be done before we know if we can use the technique to treat infertility.
09:30 - The creation of 'Synthia' - Synthetic life
The creation of 'Synthia' - Synthetic life
with Victoria Gill, BBC Science Correspondent; Dr Craig Venter, J Craig Venter Institute
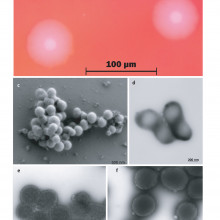
Chris - This week the J Craig Venter Institute announced the creation to huge fanfare of a brand new synthetic microorganism dubbed, "Synthia." This has prompted lots of excitement but also lots of controversy. Some people have argued that Synthia isn't entirely synthetic. So to tell us more here's Craig Venter and Victoria Gill.
Craig - Their generic heritage is the computer, so it is absolutely the first synthetic life form. A cell, driven, controlled totally by synthetic DNA. So, we call it synthetic because everything in the cell has been made and dictated by that synthetic chromosome even though we do start with another living species, we use that to initially read the genetic code and until it can transform itself into the species controlled and dictated by that synthetic chromosome.
Victoria - That's Dr. Craig Venter from the eponymous J. Craig Venter Institute, talking about his research team's new synthetic cells. But are they really synthetic cells? Is this synthetic life? Well strictly speaking, it's just the genome that's synthetic. What they've done is taken a copy of an existing bacterial genome, looked at all the DNA inside a simple bacterial cell, decoded that on a computer and then they've taken that and used the information to chemically construct a new genome, synthesising a genome in the lab from scratch. It's an impressive technological step but many biologists say that it's overstating the development to call it synthetic life. But their new cell does live. It's replicated now over a billion times. So why are scientists doing this? Well, Dr. Venter says the endeavour began as an effort to understand life on the most intimate level. What he has developed now, he says, are the tools to design new organisms which could mark a new era of biotechnology.
Craig - I think they're going to potentially create a new industrial revolution if we can really get cells to do the production we want, if they could help wean us off off oil, and reverse some of the damage to the environment like capturing back carbon dioxide. I 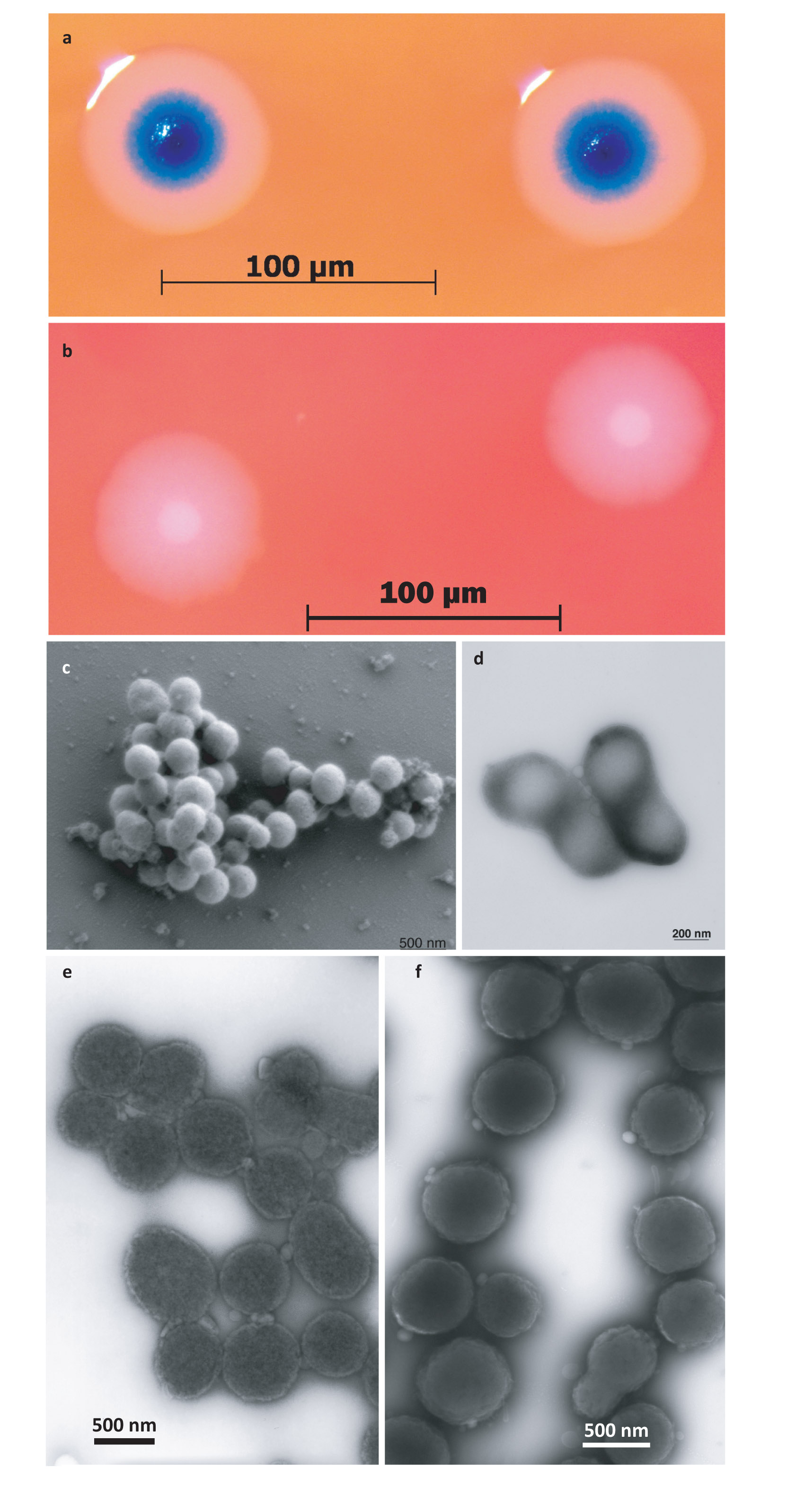 would be pretty satisfied with that outcome alone. We think some of the earliest applications people will see are new vaccines. We can make, in a day, new flu vaccines that have taken much longer to produce by conventional methods and we're working with the National Institute of Health and Novartis to build the process for very rapidly as new infections emerge to synthetically in 24 hours or less, make those vaccine candidates and get them into testing.
would be pretty satisfied with that outcome alone. We think some of the earliest applications people will see are new vaccines. We can make, in a day, new flu vaccines that have taken much longer to produce by conventional methods and we're working with the National Institute of Health and Novartis to build the process for very rapidly as new infections emerge to synthetically in 24 hours or less, make those vaccine candidates and get them into testing.
Victoria - But these claims too have sparked criticism, not just by scientists who feel the potential of this technology has been overstated but by the wider community. Julian Savulescu an ethics professor from the University of Oxford has said that the potential of this science is - although very far in the future - very real and significant, dealing with pollution and creating the new energy sources that Dr. Venter himself is so enthusiastic about. But as he pointed out, the risks are also unparalleled and this is a very rapidly moving and new field. It seems that the regulatory and safety discussions haven't really kept pace. This technology could be used in the future to make some very powerful bio-weapons. That's a very extreme example, but the potential is there. It's less than 15 years since Dr. Venter first announced that he wanted to create a synthetic organism and we're already at this stage. What concerns many people now is that the pace of this exciting new field of biology should not overtake those ethical and safety discussions. As Professor Savulescu puts it, "The challenge now is to eat the fruit without the worm."

13:32 - BioBlitz in Bristol - engaging the public with nature
BioBlitz in Bristol - engaging the public with nature
with Ed Drewitt, Bristol Natural History Museum
Chris - 2010 is the International Year of Biodiversity and a park in the centre of Bristol may not seem the obvious place to study biodiversity. It depends to what you're up to I suppose. But this weekend, Blaise Park has been host to what's known as a BioBlitz which is an attempt to find and catalogue all the different types of wildlife that you might come across. BioBlitzes are going to be happening all over the country in the next few months, so to explain more about what's coming and to hear about what they've done over the weekend, we're joined by Ed Drewitt and he's from the Bristol Natural History Consortium. Hello, Ed.
Ed - Hello, Chris.
Chris - Welcome to the Naked Scientists. Thank you for joining us. First of all, could you tell us what actually is a BioBlitz?
Ed - Yes. Well a BioBlitz is basically an opportunity to bring scientific experts, naturalist  volunteers and the public, schools and families together to basically see and find as many different species that are living in their area as possible. So as you mentioned, in Bristol Blaise Castle Estate and we had lots of schools on a Friday and then families on a Saturday engaging with experts, naturalists and volunteers looking for the different trees, lichens, aquatic insects, birds, and everything else that lives out there.
volunteers and the public, schools and families together to basically see and find as many different species that are living in their area as possible. So as you mentioned, in Bristol Blaise Castle Estate and we had lots of schools on a Friday and then families on a Saturday engaging with experts, naturalists and volunteers looking for the different trees, lichens, aquatic insects, birds, and everything else that lives out there.
Chris - What are you hoping to get out of this? Why do we think this is worth doing?
Ed - Primarily really to sort of engage the public, engage people in different parts of the country - in this case, in Bristol really with what's on their door step and opening people's eyes up to what's actually there. But also, there are some real kind of scientific outputs as well. On the BioBlitz that we had over the last couple of days or so, we found 536 species of which two were nationally scarce and I think not really recorded before including such as the Grass Rivulet Moth for example. And so, it's an opportunity to find out what's there and to then be able to advise the - for example the land manager for Blaise which is owned by Bristol City Council on what's there and what they can do to help some of that wildlife.
A lot of that data then goes, or all of that data then goes to the Bristol Regional Environmental Record Centre and they then put that data into a special database which can be used by members of the public and businesses who perhaps want to then find out what's on there. Particularly for example if there was a building application which is probably not going to happen on this particular place but might happen elsewhere in the country and so we can have a good idea of what's actually living in these places.
Chris - So when people come along to get involved, how will they actually go out and collect the data? Will they be given a 'pooter' - one of those pots with tubes coming out to suck things up or do they go around in little teams? How's the data gathered?
Ed - Well basically, we had families - you might have say, 10 people, it might be 2 or 3  families going out with a naturalist and a couple of volunteers so they might for example be going into some grassland. So they'll take out a couple of sweep nets and some white trays, and ID charts and actually, be doing their own sweep netting and discovering what's in that grassland. Likewise, if they're looking in a stream or a pond, they'd also will be doing that with nets and also using pooters as well to get some of the very tiny insects. And then that information is then put into recording forms which is kind of almost like quality controlled through the naturalist who'll be putting that onto the recording form, and from there, then it gets put on to a natural database. So it's very much about getting the public and schools hands on with nature. So we had school children and families properly doing sweep netting and then really discovering on a small, kind of minute level, what was actually living on their step.
families going out with a naturalist and a couple of volunteers so they might for example be going into some grassland. So they'll take out a couple of sweep nets and some white trays, and ID charts and actually, be doing their own sweep netting and discovering what's in that grassland. Likewise, if they're looking in a stream or a pond, they'd also will be doing that with nets and also using pooters as well to get some of the very tiny insects. And then that information is then put into recording forms which is kind of almost like quality controlled through the naturalist who'll be putting that onto the recording form, and from there, then it gets put on to a natural database. So it's very much about getting the public and schools hands on with nature. So we had school children and families properly doing sweep netting and then really discovering on a small, kind of minute level, what was actually living on their step.
Chris - And what did the scientists and naturalists who you've had involved in this, what do they make of it and are they supportive?
Ed - Absolutely. I think that what we found early on particularly perhaps in previous years and last year when we first sort of started this was scientists and naturalists, being particularly modest about themselves and don't always necessarily see themselves as someone who can offer loads of opportunities. But I think now we've got the balance right of being able to enable and give the confidence to naturalists and other scientists to come forward and realise that they can feel empowered and actually take families or school groups out themselves, and actually engage people with them. So, it's had a very positive output and I think it's really nice where I think people that have enjoyed actually transfering their knowledge and their skills onto people perhaps who wouldn't normally engage or do this sort of thing.
Chris - And it's not just Bristol. This is going to be scaled up or is going to be taken to other cities around the country so we'll have one coming to Cambridge, won't we?
Ed - Absolutely. That's right. So Bristol has been leading on this in terms of being one of the first city to do this this year, linking in with the year of biodiversity and there's going to be lots of other ones over 15 or 16 across the country taking place. And people can find out where they're taking place by visiting the website bioblitzuk.org.uk and as you say, you can find out where things are going to be happening close to you. There's going to be one in Derby, there'd be one that The Natural History Museum are doing down on a coast in Devon for example. So they're going to be happening all across the country and therefore, families, the public, scientists can all engage on a local scale.
Chris - And finally Ed, what do the people who come and take part, members of the public actually make of the experience? Do they think it's just a run around in the grass with their kiddies or do they actually take away the scientific message as well?
Ed - I think people have actually really been engaging. When you're seeing actually getting down to the minute level and wanting to do more, and we had lots of families come back. So we have families for example doing the dawn chorus walk and then they came back later on to perhaps do some stream sampling or doing some insect work. So from what we can tell so far, it's been a very positive engagement with people wanting to come back and do more and hopefully continue with our Bristol Festival of Nature we've got for example in a couple of week's time in June.
Chris - Ed, brilliant. We'll have to leave it there, but thank you very much for joining us.
Ed - Thank you.

19:40 - Studying Devil Facial Tumour Disease
Studying Devil Facial Tumour Disease
with Elizabeth Murchison, Wellcome Trust Sanger Institute
Chris - A very unusual type of cancer is currently hitting Tasmanian devils called Devil Facial Tumour disease. As the name suggests, it leads to tumours on these devils' faces which makes it, amongst other things, very hard for them to eat which means they don't tend to live very long once they actually begin to show the symptoms. But what's really unusual about this tumour is that it's directly passed between the animals probably when they bite each other and Elizabeth Murchison is from the from the Wellcome Trust Sanger Institute. She's with us today and she's been looking to the genetic basis of the disease. Hello, Elizabeth. Thank you for coming in and joining us.
Elizabeth - Hello.
Chris - First of all, for people that are not acquainted or ill-acquainted with what Tasmanian devils are, just describe one for us.
Elizabeth - Tasmanian devils are a small dog-sized black creature. They have a black  coat with a white stripe under their chest and they're very well-known for their piercing nocturnal scream which is I think where they got their name from and they have very, very strong powerful jaws which they use for crunching bones.
coat with a white stripe under their chest and they're very well-known for their piercing nocturnal scream which is I think where they got their name from and they have very, very strong powerful jaws which they use for crunching bones.
Chris - They sound like wonderful creatures. What's the background to the emergence of this problem? When did it first become apparent that there was an issue with them?
Elizabeth - The story really started back in 1996 when a wildlife photographer took a picture of a devil with a strange mass on its face and he was a bit concerned at the time and he took this photograph to the local authorities and people just thought that this was just one particular devil with one strange cancer and didn't really think too much more about that. But then over subsequent years, more and more devils started to show up with these unusual facial tumours all up and down the east coast of Tasmania, and around 2000-2001, it became very, very apparent that this was a new type of infectious disease affecting devils.
Chris - And from a conservation point of view, people were presumably worried because they don't exactly go far across anywhere. They're just stuck in Tasmania, aren't they now?
Elizabeth - That's right. So devils used to be found all over Australia but they went extinct about a thousand years ago in the mainland of Australia. They've been isolated now on the island of Tasmania for about 14,000 years and they're very unique. They're not found anywhere else and they're really an icon for Tasmania.
Chris - Indeed. Well the name says it all, doesn't it? But what have researchers done then to try and work out what these tumours are and get to the bottom of how they're spreading amongst the animals?
Elizabeth - Well obviously, it was a very, very strange thing to find a cancer which was being transmitted as an infectious disease. So the first thought that people thought of was that it was probably a virus. And so, experiments were directed at trying to find viral particles in these cells and really didn't get anywhere and at the same time, researchers in Tasmania were looking at the chromosomes of the tumour, and they found surprisingly that all the Tasmanian devil tumours that they looked at had remarkably similar chromosomal rearrangement. So cancers tend to have very rearranged chromosomes but each cancer is different and has a different set of rearrangements. But the striking thing about this cancer was that all the tumours had the same, almost identical rearrangements which really couldn't occur in any other way other than them actually being the same cancer.
Chris - So somehow physically, cells from one tumour were going from one animal to the other and seeding a fresh tumour in the recipient animal.
Elizabeth - That was the only conclusion that could kind of be consistent with this data - that the same actual physical cancer cell was being transmitted between individuals probably by biting, and that the same cancer which arose once in a single individual that probably lived back in the mid-1990s has actually spread through the Tasmanian devil population and is now affecting thousands of devils around Tasmania.
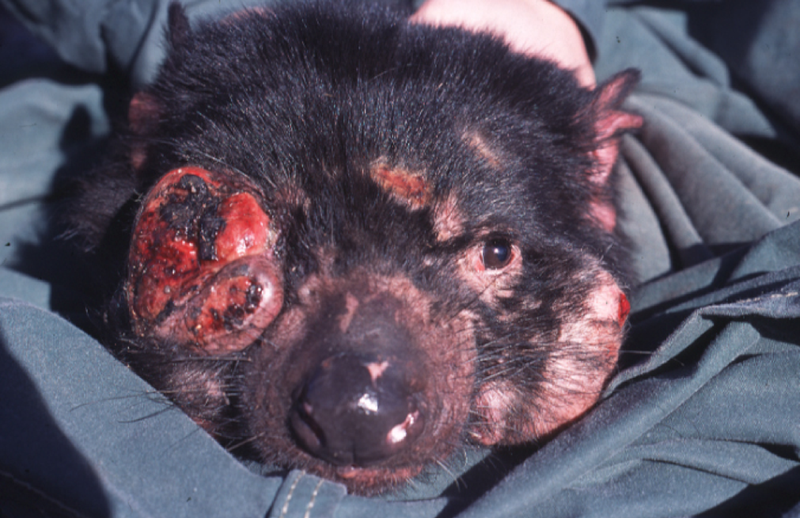 Chris - So some poor devil - excuse the pun, originally had a cancer because its chromosomes were rearranged, it had some genetic changes that made it develop a tumour and it then spawned this disease which began to pass on to other individuals.
Chris - So some poor devil - excuse the pun, originally had a cancer because its chromosomes were rearranged, it had some genetic changes that made it develop a tumour and it then spawned this disease which began to pass on to other individuals.
Elizabeth - Exactly and we really don't know very much about those early events but we think that one individual devil that probably lived up in the northeast of Tasmania got some normal type of cancer which then acquired the capability of being transmitted between individuals.
Chris - So what's special about it so it can do that because is it that the animals, because they're a restricted population, they're very, very alike and therefore, putting a cell from one animal into another, the immune system doesn't view it as necessarily that hostile so it kind of tolerates it?
Elizabeth - That's right. So there's something very, very odd about this cancer because normally if you take any tissue from one individual and put it into another individual, it gets rejected because our immune systems are able to tell self from non-self. In this case, this tumour is not being recognised as non-self and is not being rejected. And we don't really understand how that works, but one possibility is that devils are very restricted in in-bred population that don't tend to recognise self from non-self because they're too closely related. The other possibility is that perhaps the tumour is secreting substances or somehow actively tricking the immune system not to see it as a foreign tissue.
Chris - That's interesting. So devils can do this. Does that mean that other animals can or is this an isolated thing? Is this the only example of a cancer we're seeing spreading like this?
Elizabeth - No. There's another case of a naturally occurring transmittable cancer which is spread by living cancer cells in dogs actually and it's a very, very interesting cancer. It's venereal and it's transmitted by sexual contact. And it's actually a very, very old cancer that probably is at least 2,000 years old if not older than that which is spread through the entire world population of dogs and is found everywhere, but it's all derived from single cancer which arose in a dog some thousands of years ago. So the devil is not the only case.
Chris - So can you get clues from what's going on in the dogs to ask how this is happening in devils then? Does it give you clues?
Elizabeth - Exactly. That's what we're hoping to do. I'm actually studying this dog cancer quite intensively as well because I'm a geneticist and we don't have a lot of genetics tools for devils at least at the moment and so, we have a dog genome sequence that we can use to study this dog cancer and study the genetic mutations that have happened to allow this dog cancer to evade the immune system and we're hoping to perhaps transfer that to the devil.
Chris - Because if those cancers, both the dog's and the devil's are secreting something interesting, which puts the immune system off the scent, that could be really helpful medically, couldn't it? If you can work out how it's doing that because we've got a big problem with organ transplants where we have to immunosupress people very heavily to tolerate donor organs. If we had a way of making the immune system tolerate specific tissues, that could be a massive breakthrough.
Elizabeth - Absolutely and I think it's going to be very, very interesting when we start to learn how these cancers are evading the immune system and to see whether or not we could use similar strategies to trick immune systems to not recognising foreign grafts as really being foreign.
Chris - Any progress yet?
Elizabeth - It's still early days. We are finding mutations in the devil cancer which is allowing us to start to track how the devils cancer is spread through Tasmania and in the case of the dog, we're finding interesting different pockets of cancer mutations that have arisen in different continents. But it's still early days and we're hoping to eventually develop something that will be able to help the devils in the wild.
Chris - Well we wish you luck. Thank you very much. Elizabeth Murchison from the Wellcome Trust Sanger Institute.
Kat - It's also important to point out that so far, the only cancers you can catch are these devil cancer and the dog cancer and there's no worry that you can catch cancer from another person with cancer as I should point this out. I get asked that a lot. "Can you catch cancer from someone?"
Chris - Well having said that Kat, what about organ transplants because obviously, if there is a cancer that we don't know about lurking inside the donor organ, there's a possibility you could transmit that, couldn't you?
Kat - There is a possibility and also, interestingly, in patients who have had organ transplants, they're often on immunosuppressive drugs to stop their immune system attacking the cancer, and in fact, this can lead to an increase in certain types of cancer in a patient. But you shouldn't be worried if one of your relatives is affected by cancer. You can't catch it off them so that's important to point out.
Can you catch cancer?
Kat - I get asked that a lot. As far as we know, the only cancers that are contagious are these Tasmanian Devil facial cancers and this dog venereal cancer. There's no need to worry that you can catch cancer from another person with cancer.
Chris - Well having said that Kat, what about organ transplants because obviously, if there is a cancer that we don't know about lurking inside the donor organ, there's a possibility you could transmit that, couldn't you? Kat - There is a possibility and also, interestingly, in patients who have had organ transplants, they're often on immunosuppressive drugs to stop their immune system attacking the cancer, and in fact, this can lead to an increase in certain types of cancer in a patient. But you shouldn't be worried if one of your relatives is affected by cancer. You can't catch it off them so that's important to point out.
28:43 - HPV and Cervical Cancer
HPV and Cervical Cancer
with Professor Margaret Stanley, Dept. of Pathology, Cambridge University
Kat - There's lots of ways and reasons that cancer develops, but in some cases, we do know that viruses can cause the disease and the human papillomavirus or HPV is the main cause of the majority of cases of cervical cancer. And today, we're joined in the studio by Professor Margaret Stanley from the Department of Pathology at Cambridge University. Hello, Margaret.
Margaret - Hi there, Kat.
Kat - Let's talk a little bit about HPV, this virus we hear so much about in the news. How does it actually cause cancer? How does a virus cause cancer?
Margaret - Well the first thing I have to say is that HPV is a huge family of viruses, so we're only talking about a few members of this family that actually have the ability to cause cancer because they cause lots of other things, but only a few of them cause cancer. How do they do it? Well, the ones that cause cancer actually are pretty decent people on the whole, but in certain circumstances, the way in which the virus is growing in the cells is de-regulated. There are accidents that happen and the virus actually uses the cell's own ability to divide to help it make its own virus particles. But if it's turned on, if certain genes are turned on in cells that really are actively dividing then it makes the cell cycle of those cells completely chaotic. And so, it's an accident that happens, it's a rare accident, but once it happens, the cell is de-regulated, it no longer can control how often it divides, and that's the way this virus causes cancer - accidentally.
Kat - So it effectively hijacks the cell and makes them multiply.
Margaret - Absolutely.
Kat - And we're talking about lots and lots of different types of HPV. There is only a few that cause cancer. Do they cause other diseases as well?
Margaret - Yes. HPV is not just the cause of cervical cancer. It causes cancer of the vulva in women, cancer of the vagina - only 50% of those cases but it causes cancer of the anus which is the back passage and it's looking as though it causes probably more than 90% of those. And recently, it has become clear it also causes cancer in the mouth. Now it's only special places in the mouth. It's the back of the mouth, the skin that covers the tonsil and at the base of the tongue. The skin that covers the area there and it looks as though it causes probably 80 to 90% of the cancers in those sites.
Kat - Obviously, we hear about HPV infection. How does someone become infected with HPV?
Margaret - Well, in the genital area, it's a sexually transmitted infection and everybody throws their hands up at this. But I always say it's actually easier to catch HPV than it is to get pregnant. It's an inevitable part of having a normal sex life. So virtually, all of us are actually being exposed to this virus in our genital area. 80% of us probably will have been infected throughout our lives, but nearly all of us get rid of it. It's just a small fraction of people who somehow can't get rid of this virus. Their immune system can't do the business.
Kat - So this is the question obviously if many, many thousands, hundreds, millions of people are infected with HPV, but only every year, say 3,000 or 4,000 women get cervical cancer: What is the difference between having an HPV infection and getting cancer and having an HPV infection and not?
Margaret - I wish I knew.
Kat - What are the clues?
Margaret - Well of course, we don't know who is susceptible to HPV infection. We don't know which women and men are totally unable to get rid of it. What we can do of course is identify those people, those women who have not manage to get rid of the virus, and in whom these genetic events that cause cancerous cells are occurring. That's why you have cervical smears. So we can identify those people once they've started that process of turning cells into abnormal cells. But I can't go out into the population and say, "Look, I know you won't be able to get rid of HPV, so I'm going to do something about it." I can't do that.
Kat - We're going to hear later a bit more about cervical screening, but let's talk now about the vaccine because obviously, if we can prevent people from getting infected with HPV, we could actually prevent the process of developing cervical cancer at all. How does the vaccine actually work? What's it designed for? 
Margaret - The vaccine is designed to generate the immune response that would prevent the virus infecting cells. In other words, it generate antibodies and antibodies are things that bind viruses and stop them getting into cells, and if the virus can't get in to a cell, then it can't start the business of changing the cell. So the vaccine generates antibodies in you and it generates antibodies at a good level and probably all sorts of other bits of the immune response. So, you take 13-year-olds which is what we do in this country and we give them the vaccine, and that means that as they grow up through their teens, 20s and 30s, if they are exposed to the virus, the virus can't get into cells because the antibody binds to it and stops it. So that's how the vaccine works.
Kat - So it's important to protect girls before they become sexually active.
Margaret - Absolutely. Vaccines don't work once you're infected. They only work to stop you getting infected which is the reason why you take adolescents who are at that early stage in their lives, and they haven't started their sexual life.
Kat - You would certainly hope not.
Margaret - I would definitely hope so.
Kat - And how is the vaccination program going so far? What are the early results?
Margaret - It's been a stunning success. I think it's the only way I can describe it. If you're going to be effective with a vaccine, you probably need to get 80% of people vaccinated. Now, in the couple of years that this vaccination program has been going, on average, between 80% and 90% of 13 year olds in Britain have been vaccinated - an absolutely stunning success. Probably the best results in the world.
Kat - Fantastic! So in a few years, we should see a big drop in cervical cancer incidents.
Margaret - Well, initially, we're going to see a drop in the pre-cancers, the things that you hope are identified by the smears. But I think what's really important to emphasize is that we will see a drop in young women with cervix cancer - people think of cervix cancer as something that you get when you're 40, 50, 60. Actually, in this country, there are about 300 women under 30 every year who get cervical cancer. We ought to see a drop in that in the next 10 years.
Kat - Wow! We'll look forward to that. Thank you. That's Margaret Stanley from Cambridge University, shedding light on the link between HPV and cervical cancer.
36:11 - Diagnosing abnormalities from a Cervical Smear
Diagnosing abnormalities from a Cervical Smear
with Tanya Levine, Northwick Park Hospital and Thomas Ind, Sloane Street Clinic
Meera - This week, I've come along Northwick Park Hospital in London to find out the basics of the cervical screening program. Here to fill me in on this process is Tanya Levine, Consultant Cellular Pathologist here at Northwick Park Hospital. First of all, who should be screened?
Tanya - Women between the ages of 25 and 64 are invited for screening.
Meera - And when somebody comes in for a sample, we know that the sample is taken from their cervix, but what part of the cervix is the sample taken from and why that particular area? 
Tanya - The sample should come from an area of the cervix, which is the neck of the womb, and this area is called the transformation zone. And it develops at about the time of puberty and what happens at that stage is that under the influence of oestrogens, the cervix increases in size and bulk. And in so doing, some of the surface layer of cells undergo a process of squamous metaplasia, and what this really means is that the cells change their appearance, and this is a normal physiological process, but it can be hijacked if you get human papillomavirus onboard. The cells can be converted from this normal physiological pathway to the pre-cancer sequence of events.
Meera - Okay, so you have a sample and you have a slide of the cells from this transformation zone around the cervix. What changes are looked for?
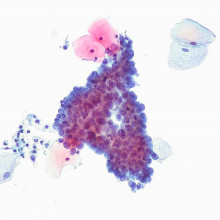
Tanya - Of the many cells that you can see on a sample, there are two basic type of cells that we are particularly interested in as cytologists. One are called squamous cells and the other are called endocervical cells. Now the squamous cells look not a little unlike fried eggs. In that the yolk of the egg is a nucleus and the white of the egg is a vision of the cell that we call the cytoplasm. We're looking to see the consistency of the nucleus or consistency of that yolk, if you will. And in so doing, we will grade those cells as mild, moderate or severely diskaryotic cells.
Meera - Okay and so, in order to just show me how clear some of these differences can be, you've got some slides here with samples taken from patients in the past.
Tanya - What I thought I'd show you is a normal sample, just to get your eye in on what we're looking at down a microscope, and Meera, if you look down the field at the moment, what you can see are normal squamous epithelial cells. Now these are the fried egg cells that I was talking about earlier.
Meera - And looking through actually, the nucleus is very small compared to the overall size of the cell.
Tanya - These are entirely normal. If you look at this sample now, there's actually a 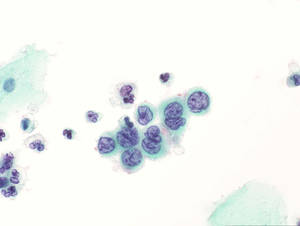 range of appearances that we can see here in these squamous epithelial cells. The nucleus is taking up much more of the surface area of the cell. In fact in this cell, it's virtually filling it and this is a severely diskaryotic cell.
range of appearances that we can see here in these squamous epithelial cells. The nucleus is taking up much more of the surface area of the cell. In fact in this cell, it's virtually filling it and this is a severely diskaryotic cell.
Meera - How many of the samples that come through are abnormal?
Tanya - In our laboratory, we process just under 60,000 samples a year, and about 93% to 94% will be negative.
Meera - So of those 6% to 7% that are abnormal, what's the next step?
Tanya - Someone with low grade abnormalities may have repeat smear. For women with moderate or worse abnormalities, they will be referred to the colposcopy unit.
Meera - That was Tanya Levine, Consultant Cellular Pathologist at Northwick Park Hospital. The presence of abnormal cells in a cervical smear doesn't mean that a treatment will be needed. The next step as we've heard is to have a colposcopy to investigate the area further. So I'm now at the Sloane Street Clinic in London with gynaecological surgeon, Thomas Ind.
Thomas - Some abnormal smears just need to be repeated. If you have another abnormality, you would come for a colposcopy which is an examination of the cervix using a specially designed microscope with some dyes. If there is an area that we can see suspicious or pre-cancerous change, we would take a local biopsy.
Meera - What's the next step then if any abnormality is confirmed?
Thomas - Most of the time, your body has the natural ability to clear these cells, but what they can do is they can form abnormalities at the bottom part of the basement membrane which is the area of the cervix that lines the cervix. Now with only the bottom third of that basement membrane is affected and has had cellular change in the nucleus, we would call that CIN1 and most of the time, that goes away on its own unchanged. If two-thirds to three-thirds of that area is affected, that would be CIN2 and CIN3 respectively. There is a good chance if we don't treat those abnormalities, that it would progress to cancer in the future. So women with those abnormalities generally have treatment. 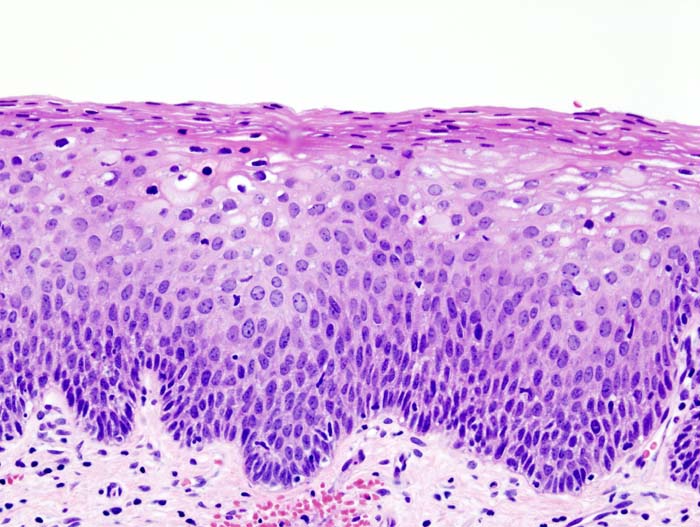
Meera - And what does CIN stand for?
Thomas - Cervical Intraepithelial Neoplasia. What that really means is cervix in the skin, new cells.
Meera - So a patient has come in and been found to have say, CIN levels 2 or 3, what are the options available to them?
Thomas - The most common treatment in the UK at the moment is something called a loop cone biopsy. It's also called a LETTS procedure and in the States, they call a LEEP procedure, and what normally happens is that during a colposcopy, a small sugar cube sized piece of tissue is excised from your cervix, removing the area of abnormality. We now use a form of energy called diathermy which is a just a very high voltage electrical instrument that removes the piece of tissue a bit like a cheese wire and it's done very swiftly in a few minutes.
Meera - What would you say the success rate is for people that come in for these treatments to not need them again or to actually prevent them from getting cancer?
Thomas - If you have a treatment, it's generally about 95% successful and by that, I mean, you will never have another abnormal smear again.
Meera - And just lastly, how would you summarise then the benefits of the screening process as a preventative measure against cervical cancer?
Thomas - Well I think most people would agree that the National Health Service Cervical Screening Program is probably one of the best cervical cancer prevention programs in the world. It's all about getting people to attend and in this country, nearly 80% of people attend for their cervical smears. It's attendance which is the key issue, not the process that you go through afterwards, and this is the problem that we've encountered with the vaccine is that if people don't attend for the vaccine, it doesn't matter how effective it is, it's not going to prevent cervical cancer.
Chris - Thomas Ind from the Sloane Street Clinic and before him, Tanya Levine from Northwick Park Hospital and they were talking to Meera Senthilingam about the importance of cervical screening.
What are the consequences of HPV infection in males?
We posed this question to Margaret Stanley from the University of Cambridge:
HPV is transmitted from skin to skin. So it's very important to emphasize that you don't have to have full sexual intercourse, penetrative intercourse. Foreplay, kissing is an easy way of transmitting. Now, more men than women get cancer of the anus, the back passage. Men get cancer of the head and neck and it looks as though more men than women get cancer there as well. So yes, there are men who get HPV from women, women who get it from men, men get it from other men if they have sex with them, and it's the same for women with women.
How are translocations related to cancers?
We posed this question to Elizabeth Murchison from the Wellcome Trust Sanger Institute...
Elizabeth - Well cancer happens when genes called tumour suppressor genes and oncogenes are mutated and cause the cell to start dividing abnormally. And this can happen when you get single point mutations in your DNA which mutate an oncogene or a tumour suppressor gene, but they can also occur when two genes can come together abnormally in a translocation and what this can often do is to drive a gene which is not normally active in a particular cell type up to an abnormal level of activity which can sometimes cause the cell to become cancerous. Chris - I get it. So by the chromosomes rearranging themselves, the gene which would normally be off in a cell can end up being put next to a gene which is normally on in that cell, so the cancer causing gene also gets turned on abnormally and makes the cell misbehave. Elizabeth - That type of thing, yes.

51:37 - Why do donkeys sound different to horses?
Why do donkeys sound different to horses?
We posed this Question to Dr Alban Lemasson from University of Rennes in France...
Alban - So to this question, I really can't say because there's just very few work done on equine vocal communications. The only thing we know is from horses. We don't know anything between mules and donkeys, or zebras for instance. My only experience is when I was working in the fields, I often listened to zebras and it sounds like in between mules and horses. But we really don't know this has to be studied more systematically. It has something to do with phylogeny and anatomy. Diana - Believe it or not, no one has worked on comparing the noises of these animals properly. Alban suggested anatomy may play a role. So let's hear how different these noises are and here's a horse: A donkey: And a zebra: There is a sort of similarity between them all with both the zebra and the donkey doing that sort of hiccup with their braying. Now donkeys and zebras are thought to be more closely related. So it could be something the modern horse hasn't inherited, or they might differ because of the social organisation of their species. Horses actually have a number of different calls as Alban describes. Alban - They have a very small vocal repertoire of a few calls and one call is particularly interesting. It's the weenie call that we have studied more intensively and this is a particular call that they often produce when they are far from each other. So it's a kind of long distance contact call. So in order to be sure that this has a social function, we studied the acoustic structures of weenie calls to see if we can find acoustic differences between individuals. And we found that duration or frequency parameters change. For instance, you can have a much higher pitch voice in mares than in geldings which are also higher pitched than stallions. But it also depends on the social status of the animal because dominant stallions have a much lower pitch voice than subordinate stallions. Then finding these acoustic differences doesn't guarantee that the animals will use it, so we have conducted a playback experiment and we played the weenie calls of three social categories of horses, the familiar neighbours, familiar strangers, and group members and we found that our horses when hearing these three voices could discriminate the social category of the caller, and they adapted their behaviour response in accordance to the caller. They would be more attracted and willing to go towards the loud speaker for familiar animals, but they would be very vigilant and careful when hearing unfamiliar animals. So that gives us the conclusion that we found acoustic differences between individuals and these acoustic differences can be used by animals and decoded by animals. Diana - So if a horse has developed different calls for social encounters, perhaps the divergence in their societies has caused a divergence in their noises. We had one listener, Siobhan in Ireland, he wrote in to tell us about the breeding program in Russia to domesticate silver foxes. One of the notable developments was that they began to bark, they began to wine and they developed a more diverse range of vocal communication. So, if we domesticate horses and donkeys on the basis of their ability to communicate just a bit with us, perhaps that's caused a change in their voices too. If anyone out there has cleaned out a stable, they'll know all about the smell of urine. But what if it smells of your last meal?
- Previous Biofuels from the Burning Bush
- Next Why can't we Tickle Ourselves?











Comments
Add a comment